Key messages
Why is it important?
Oral health is essential to overall wellbeing yet remains an area of persistent inequity for Aboriginal and Torres Strait Islander (First Nations) people. Poor oral health contributes significantly to preventable hospitalisations and is linked to chronic diseases such as diabetes and cardiovascular disease. Despite being largely preventable through good oral hygiene, fluoridation, and early dental care, oral diseases remain widespread due to social, economic and environmental disadvantage, with rural and remote communities facing challenges in accessing services. For First Nations people, these inequities are compounded by racism, affordability barriers, and a lack of culturally safe care. Improving oral health outcomes therefore requires early prevention, culturally competent service delivery, and integration of oral health within broader health and social systems.
Data findings
-
In 2022, oral disorders accounted for 2.0% (6,370 out of 317,083 total DALY) of the total disease burden for First Nations people, and 4.0% (6,362 out of 158,693 total YLD) of the non-fatal burden (years lived with disability).
-
In 2022–23, 58% (161,100) of First Nations children aged 2–14 had a dental consultation in the last 12 months based on survey data (with adults responding on behalf of the children), while 20% (55,700) had never attended a dental practice. The attendance rate was much lower in remote areas.
-
An estimated 4.3% (27,700) of First Nations people aged 15 and over in 2022–23 had complete tooth loss and 45% (294,000) had lost at least one tooth (excluding wisdom teeth), based on self-reported survey data.
-
In 2022–23, an estimated 21% (201,500) of First Nations people aged 2 and over did not go to a dentist when they needed to in the previous 12 months (based on self-reported survey data). The leading reasons reported were cost (45%; 91,600); followed by being too busy (24%; 47,400); disliked service or professional or felt embarrassed or afraid (23%; 45,600); or waiting time too long or an appointment not available at the time required (21%; 41,500).
-
In 2022–23, among First Nations people aged 2 and over living in non-remote areas who had last received non-urgent dental treatment at a public dental service, 42% (111,000) waited less than a week (including those who did not wait at all). Conversely, 15% (40,000) waited 3 months or more.
-
In 2024, 61,371 First Nations children received dental services under the Child Dental Benefits Schedule, representing 23% of those eligible for these services. In comparison, 36% of eligible non-Indigenous children had received these services.
-
Between July 2021 and June 2023, after adjusting for differences in the age structure between the two populations, First Nations people were hospitalised for diseases of the oral cavity, salivary glands and jaws at a lower rate than non-Indigenous people – 5.8 and 7.0 hospitalisations per 1,000 population respectively.
-
Between July 2021 and June 2023, First Nations children aged 0–4 were hospitalised for dental conditions at 1.4 times the rate of non-Indigenous children.
-
Between July 2021 and June 2023, among First Nations people, children aged 5–9 had the highest rate of hospitalisation for dental conditions involving general anaesthesia (14.5 per 1,000), followed by those aged 0–4 (7.3 per 1,000).
Research and evaluation findings
-
First Nations children experience twice the rate of dental caries as non-Indigenous children, with many families deterred from seeking care due to judgmental attitudes and a focus on individual treatment over preventive measures.
-
Oral health disparities are linked to socioeconomic disadvantage, affordability and accessibility and limited culturally safe services.
-
Structural racism and systemic barriers deter First Nations people from seeking dental care. Building the cultural competency of oral health care staff can build staff confidence in delivering oral health care and build trust with First Nations clients.
-
Community-driven, preventive oral health programs delivered through Aboriginal Community Controlled Health Services are effective in reaching remote populations but remain limited by funding and workforce shortages.
-
Researchers and stakeholders see the potential benefits of integration of oral health into primary care, particularly in rural and remote locations but there are hurdles to overcome.
-
A study of 29 Aboriginal Community Controlled Health Services (ACCHSs) in New South Wales found that while 56% provided oral health services, 79% reported unmet community needs due to funding and workforce shortages. Despite these challenges, ACCHSs demonstrated strengths in delivering culturally appropriate and community-driven oral health care, integrating these services with broader health initiatives tailored to local needs.
-
An economic evaluation of the Midwifery Initiated Oral Health Program in Australia found that providing oral health education, assessment, and referral (by midwives alone) was a cost-effective, low-cost intervention compared to current practice. Combining interventions by midwives and dentists was also cost-effective when benefits were assessed over a longer period.
Implications
Persistent inequities in oral health outcomes for First Nations people demonstrate the need for structural reform, culturally safe models of care, and equitable access to preventive services. National strategies — including the forthcoming National Oral Health Plan 2025–2034, the National Aboriginal and Torres Strait Islander Health Plan 2021-2031 and the new Northern Territory Partnership Agreement with the Northern Territory government and Aboriginal Peak Organisations Northern Territory (APO NT) — emphasise community leadership, co-design and integration of oral health within broader health systems. Ongoing challenges such as affordability, geographic isolation and workforce shortages continue to restrict access, particularly for children, despite programs like the Child Dental Benefits Schedule and state-funded dental agreements. Strengthening Aboriginal Community Controlled Health Organisations (ACCHOs) as key providers, expanding the role of Aboriginal Health Practitioners, and embedding cultural safety across dental services are central to achieving long-term improvements. Sustainable progress will depend on investment in prevention, workforce development, and community-led approaches that address the social and structural determinants driving poor oral health.
Why is it important?
Oral health is a fundamental component of overall health, wellbeing and quality of life, enabling individuals to eat, speak and socialise without discomfort or embarrassment. Poor oral health places a significant burden on individuals, families and the health-care system, ranking as one of the leading reasons for acute potentially preventable hospitalisations. Untreated tooth decay affects one-third of Australian adults and one-quarter of children aged 5–10, while one-third of adults experience moderate or severe gum disease. Inequities in oral health outcomes are influenced by social, economic and environmental factors, particularly for people living in rural and remote areas, who face higher rates of oral diseases and reduced access to dental care due to workforce shortages (NOHA 2023). While oral health inequities are a concern across various populations, they are particularly pronounced among Aboriginal and Torres Strait Islander (First Nations) people, who face additional barriers to care and prevention.
Oral health refers to the health of tissues of the mouth: muscle, bone, teeth and gums. The two most frequently occurring oral diseases are tooth decay (termed ‘caries’) and gum (periodontal) disease. If not treated in a timely manner, these can cause discomfort and tooth loss, impacting a person's ability to eat, speak, and socialise without discomfort or embarrassment (Williams et al. 2011). Oral diseases can intensify other chronic diseases (Jamieson et al. 2010) and have been found to be associated with cardiovascular diseases (Ylöstalo et al. 2006), diabetes (Taylor and Borgnakke 2008), stroke (Joshipura et al. 2003) and pre-term low birthweight (Roberts-Thomson et al. 2008; Williams et al. 2011; Xiong et al. 2006). There is evidence of a two-way relationship between periodontitis and diabetes. The risk of developing periodontitis is greater among people with diabetes particularly when blood glucose levels are not well-managed. Periodontitis may also negatively affect blood glucose levels potentially increasing the risk of developing diabetes (Diabetes Australia 2025).
First Nations people experience disproportionately poor oral health, including higher rates of untreated dental disease and multiple caries than non-Indigenous Australians, and are less likely to receive preventive dental care. Accessibility challenges, high costs, and a lack of cultural awareness in some services contribute to unfavourable dental visiting patterns. Poor oral health impacts overall health and quality of life, with significant long-term effects, particularly for children (AIHW 2024b).
Tooth decay can be largely prevented by diet (for example reducing intake of processed sugary foods/drinks), fluoridation of water supplies (Chondur et al. 2024; Lalloo et al. 2015), appropriate use of fluoridated toothpaste, good oral hygiene and regular dental check-ups (Sicca et al. 2016). Smoking, vaping, alcohol and substance use, stress, obesity, diabetes, osteoporosis, low dietary calcium and vitamin D, and genetics are also risk factors for periodontal disease (such as gingivitis and periodontitis) (Iacob et al. 2024; Quaranta et al. 2022). Lower levels of education and income and sub-standard living conditions are associated with oral diseases (Lalloo et al. 2016). In addition to oral hygiene and dental care, tooth loss is associated with increased age and accidents and injuries (Jamieson et al. 2010; Williams et al. 2011).
Racism and structural barriers profoundly impact the oral health of First Nations people, resulting in poor access to culturally sensitive dental care and exacerbating oral health inequities. Institutional and interpersonal racism contribute significantly to negative dental experiences, deterring First Nations patients from seeking or continuing treatment and thus worsening oral health outcomes. These inequities are further compounded by geographical isolation, shortages of oral health professionals in rural and remote areas, high out-of-pocket costs for dental care, and limited availability of preventive measures for some communities such as water fluoridation. Addressing these challenges requires a multi-faceted approach: culturally competent dental workforce training, improving service accessibility through outreach and mobile clinics, and integrating oral health care within broader public health strategies (Genco and Borgnakke 2013; Hedges et al. 2021; Loos and Van Dyke 2020; Watt et al. 2019).
