Key messages
Why is it important?
Disability is an umbrella term for impairments of body function or structure, activity limitations or participation restrictions. The causes of disability are complex. It can be the result of genetic disorders, illnesses, accidents, ageing, or a combination of these factors. People experience different degrees of impairment, activity limitation and participation restriction. For Aboriginal and Torres Strait Islander (First Nations) people experiences of disability are shaped by broader social determinants and systemic inequities. These include limited access to culturally safe health care, early intervention, and rehabilitation services, as well as the impacts of colonisation and intergenerational disadvantage. First Nations people with disability are twice as likely to experience discrimination and face significantly lower access to health care, education, and employment opportunities compared to the general population. A social model of disability highlights how systemic and environmental barriers – not impairments alone – limit full participation.
Data findings
-
In 2022–23, 37% (about 367,700) of First Nations people reported having a lived experience of disability, based on the 2022–23 National Aboriginal and Torres Strait Islander Health Survey (NATSIHS).
-
After adjusting for differences in the age structure between the two populations, the 2022–23 NATSIHS reported that First Nations people were 1.5 times as likely as non-Indigenous Australians to live with disability (42% and 29%, respectively) and 2.0 times as likely to have a profound/severe core activity limitation (7.6% and 3.9%, respectively).
-
In the 2022–23 NATSIHS, the 4 most common self-reported disability types for First Nations people aged 15 and over were physical disabilities (55%, or 202,400 of those living with disability), sensory and speech disabilities (43%, or 156,800), learning and understanding disabilities (28%, or 102,300) and psychosocial disabilities (28%, or 102,000).
-
The proportion of First Nations people living with any type of disability in the 2022–23 NATSIHS increased with age until 65 years and older, ranging from 21% of those aged 0–14 to 68% of those aged 55–64.
-
In 2022–23, 39% (122,300) of First Nations people aged 5–64 living with disability reported having an education restriction due to disability. For those aged 5–14 the proportion of people living with disability reporting having an education restriction was 61% (or 35,700 children).
-
In the 2022–23 NATSIHS, First Nations people aged 15 and over who reported living with disability were less likely than those without disability to be employed (42% compared with 63% respectively), more likely than those without a disability to be living in households in the lowest income quintile (31% and 25%, respectively), and to have had problems accessing services (60% and 35%, respectively).
-
As at 30 June 2025, 60,529 First Nations people were participants of the National Disability Insurance Scheme (NDIS) (8.2% of all participants) – an increase from 52,782 (8.0%) in June 2024.
-
In 2021, 15% (76,600) of First Nations people aged 15 and over provided unpaid assistance to a person with disability, long-term health conditions or problems related to ageing. First Nations females were more likely to be providing unpaid care than First Nations males – 18% compared with 12%.
-
In 2021, after adjusting for differences in the age structure between the two populations, the Census data show that the proportion of First Nations people providing unpaid care to a person with disability, long-term health condition or problems related to ageing was 1.3 times the proportion for non-Indigenous Australians.
Research and evaluation findings
-
Disability services often fail to meet the cultural needs of First Nations people, with persistent gaps in culturally responsive and high-quality support, particularly in regional and remote areas. These findings highlight the urgent need for systemic reform to ensure services are culturally safe, inclusive, and aligned with First Nations priorities.
-
Common barriers to accessing health services include cost, competing work or personal responsibilities, fear or discomfort in seeking care, choosing not to seek care, and long waiting times or unavailable service. Accessing the NDIS is particularly challenging, especially in remote and very remote communities. Mainstream services often overlook cultural needs, leading to mistrust and disengagement.
-
The Disability Royal Commission underscored the importance of listening to the voices of First Nations people with disability in shaping policies and services where First Nations people: i) prefer services delivered by First Nations providers; ii) Find mainstream services geographically and culturally inaccessible and hard to navigate; iii) often received health care at a later stage, and potentially in acute hospital settings when the issues became more critical.
-
A recent review of current literature about First Nations people with disability concluded that many disability services do not adequately consider the cultural needs of First Nations people or communicate in a culturally appropriate manner, and more work is needed to align disability services with culturally appropriate support to provide better health outcomes.
-
A study focusing on access to services that increase the likelihood of First Nations people with disability to live independent and socially inclusive lives identified: i) significant access and equity barriers to culturally appropriate disability support services; ii) the importance of strategies to attract, develop and retain First Nations workers in the First Nations disability workforce; iii) the importance of culturally safe disability services and community-centred principles; and iv) the importance of strategies such as cultural training for workforce development.
Implications
- National strategies must embed First Nations cultural understandings of disability, which prioritise collective wellbeing and inclusion. Improving accessibility to the NDIS – particularly in remote areas – requires investment in First Nations-led, culturally safe service models. The NDIS First Nations Strategy 2025–30, co-designed with the National Aboriginal Community Controlled Health Organisation (NACCHO), First Peoples Disability Network (FPDN), and other community partners, aims to make the NDIS more equitable and responsive. Strengthening partnerships across First Nations health, aged care, and disability services, alongside sustained investment in First Nations workforce development and community-controlled organisations, is essential to delivering inclusive, integrated care.
Why is it important?
Disability is an umbrella term for impairments of body function or structure, activity limitations or participation restrictions. The causes of disability are complex and are often unidentified in datasets. The ‘medical model’ of disability frames disability as a health condition which can be the result of genetic disorders, illnesses, accidents, ageing, or a combination of these factors. People experience different degrees of impairment, activity limitation and participation restriction (AIHW 2024).
However, disability is increasingly understood using a ‘social model’ where disability is seen as socially constructed as the result of interactions between individuals living with impairments and the physical, social, and attitudinal barriers to full participation in society. Rather than focusing on impairments, this approach highlights the barriers that can restrict access, inclusion, and opportunity (People with Disability Australia 2025). According to the AIHW, disability reflects a dynamic relationship between health conditions, environmental factors, and personal circumstances (AIHW 2024). For Aboriginal and Torres Strait Islander (First Nations) people, experiences of disability are shaped by broader social determinants and systemic inequities. These include limited access to culturally safe health care, early intervention, and rehabilitation services, as well as the impacts of colonisation and intergenerational disadvantage.
First Nations people with lived experience of disability often encounter systemic barriers rooted in colonisation and racism, which continue to shape life outcomes and access to opportunity. These intersecting forms of discrimination contribute to exclusion across key areas such as health care, education, and employment (Daniels-Mayes 2023). Research shows that First Nations people with disability are twice as likely to experience discrimination and face significantly reduced access to essential services compared to the broader population (Avery 2018). The intersecting layers of racism and disability discrimination create a double disadvantage for First Nations people, as highlighted in the Disability Royal Commission Final Report – Volume 9: First Nations People with Disability. This volume documents systemic barriers and recommends reforms to improve cultural safety and service access. Common barriers to accessing health services include cost, competing work or personal responsibilities, fear or discomfort in seeking care, choosing not to seek care, and long waiting times or unavailable services (AIHW 2024). Accessing the National Disability Insurance Scheme (NDIS) is particularly challenging, especially in remote and very remote communities. These difficulties occur both in entering the scheme and in receiving supports once approved. Contributing factors include thin markets (limited availability of providers in remote areas), significant service delivery gaps, low awareness of NDIS eligibility and benefits, and cultural barriers that affect trust and engagement (Royal Commission into Violence‚ Abuse‚ Neglect and Exploitation of People with Disability 2023). Mainstream services, designed for the general population rather than First Nations‑specific services, often overlook cultural needs, which can contribute to mistrust and disengagement among First Nations people (Avery 2018).
