Key messages
Why is it important?
A significant proportion of deaths among Aboriginal and Torres Strait Islander (First Nations) people are from avoidable causes such as coronary heart disease, diabetes, respiratory disease and suicide . Avoidable mortality serves as a key indicator of the quality, effectiveness, and accessibility of the health system, as well as the effectiveness of disease and risk factor prevention efforts (such as smoking cessation). Understanding the causes of avoidable deaths and the social and cultural determinants provides context to support the design, resourcing, delivery and improvement of targeted programs and services to improve outcomes for First Nations people and close the gap.
Data findings
- In the period 2019–2023, in the 5 jurisdictions where Indigenous identification was of adequate quality there were 8,972 deaths of First Nations people aged 0–74 from potentially avoidable causes. This represents 59% of all deaths of First Nations people aged 0–74, and equates to a rate of 211 deaths per 100,000 population.
- In 2019–2023, in the 5 jurisdictions where Indigenous identification was of adequate quality, First Nations males were more likely to die from potentially avoidable causes than First Nations females (244 and 179 per 100,000 population, respectively).
- Three conditions contributed to more than half of the avoidable mortality gap between First Nations people and non-Indigenous Australians – coronary heart disease (23% of the gap), diabetes (18% of the gap) and chronic obstructive pulmonary disease (14% of the gap).
- Based on age-standardised rates, the gap in potentially avoidable mortality between First Nations people and non-Indigenous Australians was higher in Remote and very remote areas than in Major cities and Inner and outer regional areas (rate difference of 344 compared with 153 and 149 deaths per 100,000 population, respectively).
- The largest relative difference in rates of potentially avoidable deaths between First Nations people and non-Indigenous Australians was for diabetes with a rate for First Nations people 8 times that of non-Indigenous Australians (42 and 5 deaths per 100,000 population).
Research and evaluation findings
- Regular and comprehensive health checks enable early identification and management of chronic conditions such as cardiovascular disease, diabetes, and chronic obstructive pulmonary disease – which are among the leading contributors to avoidable deaths among First Nations people. However, there is wide variability in the delivery of primary health care and preventive services for First Nations people in Australia.
- In 2018, modifiable risk factors accounted for 49% of the total (fatal and non-fatal) burden of disease for First Nations people, with tobacco use being the leading risk factor, contributing to 23% of deaths, 12% of total burden (DALY) and 19% of fatal burden (YLL).
- Evidence from remote Northern Territory communities has shown that higher primary care use can reduce avoidable hospitalisations and deaths from renal and heart disease by up to 85%, and every $1 invested in care can save up to 12 times that in hospital costs. Barriers to access to health services include geographic isolation, affordability, service availability, cultural safety, and limited awareness, while enablers include community-led and self-determined approaches.
- Overcrowded housing is associated with increased avoidable hospitalisations, reflecting broader systemic, socioeconomic and environmental challenges.
- An evaluation of the Indigenous Australians’ Health Program showed that it provides critical investment in primary health care for First Nations people, particularly through Aboriginal Community Controlled Health Services (ACCHSs). However, the report also stated that funding was too low for ACCHSs to consistently deliver values-aligned care.
Implications
A broad range of risk factors and conditions such as smoking, injury, mental health issues, substance use disorders, heart disease, diabetes, respiratory disease, and renal disease all require service responses across the health-care continuum from prevention to tertiary care. Efforts to address the social determinants of health also remain fundamental in preventing avoidable deaths. The findings in this measure highlight the critical role of ACCHSs in reducing avoidable deaths among First Nations people. ACCHSs deliver culturally safe, comprehensive care, which is particularly important for chronic disease prevention and management. Expanding these services to address gaps in primary health care – alongside sustained investment in early intervention – is essential to closing the health gap and achieving the outcomes outlined in the National Aboriginal and Torres Strait Islander Health Plan 2021–2031 and the National Agreement on Closing the Gap.
Why is it important?
Avoidable and preventable deaths refers to deaths from conditions that are considered avoidable given timely and effective health care (including disease prevention and population health initiatives) (AIHW 2010; Page et al. 2007). Avoidable deaths have been used in various studies to measure the quality, effectiveness, and accessibility of the health system. However, mortality from most conditions is influenced by broader determinants such as environmental factors, social disadvantage, and health behaviours. Almost 60% of deaths among Aboriginal and Torres Strait Islander (First Nations) people aged under 75 years are considered avoidable (see Data findings).
Disparities between First Nations people and non-Indigenous Australians can be seen across the disease groups and risk factors that drive avoidable mortality; disparities are also seen across age groups (particularly infants, middle and older ages) and remoteness categories. Reducing avoidable mortality would lead to substantial improvements in overall health outcomes and quality of life for First Nations people, and help in closing the health gap between First Nations and non-Indigenous people. Improved understanding of the causes of avoidable mortality helps in designing targeted health interventions and ensuring effective resource allocation. Providing communities with information about avoidable mortality enables self-determination and empowers communities to take proactive steps in improving their health and wellbeing.
The National Agreement on Closing the Gap (the National Agreement), was developed in partnership between Australian governments and the Coalition of Aboriginal and Torres Strait Islander Peak Organisations. It is built around 4 Priority Reforms directly informed by First Nations people. These reforms aim to change how governments work with First Nations people by fostering partnership and shared decision-making, building the Aboriginal community-controlled sector, transforming government organisations, and improving and sharing access to data and information to enable informed decision making by First Nations communities. The National Agreement has identified the importance of making sure First Nations people enjoy long and healthy lives (Target 1 on life expectancy), and that First Nations people enjoy high levels of social and emotional wellbeing (Target 14 on suicide).
The National Agreement identifies several supporting indicators considered to be key drivers of life expectancy such as potentially avoidable mortality (the focus of this HPF measure), all-cause mortality and leading causes of death (see measures 1.22 All causes age-standardised death rates and 1.23 Leading causes of death, respectively, for information on these topics).
For the latest data on the Closing the Gap targets, see the Closing the Gap Information Repository.
The National Aboriginal and Torres Strait Islander Health Plan 2021–2031 (Health Plan) represents the Australian Government’s ongoing commitment to improving health outcomes for First Nations people. Its vision is for First Nations people to enjoy long, healthy lives centred in culture, with access to services that are prevention-focused, culturally safe and responsive, equitable and free of racism. The Health Plan also identifies early intervention and access to person-centred and family-centred care as priorities.