The National Aboriginal and Torres Strait Islander Health Plan 2021–2031 (the Health Plan) continues to guide actions to ensure First Nations people can live long and healthy lives. Co-designed in genuine partnership with First Nations health leaders, the Health Plan identifies priority areas for action and reform. It is the first national health document to address the health outcomes and Priority Reforms of the National Agreement on Closing the Gap.
‘Priority Five’ focuses on early intervention approaches that are accessible to First Nations people and provide timely, high quality, effective, culturally safe and responsive care. One objective specifically addresses oral health:
- Objective 5.2. Deliver activities to improve oral health, particularly for children
The Health Plan is discussed further in the Implications section of this measure.
Burden of disease
Disability-Adjusted Life Years (DALY) measure the total years of healthy life lost in a population by combining years of life lost (YLL; the fatal burden) due to premature death and years lived with disability (YLD; the non-fatal burden) due to illness or injury. One DALY is equivalent to the loss of one year of healthy life (AIHW 2026).
In 2022, oral disorders accounted for 2.0% (6,370 out of 317,083 total DALY) of the total disease burden for First Nations people, and 4.0% (6,362 out of 158,693 total YLD) of the non-fatal burden (years lived with disability). First Nations males experienced slightly more of the total burden due to oral disorders than First Nations females (53% compared with 47%, respectively).
Dental caries was the leading cause of oral disease burden among First Nations people, accounting for almost two-thirds (61%; 3,902 out of 6,370 total DALY due to oral disorders) of the burden due to oral disorders. This was followed by periodontal disease (21%; 1,364 DALY) and severe tooth loss (17%; 1,080 DALY) (AIHW 2026).
Data findings
Oral health based on self-reported data
Data on oral health and dental consultations are available from the 2022–23 National Aboriginal and Torres Strait Islander Health Survey (NATSIHS), based on self-report (for children 2 to 14, an adult was asked to respond on their behalf).
Based on these data, in 2022–23, 83% (772,100) of First Nations people aged 2 and over brushed their teeth daily, including 47% (431,400) brushing their teeth twice a day. An estimated 45% (427,600) of First Nations people aged 2 and over had seen a dentist in the last 12 months and 11% (100,500) had never seen a health professional about teeth (Table D1.11.11).
Of First Nations people aged 2 and over who had previously seen a dentist, 48% (403,100) had last visited a private dental clinic, 25% (208,300) a government dental clinic, 11% (96,400) a school dental clinic, and 13% (112,900) a dentist at an Aboriginal Medical Service. Among First Nations people living in non-remote areas who had last received non-urgent dental treatment at a public dental service, 42% (111,000) waited less than a week (including did not wait at all). Conversely, 15% (40,000) waited 3 months or more (Table D1.11.11).
An estimated 21% (201,500) of First Nations people aged 2 and over did not go to a dentist when they needed to in the previous 12 months, based on data from the 2022–23 NATSIHS. Reasons included: cost (45%; 91,600), too busy (24%; 47,400), disliking service or professional, or feeling embarrassed or afraid (23%; 45,600) and waiting time being too long or service being not available at time required (21%; 41,500) (Table D3.08.3, Figure 1.11.1).
Figure 1.11.1: First Nations people aged 2 and over who needed to go to a dentist in the last 12 months but did not, by reason, 2022–23
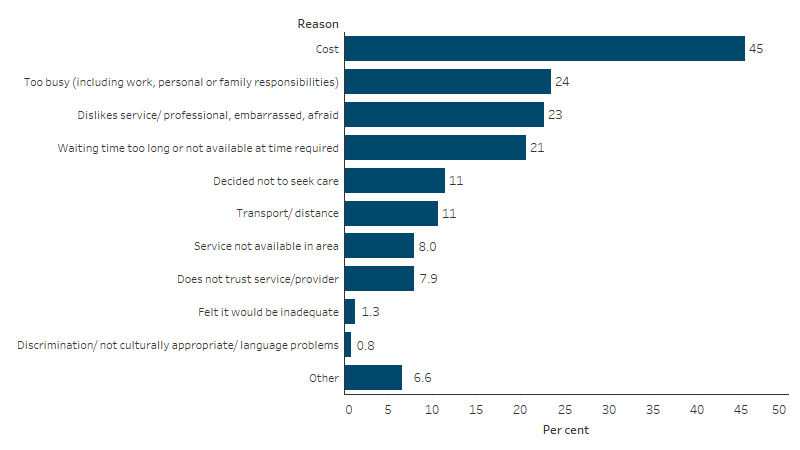
Source: Table D3.08.3. AIHW and ABS analysis of National Aboriginal and Torres Strait Islander Health Survey 2022–23.
In 2022–23, an estimated 82% (229,300) of First Nations children aged 2–14 brushed their teeth daily – 84% (203,400) in non-remote areas and 70% (25,400) in remote areas. About 58% (161,100) had their last dentist or dental professional appointment within the previous 12 months (60% (144,300) in non-remote areas and 47% (17,100) in remote areas), while 20% (55,700) had never seen a health professional about their teeth (19% (45,400) in non-remote areas and 29% (10,400) in remote areas) (Table D1.11.29).
Based on the 2022–23 survey, of around 223,400 First Nations children aged 2–14 who had seen a dentist, 30% had attended a school dental clinic for their most recent consultation, 43% attended a private clinic (including specialists), 16% attended a government dental clinic and 8.9% attended a dentist at an Aboriginal Medical Service. Of around 25,800 First Nations children living in remote areas (Remote and Very remote areas combined) who had seen a dentist, 40% went to a school dental clinic, compared with 28% of those in non-remote areas (Major cities, Inner regional and Outer regional areas combined) (Table D1.11.29, Figure 1.11.2).
Figure 1.11.2: Place of last dental consultation among First Nations children aged 2–14 who had attended a dental practice, by remoteness, 2022–23
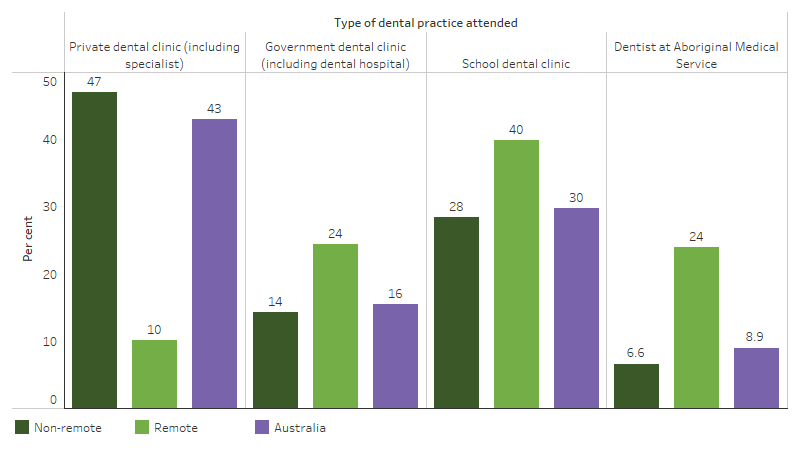
Note: Denominator for the percentages is the number of children 2–14 who had attended a dental practice (in non-remote areas, remote areas, or Australia, as applicable).
Source: Table D1.11.29. AIHW and ABS analysis of National Aboriginal and Torres Strait Islander Health Survey 2022–23.
In 2022–23, an estimated 5.8% of First Nations children aged 2–14 needed to go to the dentist in the past 12 months but did not (Table D3.08.3).
Note – The National Aboriginal and Torres Strait Islander Social Survey (NATSISS) which collects detailed information on the social and cultural experiences of First Nations people has not been conducted since 2014–15. The following data therefore cannot be updated.
Based on data from the 2014–15 NATSISS, 28% of First Nations children aged under 15 had teeth or gum problems in 2014–15 (Table D1.11.1). The most common types of problems reported were cavities or dental decay (12%), fillings due to dental decay (11%), needing braces/plate/retainer (6%) and having teeth pulled out due to dental decay (5%) (Table D1.11.3, Figure 1.11.3).