The National Agreement on Closing the Gap (the National Agreement), was developed in partnership between Australian governments and the Coalition of Aboriginal and Torres Strait Islander Peak Organisations. It is built around 4 Priority Reforms directly informed by First Nations people. These reforms aim to change how governments work with First Nations people by fostering partnership and shared decision-making, building the Aboriginal community-controlled sector, transforming government organisations, and improving and sharing access to data and information to enable informed decision making by First Nations communities. The National Agreement has identified the importance of making sure First Nations people enjoy long and healthy lives. It aims to centre First Nations people with disability in national policies, programs, and reforms, ensuring that investments across all targets and Priority Reforms are accessible, inclusive, and equitable for First Nations people with disability.
Furthermore, there are several disability specific strategies that have been developed that either identify First Nations people as a priority population or are tailored to First Nations people’s needs at various stages in the disability services policy environment. For example, the NDIS First Nations Strategy 2025–2030 emphasises the importance of culturally safe access, stronger community engagement, and co‑design with First Nations people and organisations. The National Disability Advocacy Framework 2023–2025 commits governments to work together to improve access to disability advocacy services and work with First Nations people and organisations in line with the Closing the Gap Priority Reforms.
The First Peoples Disability Network (FPDN) is the peak national organisation representing First Nations people with disability, their families, and communities. FPDN actively engages with communities across Australia and advocates for their interests both nationally and internationally. Their work aims to ensure that the voices and needs of First Nations people with disabilities are heard and addressed. In addition to its advocacy and research work the FPDN has been actively partnering with government agencies to improve disability policy and services to better meet the needs of First Nations people with disability, including work that is aligned with Priority Reform 2 of the National Agreement, building the community-controlled sector.
The National Aboriginal and Torres Strait Islander Health Plan 2021–2031 (the Health Plan) sets out a clear vision for First Nations people to live long, healthy lives grounded in culture, supported by services that are prevention-focused, culturally safe, responsive, equitable, and free from racism. As part of this vision, the Health Plan actively supports First Nations people with disability by embedding partnerships and shared decision-making across the health, disability, and aged care systems (Objective 1.1). It drives the implementation of strategies to grow the First Nations workforce across health, mental health, disability, and aged care (Objective 3.1), and works to improve cultural safety in workplaces across these sectors (Objective 3.2). The Health Plan also acknowledges and addresses institutional racism, ensuring it is measured and reported (Objective 8.1), and commits to improving access to responsive health care for people with disability (Objective 9.7).
The National Agreement, FPDN, disability specific strategies and the Health Plan are discussed further in the Implications section of this measure.
Data findings
Disability prevalence: findings from ABS survey data
There are 2 main surveys that provide data on First Nations people with disability, the Australian Bureau of Statistics’ (ABS) Survey of Disability, Ageing and Carers (SDAC), and the National Aboriginal and Torres Strait Islander Health Survey (NATSIHS). The Census also provides data on the need for assistance with core activities in Australia (see ‘Box 1.14-1: Sources of disability data’).
Based on data from the 2022 SDAC, an estimated 25% (183,700) of First Nations people surveyed reported living with disability in 2022, similar to the proportion in 2018. An estimated 12% (84,400) of First Nations people surveyed reported living with severe or profound limitation, meaning they need help or supervision always (profound) or sometimes (severe) to perform activities that most people undertake at least daily – core activities of self-care, mobility and/or communication (ABS and Avery 2025a).
Based on data from the 2022–23 NATSIHS, 37% (an estimated 367,700 out of 993,800) of First Nations people reported they lived with disability. The rate of disability was similar for First Nations males and First Nations females (36% and 37% respectively) and generally increased with age (21% for those aged 0–14, and 64% for those 65 and over) (Table D1.14.2).
The estimated total proportion of First Nations people living with disability based on the NATSIHS is higher than those from the SDAC as NATSIHS uses the Short Disability Module (SDM) to determine disability status and severity. Additionally, NATSIHS has been designed to generate results that are more representative for First Nations people, particularly in more remote areas while SDAC excludes First Nations people in Very remote areas (see ‘Box 1.14-1: Sources of disability data’). The remainder of this section therefore focuses on data from NATSIHS.
Based on 2022–23 NATSIHS, the 4 most common self-reported disability types for First Nations people were physical restriction disabilities (55% of those with disability; 202,400 people), sensory and speech disabilities (43%; 156,800), learning and understanding disabilities (28%; 102,300) and psychosocial disabilities (28%; 102,000) (Table D1.14.4, Table D1.14-1).
Table 1.14-1: Disability type for First Nations people with disability, by age group, 2022–23
|
Disability type |
0–14 |
15–24 |
25–34 |
35–44 |
45–54 |
55–64 |
65+ |
Total |
|---|---|---|---|---|---|---|---|---|
|
Sensory and speech |
50.6% |
33.1%# | 36.9% | 29.0% | 43.6% | 48.1% | 54.5% | 42.6% |
|
Physical restriction |
15.2% |
39.7% | 59.9%# | 65.3%# | 73.4% | 78.6% | 80.8% | 55.0% |
|
Learning and understanding |
51.7%# |
44.6%# | 22.4% | 15.9% | 13.4% | 14.8% | 11.7% | 27.8% |
|
Psychosocial |
29.8% |
37.4%# | 33.8% | 29.3% | 23.5% | 21.8% | 13.8% | 27.7% |
|
Head injury, stroke or acquired brain damage |
0.9%# |
0.6%# |
1.4%# |
0.9%# | 7.1% | 3.7% | 3.4% | 2.4% |
|
Other |
14.5% |
13.9% | 21.2%# | 26.8%# | 37.1%# | 37.6% | 40.8% | 25.7% |
|
Total number with disability |
70,200 |
66,800 |
50,900 |
44,100 |
47,700 |
51,300 |
38,500 |
367,700 |
# Due to the high margin of error, the data may not be statistically reliable and should be interpreted with caution.
Note: More than one disability type may be reported and thus the sum of the components may add to more than 100 per cent.
Source: Table D1.14.4. AIHW and ABS analysis of the National Aboriginal and Torres Strait Islander Health Survey 2022–23.
Around 7% (69,200) of First Nations people had a profound or severe core activity limitation according to the 2022–23 NATSIHS, and 12% (121,900) reported a moderate or mild core activity limitation. A further 7% (69,900) reported they had disability that only restricted their engagement with school and/or employment activities (Table D1.14.4, Figure 1.14.1).