Both the National Agreement and the Health Plan are discussed further in the Implications section of this measure.
Data findings
Potentially avoidable deaths are classified using nationally agreed definitions based on cause of death for people aged less than 75. They include deaths from conditions that are potentially preventable through individualised care and/or treatable through existing primary or hospital care (AIHW 2025). Note that COVID-19 is not currently included in the definition of potentially avoidable deaths.
Nationally, in the period 2019–2023, there were 9,902 deaths of First Nations people aged 0–74 from potentially avoidable causes, representing 58% of all deaths nationally of First Nations people aged 0–74 (Table D1.24.1).
Mortality data in the remainder of this measure are from 5 jurisdictions for which the quality of Indigenous identification in the deaths data is adequate: namely, New South Wales, Queensland, Western Australia, South Australia, and the Northern Territory. Data by remoteness are reported for all Australian states and territories combined (see Data sources: National Mortality Database).
In the period 2019–2023, in the 5 jurisdictions where Indigenous identification was of adequate quality, there were 8,972 deaths of First Nations people aged 0–74 from potentially avoidable causes. This equates to a rate of 211 deaths per 100,000 population and represents 59% of all deaths of First Nations people aged 0–74 (Table D1.24.1, Table D1.24.3).
Avoidable deaths by sex and age
In the 5-year period 2019–2023, in the 5 jurisdictions where Indigenous identification was of adequate quality, First Nations males who died from potentially avoidable causes tended to be younger than First Nations females who died from these causes; 56% of potentially avoidable deaths for First Nations males occurred before age 55 compared with 46% of deaths for First Nations females. Overall, First Nations males were more likely to die from potentially avoidable causes than First Nations females (244 and 179 per 100,000 population, respectively) (Table D1.24.3).
Rates of potentially avoidable deaths were higher for First Nations males than First Nations females across all age groups. For those aged 15–24 and 25–34, the rate of potentially avoidable deaths was more than twice as high for First Nations males as for First Nations females (92 compared with 43 deaths per 100,000, and 169 compared with 81 per 100,000, respectively) (Table D1.24.3, Figure 1.24.1).
Figure 1.24.1: Age-specific rates of potentially avoidable deaths, persons aged 0–74, by Indigenous status, age and sex, NSW, Qld, WA, SA, and NT, 2019–2023
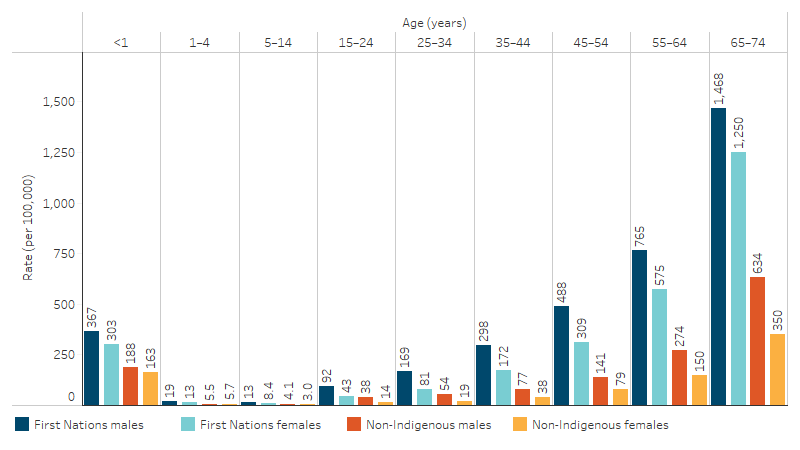
Source: Table D1.24.3. AIHW National Mortality Database.
Potentially avoidable deaths by jurisdiction
Among First Nations people in 2019–2023, and for the 5 jurisdictions for which Indigenous identification in deaths data is considered adequate:
- the rate of potentially avoidable deaths was highest in the Northern Territory (386 deaths per 100,000 population), followed by Western Australia (280 per 100,000), South Australia (224 per 100,000), Queensland (187 per 100,000) and lastly New South Wales (165 per 100,000).
- the rate of potentially avoidable deaths in the Northern Territory was 2.3 times as high as that in New South Wales and 2.1 times that in Queensland (Table D1.24.4, Figure 1.24.2).
Figure 1.24.2: Rates of potentially avoidable deaths, First Nations people aged 0–74, by state and territory, NSW, Qld, WA, SA, and NT, 2019–2023
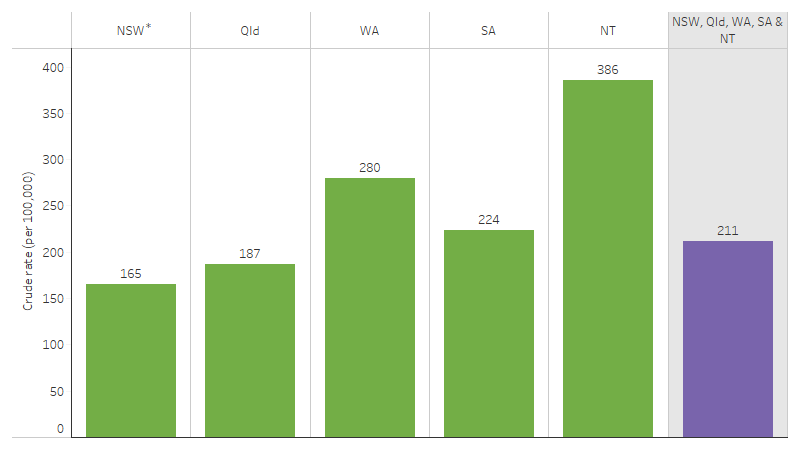
Note: Caution should be used when interpreting differences in death rates between jurisdictions due to a break in the series in 2021 for New South Wales (see Box 1.24.1).
Source: Table D1.24.4. AIHW National Mortality Database.
Potentially avoidable deaths by remoteness
Among First Nations people in 2019–2023 nationally, there were:
- 3,058 potentially avoidable deaths in Major cities (a rate of 154 deaths per 100,000 population)
- 4,048 potentially avoidable deaths in Inner and outer regional areas (191 per 100,000)
- 2,579 potentially avoidable deaths in Remote and very remote areas (347 per 100,000).
The rate of potentially avoidable deaths in Remote and very remote areas was 2.2 times the rate of those living in Major cities (154 per 100,000) and 1.8 times the rate of those living in Inner and outer regional areas (191 per 100,000) (Table D1.24.6).
