Key messages
Why is it important?
Early detection and treatment of non-communicable diseases, such as through screening programs, are recognised by the World Bank as one of the most cost-effective health interventions that can be delivered in primary health care settings. For Aboriginal and Torres Strait Islander (First Nations) people, who experience disproportionately high rates of chronic disease and cancer, early detection is especially important in order to identify disease in its early stages and enable appropriate treatment to slow or halt disease progression and ultimately reduce preventable deaths. However, the cultural appropriateness of the national screening programs, health assessments and timely follow-up care is a critical enabler of First Nations people seeking and participating in health care.
Data findings
-
Between 2015–16 and 2023–24, the number of First Nations people accessing health assessments increased from 191,526 to 259,941. The uptake of health assessments nationally did not change significantly over this period, with a low of 21% in 2021–22, associated with the COVID-19 pandemic, and a high of 25% in 2023–24.
-
In 2023–24, among First Nations people, 78,715 health assessments were undertaken for 76,467 (23%) children aged 0–14, 120,659 health assessments for 117,074 (23%) patients aged 15–49 and 69,198 health assessments for 66,400 (35%) patients aged 50 and over.
-
At June 2025, 55% (or around 65,000) of First Nations regular clients aged 35–74 with no known history of CVD had the necessary risk factors recorded within the previous 24 months to assess their absolute CVD risk.
-
The Breast cancer screening participation rate (age-standardised) for First Nations women aged 50–74 was 36% in 2022–2023, with no statistically significant change from 2016–2017 (32%).
-
Breast cancer screening participation rates for First Nations women aged 50–74 were lower in Remote and very remote areas (28%) than in non-remote areas (36% in Major cities and 39% in Inner and outer regional areas). The rate was lowest in the Northern Territory (20%) and highest in Queensland and the Australian Capital Territory (both 41%).
-
The proportion of First Nations women aged 50–74 who had been screened for breast cancer was 15 percentage points lower than for non-Indigenous women (36% compared with 51%).
-
Data from the National Key Performance Indicators Data Collection show that the proportion of regular female clients aged 25–74 of First Nations-specific primary health care services (who had not had a hysterectomy) who had a cervical screening test in the previous 5 years has been increasing over time – from 38% as at December 2020 to 51% as at June 2025.
-
The participation rate in the National Bowel Cancer Screening Program for First Nations people aged 50–74 was estimated to be 38% in 2022–2023, 4 percentage points lower than non-Indigenous Australians (42%).
-
Data from the National Bowel Cancer Screening Program show First Nations participants were more likely to receive a positive result, indicating potential cancer, than non-Indigenous participants (8.0% and 5.8%, respectively). However, First Nations participants with a positive result had a lower rate of follow-up colonoscopy (78% compared with 86%) and a longer median time between a positive screen and assessment (78 days compared with 62 days, respectively).
Research and evaluation findings
-
Community-led initiatives have demonstrated measurable success in improving early detection and treatment outcomes. For example, the Beautiful Shawl Project, led by the Victorian Aboriginal Community Controlled Health Organisation (VACCHO), increased breast screening of First Nations women by creating culturally affirming experiences. In 2023–24, 40% of participants were screened for the first time while 26% had been overdue, showing the program’s success in reaching women who were previously missed.
-
Barriers to implementing health checks include constraints on physical space at health services, competing demands, complex Medicare billing, limited cultural competency, inconsistent identification of Indigenous status, patient concerns about privacy, trust and fear of stigma. Enablers include employing First Nations staff, offering flexible service models, using digital tools and fostering strong community engagement.
-
International research shows Indigenous populations underutilise cancer screening, especially for non-breast cancers, due to lower awareness, negative attitudes, and distrust in health systems.
-
In Australia, First Nations people have lower participation in the national cancer screening programs but innovative culturally sensitive approaches to encouraging participation have led to improvements (for example, enabling self-collection in cervical screening). Geographic barriers have also led to innovations in bowel cancer screening practice by enabling immunochemical Faecal Occult Blood Test kits to be provided directly by local health services.
-
Nationally, First Nations women make up 2.3% of women aged 50–74, but in regions located more than 2 hours from the nearest BreastScreen Australia screening site, they represent 57% of this population.
-
Cardiovascular disease (CVD) risk in First Nations people starts early, with research showing 1.1% at high risk by age 18–24 and 4.7% by age 25–34. Those aged 35–74 at high risk were undertreated with only 42% using lipid lowering medication. Guidelines now recommend risk factor screening from age 18 and absolute CVD risk assessment from age 30 to address early onset and higher prevalence of CVD for First Nations people.
Implications
Early detection and timely treatment through culturally safe, community-led primary health care provide measurable benefits for First Nations people. National data show increasing participation of First Nations people in health checks and preventive programs, supported by Aboriginal Community Controlled Health Organisations (ACCHOs) and other First Nations-specific health care providers. However, First Nations people continue to be underserved by national cancer screening programs. For mainstream primary health care, identification of First Nations patients is critical for accessing targeted health initiatives. Other barriers remain, such as the cultural competency of staff, inconsistent follow-up of abnormal results and delays or difficulties in accessing specialist care after an abnormal finding. Additional challenges include geographic remoteness, cost, transport and limited availability of culturally safe services. Australian Government investments aim to improve prevention, early intervention and coordinated care, such as through extended funding for Deadly Choices, efforts to improve the cultural safety of cancer screening programs, and investment in ACCHOs to deliver culturally safe and community-led comprehensive primary health care.
Why is it important?
Early detection refers to identifying a condition at an early stage, often before symptoms appear, through routine care or targeted screening. Early treatment follows promptly after diagnosis, aiming to manage or cure the condition before it progresses (Zwar and Ackermann 2016). Aboriginal and Torres Strait Islander (First Nations) people experience disproportionately high rates of chronic health conditions which are considered potentially preventable with timely, culturally safe primary health care.
The Population-based screening framework (endorsed by all Australian governments) sets out the principles of screening programs for cancer and chronic diseases, providing guidance for decision makers when considering potential population-based screening programs nationally. Screening programs need to meet a range of criteria to ensure their efficacy and acceptability to the public. They also need to promote equity of access for all members of the target population, including important subgroups such as First Nations people and people from culturally and linguistically diverse backgrounds (Clinical Principal Committee Standing Committee on Screening 2018).