Figure 1.14.1: Prevalence of disability by severity for First Nations people, 2022–23
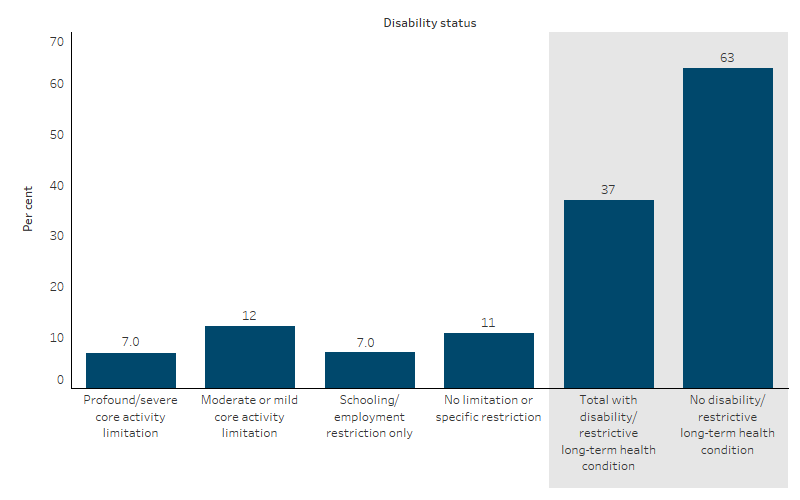
Note: 'Has an impairment with no limitation or specific restriction' includes persons living with an impairment but having no specific limitation with core activities or restriction with schooling or employment activities..
Source: Table D1.14.4. AIHW and ABS analysis of National Aboriginal and Torres Strait Islander Health Survey 2022–23.
Based on the 2022–23 NATSIHS, after adjusting for differences in the age structure between the two populations, First Nations people were 1.5 times as likely as non-Indigenous Australians to live with disability (42% and 29%, respectively) and 2.0 times as likely to live with a profound/severe core activity limitation (7.6% and 3.9%, respectively) (Table D1.14.3).
The rate of First Nations people living with any type of disability increased with age until 65 and over, ranging from 21% of those aged 0–14 to 68% of those aged 55–64. The prevalence of disability was significantly higher amongst First Nations people compared with non-Indigenous Australians in all age groups excluding 65 and over, where the difference was not statistically significant (Table D1.14.3, Figure 1.14.2).
Figure 1.14.2: Disability status, by Indigenous status and age, 2022–23
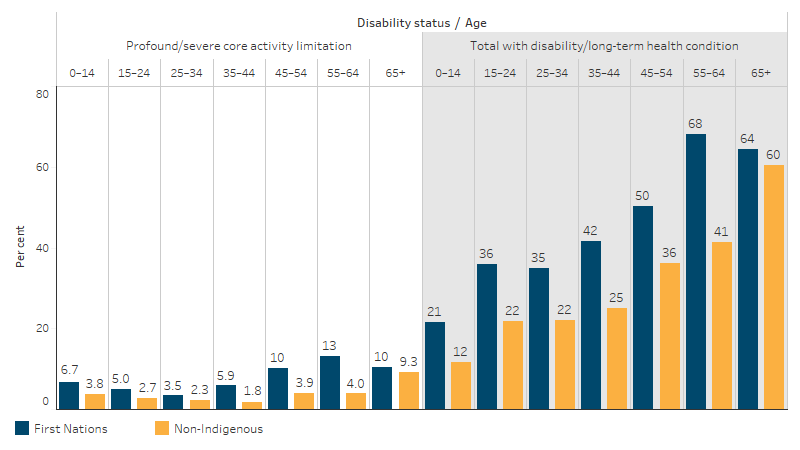
Source: Table D1.14.3. AIHW and ABS analysis of National Aboriginal and Torres Strait Islander Health Survey 2022–23 and National Health Survey 2022.
In 2022–23, 39% (122,300) of First Nations people aged 5–64 living with disability reported having an education restriction due to disability. For those aged 5–14 the proportion living with disability reporting having an education restriction was 61% (or 35,700 children). The proportion of First Nations people living with disability reporting having an education restriction was higher in non-remote areas than in remote areas (40% compared with 25% respectively) (Table D1.14.5).
Over half (54% or 140,900) of First Nations people aged 15–64 living with disability reported having an employment restriction due to disability. The proportion of First Nations people living with disability reporting having an employment restriction was higher in non-remote areas than in remote areas (56% compared with 41% respectively) (Table D1.14.5).
For First Nations people aged 15–64 who reported having an employment restriction due to disability the employment rate was 26%, compared with 69% for other First Nations people with disability (but with no employment restriction) (Table D1.14.5).
In 2022–23, 42% of First Nations people aged 15 and over who reported living with disability were employed, compared with 63% of First Nations people who did not report living with disability (Table D1.14.8). First Nations people aged 15 and over living with disability were more likely than those without disability to be living in households in the lowest income quintile (31% compared with 25%, respectively), and to have had problems accessing health services in the previous 12 months (60% and 35%, respectively) (Table D1.14.8, Table D1.14.28).
First Nations people aged 15 and over who reported living with a disability in 2022–23 were 9.6 times as likely to live with 3 or more chronic conditions as First Nations people who reported not living with a disability (27% compared with 2.8% respectively). Those reporting living with disability were also 2.8 times as likely to experience high and very high levels of psychological distress as those without disability (48% and 17% respectively) (Table D1.14.28).
The self-reported rate of disability was the lowest amongst First Nations people in the Northern Territory (29%) and highest in Victoria and Tasmania (44%) based on the 2022–23 NATSIHS. The rate was significantly different across remoteness areas (38% in non-remote areas and 31% in remote areas) (Table D1.14.2, Figure 1.14.3).
Figure 1.14.3: First Nations people reporting disability, by jurisdiction and remoteness, 2022–23
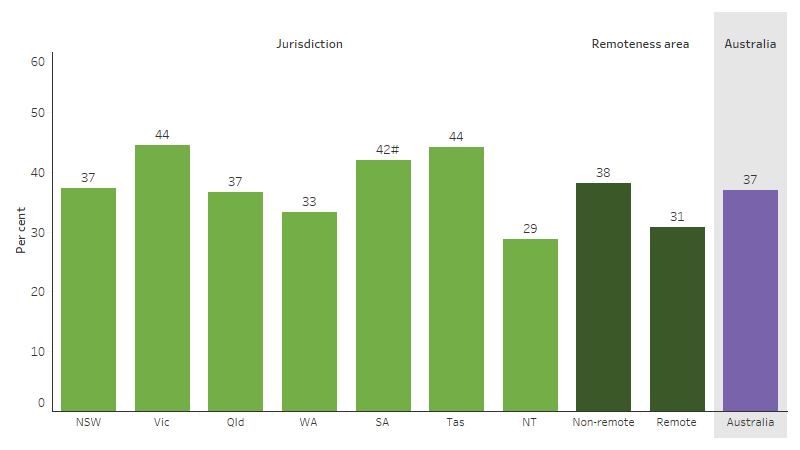
# Due to the high margin of error (>10 percentage points), the data may not be statistically reliable and should be interpreted with caution.