Figure 1.11.3: Proportion of First Nations children aged 0–14 with reported teeth or gum problems, by type of dental or gum problem, 2014–15
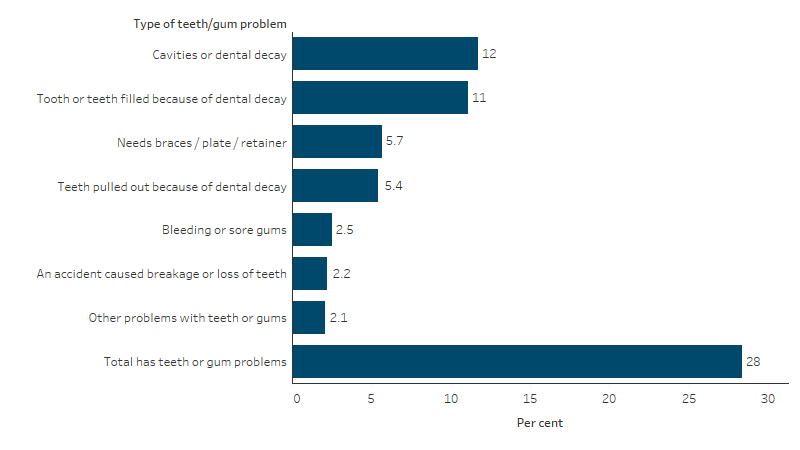
Source: D1.11.3. AIHW and ABS analysis of National Aboriginal and Torres Strait Islander Social Survey 2014–15.
Based on survey estimates, of around 63,400 First Nations children with teeth or gum problems, 56% had experienced the problem for at least 12 months. This was more common for First Nations children living in non-remote areas (58% of those with teeth or gum problems) compared with remote areas (45%) (Table D1.11.5). Of around 63,000 First Nations children with teeth or gum problems, 29% of had their last dental check less than 3 months ago and 8% had never been to a dentist (Table D1.11.6).
Across age groups, the proportion of First Nations children with reported teeth or gum problems was 39% for those aged 10–14 (an estimated 28,900 children), 33% for those aged 5–9 (26,800 children), and 11% for those aged 0–4 (7,400 children) (Table D1.11.4).
Child Dental Benefits Schedule services
In 2024, 61,371 First Nations children aged 0-17 received dental services under the Child Dental Benefits Schedule, representing 23% of those eligible for these services. In comparison, 36% of eligible non-Indigenous children had received these services (Data provided by Department of Health, Disability and Ageing).
Child dental health services in the Northern Territory
Data was collected under successive national agreements that supported the delivery of oral health services for First Nations children in the Northern Territory. The Child Health Check Initiative program (2007 to mid-2012) was replaced by the Stronger Futures in the Northern Territory (SFNT) program, introduced in mid-2012, which was then was replaced by the Northern Territory Remote Aboriginal Investment Oral Health Program (NTRAI OHP) in July 2015. Across these programs, First Nations children aged 0–15 received oral health services, providing a consistent dataset despite changes in program structures. A new Partnership Agreement began in 2025 (see Implications section for more information).
Between August 2007 and June 2012, 7,403 First Nations children received dental services under the Child Health Check Initiative Program and 46% of those children were treated for at least one dental problem. Thirty-eight per cent of First Nations children who received dental services under the program were treated for untreated tooth decay (Table D1.11.25).
Between July 2012 and December 2023, 23,147 First Nations children received 50,960 clinical services. The numbers fluctuated over time but the number in 2023 was higher than all other years except for 2022. The proportion of dental service recipients with tooth decay decreased for most age groups between March 2009 and December 2023, although there has been increases from 2022 to 2023 in most age groups. The largest decrease was for First Nations children aged 1–3 years combined (from 73% to 45%), followed by those aged 8 years (from 93% to 84%) (AIHW 2025b).
Between August 2007 and December 2023, 54,966 dental services were provided to 18,139 First Nations children under the National Partnership Agreement on the Northern Territory Remote Aboriginal Investment (NTRAI). Over this period, 89% of First Nations children who had a dental service had two or more dental checks (Table D1.11.22). Over half (51%) of First Nations children who received a dental service were aged 6–11 (Table D1.11.23).
Tooth loss
In the 2022–23 NATSIHS, self-reported data was collected on tooth loss. Based on this, an estimated 4.3% (27,700) of First Nations people aged 15 and over had complete tooth loss, and a further 45% (294,000) had lost at least one tooth (excluding wisdom teeth) (Table D1.11.7, Figure 1.11.4).
Figure 1.11.4: Status of tooth loss of First Nations people aged 15 and over, by age, 2022–23
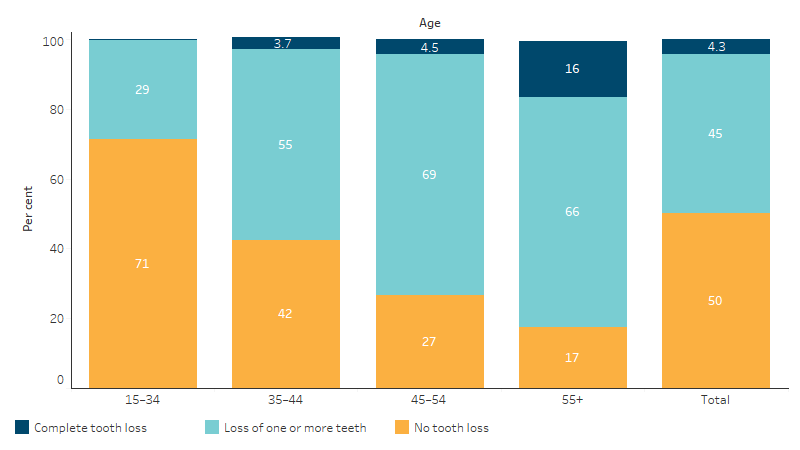
Source: Table D1.11.7. AIHW and ABS analysis of National Aboriginal and Torres Strait Islander Health Survey 2022–23.
In 2022–23, by age group, the rate of complete tooth loss was highest for First Nations people aged 55 and over, with 16% (19,800) having complete tooth lost. The proportion of First Nations people aged 55 and over with complete tooth loss was higher in non-remote than remote areas – 17% (17,800 people) in non-remote areas, compared with 13% (2,300 people) in remote areas, although the difference was not statistically significant (Table D1.11.10).
In 2022–23, the proportion of First Nations people with complete tooth loss was higher for those with: three or more chronic conditions (11.3 times those with no conditions); a self-assessed health status of fair or poor (6.4 times of those with an excellent/very good/good status); a disability (5.6 times those with no disability); Year 9 or below as the highest year of schooling (4.7 times those with Year 12); heart or cardiovascular (circulatory) problems (3.6 times those without heart/cardiovascular problems); and reported diabetes or high blood sugar levels (3.5 times those without diabetes or high blood sugar levels) (Table D1.11.8, Table D1.11.9).
Hospitalisations for dental and oral problems
Between July 2021 and June 2023, there were 13,277 hospitalisations among First Nations people due to diseases of the oral cavity, salivary glands and jaws. This a rate of 6.6 hospitalisations per 1,000 population and accounts for 1.8% of all hospitalisations of First Nations people (excluding dialysis) (Table D1.02.1, Table D1.11.21). First Nations children aged 0–4, 5–14 and 15–24 had the highest rates of hospitalisation, at 7.5, 9.7 and 7.5 per 1,000 population respectively, with rates ranging between 3.0 and 6.3 per 1,000 population in older age groups.
After adjusting for differences in the age structure between the two populations, First Nations people were hospitalised for diseases of the oral cavity, salivary glands and jaws at a lower rate than non-Indigenous people – 5.8 hospitalisations per 1,000 population compared with 7.0 hospitalisations per 1,000 population respectively (Table D1.11.21).
First Nations children aged 0–4 were hospitalised for dental conditions at 1.4 times the rate of non-Indigenous children. Conversely, among people aged 5–14, 15–24, 55–64 and 65 and over, the rates of hospitalisation due to dental problems were lower for First Nations people than for non-Indigenous Australians (Table D1.11.21, Figure 1.11.5).
Figure 1.11.5: Age-specific hospitalisation rates for a principal diagnosis of dental and oral problems, by Indigenous status and age, Australia, July 2021 to June 2023
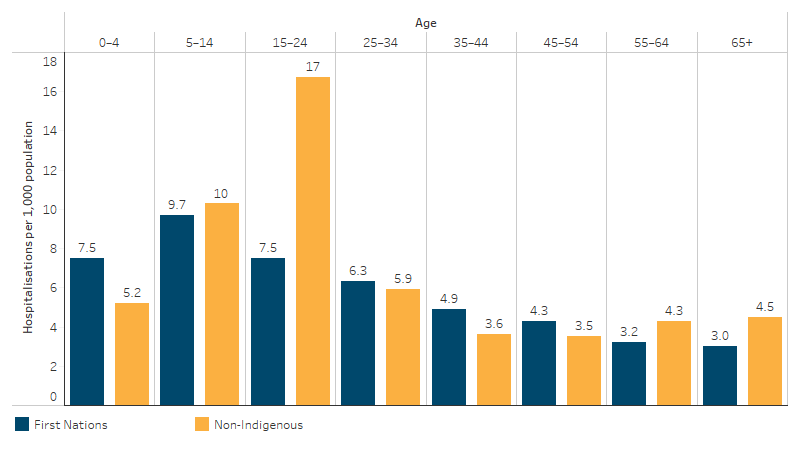 Note: Principal diagnosis of dental problems includes ICD-10-AM codes K00-K14.