Cancer screening programs are organised, systematic approaches designed to reduce illness and death through early detection of cancer or pre-cancerous abnormalities. National programs for breast and cervical screening were implemented in Australia in the early 1990s, in 2006 for bowel cancer screening and, a new national program for lung cancer screening began on 1 July 2025. The National Cervical Screening Program (NCSP) currently recommends that asymptomatic women aged 25 to 74 should have a cervical screening test every 5 years. The BreastScreen Australia Program recommends two-yearly screening for women aged 50 to 74, with all women aged 40 and over eligible to attend. The National Bowel Cancer Screening Program (NBCSP) provides biennial bowel cancer screening for eligible Australians aged 45 to 74 (those 45–49 can request a kit and those 50–74 are automatically sent a kit every 2 years), allowing for early detection and treatment. The National Lung Cancer Screening Program (NLCSP) began on 1 July 2025 and recommends two-yearly screening for asymptomatic, 50 to 70 year old people with a tobacco cigarette smoking history equivalent to 30-pack years or who have quit within the last 10 years. People do not need to quit smoking to be screened.
The World Bank recognises early detection and management of non-communicable diseases (such as through screening programs) as one of the seven cost effective interventions that can be delivered in the primary health care setting to prevent adverse health outcomes (WHO 2023, n.d.). In Australia, primary health care providers, including Aboriginal Community Controlled Health Organisations (ACCHOs) and general practices, and their multidisciplinary teams, play a critical role in the early detection and management of disease. This includes the work of Aboriginal and Torres Strait Islander Health Practitioners and Workers, practice nurses, and other clinical staff who are central to delivering culturally safe, community-led care.
The Australian Government enables General practitioners (GP) to conduct health assessments and checks for First Nations people under the Medicare Benefits Schedule (MBS), as well as incentive payments for improved chronic disease management and cheaper medicines through the Pharmaceutical Benefits Scheme (PBS). The MBS Item 715 is a general health assessment for First Nations people and is used for detecting a wide range of potential health issues that may need follow-up care such as cancer screenings, high blood pressure, high sugar levels, oral health, mental health, sexual and reproductive health, immunisation status, hearing and vision. Following a health check, First Nations patients are eligible to access up to ten allied health services (Medicare-subsidised) per calendar year.
The National Aboriginal and Torres Strait Islander Health Plan 2021-2031 (Health Plan) is an Australian policy representing the Government’s ongoing commitment to improving health outcomes for First Nations people. Its vision is for First Nations people to enjoy long, healthy lives centred in culture, with access to services that are prevention-focused, culturally safe and responsive, equitable and free of racism. The Health Plan identifies priorities and objectives on prevention, early intervention (including screening) and improving access to person-centred and family-centred care.
Data findings
Health checks
Health checks through MBS health assessment items for First Nations people aged 55 and over were introduced in 1999, for those aged 15–54 in 2004, and for those aged 0–14 in 2006. In 2009–10, measures to increase take-up of health assessments by those aged 15 and over were introduced.
In 2023–24, a total of 78,715 health assessments were undertaken for 76,467 First Nations children aged 0–14, representing 23% of First Nations children. There were 120,659 health assessments provided for 117,074 First Nations patients aged 15–49 (representing 23% of this population) and 69,198 health assessments provided for 66,400 First Nations patients aged 50 and over (representing 35% of this population). Overall, 25% (259,941) of First Nations people received a health assessment in 2023–24 (Table D3.04.1).
For Commonwealth-funded First Nations-specific primary health care organisations, 37% (13,676) of First Nations children aged 0–4 (who were regular clients) had received an MBS health assessment in the 12 months prior to June 2025, as did 36% (24,885) of First Nations children aged 5–14. For eligible adults who were regular clients, 50% (102,311) of those aged 15–54 had received a health check in the previous 24 months, as had 61% (34,919) of those aged 55 and over. Overall, 48% (175,791) of First Nations people who were regular clients received a health assessment in the 12 months (for those aged 0–14) or 24 months (for those aged 15 and over) prior to June 2025 (Table D3.04.25).
Cardiovascular disease (CVD) and kidney disease risk assessments
Cardiovascular disease (CVD) includes a range of conditions that affect the heart and blood vessels. The most common and serious types of CVD include coronary heart disease, stroke and heart failure. As a number of its risk factors are modifiable, CVD is preventable in many cases. Risk factors for CVD include overweight and obesity, tobacco smoking, high blood pressure, high blood cholesterol, insufficient physical activity, poor nutrition and diabetes.
At June 2025, 55% (or around 65,000) of First Nations regular clients aged 35–74 with no known history of CVD had the necessary risk factors recorded within the previous 24 months to assess their absolute CVD risk. This proportion was lowest in Very remote areas (51%), followed by Inner regional areas (55%) and Major cities and Outer regional areas (both 56%). In Remote areas a higher proportion of First Nations clients had their CVD risk assessed in the previous 24 months (57%) (AIHW 2026: Table S2.74).
Kidney function tests are another important early detection tool. If kidney disease is diagnosed early, appropriate treatment can be given, and its effects can be closely monitored. The Royal Australian College of General Practitioners (RACGP) guidelines recommend screening kidney function annually for patients with type 2 diabetes and every 1 to 2 years for patients with CVD. This screening checks urine albumin/creatinine ratio (ACR) for albuminuria, and estimated glomerular filtration rate (eGFR) (Kidney Health Australia 2020; RACGP and Diabetes Australia 2024).
At June 2025, both an eGFR and an ACR test result was recorded within the previous 12 months for:
- 48% (or around 23,300) of First Nations regular clients aged 18 and over with type 2 diabetes
- 44% (or around 8,700) of First Nations regular clients aged 18 and over with CVD
- 46% (or around 26,100) of First Nations regular clients aged 18 and over with type 2 diabetes and/or CVD (AIHW 2026: Tables S3.91, S3.109 and S3.127).
Cancer screening
People who identify as First Nations are less likely to participate in breast, cervical and bowel population screening programs than non-Indigenous Australians (AIHW 2024b, 2024d, 2025a). This section provides information on cancer screening participation rates based on available data, noting there are limitations in the data used for calculating the screening participation rates due to under-reporting of Indigenous status.
Breast screening
BreastScreen Australia is a joint initiative of the Australian and state and territory governments that offers free mammographic screening every 2 years for women aged 40 and over, and actively invites women aged 50–74.
The latest BreastScreen Australia data (2022–2023) showed that 36% of First Nations women aged 50–74 were screened for breast cancer (Table D3.04.9).
Breast cancer screening participation rates for First Nations women aged 50–74 were lower in Remote and very remote areas (28%) than in non-remote areas (36% in Major cities and 39% in Inner and outer regional areas) (Table D3.04.30). Screening participation rates for First Nations women aged 50–74 also varied by states and territories, with the lowest rate in the Northern Territory (20%) and the highest in Queensland and the Australian Capital Territory (both 41%) (Table D3.04.9).