The death rate due to potentially avoidable causes was higher for First Nations males than First Nations females across all remoteness areas. For First Nations males in both Major cities and Inner and outer regional areas, the rate was 1.4 times that of First Nations females. The rate for First Nations males in Remote and very remote areas was 1.3 times that of First Nations females. For both First Nations males and females, the rate increased as remoteness increased (Table D1.24.6, Figure 1.24.3).
Figure 1.24.3: Rates of potentially avoidable deaths, First Nations people aged 0–74, by sex and remoteness, Australia, 2019–2023
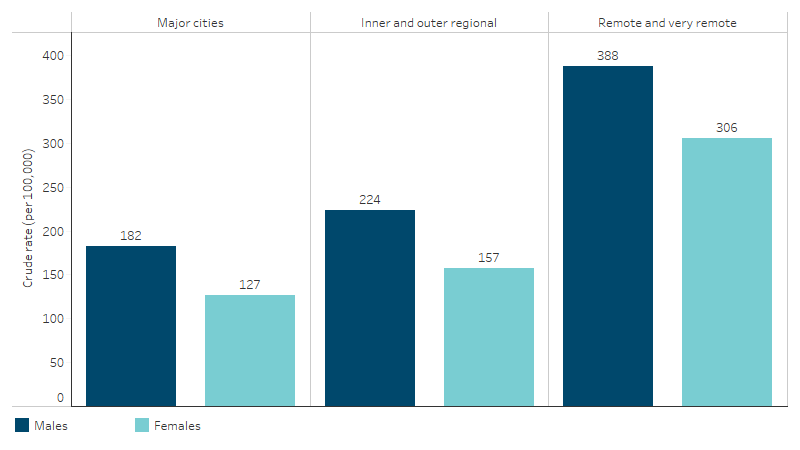
Source: Table D1.24.6. AIHW National Mortality Database.
Causes of avoidable deaths
Of the 8,972 potentially avoidable deaths among First Nations people in 2019–2023 in the 5 jurisdictions where Indigenous identification was of adequate quality:
- 19% (1,741 deaths) were due to coronary heart disease
- 12% (1,109) were due to diabetes
- 12% (1,040) were due to suicide and self-inflicted injuries
- 10% (899) were due to chronic obstructive pulmonary disease
- 8.6% (776) were due to cancer (Table D1.24.5, Figure 1.24.4).
Figure 1.24.4: Potentially avoidable deaths, First Nations people aged 0–74, by cause of death, NSW, Qld, WA, SA, and NT, 2019–2023 (per cent)
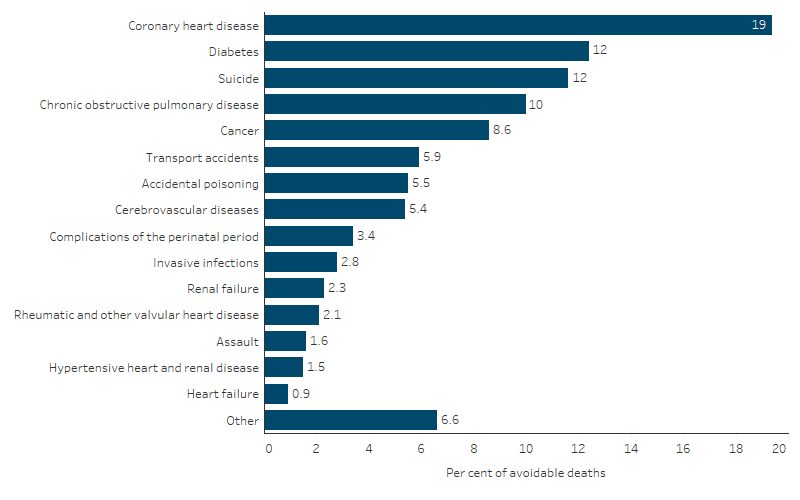
Note: 'Other' includes all avoidable mortality not specifically detailed in the figure.
Source: Table D1.24.5. AIHW National Mortality Database.
Comparisons with non-Indigenous Australians
After adjusting for differences in the age structure between the two populations, First Nations people died from potentially avoidable causes at 3.2 times the rate of non-Indigenous Australians in the 5 jurisdictions where Indigenous identification was of adequate quality in 2019–2023 (Table D1.24.1).
Rates of potentially avoidable deaths were higher for First Nations people than for non-Indigenous Australians across all age groups. The rate of potentially avoidable deaths was highest for First Nations people aged 65–74 (1,353 deaths per 100,000), and this age group also had the largest absolute difference in rates between First Nations people and non-Indigenous Australians (a difference of 865 deaths per 100,000).
The very high rate in the 65–74 age group can be explained by the smaller population base due to natural attrition and historical birth rates. Even a modest number of deaths could result in a high rate when the denominator is small. The high rate can also be explained by higher baseline risk and cohort effects from earlier onset of chronic diseases in middle age for First Nations people (such as coronary heart disease, diabetes, chronic obstructive pulmonary disease, and lung cancer), in addition to the greater risk of chronic disease related complications in older adults.
The relative difference in potentially avoidable death rates was highest in those aged 35–44, with the rate for First Nations people in this age group 4.1 times as high as the rate for non-Indigenous Australians (234 and 57 deaths per 100,000, respectively) (Table D1.24.3, Figure 1.24.1).
It is important to note that potentially avoidable deaths (as well as all-cause deaths) at younger ages contribute to more Potential Years of Life Lost (PYLL). The rate of PYLL was higher for First Nations people than non-Indigenous Australians in all age groups, but First Nations people experience more PYLL at younger age groups than non-Indigenous Australians (see measure 1.22 All-cause age-standardised death rates).
Based on age-standardised rates, the gap in potentially avoidable mortality between First Nations people and non-Indigenous Australians was higher in Remote and very remote areas than in Major cities and Inner and outer regional areas (rate difference of 344 compared with 153 and 149 deaths per 100,000 population, respectively) (Table D1.24.6).
After adjusting for differences in the age structure between the two populations, the conditions contributing most to the gap between First Nations people and non-Indigenous Australians in rates of potentially avoidable deaths were coronary heart disease (23% of the gap in avoidable deaths), diabetes (18% of the gap) and chronic obstructive pulmonary disease (14% of the gap) (Table D1.24.5).