Source: Table D1.14.2. AIHW and ABS analysis of National Aboriginal and Torres Strait Islander Health Survey 2022–23.
Assistance with core activities: Findings from Census data
The ABS Census of Population and Housing (the Census) collects data on a subset of people with disability, specifically those needing assistance with core activities (equivalent to severe or profound disability as collected in the NATSIHS) (see also Box 1.14-1: Sources of disability data).
In 2021, 8.6% (about 66,400) of the total First Nations population were identified as needing assistance with core activities (self-care, mobility or communication) some or all the time (Table D1.14.10). This proportion was 9.3% for First Nations males, compared with 7.9% for First Nations females.
Based on the 2021 Census, among First Nations people:
- 2.7% of children aged 0–4 needed assistance with core activities, increasing to 8.5% and 8.8% for children aged 5–9 and 10–14, respectively.
- In age groups between 15–19 to 40–44, the proportion who needed assistance with core activities varied between 4.5% and 7.0%.
- For those aged between 45–49 to 75 and over, the proportion who needed assistance with core activities increased with age, from 8.7% to 43% (Table D1.14.10, Figure 1.14.4).
While broadly similar patterns by age were seen among non-Indigenous Australians, the proportion of First Nations people who needed assistance with a core activity was higher in all age groups when compared with non-Indigenous Australians. The increasing prevalence with age also began earlier for First Nations people (from around age 30) than for non-Indigenous Australians (from around age 40). The relative difference in rates for First Nations people and non-Indigenous Australians was highest between the ages 35 and 59 (rate ratios between 2.8 and 3.0) (Table D1.14.10, Figure 1.14.4).
Figure 1.14.4: People needing assistance with core activities, by Indigenous status and age group, 2021
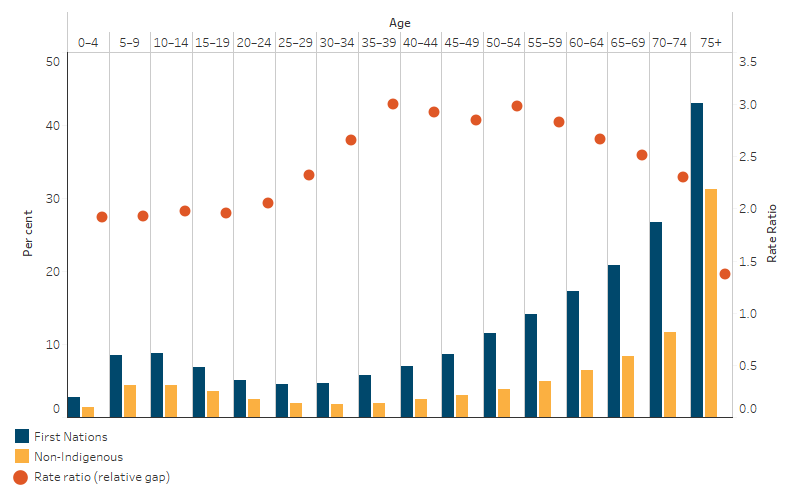
Source: Table D1.14.10. AIHW and ABS analysis of Census of Population and Housing 2021.
Across jurisdictions, the proportion of First Nations people who reported needing assistance with a core activity in 2021 varied between 5.5% in the Northern Territory to 10.4% in Victoria (Table D1.14.12).
In 2021, the proportion of First Nations people with a need for assistance with a core activity ranged from 4.3% in Very remote areas and 9.7% in Inner regional areas (Table D1.14.11).
In 2021, First Nations people were 2.1 times as likely to need assistance with a core activity when compared with non-Indigenous Australians, based on age-standardised rates (Table D1.14.12).
Social and cultural connections
Note – The National Aboriginal and Torres Strait Islander Social Survey (NATSISS) which collects detailed information on the social and cultural experiences of First Nations people has not been conducted since 2014–15. The following data therefore cannot be updated.
Connections to culture, family and the community, along with engagement in cultural activities, are important in reducing isolation and improving access to supportive networks. A feature article from the 2014–15 NATSISS presented findings on the lived experiences of First Nations people who were living with disability or a long-term restrictive condition (ABS 2016).
First Nations people with severe or profound disability were less likely to have had daily face-to-face contact with family or friends outside their household, compared with those with no disability (35% compared with 45%).
In 2014–15, First Nations people with severe or profound disability were less likely to have received support in a time of crisis from a family member (78%) or friend (55%) from outside their household, compared with those who did not have disability (85% and 64%, respectively). However, they were more likely to have received crisis support from community, charity or religious organisations (20%) or health, legal or financial professional (15%) than those with no disability (12% and 8%, respectively).
In 2014–15, the proportion of First Nations people who reported they recognised their homelands or traditional Country, identified with a clan, tribal group or language group and/or spoke an Indigenous language was similar for those who were living with disability and those who did not. Reporting participation in cultural events was also similar, regardless of disability status (ABS 2016).
Unpaid carers
The ABS Census of Population and Housing 2021 collected data on those who provided care for family members or others. In 2021, 15% (76,600) of First Nations people aged 15 and over provided unpaid assistance to a person with disability, long-term health conditions or problems related to ageing (excluding those for whom carer status was not stated). By age group, the proportion of First Nations people who were providing unpaid care was highest for those aged 45–54 (21%), followed by those aged 35–44 and 55–64 (both 20%) (Table D1.14.15).
First Nations females were more likely to be providing unpaid care than First Nations males – 18% compared with 12% (AIHW analysis of ABS 2023).
After adjusting for differences in the age structure between the two populations, the proportion of First Nations people providing unpaid care to a person with disability, long-term health condition or problems related to old age was 1.3 times the proportion for non-Indigenous Australians (Table D1.14.15).
In 2021, of First Nations people who provided unpaid assistance to a person with disability, long-term health condition or problems related to ageing, 48% (36,300) were employed, 8.0% (6,000) were unemployed, and 44% (33,800) were not in the labour force. First Nations people providing unpaid assistance were slightly less likely to be in the labour force than those who did not provide unpaid care (56% compared with 58%) (Table D1.14.26). From 2011 to 2021, the median weekly income of First Nations carers providing unpaid assistance to a person with disability, long-term illness or problems related to old age increased from $359 to $563 (Table D1.14.27).
It is important to note that these data may underestimate the true extent of unpaid caring in First Nations communities. Census data rely on definitions of unpaid work that may not relate to the experience of respondents, particularly where there are cultural expectations around unpaid care, with reciprocity playing an important role in social relationships (Klein et al. 2023).
National Disability Insurance Scheme
As at 30 June 2025, 60,529 First Nations people were participants of the National Disability Insurance Scheme (NDIS), comprising 8.2% of all participants – an increase from 52,782 (8.0%) in June 2024 (NDIS 2025c).
New South Wales and Queensland had the largest number of First Nations NDIS participants (20,541 and 17,279, respectively) – these are also the jurisdictions with the largest First Nations populations. The highest rate of NDIS use among First Nations people was in Victoria (86 per 1,000 population), followed by South Australia (77 per 1,000 population) (Figure 1.14.5).