Note: Principal diagnosis of dental problems includes ICD-10-AM codes K00-K14.
Source: Table D1.11.21. AIHW analysis of National Hospital Morbidity Database.
The leading cause of hospitalisation for dental and oral health problems between July 2021 and June 2023 among First Nations people was dental caries (5,120 hospitalisations, 2.6 per 1,000 population), followed by embedded and impacted teeth (2,779 hospitalisations, 1.4 per 1,000 population).
First Nations people were 2.7, 2.2 and 1.4 times as likely as non-Indigenous people to be hospitalised for stomatitis and related lesions, diseases of the pulp and periapical tissues and diseases of salivary glands respectively. Diseases of the pulp and periapical tissues also had the largest absolute gap between First Nations people and non-Indigenous Australians, with a rate difference of 0.6. However, First Nations people were hospitalised less for disorders of tooth development and eruption, embedded and impacted teeth and dentofacial anomalies than non-Indigenous Australians (Table D1.11.32).
Dental care under general anaesthetic carries an additional risk and is resource intensive, however it may be preferable depending on the complexity of the procedure and characteristics of the patient. Among First Nations people, there were 10,856 hospitalisations for dental procedures that involved general anaesthesia between July 2021 and June 2023 – a rate of 5.4 per 1,000 population (Table D1.11.28).
The highest rates were for First Nations children aged 5–9 (14.5 per 1,000) followed by those aged 0–4 (7.3 per 1,000). Rates of hospitalisation for dental procedures involving general anaesthesia were higher for First Nations children than non-Indigenous children aged 0–4 and 5–9 (1.4 and 1.2 times the rate, respectively). The rate of hospitalisation for dental procedures involving general anaesthesia was considerably lower for First Nations people aged 15–24 compared with non-Indigenous people (6.5 compared with 15.4 per 1,000, rate ratio of 0.4). Rates of hospitalisation for dental procedures involving general anaesthesia were either similar or higher for non-Indigenous people in older age groups (Table D1.11.28).
Data on hospitalisation due to periodontal disease indicates that, overall, the rates were similar for First Nations people and non-Indigenous Australians (Table D1.11.31). However, this varied by age group. In every age group except those aged 55–64 and 65 and over, the rate of hospitalisation due to periodontal disease was higher for First Nations people than non-Indigenous Australians. First Nations people aged 35–44 were 3.4 times as likely to be hospitalised for periodontal disease as non-Indigenous Australians (Table D1.11.31).
National Child Oral Health Study
The 2025–26 National Child Oral Health Study (NCOHS) is underway with findings expected to be released in 2027. The 2012–14 National Child Oral Health Study (NCOHS) provides a snapshot of oral health in the total child population in Australia. Data are collected nationally from children aged 5–14 using interviews and standardised dental examinations. A total of 24,664 children from across Australia participated in the study and 5.5% of survey respondents identified as Aboriginal and/or Torres Strait Islander (Do and Spencer 2016).
The study found that 59% of First Nations children aged 5–8 had decayed, missing or filled tooth surfaces in their primary (or baby) teeth and 46% of First Nations children aged 9–14 had decayed, missing or filled tooth surfaces in their permanent teeth.
First Nations children aged 5–8 had an average number of 6.3 decayed, missing or filled tooth surfaces in their primary teeth. First Nations children aged 9–14 had an average of 1.8 decayed, missing or filled tooth surfaces in their permanent teeth (Figure 1.11.6).
Figure 1.11.6: Average number of decayed, missing or filled tooth surfaces among First Nations children in primary (baby teeth) or permanent teeth, children aged 5–8 and 9–14, 2012–14
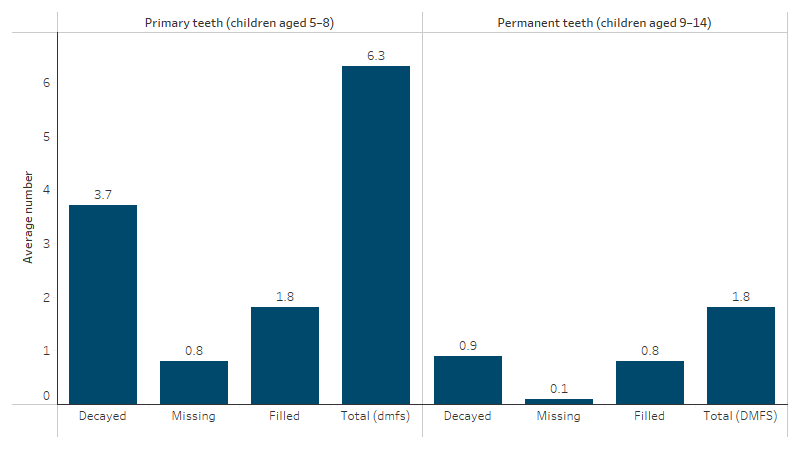
Source: 2012–14 National Child Oral Health Study (Do and Spencer 2016).
First Nations children aged 9–14 in Remote and very remote areas had 4.3 times the number of untreated decayed surfaces in their permanent teeth compared with First Nations children in Major cities (1.7 compared with 0.4 surfaces).
First Nations children aged 5–8 who last visited the dentist for a dental problem had an average number of 13 decayed, missing or filled tooth surfaces in their primary teeth, whereas those who last visited for a check-up had an average of 4.6 decayed, missing or filled tooth surfaces.
The proportion of First Nations children with decayed, missing or filled tooth surfaces in their primary teeth was 1.6 and 1.5 times as high as that of non-Indigenous children in the 5–6 and 7–8 age groups, respectively. For permanent teeth, this was 1.9 times as high for First Nations children as non-Indigenous children in the 9–11 age group, and 1.4 times as high for First Nations children as non-Indigenous children in the 12–14 age group (Figure 1.11.7).
First Nations children had higher levels of oral disease and had lower rates of favourable dental visiting pattern than non-Indigenous children. Around 45% of First Nations children aged 5–14 attended their first dental visit before the age of 5 and 75% last visited a dental provider within the last 12 months (58% and 82% for non-Indigenous children, respectively). Regular dental visits are recommended, however, 31% of First Nations children and 20% of non-Indigenous children had an irregular dental visiting pattern.
Around 68% of First Nations children aged 5–14 last visited their dental provider for a check-up (rather than for a dental problem), while this was 81% for non-Indigenous children. Almost one-quarter (23%) of First Nations children had their most recent dental visit at a private practice (58% for non-Indigenous children) and the remaining proportion had their last visit at public dental services (Do and Spencer 2016).
Figure 1.11.7: Percentage of children with experience of decayed, missing or filled tooth surfaces in primary (baby teeth) or permanent teeth, by Indigenous status and age group, 2012–14
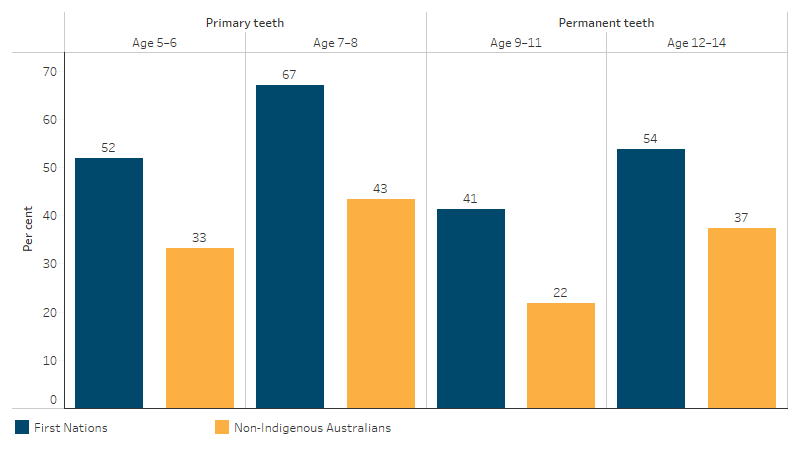
Source: 2012–14 National Child Oral Health Study (Do and Spencer 2016).
Research and evaluation findings
Poor oral health is strongly associated with low socioeconomic status. Research has shown that adults who are socially disadvantaged or on a low income have more than double the rate of poor oral health than those on higher incomes, including higher rates of untreated decay (Brennan et al. 2019).
Consistent with these socioeconomic gradients, national survey data indicate that unmet need for dental care remains widespread among First Nations people. Analysis of the 2022–23 National Aboriginal and Torres Strait Islander Health Survey (NATSIHS) shows that 1 in 5 (21%) of First Nations people aged 2 years and over reported there was a time in the previous 12 months when they needed dental care but did not receive it. This finding is consistent with earlier AIHW analysis using the 2018–19 NATSIHS, which similarly identified dental care as one of the primary health services with the highest levels of unmet need among First Nations people (AIHW 2024a, 2025a).