Potentially avoidable death rates were higher for First Nations people than for non-Indigenous Australians for all causes of death, after adjusting for differences in the age structure between the two populations. The largest relative difference was for diabetes with a rate for First Nations people 8 times that of non-Indigenous Australians (42 and 5 deaths per 100,000 population), while coronary heart disease had the largest absolute difference between these populations (a difference of 47 deaths per 100,000) (Table D1.24.5, Figure 1.24.5).
Figure 1.24.5: Age-standardised rates of potentially avoidable deaths, persons aged 0–74, by Indigenous status, cause of death, NSW, Qld, WA, SA, and NT, 2019–2023
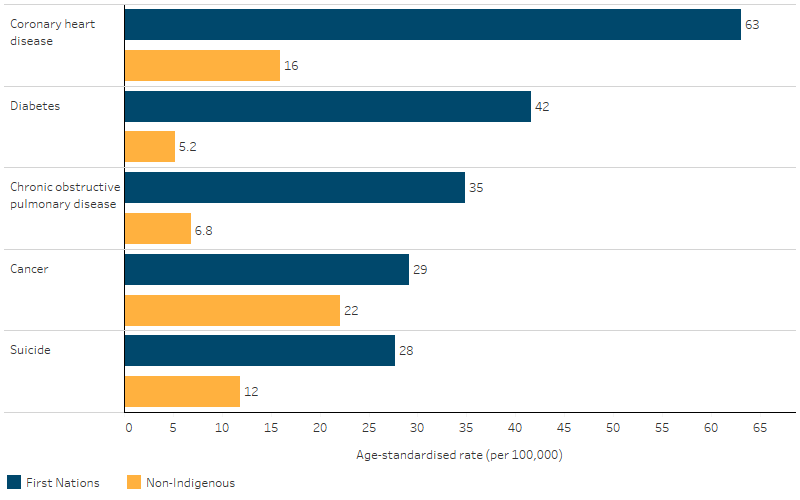
Source: Table D1.24.5. AIHW National Mortality Database.
Changes over time
The proportion of all deaths among First Nations people aged 0–74 that were considered potentially avoidable decreased from 61% in 2016 to 57% in 2021; however, this was not a statistically significant change (Table D1.24.7).
Between 2016 and 2021, the age-standardised rate of potentially avoidable deaths did not change significantly for First Nations people, increasing by 3%, while for non-Indigenous people the rate decreased significantly by 11% (Table D1.24.2, Figure 1.24.6).
Over this same period, the relative difference in rates between First Nations people and non-Indigenous Australians (rate ratio) ranged between 2.6 in 2017 and 3.1 in 2020 (Table D1.24.2, Figure 1.24.6).
Figure 1.24.6: Age-standardised rates of potentially avoidable deaths, by Indigenous status, NSW, Qld, WA, SA, and NT, 2016–2023
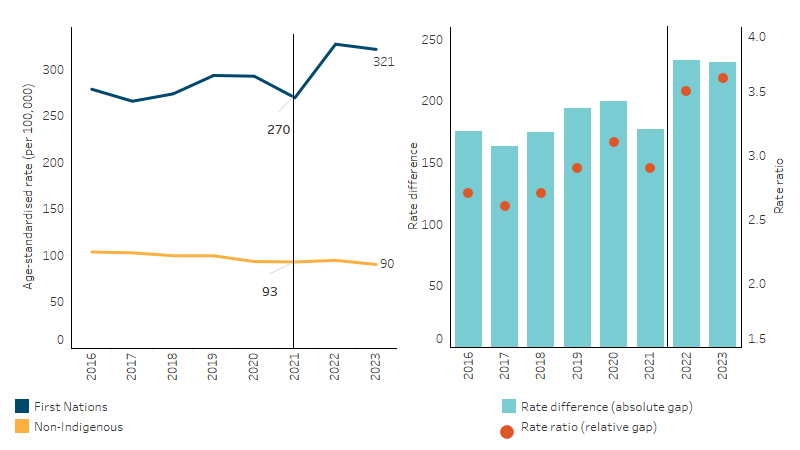
Note: The vertical line indicates break in series in 2022 due to changes in Indigenous identification method in New South Wales. Caution should be used when interpreting changes in death rates over time (see Box 1.24.1).
Source: Table D1.24.2. AIHW National Mortality Database.
Research and evaluation findings
Regular and comprehensive health checks are a vital tool in reducing avoidable mortality. They enable early identification and management of chronic conditions such as cardiovascular disease, diabetes, and chronic obstructive pulmonary disease – which are among the leading contributors to avoidable deaths among First Nations people. However, there is wide variability in the delivery of primary health care and preventive services for First Nations people in Australia. While basic health checks are often well delivered, services such as follow-up of abnormal results and breast cancer screening have been underutilised (Bailie et al. 2016). Barriers to accessing services include geographic isolation, affordability, service availability, cultural safety, and limited awareness, while enablers include community-led and self-determined approaches (Peake et al. 2021; Schütze et al. 2016). Community-led and self-determined approaches have proven effective in improving access and engagement.
The COVID-19 pandemic further disrupted access to primary health care. While performance data shows increases in client numbers and episodes of care due to COVID-19 vaccinations and testing, there were substantial declines in other types of service use such as for preventative health assessments and chronic disease management particularly in Very remote areas (AIHW 2023a; Sutherland et al. 2020). Nevertheless, First Nations-led responses – such as point-of-care testing and strategic governance through the National Aboriginal and Torres Strait Islander Health Protection (NATSIHP) Subcommittee – demonstrated resilience, innovation, and a strong commitment to protecting community health (Nous Group 2022). Rapid, community-led biosecurity measures minimised the infection and death of First Nations people in the early stages of the pandemic (PM&C 2024).
Burden of disease
An AIHW report (AIHW 2023b) looking at avoidable fatal burden (AYLL) due to potentially avoidable deaths among people aged under 75 years showed that in 2018:
- The main causes of avoidable fatal burden (AYLL) among First Nations people under 75 were coronary heart disease (17.1%), suicide and self-inflicted injuries (16.1%), poisoning (7.5%), chronic obstructive pulmonary disease (5.9%), chronic kidney disease (5.7%), road traffic injuries for motor vehicle occupants (5.0%), pre-term birth and low birthweight complications (4.3%), and type 2 diabetes (3.9%). However, from age 55 onwards chronic disease dominates the causes of avoidable fatal burden (particularly coronary heart disease, chronic obstructive pulmonary disease, chronic kidney disease and type 2 diabetes) while suicide and injuries are much less prominent.