Figure 1.14.5: First Nations NDIS participants, by jurisdiction, 30 June 2025
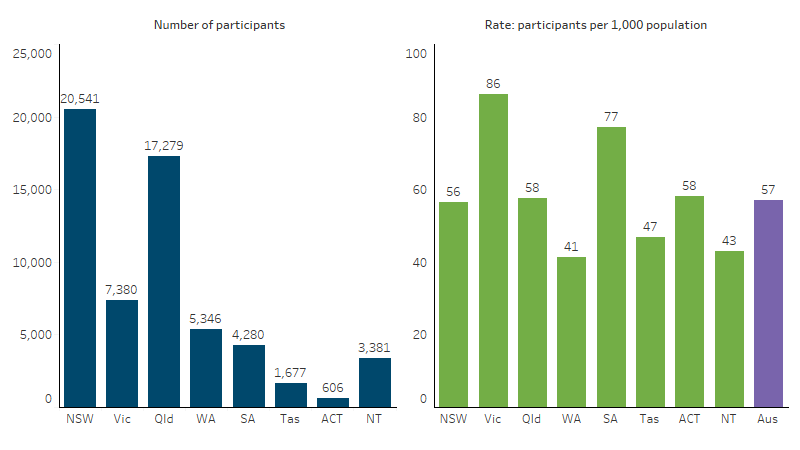
Note: Rates calculated using ABS projections of the First Nations population at 30 June 2025 (medium series) based on the 2021 Census of Population and Housing.
Source: AIHW analysis of National Disability Insurance Scheme data.
Among the First Nations NDIS participants on 30 June 2025, the average annualised committed support was $84,000 per person, similar to that for all participants ($83,000) (NDIS 2025a, 2025b, 2025c). The average annualised committed support is calculated using participants’ support budget converted to a yearly rate and divided by the number of participants (rounded to the nearest thousand dollars). Note that not all committed support may have been accessed or used by participants.
In Remote and very remote communities, the average annualised committed support for First Nations NDIS participants was $128,000 per person, compared with $81,000 for First Nations participants in Metropolitan areas and $78,000 in Regional centres and Rural towns (AIHW analysis of NDIS 2025a). People with disability in remote communities, along with their families and carers, can face particular challenges such as limited service choice and availability, the need for travel and transportation, and difficulties with recruiting, training and retaining professionals (NDIS 2016).
More detailed, but less recent, data on First Nations NDIS participants are available for the period ending 30 June 2019 (NDIS 2019). As at 30 June 2019, the most common primary disabilities amongst First Nations participants were intellectual disability (30%) and autism (28%). For non-Indigenous participants, these were also the two most common primary disabilities – 27% and 31%, respectively.
The two-thirds (65%) of First Nations NDIS participants were aged under 25, compared with 54% of non-Indigenous participants.
First Nations participants were less likely to be living in Major cities than non-Indigenous participants (43% compared with 68%, respectively), and more likely to live in Remote and very remote areas than non-Indigenous participants (11% compared with 1%, respectively).
Supported Independent Living arrangements (help with and/or supervision of daily tasks) were included in the plans of 6% of First Nations participants aged under 25 and 15% of those aged 25 and over, similar to the proportions for non-Indigenous Australians (7% and 15%, respectively).
First Nations participants utilised less of the committed supports in their plans than non-Indigenous participants – 60% compared with 67%, respectively (NDIS 2019).
Disability support services
Specialist disability support services for Australians with permanent and significant disability are now largely provided through the NDIS. Most, but not all, National Disability Agreement (NDA) services, and the people using them, have transitioned to the NDIS. Information on the use of services provided under the NDA was previously collected annually in the Disability Services National Minimum Data Set, with 2018–19 being the last year of collection under this data set.
In 2018–19, 12,079 First Nations people were receiving services under the NDA, 5.5% of all users (excluding those for whom Indigenous status was not stated) (AIHW 2020). The majority (78%) of First Nations service users were aged under 50, 21% were aged 50–64, and 1% were aged 65 and over. First Nations service users were generally younger than non-Indigenous service users, with an average age of 35, compared with 40 for non-Indigenous users.
Research and evaluation findings
Recent reviews and systematic analyses consistently show that disability services often fail to meet the cultural needs of First Nations people and lack culturally appropriate communication. Evidence highlights persistent gaps in culturally responsive and high-quality services, particularly for families in regional, rural, and remote areas. These findings underscore the need for systemic reform to ensure services are culturally safe, inclusive, and aligned with First Nations priorities (D’Aprano et al. 2024; James et al. 2023; Trounson et al. 2022).
Further research highlights persistent environmental and systemic barriers to delivering services for First Nations adults with disability in remote communities, including geographic isolation, high costs, inadequate infrastructure, inflexible policies, and cultural mismatches in service delivery models. These factors continue to limit access to culturally responsive disability services and require policy solutions that address both environmental and systemic challenges (Gilroy et al. 2021).
People with disability living in rural and remote areas often face additional challenges that are distinctly different from those faced by people who live in metropolitan areas. A Department of Social Services evaluation published in 2018 on the performance of the NDIS in the Barkly region in the Northern Territory found the prevalence of disability and associated health and social support needs were high in the area. The number of actual participants in the NDIS, however, was felt to be an underestimate of these high levels of disability. While attempts were made over time to adapt NDIS processes to local need, by the end of the evaluation period it was still felt that both the approach and implementation of the NDIS trial in the Northern Territory had been ineffective. In particular, the NDIS was not perceived to have adapted sufficiently to address the specific needs of the Barkly region, and the individualised approach of the NDIS was considered inappropriate when working with First Nations people with disability. The adoption of a model which was more culturally sensitive and appropriate to remote needs and service delivery was recommended (Mavromaras et al. 2018).
The book Culture is Inclusion: A Narrative of Aboriginal and Torres Strait Islander People with Disability explores the experiences of First Nations people with disability across Australia. It presents a world where social inequality and injustices are prevalent, highlighting the challenges that many Australians take for granted. Despite these overwhelming disadvantages, proud and resilient First Nations people continue to embrace their traditional culture of inclusivity. The book emphasises the importance of community-led solutions and suggests that First Nations communities should play a central role in designing services (Avery 2018). The Royal Commission into Violence, Abuse, Neglect, and Exploitation of People with Disability (Disability Royal Commission, Volume 9 First Nations people with disability) also underscored the importance of listening to the voices of First Nations people with disability in shaping policies and services. By valuing personal stories and community perspectives, the Disability Royal Commission Final Report calls for solutions that respect First Nations culture and support self-determination (Royal Commission into Violence‚ Abuse‚ Neglect and Exploitation of People with Disability 2023).