Unmet need varied markedly by age, with relatively low levels among children aged 5–14 years (around 7%), likely reflecting targeted child dental programs, and substantially higher levels among young adults aged 15–34 years (around 27%) and adults aged 35–54 years (around 34%), who also accounted for the largest number of people experiencing unmet need. Importantly, unmet need for dental care was similar among First Nations people who usually accessed Aboriginal Medical Services or Aboriginal Community Controlled Health Services and those who usually accessed mainstream general practitioners, indicating that barriers to dental care persist across service settings rather than being confined to one sector (AIHW 2025a).
Across both survey cycles, the most commonly reported reasons for unmet dental need were cost, long waiting times, and services being unavailable or too far away. In 2022–23, cost was much less of a barrier for those using an Aboriginal Medical Service or Community Clinic (AMS/CC) (28%) than for those using a mainstream GP (52%), while waiting time being too long or the service not being available at the time required was much less of a barrier for those using a mainstream GP (16%) than those using an AMS/CC (31%). In 2018-19, cost was the most common reason for both types of health care (29% for AMS/CC and 48% for GP) (AIHW 2024a, 2025a).
First Nations children experience twice the rate of dental caries as non-Indigenous children, with many families deterred from seeking care due to judgmental attitudes and a focus on individual treatment over preventive measures. A study in Western Australia examined structural factors outside individual control that were affecting oral health in First Nations children. It used perspectives from Aboriginal Health Workers, parents/carers, and dental professionals to identify structural factors such as access to and cost of dental services and discrimination from service providers. The findings highlight how structural determinants such as systemic racism, economic disadvantage, and health care practices that blames and penalises individuals undermine the opportunities and choices of First Nations people. This further exacerbates oral health disparities while these structural determinants and the harm they cause remain unexamined. Reducing health inequities and improving oral health outcomes for First Nations families requires dental care models to be more accountable for delivering high quality care, prioritising prevention, addressing racism and integrating First Nations peoples lived experiences (Durey et al. 2023).
International research on oral health inequalities has shown geographic isolation, economic disadvantage, and limited resources restrict access to necessary services, while patient-centred barriers, including dental anxiety and communication challenges, further exacerbate disparities. Additionally, a lack of training among dental professionals and fragmented service networks between primary, community, and hospital care contribute to inadequate and poorly coordinated oral health services. Many interventions remain treatment-focused, with limited emphasis on prevention or integration with broader public health and primary care systems. To address these gaps, recommended actions include training dental teams in patient-centred care, conducting equity audits, expanding community-based prevention programs, and advocating for policies to reduce sugar, tobacco, and alcohol consumption. Strengthening managed care pathways and collaboration between dental, medical, and social care providers is essential, alongside research and education initiatives to support workforce capacity and reduce inequalities (Watt et al. 2019).
A study on the contribution of socio-demographic, economic and behavioural risk factors on fair/poor self-rated oral health found that negative life events and racism significantly impact the oral health of First Nations adults, with 33.5% reporting poor oral health and those experiencing racism being at greater risk (Jamieson et al. 2023). This finding aligns with research indicating racism's structural impacts, including culturally insensitive care, clinician bias towards tooth extraction rather than restoration, and differential access to dental services among First Nations people. Moreover, addressing oral health disparities requires trauma-informed, culturally safe, and culturally competent dental care, including workforce training and systemic reforms (Hedges et al. 2021; Jamieson et al. 2023).
First Nations adults experience significantly poorer oral health outcomes than non-Indigenous populations, with disparities not fully explained by socio-demographic factors alone. Lower oral health-related self-efficacy significantly contributes to these poorer oral health outcomes, highlighting the importance of culturally tailored interventions addressing social determinants and psychosocial factors to improve overall health and wellbeing (Parker et al. 2022a; Parker et al. 2022b). Western dental approaches (for example fluoride varnish), while clinically efficacious may not be enough to lead to lasting dental improvement in First Nations children, where other determinants such as socioeconomic status, access to services, and cultural and environmental factors act as barriers to oral health (Patel et al. 2017; Smith et al. 2007; Williams et al. 2011).
First Nations Health Workers can play a pivotal role in improving access to oral health care for First Nations communities by bridging cultural and systemic gaps between mainstream health services and First Nations patients. Their involvement fosters trusted relationships, enhances service use, and increases access to culturally safe care. When trained and supported within a defined oral health role, First Nations Health Workers directly contribute to increased access to dental services and have the potential to reintroduce cultural values and knowledges into oral health practices. Expanding their role and leadership in both community-controlled and mainstream oral health services would help address barriers to care, particularly in remote communities where dental services are limited (Poirier et al. 2023).
A review of oral health interventions for First Nations communities found oral health interventions should not just be community-based but also community-driven with a shared understanding of outcomes, and with coordinated activities that use the skills of local staff and build capacity in oral health promotion. This review drew on evidence from multiple service-level interventions but notes that the impact of social determinants will continue to limit the effect of oral health interventions on First Nations health outcomes if those determinants are not understood and addressed (Patel et al. 2017).
A cross-sectional study of First Nations adults attending at the Southern Queensland Centre of Excellence in Aboriginal and Torres Strait Islander Primary Health Care between January 2014 and December 2015 explored oral health behaviours, status and impacts among 945 First Nations adults. The participants, aged 20 or older (average age 41.3 years, 49.3% female), reported high rates of dental caries (49.2–76.4%) and dental problems (29.6–64.6%), with 39.9% experiencing pain or discomfort in the previous 6 months. Despite these significant issues, only 28.4% expressed dissatisfaction with their dental appearance. The authors suggest this indicates people are resigned to their own poor oral health. While 97.3% owned a toothbrush and 56.2% brushed their teeth at least twice daily, dental service utilisation was low, with just 28.8% visiting a dentist in the previous year, primarily for problem-driven (84.3%) rather than preventive care. Barriers such as high costs and restricted access to public dental services were significant contributors to the underutilisation of care (Schluter et al. 2017).
Qualitative studies exploring oral health experiences among First Nations women identified significant challenges linked to systemic racism, intergenerational trauma, and distrust of health care systems. The long-term effects of colonisation continue to shape access to oral health care, with women experiencing shame, fear, and anxiety when engaging with services. Pregnancy was identified as a critical period for oral health, yet culturally safe care remains limited. Motherhood brought additional challenges, as many women associated pregnancy with oral health decline. Mothers often prioritised their children’s oral health over their own, constrained by time, resources and a lack of culturally appropriate information. Participants highlighted the need for community-driven education, holistic antenatal oral health integration, and greater involvement of First Nations health workers to improve accessibility and engagement (Butten et al. 2020; Kong et al. 2020). Maternal oral health knowledge and level of education did have a protective effect on the dental decay of children. Higher knowledge and levels of education reduced the odds of having decayed-missing-filled teeth of one or more by over 50% (OR 0.473), and almost 80% (OR 0.212) respectively (George et al. 2023). Economic evaluation of the Midwifery Initiated Oral Health Program in Australia found that compared with current practice, the midwives’ only intervention providing oral health education, assessment and referral to existing dental services was cost-effective, and represents a low-cost intervention. Midwives and dentists combined interventions were cost-effective when the benefits were considered over longer periods (Tannous et al. 2021).
A collaborative study in South Australia using participatory action research methods from 2018 to 2023 co-designed culturally safe oral health strategies for First Nations Kidney Warriors (First Nations people living with kidney disease). This cohort faces unique oral health challenges, including dry mouth, erosion, periodontal disease, and caries due to dialysis, medications, and reduced fluid intake – factors that can delay or prevent kidney transplantation. This co-designed approach adopted culturally safe practices such as Dadirri - deep listening, Ganma - knowledge sharing, and clinical yarning, positioning Kidney Warriors as educators and co-designers to shape care strategies. Co-designed clinical placements at the Kanggawodli Aboriginal Hostel strengthened trust in health services and enhanced oral health literacy, benefiting both patients and dental hygienist students, who gained confidence in delivering culturally safe, patient-centred care. The study developed a framework for integrating cultural safety education into kidney and oral health services, supporting expanded clinical placements and community-based outreach programs (Kelly et al. 2024).
A large population-based study in Victoria found that First Nations children had a 57% higher risk of developing early childhood caries (ECC) than non-Indigenous children and experienced caries earlier, with half affected by ECC and 40% having untreated decay – well above the national average (Singh et al. 2025). In the Northern Territory, where dental caries affected 87% of First Nations children aged 11, the introduction of community water fluoridation (CWF) in remote communities led to significant reductions in caries across all age groups. A cost–benefit analysis found that within one year of implementation, CWF was associated with a 7% reduction in dental caries and a 10% reduction in preventable hospitalisations, with a clear and significant decline in mean decayed, missing or filled teeth across birth cohorts. This approach was also highly cost-effective, generating savings to health services ranging from $1.10 per $1 invested in small communities to $16 in larger ones. Expanding CWF in remote First Nations communities can deliver oral health improvements and long-term economic and public health benefits (Chondur et al. 2024; Zhao et al. 2023).