- For overall fatal burden (YLL) nearly two-thirds (64%) of fatal burden among First Nations people was avoidable compared with just over half (54%) among non-Indigenous Australians (AIHW 2023b).
- Modifiable risk factors accounted for 49% of the total (fatal and non-fatal) burden of disease (DALY) for First Nations people.
- Tobacco use was the leading modifiable risk factor contributing to the burden of disease among First Nations people in 2018, contributing to 23% of all deaths, 12% of total burden (DALY) and 19% of fatal burden (YLL) (AIHW 2022).
A national cohort study found that frequent smoking was associated with the highest risk of death among First Nations people, while those who had never smoked had the lowest risk. Importantly, quitting smoking at any age reduced risk of death, with individuals who quit before age 45 having a similar mortality risk to those who had never smoked. More than half of deaths among First Nations adults aged 45 and over were attributable to smoking, with current smokers living over 10 years less than never-smokers (Thurber et al. 2021).
Social determinants
Social determinants have been associated with the chronic diseases that contribute to potentially avoidable deaths. First Nations people living in the Northern Territory experience the greatest area level socioeconomic disadvantage among the jurisdictions with nearly 7 in 10 First Nations people living in the most disadvantaged quintile of Indigenous Areas nationally (see measure 2.09 Socioeconomic indexes). The Northern Territory also has the highest rates of potentially avoidable deaths for First Nations people (Figure 1.24.2), particularly driven by diabetes, ischaemic heart diseases and chronic lower respiratory diseases (see measure 1.23 Leading causes of death). Similar observations about First Nations people in the Northern Territory specifically regarding diabetes were made by Agarwal et al. (2023), in their global review of diabetes inequity, highlighting the role of structural racism, intergenerational trauma and geographic inequities in diabetes outcomes.
Social determinants such as household crowding, poor housing infrastructure, early childhood infections, tobacco exposure, and limited access to health care are particularly evident in remote areas and non-urban First Nations communities. These social and environmental conditions have led to persistently higher rates of chronic respiratory disease and hospitalisation compared to non-Indigenous Australians, and this impact is seen early in the life course including in children (Bush et al. 2024).
Housing is also associated with preventable burden of disease. A study of Indigenous areas (IAREs) in New South Wales identified a relationship between the percentage of houses in an IARE that were overcrowded, and avoidable hospital admissions. For every 1% increase in overcrowded households, avoidable hospital admissions increased by 130 cases per 100,000 people (Doyle et al. 2024).
Upstream factors and determinants are compounded by barriers to preventive health services, such as limited availability of screening, health promotion, and early intervention in remote and regional areas.
Changes in avoidable mortality over time
There is limited time series research on First Nations avoidable mortality in most Australian jurisdictions; however, there are several studies using mortality data from the Northern Territory.
A 20-year (1985–2004) analysis of avoidable mortality in the Northern Territory revealed significant health gains, with improvements most evident in conditions amenable to medical care, for example, neonatal and paediatric care, infectious diseases, and stroke. These outcomes reflect the positive impact of expanded health-care access, including antibiotics, immunisation, and chronic disease management. While the overall reduction in avoidable mortality was smaller for First Nations people (19%) compared with non-Indigenous Territorians (61%), the findings underscore the effectiveness of targeted medical interventions. However, limited progress in conditions linked to smoking and alcohol highlights the need for more culturally responsive public health strategies for First Nations people (Li et al. 2009). More recently, further gains in First Nations life expectancy between 1999 and 2018 have been attributed to reductions in years of life lost from cancer, injuries and preventable chronic diseases (Zhao et al. 2022).
Hoy et al. (2017) analysed mortality trends among the Tiwi people on Bathurst and Melville Islands off the coast of the Northern Territory between 1960 and 2010, revealing a significant epidemiological transition. In the 1960s, infant deaths from diarrhoea, respiratory infections, and failure to thrive were prevalent. Over time, these shifted to chronic conditions such as lung disease, cardiovascular disease, and renal failure in older age groups. The study also highlighted a concerning rise in deaths among 15–45-year-olds from non-natural causes such as accidents, suicide, and homicide, peaking in the early 2000s (Hoy et al. 2017). The study illustrated the Barker Hypothesis (Almond and Currie 2011; Hoy and Nicol 2019), showing that children with low birthweight who previously faced early mortality are now surviving into adulthood, but with increased vulnerability to chronic disease. Importantly, enhanced primary health care services introduced in the mid-1990s led to an almost 50% reduction in non-violent deaths within just over 3 years, demonstrating both the effectiveness and cost-efficiency of targeted health interventions in remote communities (Hoy et al. 2003).
Health care and avoidable mortality
A study of First Nations people living in remote Northern Territory communities found that those who attended a remote clinic more than twice a year (on average) experienced lower rates of hospitalisation and death than those with low primary health care usage (fewer than 2 clinic visits a year, on average) (Zhao et al. 2014). This was a historical cohort study involving a total of 14,184 First Nations people aged 15 and over who lived in remote communities and used a remote clinic or public hospital from 2002 to 2011. Higher levels of primary care usage reduced avoidable hospitalisations for renal disease by 82–85%, deaths by 72–75%, and years of life lost (YLL) by 78–81%. For ischaemic heart disease the reduction in avoidable hospitalisation was 63–78%, deaths by 63–66% and YLL by 69–73%. This study also estimated that investing $1 in primary health care in remote First Nations communities could save between $3.95 and $11.75 in hospital costs in addition to the health benefits for patients. While use of primary health care has clear benefits, First Nations people face unique barriers to accessing health care (see measures 3.08 Cultural competency and 3.14 Access to services compared with need).
Studies on respiratory disease services have shown positive outcomes. In Western Australia, an integrated chronic obstructive pulmonary disease multidisciplinary community service reduced long-term respiratory hospitalisations (Chung et al. 2016). A large pilot study in Queensland highlighted the importance of working with communities and First Nations staff to develop and deliver a culturally appropriate and accessible specialist respiratory service (Medlin et al. 2014).