After adjusting for differences in the age structure between the two populations, the proportion of First Nations women aged 50–74 who had been screened was 15 percentage points lower than for non-Indigenous women (36% compared with 51%) (Table D3.04.9).
Cervical screening
The National Cervical Screening Program (NCSP) is a joint initiative of the Australian and state and territory governments. It aims to reduce cervical cancer cases, illness, and deaths by detecting precancerous abnormalities in asymptomatic women and people with a cervix.
Cervical screening participation by Indigenous status cannot be reported at the national level due to incomplete and inconsistent recording of Indigenous status at time of collection. An alternative methodology for estimating participation in cervical screening by Indigenous status was developed by Professor John Condon and endorsed by First Nations representatives and NACCHO. A review has confirmed that the alternative methodology is robust and appropriate, but cannot overcome the degree of missing Indigenous status data in the NCSR to support meaningful participation data. Work continues to progress this reporting priority (AIHW 2025b).
The most recent cervical screening data from the National Key Performance Indicators Data Collection show that, as at June 2025, 51% (53,845) of regular First Nations female clients aged 25–74 of First Nations-specific primary health care services (who had not had a hysterectomy) had a cervical screening test in the previous 5 years. The proportion was lowest in Inner regional and Outer regional areas (47% and 48%, respectively) and higher in Major cities (53%) and Remote and Very remote areas (53% and 55%, respectively) (Table D3.04.27). Proportions also varied by jurisdiction, ranging from 43% (2,543) in South Australia, to 59% (8,341) in Western Australia (Table D3.04.28).
The 2022–23 National Aboriginal and Torres Strait Islander Health Survey (NATSIHS) collected self-reported data on Pap smear tests to check for cervical cancer among First Nations women aged 25–74. While at the time of the survey, the 2 yearly Pap smear had been replaced by the five yearly Cervical Screening Test, the ABS decided to maintain the existing terminology for the 2022–23 survey. Instead, a new question was added on testing frequency, and changes in terminology will be considered for a future iteration of the survey.
In the 2022–23 NATSIHS, 65% (151,000) of First Nations women aged 25–74 reported having had a Pap smear test at least every 5 years. Proportions varied by remoteness area, from 60% (12,300) in Very remote areas to 72% (10,500) in Remote areas (Table D3.04.15, Table D3.04.16, Figure 3.04.1).
Figure 3.04.1: First Nations women aged 25–74 reporting whether had a Pap smear test to check for cervical cancer at least every 5 years, by remoteness, 2022–23
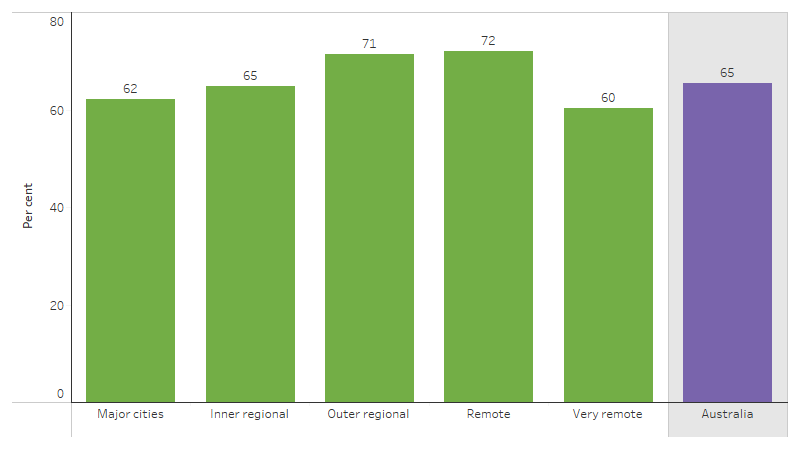
Source: Table D3.04.15. AIHW and ABS analysis of National Aboriginal and Torres Strait Islander Health Survey 2022–23.
National Bowel Cancer Screening Program
Over the period January 2022 to December 2023, a total of 2,616,787 Australians returned a valid screening test in the National Bowel Cancer Screening Program (NBCSP). Of the 1,453,354 valid screening tests returned in 2023, 25,219 (1.7%) were from those who identified as Indigenous (94% were from those who identified as non-Indigenous, and the remaining 4.3% were from those with no Indigenous status identified) (AIHW 2025a: Table A3.9).
To determine participation rates by Indigenous status, the number of screening invitations sent out by Indigenous status is also needed. At present, this information isn’t available, so must be estimated. To estimate the number of invitations sent out to First Nations people, the percentages of those aged 50–74 who reported being First Nations in the 2021 Census was applied to the number of overall invitations (by age group and sex). However, the proportion of ‘not stated’ results between the 2021 Census and NBCSP participation data differs, so care must be taken when interpreting these data (see Appendix C of AIHW 2025a).
The estimated participation rate in the NBCSP for First Nations people aged 50–74 was 38% in 2022–2023. This was 4 percentage points lower than the estimated participation rate of 42% for non-Indigenous Australians. Given the limitations in the data available to estimate First Nations participation in the NBCSP, caution should be used when interpreting these data (AIHW 2025a).
In 2023, First Nations participants were more likely to receive a positive Immunochemical faecal occult blood test (iFOBT) result – meaning detection of blood in a faecal sample – than non-Indigenous participants (8.0% and 5.8%, respectively). However, First Nations participants with a positive result had a lower rate of follow-up colonoscopy (78% compared with 86%) and a longer median time between a positive screening result and a diagnostic assessment (78 days compared with 62 days, respectively) (AIHW 2025a) (Table 3.04-1).
Table 3.04-1: Summary of National Bowel Cancer Screening Program screening, results and assessments, people aged 50–74, by Indigenous status, 2023
|
Number |
First Nations |
Non-Indigenous |
|---|---|---|
|
Screened |
25,219 |
1,365,638 |
|
Positive iFOBT result |
2,026 |
78,951 |
|
Diagnostic assessment (colonoscopy) |
1,575 |
68,172 |
|
Rates (%) |
First Nations |
Non-Indigenous |
|---|---|---|
|
iFOBT positivity rate |
8.0 |
5.8 |
|
Diagnostic assessment rate |
77.7 |
86.3 |
|
Time between positive screen and assessment (days) |
First Nations |
Non-Indigenous |
|---|---|---|
|
Median |
78 |
62 |
|
90th percentile |
170 |
149 |
Source: Tables A3.9, A3.13, A3.21 (AIHW 2025a). National Bowel Cancer Screening Program monitoring report 2025.
Self-reported data from the 2022–23 NATSIHS indicates that 25% (19,400) of First Nations males and 20% (17,400) of First Nations females aged 50–74 had at least one bowel cancer screening test in their lifetime (Table D3.04.17).