A randomised controlled trial in South Australia assessing an ECC intervention among First Nations children found that initiating oral health interventions during pregnancy and infancy was associated with lower caries experience in the primary dentition at age nine compared to a later start. The community co-designed and culturally safe ECC intervention reduced dental caries in both primary and permanent teeth, demonstrating sustained benefits for First Nations children (Ju et al. 2025).
A randomised controlled trial assessing atraumatic restorative treatment and Hall technique (ART/HT) among First Nations children in remote Western Australia found the model to be both feasible and effective in improving child oral health-related quality of life (COHRQoL) and reducing dental anxiety. The intervention delivered effective dental care using minimally invasive techniques without anaesthesia, resulting in more completed treatments and stabilised oral health outcomes, while children receiving standard care experienced deterioration in quality of life. The culturally safe, community-based approach enabled dental services to be provided in non-traditional settings, improving accessibility for families and reducing the need for hospital-based treatment (Arrow et al. 2022).
A study of 29 Aboriginal Community Controlled Health Services (ACCHSs) in New South Wales found that while 56% provided oral health services, 79% reported unmet community needs due to funding and workforce shortages. Despite these challenges, ACCHSs demonstrated strengths in delivering culturally appropriate and community-driven oral health care, integrating these services with broader health initiatives tailored to local needs (Campbell et al. 2015).
An analysis of oral health programming and promotion by 12 Aboriginal Community Controlled Health Organisations (ACCHOs) in South Australia highlighted their key role in preventive care, education and advocacy. Despite geographic gaps in service availability, ACCHOs demonstrated leadership and adaptability, particularly during the COVID-19 pandemic, by addressing community needs through culturally secure approaches (Poirier et al. 2022). A study in a rural First Nations community in Queensland further emphasised the importance of community-led oral health education, with older participants highlighting oral health as a priority shaped by personal experiences of severe pain from untreated disease and its impact on appearance, confidence and social interactions (Tynan et al. 2020). Despite this, oral health often competed with other urgent health and social priorities, such as managing chronic diseases and meeting basic needs, which constrained access to timely care. Participants demonstrated strong awareness of oral health’s connection to chronic conditions like diabetes and expressed a commitment to educating younger generations. The findings reinforce the need for establishing affordable, culturally appropriate, community-based oral health care services and oral health promotion to sustain long-term improvements in oral health outcomes (Poirier et al. 2022; Tynan et al. 2020).
A recent Issues Brief examined the potential of oral health care integration into primary health care in rural and remote Australia, with a particular focus on First Nations populations. These communities face significant oral health inequities, including high rates of periodontal disease and untreated caries, compounded by co-existing chronic conditions such as diabetes and kidney disease. The research found that disparities were exacerbated by workforce shortages, limited oral health training for primary care providers, and restrictive funding models. The recommendations to improve First Nations access to oral health care included expanding oral health training for primary health care professionals, recognising oral health as a core component of primary health care, and innovative oral health models of care integrated into primary health care. Primary health care professionals are well positioned to provide basic oral health care such as screening for risk factors, oral health education, non-invasive preventative interventions and referral. However, limited knowledge, skills and professional boundaries and scopes of practice, and lack of coverage by Medicare subsidies restrict the degree these benefits can be realised (Veginadu and Haddock 2024).
A community-level qualitative study in rural Australia explored the perspectives of a rural First Nations community on how to resolve local oral health problems. Although the State provides a free dental service, this is not accessed freely by community members, with many facing significant financial and transport barriers. Most of the community were not aware of the Child Dental Benefits Schedule (CDBS), and rural First Nations communities have very limited access to dental personnel in comparison to the general population. The community strongly emphasised the importance of integrating oral health care services within existing primary health services and within existing community activities. The community is concerned that oral health messaging is often unavailable or only provided to those who had the means to access an oral health care service. The connection between oral disease and other health conditions provides opportunities for oral health care messages to be part of primary health care. The study showed that an individual’s connection to family has important meaning in influencing participation in oral health care activities. The study highlights that continuous consultations and co-design between oral health care services and First Nations communities are important to improve First Nations oral health in rural and remote areas (Walker et al. 2022).
The Northern Territory Remote Aboriginal Investment Oral Health Program (NTRAI OHP) focused on addressing oral health issues among First Nations children under 16 in rural and remote areas of the Northern Territory from July 2012 to December 2023. The program aimed to reduce the prevalence, severity and impact of oral health problems by providing preventive and clinical services. Over 20,000 First Nations children benefited from the program and all service delivery benchmarks, including clinical service visits and preventive applications, were met or exceeded in 2023. Despite these achievements, tooth decay remains highly prevalent, particularly among children aged 7–10 years, with 84–88% affected in 2023. (AIHW 2025b). The data highlights the need to build on past successes by expanding access to preventive measures such as fluoride varnish and fissure sealants, sustaining culturally safe service delivery, and strengthening collaboration with communities to address persistent oral health disparities.
Similarly, a state-level scoping review in New South Wales of the Aboriginal Oral Health Plan (2014–2020) examined 31 studies and initiatives and found progress in culturally tailored oral health promotion and service delivery. Community-led programs such as school-based toothbrushing, fluoride varnish application, and water fountain installation were linked to reductions in dental caries and improved oral hygiene behaviours. Workforce initiatives included scholarships, cultural competence training, and programs like the Dalang Project, placed graduate oral health therapists in ACCHSs. Mobile and community-led service models improved access to culturally safe care. However, the review identified persistent gaps in preventive care uptake, limited access to fluoride varnish programs, and underutilisation of preventive dental services among Aboriginal children. It noted the need for scaling up successful initiatives, securing long-term funding, and strengthening collaboration between health services, universities, and Aboriginal communities. These findings indicate that while progress has been made, there remains room for improvement to achieve sustained and equitable oral health outcomes (Maqbool et al. 2022).
Implications
Oral health is a key component of overall wellbeing and quality of life. Despite ongoing investment, First Nations people continue to experience disproportionate oral health challenges. It is clear that systemic and structural barriers – including racism, economic disadvantage, and limited access to culturally safe care exacerbate these challenges (Hedges et al. 2021; Jamieson et al. 2023). For example, evidence from the review of the New South Wales Aboriginal Oral Health Plan and the performance data from the Northern Territory Remote Aboriginal Investment Oral Health Program highlights that while progress has been made, gaps remain in preventive oral health care and access, indicating the need for continued improvement and community collaboration (AIHW 2025b; Maqbool et al. 2022).
On 7 February 2025, the Australian Government signed a new Partnership Agreement with the Northern Territory government and Aboriginal Peak Organisations Northern Territory (APO NT) to strengthen remote services. The Australian Government will commit $842.6 million over 6 years in support of the Partnership Agreement, commencing 1 July 2025.
The Australian Government, in partnership with states and territories, is developing the National Oral Health Plan (NOHP) 2025–2034. This will include goals to improve the oral health status of Australians and reduce inequalities in oral health across the Australian population. The previous NOHP 2015–2024 remains active (until a new plan is in place), it acknowledged the higher rates and severity of oral disease experienced by First Nations communities, and prioritised community engagement, culturally safe care, and workforce participation to improve access and equity. Building on this, the new plan will continue to prioritise First Nations communities. Targeted consultation with First Nations communities was conducted to ensure their needs and perspectives are meaningfully incorporated into the development of the new plan. Consultations informing the design of the new plan have highlighted needs for enhanced dental health care access, affordability and equity through expanded funding, preventive services, and partnerships, while incorporating emerging priorities such as data, monitoring, technology, and strengthening leadership (DoHDA 2025).
Data show that First Nations people – particularly children – experience poorer dental health than non-Indigenous Australians. Barriers include cost, limited access to healthy diets, delayed care-seeking, insufficient oral health education, unmet demand in public dental services, lack of water fluoridation in some areas, and cultural competency issues in service delivery (Durey et al. 2016; Dyson et al. 2014; Johnson et al. 2014).
The Fifth Review of the Dental Benefits Act 2008 and the NACCHO submission to the same review both highlighted persistent disparities in oral health outcomes and access to dental care for First Nations children. Despite the Child Dental Benefits Schedule (CDBS) providing a national framework for dental benefits, First Nations children consistently experience lower utilisation compared with non-Indigenous children, with an average gap of 14 percentage points between 2018 and 2022. These disparities are compounded by higher rates of dental disease (especially in remote areas) and systemic barriers including limited culturally safe care, geographic isolation, workforce shortages, and inadequate data transparency. While Aboriginal Community Controlled Organisations (ACCHOs) are preferred providers and increasingly offer dental services, they face resource constraints and lack sufficient support to meet demand. Both reports recommend targeted reforms to the CDBS, including co-designing services with First Nations organisations, expanding access for non-dental health practitioners, enhancing workforce development, improving data collection and visibility, and promoting culturally safe practices across both community-controlled and mainstream services (DoHAC 2023; NACCHO 2022).