Cancer death rates are higher for First Nations people than for non-Indigenous Australians, even after accounting for more advanced stages of cancer and competing causes of death, suggesting that some First Nations cancer deaths are avoidable (Condon et al. 2014; Tervonen et al. 2017). First Nations people diagnosed with cancer have a higher probability of dying from cancer within the first 5 years of diagnosis across a range of cancer types. One study estimated that among a typical yearly cohort of First Nations people diagnosed with cancer, about 21% of observed deaths within 5 years of diagnosis were potentially avoidable if relative survival was the same as for non-Indigenous Australians.
Interventions designed to improve early diagnosis and management, increase screening participation, and reduce risk factor prevalence, especially smoking, among First Nations people have the potential to improve cancer outcomes. These efforts could lead to more equitable outcomes for multiple cancer types including breast, colorectal, lung, cervical and head and neck cancers within the first 5 years after diagnosis (Dasgupta et al. 2022) (see measure 1.08 Cancer). However, these interventions alone are insufficient if they do not also address the systemic barriers to accessing services and the cultural appropriateness and safety of health-care settings.
A narrative review of First Nations people’s cancer care experiences found that communication barriers, a lack of cultural safety, and limited access to services were common. These challenges are often compounded by institutional racism, mistrust of the health system, and a lack of culturally appropriate care. Suggested solutions include embedding cultural safety into all levels of care, increasing the First Nations health workforce (e.g. liaison officers and care coordinators), and ensuring culturally safe communication and support throughout the cancer care journey (Sanjida et al. 2022).
Racial discrimination is another determinant of health, and could be another risk factor for higher death rates for First Nations people. Coronial findings into the death of 3 First Nations women in Doomadgee, Queensland who died from rheumatic heart disease between 2019 and 2020 described these deaths as ‘entirely preventable’. The coroner identified the hospital service’s treatment of the women and their community as racist, with evidence of covert bias and prejudicial language in clinical notes, as well as failure to treat First Nations patients with respect and seriousness (Tarrago (Wangkamahdla) et al. 2024).
An evaluation of RHD Control Programs across 4 Australian jurisdictions (2010–2017) found that these programs contributed to improved delivery of secondary prophylaxis (administration of antibiotics to people with a history of Acute Rheumatic Fever (ARF) to prevent Group A Streptococcus infection, subsequent ARF recurrence and to minimise progression to RHD). The median proportion of days covered increased from 53% in 2010 to 70% in 2017. This was associated with reduced progression to severe RHD or death (Stacey et al. 2023). However, the 2025 Australian ARF and RHD Guideline reports that more recent trends show a decline in adherence to secondary prophylaxis in some regions, due to persistent workforce, access, and system-level challenges. These findings highlight the need for renewed investment in culturally safe, community-led models of care and stronger support for frontline health workers (Menzies School of Health Research (ARF/RHD writing group) 2025).
Invasive infections are a significant contributor to avoidable mortality among First Nations children. A study found that these infections accounted for 23% of non-elective Intensive Care Unit (ICU) admissions among First Nations children, with an admission rate nearly 3 times higher than for non-Indigenous children. While ICU case fatality rates were similar, the population-based death rate for First Nations children was more than twice as high as non-Indigenous children, highlighting a disproportionate burden and the need for targeted prevention and early intervention strategies (Ostrowski et al. 2017).
Indigenous Australians’ Health Programme
An independent evaluation assessed appropriateness and effectiveness of primary health care delivered under the Indigenous Australians’ Health Programme (IAHP). Commissioned by Department of Health, Disability and Ageing (formerly Department of Health and Aged Care), the evaluation was co-designed with the First Nations health sector and conducted across 17 urban, regional, and remote sites. Evaluation findings delivered in June 2023 show that the IAHP provides critical investment in primary health care for First Nations people, particularly through Aboriginal Community Controlled Health Services (ACCHSs). However, the report also stated that funding was too low for ACCHSs to consistently deliver values-aligned care.
The evaluation identified key challenges:
- workforce pressures, including rising vacancies and an ageing workforce
- high reporting burden across multiple funders
- fragmented governance and limited integration with broader health systems
- mainstream services unable to replicate community-driven, place-based care
- data systems focused on activity rather than outcomes valued by communities.
Recommendations include strengthening shared decision-making, increasing investment, improving workforce conditions, streamlining reporting, and enhancing data systems to support Indigenous data sovereignty and community-led needs assessments (Allan + Clarke Consulting et al. 2023).
Implications
These findings emphasise the critical importance of sustained, coordinated efforts to improve First Nations health outcomes, both directly through health interventions and services, and by addressing the cultural and social determinants of health.
The findings indicate:
- Significant improvements in avoidable death rates are achievable through enhanced primary health care and such services are highly cost effective. A broad range of risk factors and conditions such as smoking, injury, mental health issues, substance-use disorders, cardiac health, diabetes prevention and treatment, and renal disease all require service responses across the health care continuum from prevention to tertiary care.
- Disparities between First Nations people and non-Indigenous Australians can be seen across disease groups, risk factors, age groups (particularly infants and middle and older ages) and remoteness categories, suggesting that policies to drive service delivery should consider the risk factors of disease, across the life course, be cognisant of location-specific needs, cultural safety to improve access, and service gaps.
- Improved inter-sectoral services with more attention to social determinants like education and housing are critical.
The National Agreement on Closing the Gap provides a framework for tackling these systemic inequities and driving meaningful change.
Despite some progress, the total burden of disease for First Nations people remains 2.3 times as high as for non-Indigenous Australians. Higher rates of potentially preventable hospitalisations and avoidable mortality from chronic disease and infections point to underutilisation of primary health care, exacerbated by barriers such as availability, distance, cost and lack of cultural safety (see measure 3.14 Access to services compared with need).
Aboriginal Community-controlled Health Services (ACCHSs) have proven effective in delivering culturally safe, comprehensive care, particularly for chronic conditions management to prevent hospitalisations and death from avoidable causes (Pearson et al. 2020).
The National Aboriginal and Torres Strait Islander Suicide Prevention Strategy (2025–2035), the Fifth National Aboriginal and Torres Strait Islander Blood Borne Virus and Sexually Transmissible Infection Strategy 2018–2022, and Cancer Australia’s Optimal Care Pathway reflect a growing commitment to culturally responsive care (see measure 1.08 Cancer).
Implementation of the National Aboriginal and Torres Strait Islander Health Plan aims to drive structural reform towards models of care that are prevention and early intervention focused, with greater integration of care systems and pathways across primary, secondary and tertiary care. It also emphasises the need for mainstream services to address racism, provide culturally safe and responsive care, and to be accountable to First Nations people and communities.