Other cancer screening
The 2022–23 NATSIHS showed that 52% (44,100) of First Nations males aged 50 and over reported having been tested for prostate cancer at least once (Table D3.04.19). Of First Nations adults, 9.8% (58,100) had been tested at least once for skin cancer, and 2.3% (13,900) had participated in a lung cancer screening test (Table D3.04.18).
Change over time
Health checks
Between 2015–16 and 2023–24, the number of First Nations people accessing health assessments through the MBS increased from 191,526 to 259,941. The uptake of these health assessments (the number of patients receiving at least one of these services divided by the First Nations population at 30 June) nationally did not change significantly over this period, with a low of 21% in 2021–22, associated with the COVID-19 pandemic, and high of 25% in 2023–24. The only age group that saw a statistically significant change in the uptake of health assessments over this period was those over 50, where uptake increased by 17% between 2015–16 and 2023–24 (Table D3.04.7).
For more detailed analysis of the impact of COVID-19 on the uptake of health assessments, including the impact of telehealth, see Indigenous-specific health checks during the COVID-19 pandemic (AIHW 2023).
New South Wales and Tasmania were the only jurisdictions to show statistically significant increases in uptake over this period (27% and 101% increase, respectively) (Table D3.04.3). Looking at uptake by remoteness area, there was a statistically significant increase in the uptake of health assessments in Major cities over the period (31% increase), while there was a statistically significant decrease in the uptake in Remote areas (30% decrease). Other remoteness areas did not have statistically significant changes in the uptake of health assessments (Table D3.04.4, Figure 3.04.2).
Figure 3.04.2: Rate of MBS health checks/assessments for First Nations people, by remoteness area, 2015–16 to 2023–24
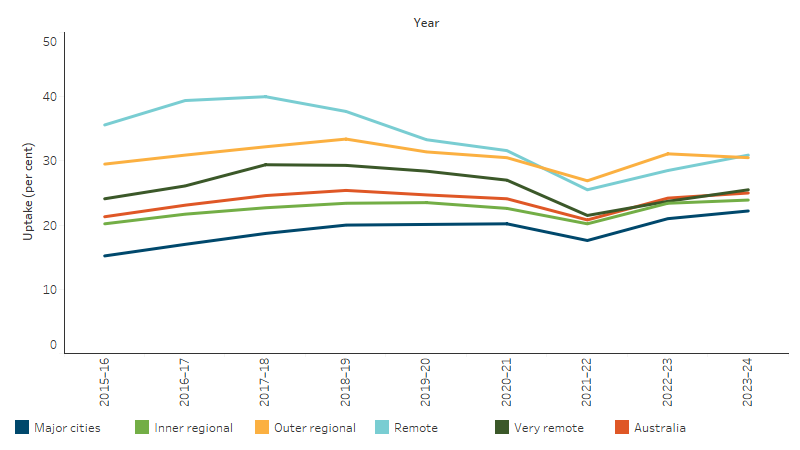
Source: Tables D3.04.4. AIHW analysis of Department of Health Medicare claims data.
Breast cancer screening
The BreastScreen Australia Program offers a free mammogram every 2 years for women aged 40 and over, and actively invites women aged 50–74. Data are only presented here for the target age range of 50–74 years.
The proportion of First Nations women in the target age range of 50–74 years screened for breast cancer showed no statistically significant change between 2016–2017 (32%) and 2022–2023 (36%). There was a low in 2020–2021, where the proportion dropped to 31%, likely due to the impact of the COVID-19 pandemic from March 2020 (Table D3.04.12).
Between 2016–2017 and 2022–2023, the age-standardised rate of First Nations women aged 50–74 who received breast cancer screening also showed no statistically significant change, ranging from 33% in 2016–2017 to 36% in 2022–2023. Similarly, the proportion for non-Indigenous women aged 50–74 remained relatively constant between 2016–2017 (55%) and 2022–2023 (51%).
However, there was a statistically significant 7 percentage point reduction in the absolute gap in breast screening participation rates between First Nations women and non-Indigenous women from 2016–2017 (22 percentage points gap) to 2022–2023 (15 percentage points gap). The relative gap (rate ratio) increased over this period, from 0.6 to 0.7, indicating an improvement in the rate of screening for First Nations women relative to non-Indigenous women (Table D3.04.12, Figure 3.04.3).
Figure 3.04.3: Age-standardised participation rates, BreastScreen Australia Program, women aged 50–74, by Indigenous status, 2016–2017 to 2022–2023
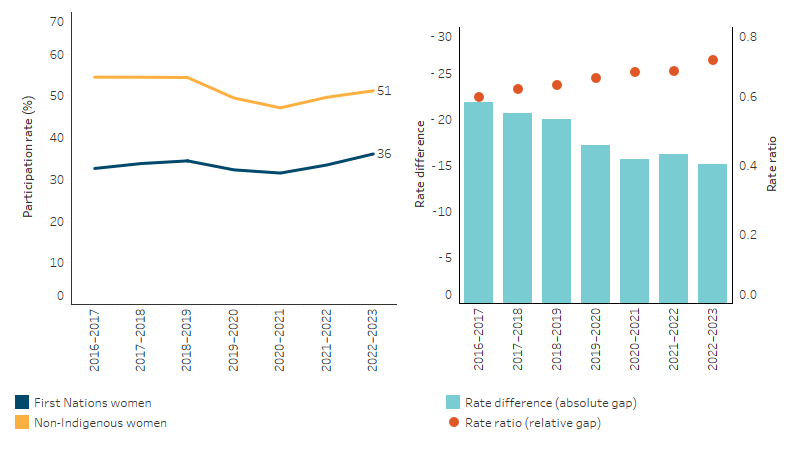
Note: Rate difference is the age-standardised rate (per cent) for First Nations people minus the age-standardised rate (per cent) for non-Indigenous Australians. Rate ratio is the age-standardised rate for First Nations people divided by the age-standardised rate for non-Indigenous Australians.
Source: Table D3.04.12. AIHW analysis of BreastScreen Australia data.
Cervical screening
Data from the National Key Performance Indicators Data Collection show that the proportion of regular female clients aged 25–74 of First Nations-specific primary health care services (who had not had a hysterectomy) who had a cervical screening test in the previous 5 years has been increasing over time – from 38% as at December 2020 to 51% as at June 2025. This increase has been consistent across age groups (AIHW 2026: Table S2.94).
Research and evaluation findings
Existing research has identified persistent barriers and effective enablers of preventative health care delivery and screening for First Nations people. Evidence from systematic reviews, program evaluations and national studies shows that while effective models exist, outcomes remain strongly shaped by service accessibility, cultural safety, and broader socioeconomic and structural factors.