The report Understanding Disability Through the Lens of Aboriginal and Torres Strait Islander People – Challenges and Opportunities (2019) explored how First Nations communities perceive and experience disability. It highlighted cultural, social, and systemic factors, and identified challenges in the National Disability Insurance Scheme (NDIS) implementation, such as an inconsistent application of engagement strategies, insufficient staff training, and misalignment with community-based care preferences. The report used a collaborative approach, engaging First Nations organisations with expertise in supporting individuals with disabilities, along with researchers and policymakers. The report recommended culturally safe, and community-driven disability services, collaborative policy development with First Nations leadership, and investment in culturally appropriate education and training for service providers. It also emphasised the need for participant plans to include family and community contexts, with adequate funding for cultural priorities like ‘return to Country’ (Ferdinand et al. 2019).
Survey and administrative data have shown a higher rate of disability across the life course for First Nations people. Research highlights the characteristics, determinants and effects of disability and can provide insight into the experiences of disability across life stages. For example:
- One study focused on family and cultural inclusion as essential components of healthy child development (Gilroy and Emerson 2016). The research analysed data collected in Wave 4 of Footprints in Time: The Longitudinal Study of Indigenous Children and found that First Nations children with low cognitive ability are at a higher risk of social exclusion than their peers.
- Another study found that frailty, or physiological decline in later life, is substantially higher in First Nations people living in remote areas than in other populations (Hyde et al. 2016).
A study examined both peer-reviewed and grey literature focusing on access to services that increase the likelihood of First Nations people with disability to live independent and socially inclusive lives. It aimed to identify methods to develop workforce capacity to better deliver NDIS services to First Nations people with disabilities in rural and remote areas. The study identified:
- significant access and equity barriers to culturally appropriate disability support services
- the importance of strategies to attract, develop and retain First Nations workers in the First Nations disability workforce
- the importance of culturally safe disability services and community-centred principles
- the importance of strategies such as cultural training for workforce development.
The study also identified the importance of maximising possible benefits from disability sector reforms for First Nations people with disabilities (Gilroy et al. 2017). Since this study, action has been taken to improve access to NDIS services for First Nations people, including through the Aboriginal Disability Liaison Officer (ADLO) program. The ADLO program strives to improve access by highlighting and reducing barriers to the NDIS through culturally safe navigation support and increasing access to and advocating for culturally safe disability services in their local areas. Funded by the National Disability Insurance Agency (NDIA) and working with the National Aboriginal Community Controlled Health Organisation (NACCHO), the program operated in 40 Aboriginal Community Controlled Health Organisations in urban and regional Australia with around 1 to 7 ADLOs in each service. The combined efforts of NACCHO and the ADLOs covered 3 core areas: access and navigation, workforce, and system reform. The program was recently evaluated (NACCHO 2024). The evaluation found that ADLOs provide culturally safe, holistic, and flexible support that clients described as ‘lifesaving’, such as outreach services, setting up appointments with other professionals, assisting with client documentation for NDIS applications and linking to other support services, as well as community awareness raising and building the self-advocacy skills of clients. ADLO workforce capability was a focus of the program which included NDIS-run training as well as a NACCHO-run Community of Practice. The NDIS-run training was seen by ADLOs as essential but not sufficient for developing the knowledge and skillset needed for the ADLO role. However, although effective, the cost of the ADLO program was unsustainable, and the evaluation made recommendations to expand the funding and capacity of the program, as well as developing a career pathway for the ADLOs with appropriate role definition and remuneration.
The Caring about Care report from the Australian National University emphasised the significant unpaid care work performed by First Nations women. It highlights how cultural expectations, and societal norms contribute to the underreporting of this care. The report underscores the need for better recognition and support for these women, acknowledging their vital role in their communities (Klein et al. 2023). The Recognising, valuing and supporting unpaid carers: Inquiry into the recognition of unpaid carers report highlights that First Nations unpaid care is deeply rooted in cultural, kinship and community responsibilities, often described as ‘collective care’. This approach goes beyond individual caregiving to include caring for family, community and Country, and is central to transferring knowledge and sustaining culture. Despite its significance, these informal systems remain largely invisible in mainstream policy and data collection, contributing to under-recognition and limited access to culturally safe supports (House of Representatives Standing Committee on Social Policy and Legal Affairs 2024). Both publications stress the need for greater acknowledgment and support for unpaid carers, particularly among First Nations communities. This recognition is crucial for addressing the systemic undervaluation of their essential work.
Implications
First Nations perspectives on disability are grounded in collective wellbeing, inclusion, and shared responsibilities within kinship and community, whereas Western views tend to frame disability primarily as individual impairment. Culture, Country, kin, and community protect First Nations people with disability from violence, abuse, neglect, and exploitation (Avery 2018; Royal Commission into Violence‚ Abuse‚ Neglect and Exploitation of People with Disability 2023). Although disability prevalence varies across data sources, all indicate a higher disability rate experienced by First Nations people than non-Indigenous Australians. The high levels of disability and earlier onset of core activity restrictions experienced by First Nations people are consistent with the higher levels of disease and injury, and lower access to health services relative to need. There is a clear link between disability and socioeconomic disadvantage (Kavanagh et al. 2013; VicHealth 2012). Lower levels of educational attainment, lower participation in the workforce and lower income are likely to be both the cause and consequence of disability (Biddle 2013). High proportions of First Nations people with disability experiencing difficulties in pursuing education or employment are concerning.
The Australian Government committed to improve the lives of people with disability through the implementation of Australia's Disability Strategy 2021–2031 (the Strategy). This collective commitment by all levels of governments aims to build an inclusive society where people with disability can fully participate as equal members of the community. The Strategy emphasises systemic reforms, community-driven initiatives, and equitable access to services to address existing barriers. It adopts an intersectional approach, recognising that the experiences and impact of disability vary among different cohorts. First Nations people with disability are identified as a priority cohort, with tailored responses to meet their specific needs.
The Royal Commission into Violence, Abuse, Neglect and Exploitation of People with Disability (Disability Royal Commission) Report Volume 9 highlighted that mainstream disability services often fail to reflect First Nations cultural understandings of disability, which are grounded in holistic, community-centred concepts of wellbeing. This disconnect contributes to systemic neglect, underdiagnosis, and exclusion from supports. The report calls for structural reform, including culturally safe service delivery, investment in First Nations community-controlled organisations, and co-designed policies that embed self-determination. This call aligns with Priority Reform Two of the National Agreement on Closing the Gap (building the community-controlled sector). The findings also reinforce the need for tailored trauma-informed approaches that address the intersectional disadvantage experienced by First Nations people with disability across health, education, justice, and child protection systems.
The Disability Sector Strengthening Plan (Disability SSP) under the National Agreement on Closing the Gap was developed in 2022 with input from all levels of government and the community-controlled sector. Governments in partnership with the First Nations disability peak body, the First Peoples Disability Network (FPDN), have progressed targeted priorities under the Disability SSP to develop and strengthen the community-controlled sector to operationalise disability as a cross-cutting outcome for all Closing the Gap socioeconomic targets. In line with Disability Royal Commission Recommendation 9.11, governments have agreed to reviewing the current Disability SSP with an evaluation guide being developed to help inform next steps for all SSPs.