Priority 5 of the Health Plan focuses on early prevention, with the desired outcome of ensuring that early intervention approaches are accessible to First Nations people and provide timely, high quality, effective and culturally safe and responsive care. More specifically, the objectives of this priority are to:
- increase the quality and uptake of health checks
- deliver activities to improve oral health, particularly for children
- enhance access to early intervention for chronic disease
- target early interventions to support cessation of tobacco use
- enhance the delivery of evidence-based sexual health screening activities at the community level, particularly for adolescents and young adults
- deliver targeted action to improve cancer screening rates and care pathways for treatment.
Priority 10 of the Health Plan focuses on mental health and suicide prevention, with the desired outcome of addressing mental health in a sustained and holistic way that is trauma-aware and healing informed, recognising the impacts of the social determinants of health and embracing the strength that First Nations people have from culture and language. The objectives are to:
- implement key reforms to First Nations mental health and suicide prevention policy
- strengthen the role of ACCHS to deliver and coordinate culturally safe and responsive mental health and suicide prevention services
- embed integrated models of suicide prevention and mental health for continuity of care
- ensure First Nations people with lived experience are at the centre of the development and delivery of mental health and suicide prevention services.
In December 2024 the National Aboriginal and Torres Strait Islander Suicide Prevention Strategy 2025–2035 was launched. The Strategy is informed by the Aboriginal and Torres Strait Islander Suicide Prevention Evaluation Project (ATSISPEP) which identifies 3 required levels of intervention – population-level interventions, targeted interventions for groups at a higher risk of suicide and self-harm, and specific interventions for individuals at higher risk of suicide and self-harm, or who have attempted suicide.
The National Road Safety Strategy 2021–30 and National Road Safety Action Plan 2023–25 aim to reduce road trauma among First Nations people, who experience disproportionately higher rates of fatalities. These plans include practical measures such as improving licensing access, enhancing road safety education, and implementing culturally appropriate interventions like child restraint programs and alternative transport options. Establishing baseline fatality data will support targeted actions and enable progress to be measured through reductions in deaths and serious injuries (see measure 1.03 Injury and poisoning).
References
- ABS (Australian Bureau of Statistics) (2023a) Causes of death, Australia methodology (2022), ABS website, accessed 27 January 2026.
- ABS (2023b) Understanding change in counts of Aboriginal and Torres Strait Islander Australians: Census (2021), ABS website, accessed 27 January 2026.
- ABS (2024) Causes of death, Australia methodology (2023), ABS website, accessed 27 January 2026.
- ABS (2025) Excess mortality by selected causes of death, 2020–23, ABS website, accessed 27 January 2026.
- Agarwal S, Wade AN, Mbanya JC, Yajnik C, Thomas N, Egede LE, Campbell JA, Walker RJ, Maple-Brown L and Graham S (2023) 'The role of structural racism and geographical inequity in diabetes outcomes', The Lancet, 402(10397):235–249, doi:10.1016/s0140-6736(23)00909-1.
- AIHW (Australian Institute of Health and Welfare) (2010) National Healthcare Agreement: P20-potentially avoidable deaths, 2010, AIHW, METEOR website, accessed 27 March 2026.
- AIHW (2022) Australian Burden of Disease Study: impact and causes of illness and death in Aboriginal and Torres Strait Islander people 2018, AIHW, Australian Government, accessed 30 March 2026, doi:10.25816/xd60-4366.
- AIHW (2023a) Aboriginal and Torres Strait Islander specific primary health care: impact of COVID-19, AIHW, Australian Government, accessed 27 March 2026.
- AIHW (2023b) Burden of avoidable deaths among Aboriginal and Torres Strait Islander people 2018, AIHW, Australian Government, accessed 2 April 2026.
- AIHW (2025) Deaths in Australia, AIHW, Australian Government, accessed 2 April 2026.
- Allan + Clarke Consulting, Central Queensland University, Monaghan Dreaming and University of Queensland (2023) Final report of the evaluation of the Australian Government’s investment in Aboriginal and Torres Strait Islander primary health care through the Indigenous Australians’ Health Programme, report to the Department of Health and Aged Care, Allan + Clarke Consulting, accessed 7 April 2026.
- Almond D and Currie J (2011) 'Killing me softly: the fetal origins hypothesis', Journal of Economic Perspectives, 25(3):153–172, doi:10.1257/jep.25.3.153.
- Bailie C, Matthews V, Bailie J, Burgess P, Copley K, Kennedy C, Moore L, Larkins S, Thompson S and Bailie R (2016) 'Determinants and gaps in preventive care delivery for Indigenous Australians: a cross-sectional analysis', Frontiers in Public Health, 4:34, doi:10.3389/fpubh.2016.00034.
- Bush A, Byrnes CA, Chan KC, Chang AB, Ferreira JC, Holden KA, Lovinsky-Desir S, Redding G, Singh V, Sinha IP and Zar HJ (2024) 'Social determinants of respiratory health from birth: still of concern in the 21st century?', European Respiratory Review, 33(172):230222, doi:10.1183/16000617.0222-2023.
- Chung LP, Lake F, Hyde E, McCamley C, Phuangmalai N, Lim M, Waterer G, Summers Q and Moodley Y (2016) 'Integrated multidisciplinary community service for chronic obstructive pulmonary disease reduces hospitalisations', Internal Medicine Journal, 46(4):427–434, doi:10.1111/imj.12984.
- Condon J, Zhang X, Baade P, Griffiths K, Cunningham J, Roder DM, Coory M, Jelfs PL and Threlfall T (2014) 'Cancer survival for Aboriginal and Torres Strait Islander Australians: a national study of survival rates and excess mortality', Population Health Metrics, 12:1, doi:10.1186/1478-7954-12-1.
- Dasgupta P, Garvey G and Baade PD (2022) 'Quantifying the number of deaths among Aboriginal and Torres Strait Islander cancer patients that could be avoided by removing survival inequalities, Australia 2005–2016', PloS One, 17(8):e0273244, doi:10.1371/journal.pone.0273244.
- Doyle M, Jackson-Pulver L, Harley S, Ring I and McBryde E (2024) 'Could adequate and more appropriate housing for Aboriginal and Torres Strait Islander people in New South Wales, Australia, reduce the risk of poorer health outcomes?', International Journal of Indigenous Health, 19(1), doi:10.32799/ijih.v19i1.41293.