A study examined the delivery of recommended preventive services for First Nations people and investigated the influence of health service and client level factors on adherence to best practice guidelines. The study highlighted that the delivery of recommended preventive care varied widely between different preventive services, with good delivery of most of the basic measurements but poor follow-up of abnormal findings. The study found that health service characteristics associated with higher quality care were found in the Northern Territory, urban services and centres that serve smaller populations. The study also reported that clients aged 25–34, women, and those who attended the health centre more regularly tended to have higher recorded delivery of the recommended preventive services. The study provided insights for improving the quality of preventive care for First Nations people and highlighted the benefit of Continuous Quality Improvement processes in identifying and addressing areas for improved service delivery (Bailie et al. 2016).
An evidence mapping review examined factors influencing the implementation of health checks for First Nations people in Australian primary health care. Based on 16 peer-reviewed studies and 5 sources of grey literature, the review identified key barriers such as physical space constraints, competing demands, a focus on acute care over prevention, complex Medicare billing processes, limited cultural competency among staff, inconsistent identification of Indigenous status, patient concerns regarding privacy, trust, and fear of stigma. Key enablers included strong clinical leadership, participation of culturally competent and Indigenous staff, flexible service delivery (for example walk-ins and transport support), digital health check systems, and active community engagement through culturally appropriate communication and materials (Yadav et al. 2025).
A systematic review of cancer studies explored knowledge, attitudes and behaviours towards cancer screening among Indigenous people worldwide. Cancer death among Indigenous people is increasing, but these populations commonly under-use cancer screening services. The review found that knowledge of and participation in screening was greater for breast cancer than for other cancers. It also found that Indigenous people tended to have less knowledge of and less favourable attitudes to screening, and a higher propensity to refuse screening than non-Indigenous populations. The review suggested that greater understanding of knowledge, attitudes and behaviours towards cancer screening in diverse Indigenous cultures is needed so that culturally appropriate cancer prevention programs can be provided (Kolahdooz et al. 2014).
In Australia, First Nations people are more likely to be diagnosed with cancer at later stages and have lower five-year survival rates. In 2014–2018, the five-year survival rate for all cancers was 44% for males and 52% for females, compared with 58% and 63% for non-Indigenous Australian males and females. This disparity contributes to a widening gap in cancer mortality, with First Nations cancer death rates increasing by 12% between 2010 and 2019, while rates declined by 10% for non-Indigenous Australians. Over 50% of the cancer burden for the First Nations population is attributable to modifiable risk factors, with tobacco use alone accounting for 37% of the cancer burden (AIHW 2022; Cancer Australia 2024). This suggests that concerted yet appropriate efforts targeting these risk factors will lead to measurable improvements over the longer term.
Socioeconomic disadvantage, including lower income, education and housing insecurity, is associated with reduced access to timely screening and treatment (AIHW 2024c). First Nations people living in the most disadvantaged areas are up to 39% more likely to die from cancer compared with those in advantaged areas (Bygrave et al. 2020). Participation in programs such as bowel cancer screening remains lower among First Nations populations, with delays in follow-up care often linked to remote location and socioeconomic disadvantage (AIHW 2025b). Structural factors, including systemic racism, intergenerational trauma and economic marginalisation, further exacerbate these inequities, while variability in preventive care delivery across health services reflects resource constraints and community disadvantage (Bailie et al. 2017; Ngampromwongse and Gall 2025).
Participation in cancer screening programs, such as the National Bowel Cancer Screening Program (NBCSP), BreastScreen Australia, and the National Cervical Screening Program (NCSP), remains lower among First Nations people compared to non-Indigenous Australians (AIHW 2024b, 2025a).
It is known that First Nations women experience lower levels of participation in cervical screening and a disproportionately higher burden from cervical cancer than non-Indigenous women. Detection of high-grade cervical abnormalities among First Nations participants was higher than non-Indigenous participants, at 11.8 and 7.7 with a high-grade abnormality detected on histology per 1,000 screened, after adjusting for age. The colposcopy (cervical examination) rate of participants who are at higher risk of a significant cervical abnormality differed across remoteness areas, from 57% for First Nations women residing in Major cities compared with 26% for First Nations women residing in Very remote areas (AIHW 2024d).
Health care providers report a range of challenges in delivering cervical screening, including providing culturally sensitive engagement, trust-building, workforce limitations, and cumbersome recall systems, noting that while patient self-collection could improve screening uptake it had faced implementation delays (Jaenke et al. 2021). From the perspective of under-screened First Nations women, barriers to participation include distress and trauma associated with the procedure, lack of privacy and control, complex relationships with providers, and culturally unsafe or pressured communication. These findings were revealed in a culturally safe Yarning session about cervical screening, after which some of the women then participated in screening (within 30 days of the session), suggesting Yarning may support women’s decisions to screen. The study also highlighted the potential for self-collection for cervical screening for maintaining privacy and autonomy, although awareness of this option remains limited (Butler et al. 2022).
First Nations women are disproportionately represented in areas with limited access to BreastScreen Australia screening services. While 96% of First Nations women aged 50–74 live within a one-hour drive of a breast screening site, they are more likely than non-Indigenous women to live in areas with limited access to regular screening services. Nationally, First Nations women make up 2.3% of women in this age group, but in regions located more than 2 hours from the nearest screening site, they represent 57% of this population. Although breast screening is recommended every 2 years, the key concern is the geographic accessibility of services, which may impact participation regardless of the recommended screening interval (AIHW 2024a).
The Beautiful Shawl Project is a culturally safe breast screening initiative led by BreastScreen Victoria in partnership with the Victorian Aboriginal Community Controlled Health Organisation (VACCHO). The project provides culturally designed shawls, created by First Nations artists, for women to wear during breast screening, helping to create a more respectful and comfortable experience. Since its launch in 2018, the project has supported 1,342 breast screens. Between July 2023 and June 2024, it partnered with 22 Aboriginal Community Controlled Organisations – an 83% increase from the previous year – to deliver 612 breast screens. Of these, 40% were first-time participants, 26% were overdue, and 34% were screened on time, demonstrating the project's success in improving access and participation in breast screening (VACCHO 2024).
A literature review identified barriers for Indigenous participation in bowel/colorectal cancer-screening programs, some of which appear to be unique to Indigenous people. The review studied the Indigenous populations of Canada, New Zealand, Australia and the United States. The review found that Indigenous populations have common barriers for screening, such as lack of access to culturally competent health services, discrimination, distrust of Western medicine and distrust of screening tests (D'onise et al. 2020).