The Australian Government continues to invest in programs that support access to dental care across both public and private sectors. Between 2021 and 2025, $431 million was provided to states and territories through the Federation Funding Agreement on Public Dental Services for Adults, with a further $107.8 million committed for 2025–26. Basic dental services for children aged 0–17 from low-income families is supported through the CDBS. Additional funding is provided under the 2020–25 National Health Reform Agreement (NHRA), which also supports access to private dental care through the Private Health Insurance rebate (DoHAC 2020). The NHRA identifies First Nations people as a priority population and promotes equitable access to culturally safe, community-led health care. It recognises the role of ACCHOs in delivering primary care and improving oral health outcomes for First Nations communities (DoHAC 2025). Monitoring frameworks should ensure that these investments translate into measurable improvements in access and outcomes for First Nations communities.
School dental programs remain important, particularly in remote areas. However, these services may be underutilised by First Nations children, potentially due to a lack of cultural safety (Parker et al. 2012). Integrating dental services within ACCHOS may offer a more culturally appropriate and effective alternative. Community-led, family-inclusive approaches are more likely to be sustainable and impactful. Coordinated efforts between schools, families, and dental providers can strengthen oral health promotion and service delivery. However, long-term improvements will require addressing the broader social determinants and systemic inequities that affect oral health outcomes.
A self-determination informed policy reform in Victoria led to an amendment of the Drugs, Poisons and Controlled Substances Regulations 2022, authorising registered Aboriginal Health Practitioners (AHPs) to obtain, possess, and administer fluoride varnish as part of their health service delivery. The initiative, led by the Loddon Mallee Aboriginal Reference Group (LMARG), aims to build a First Nations workforce capable of delivering culturally appropriate, integrated oral health care to First Nations children. This reform addresses significant barriers in mainstream dental service access caused by limited cultural responsiveness and workforce representation. By embedding oral health promotion within Aboriginal Community Controlled Organisations (ACCOs), the model supports timely fluoride varnish applications and greater community engagement in preventive oral health care (Ummer-Christian et al. 2024).
Over the past two decades, there has been a strong commitment to embedding cultural respect in the Australian health system. The Cultural Respect Framework 2016–2026 provides a nationally consistent approach to culturally safe and responsive care. While not specific to oral health, its principles are broadly applicable. Progress is monitored through frameworks such as the Aboriginal and Torres Strait Islander Health Performance Framework (see measure 3.08 Cultural competency) and the Cultural safety in health care for Indigenous Australians: monitoring framework which assess service delivery, patient experience, and access to care (AIHW 2023).
The National Aboriginal and Torres Strait Islander Health Plan 2021–2031 provides the overarching policy framework for progressing the National Agreement on Closing the Gap. It promotes structural reform towards integrated, culturally safe models of care that prioritise prevention and early intervention. In relation to oral health, the Health Plan emphasises strengths-based, holistic, and affordable care – particularly for children – to support early intervention and prevent disease. It advocates for expanded access to essential dental services, increased uptake of programs like the CDBS, and community partnerships to co-design and deliver oral health initiatives that improve literacy, access, and outcomes across generations.
References
-
AIHW (Australian Institute of Health and Welfare) (2023) Cultural safety in health care for Indigenous Australians: monitoring framework, AIHW, Australian Government, accessed 14 April 2026.
-
AIHW (2024a) Aboriginal and Torres Strait Islander people and primary health care: patterns of service use, preferences, and access to services, AIHW, Australian Government, accessed 8 April 2026, doi:10.25816/40jc-y926.
-
AIHW (2024b) Oral health and dental care in Australia, AIHW, Australian Government.
-
AIHW (2025a) Aboriginal and Torres Strait Islander people’s preferences for, use of, and access to primary health care 2025, AIHW, Australian Government, accessed 27 March 2026.
-
AIHW (2025b) Oral health outreach services for Aboriginal and Torres Strait Islander children in the Northern Territory: July 2012 to December 2023, AIHW, Australian Government, accessed 2 April 2026, doi:10.25816/vtc2-p720.
-
AIHW (2026) First Nations Burden of Disease Study 2022, AIHW, Australian Government, accessed 16 April 2026.
-
Arrow P, Piggott S, Carter S, McPhee R, Atkinson D, Brennan DS, Kularatna S, Tonmukayakul U, Nanda S, Mackean T and Jamieson L (2022) 'Atraumatic restorative treatments and oral health-related quality of life and dental anxiety in Australian Aboriginal children: A cluster-randomized trial', Community Dentistry and Oral Epidemiology, 50(6):513–521, doi:10.1111/cdoe.12704.
-
Brennan DS, Spencer AJ and Roberts-Thomson KF (2019) 'Socioeconomic and psychosocial associations with oral health impact and general health', Community Dentistry and Oral Epidemiology, 47(1):32–39, doi:10.1111/cdoe.12419.
-
Butten K, Johnson NW, Hall KK, Toombs M, King N and O’Grady K-AF (2020) 'Yarning about oral health: perceptions of urban Australian Aboriginal and Torres Strait Islander women', BMC Oral Health, 20(1):35, doi:10.1186/s12903-020-1024-x.
-
Campbell MA, Hunt J, Walker D and Williams R (2015) 'The oral health care experiences of NSW Aboriginal Community Controlled Health Services', Australian and New Zealand Journal of Public Health, 39(1):21–25, doi:10.1111/1753-6405.12294.
-
Chondur R, Raymond KJ, Zhao Y, Bailie R and Burgess P (2024) 'Effects of community water fluoridation on child dental caries in remote Northern Territory, Australia: a difference-in-difference analysis', Rural and Remote Health, 24:8904.
-
Diabetes Australia (2025) Preventing diabetes complications: Dental health, accessed 16 September 2025.
-
Do L and Spencer A (2016) Oral health of Australian children: the National Child Oral Health Study 2012–14, University of Adelaide Press.
-
DoHAC (Department of Health and Aged Care) (2020) Extending the National Partnership Agreement on Public Dental Services, Australian Government.
-
DoHAC (2023) Report on the Fifth review of the Dental Benefits Act 2008, Australian Government.
-
DoHAC (2025) National Health Reform Agreement, Australian Government.
-
DoHDA (Department of Health, Disability and Ageing) (2025) Developing the National Oral Health Plan 2025–2034, Australian Government website.
-
Durey A, McAullay D, Gibson B and Slack-Smith L (2016) 'Aboriginal Health Worker perceptions of oral health: a qualitative study in Perth, Western Australia', International Journal for Equity in Health, 15(1):4, doi:10.1186/s12939-016-0299-7.
-
Durey A, Naylor N and Slack-Smith L (2023) 'Inequalities between Aboriginal and non-Aboriginal Australians seen through the lens of oral health: time to change focus', Philosophical Transactions of the Royal Society B: Biological Sciences, 378(1883):20220294, doi:10.1098/rstb.2022.0294.
-
Dyson K, Kruger E and Tennant M (2014) 'A decade of experience evolving visiting dental services in partnership with rural remote Aboriginal communities', Australian Dental Journal, 59(2):187–192, doi:10.1111/adj.12162.
-
Genco RJ and Borgnakke WS (2013) 'Risk factors for periodontal disease', Periodontol 2000, 62(1):59–94, doi:10.1111/j.1600-0757.2012.00457.x.
-
George A, Kong A, Sousa MS, Villarosa A, Ajwani S, Dahlen HG, Bhole S, Yaacoub A, Srinivas R and Johnson M (2023) 'Long-term effectiveness of the midwifery initiated oral health-dental service program on maternal oral health knowledge, preventative dental behaviours and the oral health status of children in Australia', Acta Odontologica Scandinavica, 81(2):164–175, doi:10.1080/00016357.2022.2108896.
-
Hedges J, Haag D, Paradies Y and Jamieson L (2021) 'Racism and oral health inequities among Indigenous Australians', Community dental health, 38(2):150–155, doi:10.1922/CDH_IADRHedges06.
-
Iacob AM, Escobedo Martínez MF, Barbeito Castro E, Junquera Olay S, Olay García S and Junquera Gutiérrez LM (2024) 'Effects of Vape Use on Oral Health: A Review of the Literature', Medicina, 60(3):365, doi: 10.3390/medicina60030365.
-
Jamieson L, Hedges J, Paradies Y and Ju X (2023) 'Does the contribution of modifiable risk factors on oral health inequities differ by experience of negative life events among Indigenous Australian adults?', PloS One, 18(6):e0286697, doi:10.1371/journal.pone.0286697.
-
Jamieson LM, Roberts-Thomson KF and Sayers SM (2010) 'Risk indicators for severe impaired oral health among indigenous Australian young adults', BMC Oral Health, 10(1):1, doi:10.1186/1472-6831-10-1.