The National Disability Insurance Scheme (NDIS) provides beneficial services and support for First Nations people with disability, however the Disability Royal Commission has found that First Nations people in all areas, but particularly in remote areas, face barriers to accessing and fully participating in the NDIS. The limited availability of service providers in these areas, including culturally appropriate services and a limited First Nations disability workforce, results in accessibility and service gaps and often the need for clients to move off Country (Royal Commission into Violence‚ Abuse‚ Neglect and Exploitation of People with Disability 2023). Aboriginal Community Controlled Health Organisations (ACCHOs) are central to addressing these challenges by delivering holistic, comprehensive, and culturally safe care. ACCHOs have also developed local responses such as the Aboriginal Disability Liaison Officer (ADLO) program, which provides culturally safe navigation and advocacy support to improve NDIS access and outcomes for First Nations people with disability. Sustained and expanded funding arrangements would improve the reach of the ADLO program.
Disability support services are also provided through the Information, Linkages and Capacity Building (ILC) Program. The ILC Program provides information and capacity building supports for all people with disability, their families and carers, regardless of whether they are eligible for the NDIS. This includes First Nations people. The ILC Program seeks to do this by funding grants to eligible organisations to:
- build the capacity of people with disability to participate in their community
- create opportunities for people with disability to participate by creating more inclusive services and communities.
First Nations communities are also identified as one of the priority cohorts in the ILC Program, and funding is provided to a number of organisations targeting First Nations communities.
The Australian Government funds access to individual disability advocacy support services providing people with disability access to effective advocacy support. This support works to promote and protect the rights of people with disability by helping to remove barriers to their full and equal participation in the community. Commonwealth-funded individual disability advocacy is primarily delivered through the National Disability Advocacy Program (NDAP). Since 1 July 2023, the program also includes the Indigenous Community Advocates Pilot which is trialling improved access to advocacy services for First Nations people with disability by placing specialist First Nations advocate positions within select mainstream and First Nations operated services.
For the 2024–25 financial year, 1,625 First Nations clients received assistance through the NDAP and Indigenous Community Advocates Pilot, representing 11.9% of clients assisted through the program. The majority (64.8%) of First Nations clients were aged under 50, and 27.8% were aged between 50–64. A slight majority of First Nations clients (51.9%) identified as female (DHDA 2025b).
Evidence demonstrates the importance of culturally safe, community‑led advocacy. The Disability Royal Commission highlighted that advocacy services designed and operated by First Nations people with disability can play a critical role in providing trusted information and in facilitating access to culturally appropriate supports. The National Disability Advocacy Framework 2023–2025, supports the implementation of Australia’s Disability Strategy 2021–2031, and is a shared commitment to disability advocacy between the Australian, state and territory governments to ensure there is access to advocacy services nation-wide. The Australian Government’s response to the Disability Royal Commission reaffirmed its commitment to prioritise increasing culturally appropriate and accessible advocacy services for First Nations people with disability, within the vehicle of the Framework and associated Disability Advocacy Work Plan.
The NDIS offers funding for long-term, individualised care and support for people with permanent disabilities that significantly impact their communication, mobility, self-care, or self-management. It also funds ‘Partners in the Community’ who assist to connect all people with disability to community services, education, and state and territory support programs. In 2025, the National Disability Insurance Agency (NDIA) partnered with a range of First Nations representatives and organisations to co-design the First Nations Strategy 2025–30 with a First Nations Strategy Working Group. This group included First Nations NDIS participants, providers, community partners (Rumbalara Aboriginal Co-operative and Barengi Gadjin Land Council), the National Aboriginal Community Controlled Health Organisation (NACCHO), and advocates, representing diverse geographies, genders, ages, disabilities, and intersectional experiences. The strategy embeds First Nations knowledge and concepts of disability and wellbeing, aiming to make the NDIS more equitable, culturally safe, community-centred, and coordinated. It reflects priority issues and opportunities to improve outcomes for First Nations people with disability on an equal basis with the broader population.
The Australian Government has committed $1 billion in the 2024–25 Mid-Year Economic and Fiscal Outlook (MYEFO) to enhance NDIS participant experience and sustainability. Key investments include:
- $280 million (from 2025–26) to transition to a consistent, person-centred planning approach
- $503.5 million to improve quality and timely decision-making for NDIS participants
- $143.9 million for the NDIS Quality and Safeguards Commission to maintain regulatory oversight
- $110.4 million to strengthen fraud detection systems
- $4.5 million (2025–26 to 2026–27) to design an early intervention pathway for children under nine.
These investments align with the NDIS Review recommendations to enhance governance, safety, and efficiency within the Scheme (NDIS 2024).
The 2025–26 budget includes additional funding to further strengthen the NDIS and implement the findings of the independent NDIS review, including:
- Funding Increase: A total of $175.4 million over 4 years from 2025–26 has been allocated to safeguard the integrity of the NDIS and support people with disabilities.
- Fraud Prevention: An additional $151 million over 4 years will be dedicated to expanding the Crack Down on Fraud program.
- Workforce Capacity: $17.1 million in 2025–26 will be used to maintain the NDIA’s payment integrity workforce.
- Participant Support: An additional $7.3 million in 2025–26 will be provided to advocacy organisations through the NDIS Appeals Program.
These measures aim to ensure the NDIS remains strong, fair, and sustainable (DHDA 2025a).
The report Implementing disability policy reform: challenges and opportunities (2024) highlights opportunities to improve disability support for First Nations communities by addressing systemic barriers through the NDIS reforms. These reforms carry risks if not implemented carefully and needs active engagement with First Nations stakeholders to ensure their voices are represented and ensure momentum for the reforms continues (Dillon 2024).
The Royal Commission into Aged Care Quality and Safety, and the Disability Royal Commission, found that First Nations people:
- prefer services delivered by First Nations providers
- find mainstream services geographically and culturally inaccessible and hard to navigate
- often received health care at a later stage, and potentially in acute hospital settings when the issues became more critical.
Inadequate equipment, training, facilities, and personnel can also hinder access to care. Diagnostic overshadowing, where symptoms are attributed to disability rather than a secondary illness, is a concern. Transport is another barrier, especially for older people and those with disabilities.
Responsive, quality, and accessible health care must align with community needs and priorities, involving representative bodies like the NACCHO the FPDN or the NDIA Independent Advisory Council (IAC) First Nations Reference Group. Innovative, culturally safe disability service models should be investigated, co-designed and implemented flexibly to respond to local need and to increase access. All health services, including Aboriginal Community Controlled Health Services, play a critical role in delivering culturally safe care and should be supported to maintain appropriate infrastructure, equipment, and workforce capability. Strengthening partnerships between First Nations health organisations, aged care, and disability services will support better integration and holistic care.
The National Aboriginal and Torres Strait Islander Health Plan 2021–2031 recognises First Nations people with disability as a priority group and commits to delivering culturally safe, accessible, and inclusive health services. It emphasises disability-led approaches and prioritises the voices and lived experiences of First Nations people with disability in policy and service design. The Health Plan supports self-determination and trauma-informed engagement, encouraging flexible, culturally appropriate participation and the use of interpreters, including Auslan and First Nations languages. It also highlights the role of ACCHOs in delivering disability-specific health supports and calls for the development of disability-inclusive cultural safety standards across health, justice, and early childhood sectors.