In Australia, geographic constraints also play a role in participation in bowel cancer screening: home-based faecal occult blood test (FOBT) kits are temperature-sensitive, and the ‘hot zone policy’ prevents mailing kits to areas with average monthly temperatures above 30°C during certain periods of the year – regions that are typically remote and have higher First Nations populations (Worthington et al. 2023). To address these issues, the NBCSP introduced an ‘Alternative Access Model’, enabling immunochemical FOBT kits to be provided directly by local health services. Evaluation of the National Indigenous Bowel Screening Pilot found this approach nearly doubled First Nations participation compared to the usual mail-out method (40% compared with 23%), achieved faster kit returns (13 compared with 34 days), and reached under-screened groups. Patients and health staff reported that receiving kits in culturally safe settings removed barriers and improved engagement (Menzies School of Health Research 2020).
Biomedical data from the 2012–13 National Aboriginal and Torres Strait Islander Health Measures Survey (NATSIHMS) showed that cardiovascular disease (CVD) risk is high among First Nations adults, with 15.7% of those aged 35–74 at high absolute risk of a primary CVD event and 9.6% having had prior CVD. High risk was also found among 1.1% of those aged 18–24 and 4.7% of those aged 25–34. Most high-risk individuals were identified based on clinical criteria such as having diabetes, very high total cholesterol (greater than 7.5 mmol/L) and kidney disease. However, undertreatment was common – only 42% of those at high risk were using lipid-lowering medication. These findings indicate substantial early risk and treatment gaps in this population, highlighting the need for earlier detection and improved management to prevent CVD events (Calabria et al. 2018). At the time of the study, there were no national level recommendations regarding absolute CVD risk assessment for First Nations people aged under 35, thus potentially missing a substantial number of people at risk. However, the Aboriginal Community Controlled Health sector and other General Practice organisations were already recommending changes in preventive health assessments towards younger age groups (Agostino et al. 2020). Since then, Heart Foundation guidelines have adjusted the recommended age for commencing cardiovascular risk assessment for First Nations people. Risk factor screening should begin from 18 years, and absolute CVD risk assessment should commence from 30 years, rather than 35 years. This adjustment reflects the earlier onset and higher prevalence of CVD among First Nations communities and aims to improve early detection and preventive care (National Heart Foundation of Australia 2023).
The Evaluation of Outreach Programs found that mobile and outreach services have contributed to improving access to health care and screening in rural and remote communities. This includes initiatives such as mobile breast cancer screening, telehealth-enabled screening for diabetic retinopathy and ENT conditions, and outreach women’s health clinics providing cervical screening and breast examinations. Between 2017–18 and 2020–21, the gap in service access between metropolitan/regional centres (Modified Monash Model categories 1–2) and very remote communities (category 7) was reduced by 13.1% for medical specialists and 16.4% for allied health services. Case studies, such as True Women’s Health Service in Queensland, highlight how outreach models actively engage communities, build trust, and deliver culturally safe sexual health and screening services, including contraception advice and pregnancy planning. These services not only support diagnosis and management but also facilitate earlier identification of chronic conditions and cancer through increased availability of health professionals in underserved areas (Health Policy Analysis 2022).
Implications
Early detection and timely treatment through culturally safe, community-led primary health care delivers substantial benefits for First Nations people. Primary health care provides significant benefits for individuals at risk of disease. Identifying First Nations patients is the first step in enabling access to First Nations-specific health initiatives, including additional Medicare Benefits Schedule (MBS) and Pharmaceutical Benefits Scheme (PBS) items, immunisations and preventive care. Health checks, particularly MBS item 715, support comprehensive, culturally tailored assessments that reflect the holistic health needs of First Nations people. However, barriers remain, including under-identification of Indigenous status, limited staff training, and inconsistent follow-up. Improving the follow-up of abnormal clinical results and access to referral services is also critical to achieving the benefits of health assessments and screening programs (Bailie et al. 2016; Bailie et al. 2014; Spurling et al. 2009; Whop et al. 2016).
First Nations people living in regional and rural areas often face additional barriers to accessing screening and preventive care, particularly where services are delivered through private general practices. Cost, transport and limited availability of culturally safe services contribute to inequities in access. Health care providers report that these challenges are compounded by high workloads, underfunding and staff turnover (Taylor et al. 2024).
In the 2025–26 Budget, the Australian Government has continued its commitment to early detection and treatment of chronic and preventable conditions through several key initiatives. An additional $3.5 million was allocated in 2025–26 to extend the Deadly Choices initiative, continuing support for First Nations-specific health assessments. While this represents ongoing investment, further targeted funding is likely to be needed to address persistent gaps in early detection and follow-up care.
Recent national reporting highlights the role of Aboriginal Community Controlled Health Organisations (ACCHOs) and other First Nations-specific primary health care providers in delivering early intervention and preventive care. In 2023–24, there were 213 organisations that provided First Nations-specific primary health care services across Australia, funded under the Indigenous Australians’ Health Programme (IAHP). Of these, 69% (147) were ACCHOs, which are governed and operated by First Nations communities. The remaining 31% (66) were other service providers, including government-run and non-government organisations. Collectively, these organisations delivered over 4.2 million episodes of care, with a strong focus on chronic disease screening, risk factor management, and culturally safe health care. The national Key Performance Indicators (nKPIs) include nine preventive health measures aimed at the early detection, prevention, and management of chronic dis ease among First Nations people. The data indicates a positive trajectory in preventive health engagement, particularly in early detection and chronic disease management. For example, participation in health checks is increasing among younger age groups, reflecting efforts to promote early intervention (AIHW 2026). The Quality Assurance for Aboriginal and Torres Strait Islander Medical Services (QAAMS) program provides rapid, on-site diabetes testing in remote communities. This point-of-care model enables immediate results and timely intervention, reducing delays in diagnosis and supporting early treatment.
General practitioners (GPs) and ACCHOs play a pivotal role in assessing health risks, providing patient education, encouraging screening and instituting prompt referrals which are essential in reducing cancer morbidity and mortality (Parkin et al. 2018). However, systemic barriers, such as geographic remoteness, limited culturally safe services, and fragmented care, continue to affect timely diagnosis and treatment.
Participation in cancer screening programs, such as the National Bowel Cancer Screening Program (NBCSP), BreastScreen Australia, and the National Cervical Screening Program (NCSP), remains lower among First Nations people compared to non-Indigenous Australians (AIHW 2024b, 2025a).