-
Johnson NW, Lalloo R, Kroon J, Fernando S and Tut O (2014) 'Effectiveness of water fluoridation in caries reduction in a remote Indigenous community in Far North Queensland', Australian Dental Journal, 59(3):366–371, doi:10.1111/adj.12190.
-
Joshipura KJ, Hung H-C, Rimm EB, Willett WC and Ascherio A (2003) 'Periodontal disease, tooth loss, and incidence of ischemic stroke', Stroke, 34(1):47–52.
-
Ju X, Hedges J, Haag DG, Soares GH, Smithers LG and Jamieson LM (2025) 'Early childhood caries intervention in Aboriginal Australian children: Follow-up at child age 9 years', PloS One, 20(9):e0317024, doi:10.1371/journal.pone.0317024.
-
Kelly J, Owen K, Tyrell K, Clemente K, Steffens M, Sinclair N, Reynolds S, Allan W and project AKAKCT-ION (2024) 'Codesigning culturally safe oral health care with First Nations Kidney Warriors experiencing kidney disease in South Australia', BMC Oral Health, 24(1):864, doi:10.1186/s12903-024-04617-8.
-
Kong AC, Sousa MS, Ramjan L, Dickson M, Goulding J, Gwynne K, Talbot F, Jones N, Srinivas R and George A (2020) '“Got to build that trust”: the perspectives and experiences of Aboriginal health staff on maternal oral health', International Journal for Equity in Health, 19(1):187, doi:10.1186/s12939-020-01301-5.
-
Lalloo R, Jamieson LM, Ha D, Ellershaw A and Luzzi L (2015) 'Does fluoride in the water close the dental caries gap between Indigenous and non-Indigenous children?', Australian Dental Journal, 60(3):390–396, doi:10.1111/adj.12239.
-
Lalloo R, Jamieson LM, Ha D and Luzzi L (2016) 'Inequalities in Tooth Decay in Australian Children by Neighbourhood Characteristics and Indigenous Status', Journal of Health Care for the Poor and Underserved, 27(1 Suppl):161–177, doi:10.1353/hpu.2016.0045.
-
Loos BG and Van Dyke TE (2020) 'The role of inflammation and genetics in periodontal disease', Periodontol 2000, 83(1):26–39, doi:10.1111/prd.12297.
-
Maqbool A, Selvaraj CM, Lu Y, Skinner J and Dimitropoulos Y (2022) 'The Progress of the New South Wales Aboriginal Oral Health Plan 2014–2020: A Scoping Review', Healthcare, 10(4):650, doi: 10.3390/healthcare10040650.
-
NACCHO (National Aboriginal Community Controlled Health Organisation) (2022) Fifth review of the Child Dental Benefits Schedule: submission to the Dept of Health and Aged Care, NACCHO.
-
NOHA (National Oral Health Alliance) (2023) Joint Position Statement on Universal Access to Affordable Oral Healthcare, National Oral Health Alliance.
-
Parker E, Misan G, Shearer M, Richards L, Russell A, Mills H and Jamieson L (2012) 'Planning, implementing, and evaluating a program to address the oral health needs of Aboriginal children in Port Augusta, Australia', International Journal of Pediatrics, 2012.
-
Parker EJ, Haag DG, Spencer AJ, Roberts-Thomson K and Jamieson LM (2022a) 'Self-efficacy and oral health outcomes in a regional Australian Aboriginal population', BMC Oral Health, 22(1):447, doi:10.1186/s12903-022-02471-0.
-
Parker EJ, Mejia G, Spencer AJ, Roberts-Thomson KF, Haag D and Jamieson LM (2022b) 'Self-rated oral and general health among Aboriginal adults in regional South Australia', Australian Dental Journal, 67(2):132–137, doi:10.1111/adj.12892.
-
Patel J, Durey A, Hearn L and Slack‐Smith L (2017) 'Oral health interventions in Australian Aboriginal communities: a review of the literature', Australian Dental Journal, 62(3):283–294.
-
Poirier B, Sethi S, Hedges J and Jamieson L (2023) 'Building an understanding of Indigenous Health Workers’ role in oral health: A qualitative systematic review', Community Dentistry and Oral Epidemiology, 51(2):169–179, doi:https://doi.org/10.1111/cdoe.12743.
-
Poirier B, Tang S, Haag DG, Sethi S, Hedges J and Jamieson L (2022) 'Oral health promotion and programming provided by Aboriginal Community Controlled Health Organisations in South Australia', Health Promotion Journal of Australia, 33(S1):255–261, doi:10.1002/hpja.640.
-
Quaranta A, D'Isidoro O, Piattelli A, Hui WL and Perrotti V (2022) 'Illegal drugs and periodontal conditions', Periodontology 2000, 90(1):62–87, doi:10.1111/prd.12450.
-
Roberts-Thomson KF, Spencer AJ and Jamieson L (2008) 'Oral health of Aboriginal and Torres Strait Islander Australians', The Medical Journal of Australia, 188(10):592–593.
-
Schluter PJ, Askew DA, Spurling GK, Lee M and Hayman N (2017) 'Aboriginal and Torres Strait Islander oral health and its impact among adults: A cross-sectional study', Australian Dental Journal, 62(1):84–94, doi:https://doi.org/10.1111/adj.12439.
-
Sicca C, Bobbio E, Quartuccio N, Nicolò G and Cistaro A (2016) 'Prevention of dental caries: A review of effective treatments', Journal of Clinical and Experimental Dental, 8(5):e604–e610, doi:10.4317/jced.52890.
-
Singh A, Hegde S, Silva M, Whelan M, Karahalios A, Manton DJ, Goldfeld S, English DR and Dashper S (2025) 'Social inequities in early childhood caries in Australia: A population-based study on statewide public dental services data', International Journal of Paediatric Dentistry, 35(1):186–193, doi:10.1111/ipd.13219.
-
Smith K, Kruger E, Dyson K and Tennant M (2007) 'Oral health in rural and remote Western Australian Indigenous communities: A two‐year retrospective analysis of 999 people', International Dental Journal, 57(2):93–99.
-
Tannous KW, George A, Ahmed MU, Blinkhorn A, Dahlen HG, Skinner J, Ajwani S, Bhole S, Yaacoub A, Srinivas R and Johnson M (2021) 'Economic evaluation of the Midwifery Initiated Oral Health-Dental Service programme in Australia', BMJ Open, 11(8):e047072, doi:10.1136/bmjopen-2020-047072.
-
Taylor GW and Borgnakke W (2008) 'Periodontal disease: associations with diabetes, glycemic control and complications', Oral diseases, 14(3):191–203.
-
Tynan A, Walker D, Tucker T, Fisher B and Fisher T (2020) 'Factors influencing the perceived importance of oral health within a rural Aboriginal and Torres Strait Islander community in Australia', BMC Public Health, 20(1):514, doi:10.1186/s12889-020-08673-x.
-
Ummer-Christian R, Widdicombe D, Raichur A and Couch D (2024) 'Aboriginal Health Practitioners obtaining, possessing and administering fluoride varnish: self-determination driven regulation amendment for integrated oral health care for Aboriginal children', Australian Journal of Primary Health, 30(1):PY23201, doi:10.1071/PY23201.
-
Veginadu P and Haddock R (2024) Integrating oral health into primary healthcare for improved access to oral health care for rural and remote populations, Issues Brief No 53, Deeble Institute for Health Policy.
-
Walker D, Tynan A, Tucker T, Fisher B and Fisher T (2022) 'Engaging with a rural Aboriginal community to identify strategies to improve oral health within their community: a qualitive study', Australian Journal of Primary Health, 29(1):38–46, doi:10.1071/PY22215.
-
Watt RG, Venturelli R and Daly B (2019) 'Understanding and tackling oral health inequalities in vulnerable adult populations: from the margins to the mainstream', British Dental Journal, 227(1):49–54, doi:10.1038/s41415-019-0472-7.
-
Williams S, Jamieson L, MacRae A and Gray C (2011) 'Review of Indigenous oral health', Australian Indigenous HealthInfoNet, No. 7.
-
Xiong X, Buekens P, Fraser W, Beck J and Offenbacher S (2006) 'Periodontal disease and adverse pregnancy outcomes: a systematic review', BJOG: An International Journal of Obstetrics & Gynaecology, 113(2):135–143.
-
Ylöstalo P, Järvelin M, Laitinen J and Knuuttila M (2006) 'Gingivitis, dental caries and tooth loss: risk factors for cardiovascular diseases or indicators of elevated health risks', Journal of Clinical Periodontology, 33(2):92–101.
-
Zhao Y, Raymond K, Chondur R, Sharp W, Gadd E, Bailie R, Skinner J and Burgess P (2023) 'Costs and benefits of community water fluoridation in remote Aboriginal communities of the Northern Territory', Australian Journal of Rural Health, 31(5):1017–1026, doi:10.1111/ajr.13037.