The Health Plan aligns with the National Aboriginal and Torres Strait Islander Health Workforce Strategic Framework and Implementation Plan 2021–2031 (The National Workforce Plan), aiming to grow the First Nations health workforce across all health roles (both clinical and non-clinical) and locations. Workforces must be adequately trained and be able to provide accessible and person-centred care to people with a disability. This includes responding to the systemic social determinant factors that impact health and wellbeing. The National Workforce Plan’s implementation strategies are intended to support participation in the workforce for all First Nations people, including people with a disability.
References
-
ABS (Australian Bureau of Statistics) (2016) National Aboriginal and Torres Strait Islander Social Survey 2014–15, ABS, Australian Government.
-
ABS (2023) Australia – 2021 census community profiles, ABS website.
-
ABS (2025) ABS Sources of Disability Statistics, 2018 – 2023, Australian Bureau of Statistics website, accessed 28 November 2025.
-
ABS and Avery S (2025a) Aboriginal and Torres Strait Islander peoples with disability, 2022 [data set], 2022 Survey Disability Ageing and Carers, ABS website.
-
ABS and Avery S (2025b) Aboriginal and Torres Strait Islander peoples with disability, 2022, ABS, Australian Government.
-
AIHW (Australian Institute of Health and Welfare) (2020) Disability support services: services provided under the National Disability Agreement 2018–19, AIHW, Australian Government.
-
AIHW (2024) People with disability in Australia, AIHW, Australian Government.
-
Avery S (2018) Culture is inclusion: a narrative of Aboriginal and Torres Strait Islander people with disability, First Peoples Disability Network, Sydney.
-
Biddle N (2013) Paper 11: Income, CAEPR Indigenous Population Project 2011 Census Papers, Centre for Aboriginal Economic Policy Research, Australian National University.
-
D’Aprano A, McRae K, Dayton S, Lloyd-Johnsen C and Gilroy J (2024) 'A scoping review of early childhood support for Aboriginal and Torres Strait Islander children living with a disability in regional, rural and remote settings', Australian Journal of Rural Health, 32(5):890–905, doi:10.1111/ajr.13164.
-
Daniels-Mayes S (2023) 'Researching Indigenous people living with a disability: the urgent need for an intersectional and decolonising approach (BlakAbility)', First Nations Health and Wellbeing – The Lowitja Journal, 1:100004, doi:10.1016/j.fnhli.2023.100004.
-
DHDA (Department of Health, Disability and Ageing) (2025a) Budget 2025–26: strengthening the National Disability Insurance Scheme, DHDA, Australian Government.
-
DHDA (2025b) National Disability Advocacy Program (NDAP) program performance data, internal analysis obtained via the Data Exchange in September 2025.
-
Dillon M (2024) Implementing disability policy reform: challenges and opportunities, Centre for Indigenous Policy Research, Australian National University.
-
Ferdinand A, Massey L, Cullen J, Temple J, Chamravi D, Meiselbach K, Paradies Y, Baynam G, Savarirayan R and Kelaher M (2019) Understanding disability through the lens of Aboriginal and Torres Strait Islander people – challenges and opportunities, Centre for Health Policy, University of Melbourne.
-
Gilroy J, Dew A, Barton R, Ryall L, Lincoln M, Taylor K, Jensen H, Flood V and McRae K (2021) 'Environmental and systemic challenges to delivering services for Aboriginal adults with a disability in Central Australia', Disability and Rehabilitation, 43(20):2919–2929, doi:10.1080/09638288.2020.1725654.
-
Gilroy J, Dew A, Lincoln M and Hines M (2017) 'Need for an Australian Indigenous disability workforce strategy: review of the literature', Disability and Rehabilitation, 39(16):1664–1673, doi:10.1080/09638288.2016.1201151.
-
Gilroy J and Emerson E (2016) 'Australian indigenous children with low cognitive ability: family and cultural participation', Research in Developmental Disabilities, 56:117–127.
-
House of Representatives Standing Committee on Social Policy and Legal Affairs (2024) Recognising, valuing and supporting unpaid carers: inquiry into the recognition of unpaid carers, Parliament of Australia.
-
Hyde Z, Flicker L, Smith K, Atkinson D, Fenner S, Skeaf L, Malay R and Giudice DL (2016) 'Prevalence and incidence of frailty in Aboriginal Australians, and associations with mortality and disability', Maturitas, 87:89–94.
-
James MH, Prokopiv V, Barbagallo MS, Porter JE, Johnson N, Jones J and Smitherson T (2023) 'Indigenous experiences and underutilisation of disability support services in Australia: a qualitative meta-synthesis', Disability and Rehabilitation:1–12, doi:10.1080/09638288.2023.2194681.
-
Kavanagh AM, Krnjacki L, Beer A, Lamontagne AD and Bentley R (2013) 'Time trends in socio-economic inequalities for women and men with disabilities in Australia: evidence of persisting inequalities', International Journal for Equity in Health, 12:73, doi:10.1186/1475-9276-12-73.
-
Klein E, Hunt J, Staines Z, Dinku Y, Brown C, Glynn-Braun K, Yap M, Murray M and Williamson B (2023) Caring about care, Centre for Aboriginal Economic Policy Research, Australian National University.
-
Mavromaras K, Moskos M, Mahuteau S and Isherwood L (2018) Evaluation of the NDIS: final report, report to the Australian Government Department of Social Services, National Institute of Labour Studies, Flinders University.
-
NACCHO (National Aboriginal Community Controlled Health Organisation) (2024) ADLO program evaluation, NACCHO.
-
NDIS (National Disability Insurance Scheme) (2016) Rural and Remote Strategy, 2016–2019, NDIA, Australian Government.
-
NDIS (2019) Aboriginal and Torres Strait Islander participants 30 June 2019, NDIA, Australian Government.
-
NDIS (17 December 2024) Putting participants back at the centre of the NDIS [media release], NDIA, Australian Government.
-
NDIS (2025a) First Nations participants [data set], NDIA website.
-
NDIS (2025b) Participant numbers and plan budgets [data set], NDIA website.
-
NDIS (2025c) Q4 2024–25, NDIS Quarterly Report to the Disability Ministers, NDIA, Australian Government.
-
People with Disability Australia (2025) Social model of disability, PWDA website, accessed 20 October 2025.
-
Royal Commission into Violence‚ Abuse‚ Neglect and Exploitation of People with Disability (2023) Final report volume 9: First Nations people with disability, Commonwealth of Australia.
-
Trounson J, Gibbs J, Kostrz K, McDonald R and Peters A (2022) 'A systematic literature review of Aboriginal and Torres Strait Islander engagement with disability services', Disability & Society, 37(6):891–915, doi:10.1080/09687599.2020.1862640.
-
VicHealth (2012) Disability and health inequalities in Australia research summary: addressing the social and economic determinants of mental and physical health, VicHealth.