Strategies to improve screening participation include culturally safe, community-led approaches such as the National Indigenous Bowel Screening Pilot, which demonstrated higher uptake through primary health care centres compared to standard mail-out, leading to the NBCSP’s health care provider-led alternative access to kits model introduced in 2022 (Garvey et al. 2020). Cervical cancer remains a priority, with self-collection introduced in July 2022 driving uptake among First Nations participants from 4% to nearly 56% by late 2024, supported by culturally tailored resources and language translations (Department of Health and Aged Care 2022). Further initiatives, including the National Strategy for the Elimination of Cervical Cancer in Australia by 2035 and Point of Care HPV Testing for Cervical Screening in Aboriginal and Torres Strait Islander Communities, aim to improve access and equity in screening.
Cervical screening will remain vital for some years to come because the current HPV vaccines are not effective against all types of the virus that cause cervical cancer. A barrier to reporting on the national cervical screening rate for First Nations women is that Indigenous status information is not collected on pathology forms in all jurisdictions.
Recognising the disproportionate impact of lung cancer in First Nations people, the 2023-24 Budget announcement for the National Lung Cancer Screening Program (NLCSP) included specific funding to enable the National Aboriginal Community Controlled Health Organisation (NACCHO) to co-design the NLCSP with and for First Nations participants. This co-design has resulted in the development of culturally appropriate and tailored materials and processes to support Aboriginal Health Workers and to support First Nations people participating in the NLCSP.
The NLCSP Quality Framework, published in December 2025, outlines how the NLCSP should be measured, monitored and evaluated. It sets out the principles, standards and performance measures required to maintain high-quality program management and service delivery. The first annual monitoring report is expected to be released in June 2027 to allow for sufficient time to collect and analyse data on program performance, including adherence to quality standards, participant outcomes, and service delivery processes.
Implementation of the National Aboriginal and Torres Strait Islander Health Plan 2021-31 (the Health Plan) aims to drive structural reform towards models of care that are prevention and early intervention focused, with greater integration of care systems and pathways across primary, secondary and tertiary care. It also emphasises the need for mainstream services to address racism and provide culturally safe and responsive care, and be accountable to First Nations people and communities. Priority 5 of the Health Plan focuses on early intervention, with the desired outcome of ensuring that early intervention approaches are accessible to First Nations people and provide timely, high quality, effective and culturally safe and responsive care. Objective 5.6 focuses specifically on improving cancer screening and care pathways through culturally safe services, accessible information, and community-driven awareness initiatives.
Continued implementation of the National Aboriginal and Torres Strait Islander Cancer Framework and the Optimal Care Pathway for Aboriginal and Torres Strait Islander People with Cancer is essential to ensuring equitable access to cancer care and improving outcomes. The Aboriginal and Torres Strait Islander Cancer Plan 2023, developed through extensive national consultation, reinforces the importance of co-design, community leadership, and shared decision-making. It aligns with the Health Plan’s vision for culturally safe, effective, and community-led health services (NACCHO 2023). The Optimal Care Pathway for Aboriginal and Torres Strait Islander People with Cancer (2nd ed.) highlights the importance of improving screening participation for First Nations people in ways that are culturally safe, respectful of Men’s and Women’s Business, co-designed by First Nations people, address privacy concerns of clients through establishing trust, and backed up by dedicated staff and systems to aid recall and reminders, and service quality improvement initiatives (Cancer Australia 2024).
The Commonwealth Closing the Gap 2024 Annual Report and 2025 Implementation Plan outlines a significant investment to improve cancer outcomes for First Nations people. This includes the recruitment of up to 210 new First Nations health care positions to support cancer care, including access to chemotherapy closer to home. These roles also aim to build viable career pathways and facilitate culturally safe care on Country.
Improving early detection and treatment outcomes requires a sustained commitment to culturally safe, community-led, and strengths-based approaches. Central to this is the recognition of First Nations leadership, knowledge systems, and self-determination in shaping health policy and service delivery. Mainstream health services must work in genuine partnership with ACCHOs, embedding cultural safety, accountability, and equity at every level. Addressing systemic racism, improving Indigenous identification in screening registers, and ensuring continuity of care are essential to enhancing early diagnosis and treatment outcomes for First Nations people.
References
- Agostino JW, Wong D, Paige E, Wade V, Connell C, Davey ME, Peiris DP, Fitzsimmons D, Burgess CP and Mahoney R (2020) 'Cardiovascular disease risk assessment for Aboriginal and Torres Strait Islander adults aged under 35 years: a consensus statement', The Medical Journal of Australia, 212(9):422–427, doi:10.5694/mja2.50529.
- AIHW (Australian Institute of Health and Welfare) (2020) Cancer screening and COVID-19 in Australia, AIHW, Australian Government.
- AIHW (2022) Australian Burden of Disease Study: impact and causes of illness and death in Aboriginal and Torres Strait Islander people 2018, AIHW, Australian Government, accessed 30 March 2026, doi:10.25816/xd60-4366.
-
AIHW (2023) Indigenous-specific health checks during the COVID-19 pandemic, AIHW, Australian Government, accessed 27 March 2026.
-
AIHW (2024a) Access to BreastScreen Australia screening services, AIHW, Australian Government, accessed 8 April 2026.
-
AIHW (2024b) BreastScreen Australia monitoring report 2024, AIHW, Australian Government, accessed 8 April 2026.
-
AIHW (2024c) Determinants of health for First Nations people, AIHW, Australian Government, accessed 31 March 2026.
-
AIHW (2024d) National Cervical Screening Program monitoring report 2024, AIHW, Australian Government, accessed 8 April 2026, doi:10.25816/1smm-mp67.
-
AIHW (2025a) National Bowel Cancer Screening Program monitoring report 2025, AIHW, Australian Government, accessed 8 April 2026.
-
AIHW (2025b) National Cervical Screening Program monitoring report 2025, AIHW, Australian Government, accessed 27 March 2026.
-
AIHW (2026) Aboriginal and Torres Strait Islander specific primary health care: results from the OSR and nKPI collections, AIHW, Australian Government, accessed 12 March 2026.
-
Bailie C, Matthews V, Bailie J, Burgess P, Copley K, Kennedy C, Moore L, Larkins S, Thompson S and Bailie R (2016) 'Determinants and gaps in preventive care delivery for Indigenous Australians: a cross-sectional analysis', Frontiers in Public Health, 4:34, doi:10.3389/fpubh.2016.00034.
-
Bailie J, Matthews V, Laycock A, Schultz R, Burgess CP, Peiris D, Larkins S and Bailie R (2017) 'Improving preventive health care in Aboriginal and Torres Strait Islander primary care settings', Globalization and Health, 13:48, doi:10.1186/s12992-017-0267-z.