- Hoy WE, Mott SA and McLeod BJ (2017) 'Transformation of mortality in a remote Australian Aboriginal community: a retrospective observational study', BMJ Open, 7(8):e016094, doi:10.1136/bmjopen-2017-016094.
- Hoy WE and Nicol JL (2019) 'The Barker hypothesis confirmed: association of low birth weight with all-cause natural deaths in young adult life in a remote Australian Aboriginal community', Journal of Developmental Origins of Health and Disease, 10(1):55–62, doi:10.1017/s2040174417000903.
- Hoy WE, Wang Z, Baker PRA and Kelly AM (2003) 'Reduction in natural death and renal failure from a systematic screening and treatment program in an Australian Aboriginal community', Kidney International, 63(83):S66–73, doi:10.1046/j.1523-1755.63.s83.14.x.
- Li SQ, Gray N, Guthridge S, Pircher S, Wang Z and Zhao Y (2009) 'Avoidable mortality trends in Aboriginal and non‐Aboriginal populations in the Northern Territory, 1985‐2004', Australian and New Zealand Journal of Public Health, 33(6):544–550, doi:10.1111/j.1753-6405.2009.00451.x.
- Medlin LG, Chang AB, Fong K, Jackson R, Bishop P, Dent A, Hill D, Vincent S and O'Grady K-AF (2014) 'Indigenous Respiratory Outreach Care: the first 18 months of a specialist respiratory outreach service to rural and remote Indigenous communities in Queensland, Australia', Australian Health Review, 38(4):447–453, doi:10.1071/ah13136.
- Menzies School of Health Research (ARF/RHD writing group) (2025) Australian guideline for the prevention, diagnosis and management of acute rheumatic fever and rheumatic heart disease, accessed 7 April 2026.
- Nous Group (2022) Evaluation of COVID-19 point-of-care testing in remote and First Nations communities, report to the DHDA, Australian Government, Nous Group, accessed 7 April 2026.
- Ostrowski JA, MacLaren G, Alexander J, Stewart P, Gune S, Francis JR, Ganu S, Festa M, Erickson SJ, Straney L and Schlapbach LJ (2017) 'The burden of invasive infections in critically ill Indigenous children in Australia', The Medical Journal of Australia, 206(2):78–84, doi:10.5694/mja16.00595.
- Page A, Ambrose S, Glover J and Hetzel D (2007) Atlas of avoidable hospitalisations in Australia: ambulatory care-sensitive conditions, Public Health Information Development Unit, University of Adelaide, AIHW, accessed 7 April 2026.
- Peake RM, Jackson D, Lea J and Usher K (2021) 'Meaningful engagement with Aboriginal communities using participatory action research to develop culturally appropriate health resources', Journal of Transcultural Nursing, 32(2):129–136, doi:10.1177/1043659619899999.
- Pearson O, Schwartzkopff K, Dawson A, Hagger C, Karagi A, Davy C, Brown A, Braunack-Mayer A and on behalf of the Leadership Group guiding the Centre for Research Excellence in Aboriginal Chronic Disease Knowledge and Translation Exchange (2020) 'Aboriginal community controlled health organisations address health equity through action on the social determinants of health of Aboriginal and Torres Strait Islander peoples in Australia', BMC Public Health, 20:1859, doi:10.1186/s12889-020-09943-4.
- PM&C (Department of Prime Minister and Cabinet) (2024) COVID-19 response inquiry report, PM&C, Australian Government, accessed 7 April 2026.
- Sanjida S, Garvey G, Ward J, Bainbridge R, Shakeshaft A, Hadikusumo S, Nelson C, Thilakaratne P and Hou X-Y (2022) 'Indigenous Australians’ experiences of cancer care: a narrative literature review', International Journal of Environmental Research and Public Health, 19(24):16947, doi:10.3390/ijerph192416947.
- Schütze H, Pulver LJ and Harris M (2016) 'The uptake of Aboriginal and Torres Strait Islander health assessments fails to improve in some areas', Australian Family Physician, 45(6):415–420.
- Stacey I, Ralph A, de Dassel J, Nedkoff L, Wade V, Francia C, Wyber R, Murray K, Hung J and Katzenellenbogen J (2023) 'The evidence that rheumatic heart disease control programs in Australia are making an impact', Australian and New Zealand Journal of Public Health, 47(4):100071, doi:10.1016/j.anzjph.2023.100071.
- Sutherland K, Chessman J, Zhao J, Sara G, Shetty A, Smith S, Went A, Dyson S and Levesque J-F (2020) 'Impact of COVID-19 on healthcare activity in NSW, Australia', Public Health Research & Practice, 30(4):e3042030, doi:10.17061/phrp3042030.
- Tarrago (Wangkamahdla) A, Veit-Prince E and Brolan CE (2024) '“Simply put: systems failed”: lessons from the Coroner's inquest into the rheumatic heart disease Doomadgee cluster', The Medical Journal of Australia, 221(1):13–16, doi:10.5694/mja2.52350.
- Tervonen HE, Walton R, You H, Baker D, Roder D, Currow D and Aranda S (2017) 'After accounting for competing causes of death and more advanced stage, do Aboriginal and Torres Strait Islander peoples with cancer still have worse survival? A population-based cohort study in New South Wales', BMC Cancer, 17:398, doi:10.1186/s12885-017-3374-6.
- Thurber KA, Banks E, Joshy G, Soga K, Marmor A, Benton G, White SL, Eades S, Maddox R, Calma T and Lovett R (2021) 'Tobacco smoking and mortality among Aboriginal and Torres Strait Islander adults in Australia', International Journal of Epidemiology, 50(3):942–954, doi:10.1093/ije/dyaa274.
- Zhao Y, Li SQ, Wilson T and Burgess PC (2022) 'Improved life expectancy for Indigenous and non‐Indigenous people in the Northern Territory, 1999–2018: overall and by underlying cause of death', The Medical Journal of Australia, 217:30–35, doi:10.5694/mja2.51553.
- Zhao Y, Thomas SL, Guthridge SL and Wakerman J (2014) 'Better health outcomes at lower costs: the benefits of primary care utilisation for chronic disease management in remote Indigenous communities in Australia's Northern Territory', BMC Health Services Research, 14:463, doi:10.1186/1472-6963-14-463.