-
Bailie J, Schierhout G, Kelaher M, Laycock A, Percival N, O’Donoghue L, McNeair T, Chakraborty A, Beacham B and Bailie R (2014) 'Follow-up of Indigenous-specific health assessments — a socioecological analysis', The Medical Journal of Australia, 200(11):653–657, doi:10.5694/mja13.00256.
-
Butler TL, Lee N, Anderson K, Brotherton JML, Cunningham J, Condon JR, Garvey G, Tong A, Moore SP, Maher CM, Mein JK, Warren EF and Whop LJ (2022) 'Under-screened Aboriginal and Torres Strait Islander women’s perspectives on cervical screening', PloS One, 17(8):e0271658, doi:10.1371/journal.pone.0271658.
-
Bygrave A, Whittaker K and Aranda S (2020) Inequalities in cancer outcomes by Indigenous status and socioeconomic quintile: An integrative review, Cancer Council Australia.
-
Calabria B, Korda RJ, Lovett RW, Fernando P, Martin T, Malamoo L, Welsh J and Banks E (2018) 'Absolute cardiovascular disease risk and lipid-lowering therapy among Aboriginal and Torres Strait Islander Australians', The Medical Journal of Australia, 209(1):35–41, doi:https://doi.org/10.5694/mja17.00897.
-
Cancer Australia (2024) Optimal care pathway for Aboriginal and Torres Strait Islander people with cancer. 2nd edn, Cancer Australia.
-
Clinical Principal Committee Standing Committee on Screening (2018) Population based Screening framework, Department of Health, Australian Government.
-
D'onise K, Iacobini ET and Canuto KJ (2020) 'Colorectal cancer screening using faecal occult blood tests for Indigenous adults: A systematic literature review of barriers, enablers and implemented strategies', Preventive Medicine, 134:106018.
-
Department of Health and Aged Care (2022) National Cervical Screening Program – National Cervical Screening Policy, Department of Health and Aged Care, Australian Government.
-
Garvey G, Brands J, Tighe B, Westby M and Arley B (2020) National Indigenous Bowel Screening Pilot - FINAL REPORT, Department of Health and Aged Care.
-
Health Policy Analysis (2022) Evaluation of Outreach Programs: Evaluation Report Volume 1 – Main Report, Department of Health and Aged Care.
-
Jaenke R, Butler TL, Condon J, Garvey G, Brotherton JML, Cunningham J, Anderson K, Tong A, Moore SP and Whop LJ (2021) 'Health care provider perspectives on cervical screening for Aboriginal and Torres Strait Islander women: a qualitative study', Australian and New Zealand Journal of Public Health, 45(2):150–157, doi:https://doi.org/10.1111/1753-6405.13084.
-
Kidney Health Australia (2020) Chronic Kidney Disease (CKD) Management in Primary Care (4th edition), Kidney Health Australia.
-
Kolahdooz F, Jang SL, Corriveau A, Gotay C, Johnston N and Sharma S (2014) 'Knowledge, attitudes, and behaviours towards cancer screening in indigenous populations: a systematic review', The Lancet Oncology, 15(11):e504–e516.
-
Menzies School of Health Research (2020) Final report on the National Indigenous Bowel Screening Pilot, report to Department of Health and Aged Care, Australian Government.
-
NACCHO (National Aboriginal Community Controlled Health Organisation) (2023) Aboriginal and Torres Strait Islander Cancer Plan, NACCHO.
-
National Heart Foundation of Australia (2023) Guideline for assessing and managing cardiovascular disease risk and Australian CVD risk calculator, National Heart Foundation of Australia website, accessed 23 December 2025.
-
Ngampromwongse K and Gall A (2025) '10 years of preventive health in Australia. Part 2 – centring First Nations sovereignty', Public Health Research & Practice, 35(2):PU24023, doi:10.1071/PU24023.
-
Parkin CJ, Bell SW and Mirbagheri N (2018) 'Colorectal cancer screening in Australia', Australian Journal of General Practice, 47(12):859.
-
RACGP (Royal Australian College of General Practitioners) and Diabetes Australia (2024) Management of type 2 diabetes: a handbook for general practice, RACGP, accessed 26 March 2026.
-
Spurling G, Hayman NE and Cooney AL (2009) 'Adult health checks for Indigenous Australians: the first year's experience from the Inala Indigenous Health Service', The Medical Journal of Australia, 190(10):562–564, doi:10.5694/j.1326-5377.2009.tb02563.x.
-
Taylor EV, Dugdale S, Connors CM, Garvey G and Thompson SC (2024) '“A Huge Gap”: Health Care Provider Perspectives on Cancer Screening for Aboriginal and Torres Strait Islander People in the Northern Territory', International Journal of Environmental Research and Public Health, 21(2):141, doi: 10.3390/ijerph21020141.
-
VACCHO (Victorian Aboriginal Community Controlled Health Organisation) (2024) The Beautiful Shawl Project (BSP) June 2023 to June 2024 infographic, VACCHO.
-
WHO (World Health Organisation) (2023) Reducing risks and detecting early to prevent and manage noncommunicable diseases, WHO, accessed 13 October 2025.
-
WHO (n.d.) Management of noncommunicable diseases, WHO website, accessed 13 October 2026.
-
Whop LJ, Baade P, Garvey G, Cunningham J, Brotherton JML, Lokuge K, Valery PC, O’Connell DL, Canfell K, Diaz A, Roder D, Gertig DM, Moore SP and Condon JR (2016) 'Cervical Abnormalities Are More Common among Indigenous than Other Australian Women: A Retrospective Record-Linkage Study, 2000–2011', PloS One, 11(4):e0150473, doi:10.1371/journal.pone.0150473.
-
Worthington J, Lew J-B, He E, Broun K, D'Onise K, Grogan P, Canfell K and Feletto E (2023) 'The ‘hot zone policy’ for colorectal cancer screening presents unique risks and opportunities for rural Australia', Australian Journal of Rural Health, 31(3):580–586, doi:https://doi.org/10.1111/ajr.12977.
-
Yadav U, Thottunkal S, Agostino J, Sinka V, Wyber R, Hammond B, Butler D, Beiraghi M, Freeman K, Passey M, Wake E, Smith M, Jones B, Lovett R and Douglas K (2025) 'What influences the implementation of health checks in the prevention and early detection of chronic diseases among Aboriginal and Torres Strait Islander people in Australian primary healthcare: findings from an evidence mapping review', Health Research Policy and Systems, 23(70), doi:10.1186/s12961-025-01325-9.
-
Zwar N and Ackermann E (2016) Guidelines for preventive activities in general practice, 2016, The Royal Australian College of General Practitioners, The Royal Australian College of General Practitioners.

