Key messages
Why is it important?
Injury and poisoning are among the leading causes of death for Aboriginal and Torres Strait Islander (First Nations) people, with rates twice as high as those for non-Indigenous Australians. Suicide is the most common cause of injury-related death, particularly affecting people aged 15–44, followed by transport accidents.
These injuries are often preventable and reflect modifiable behavioural risk factors and broader systemic issues such as social disadvantage, remoteness, and limited access to culturally safe services. The impact of injury extends beyond physical harm, contributing to long-term disability, emotional distress, and social withdrawal, and affecting education, employment, and community wellbeing. Understanding these risks within the historical, social, and cultural context is essential to developing effective, community-led responses that promote safety, cultural strengths and resilience, and healing.
Data findings
- For First Nations people in 2018, injuries were the second leading cause (12%) of the total disease burden and the leading cause of the fatal burden. The rate of burden due to injuries for First Nations people was 2.4 times the rate for non-Indigenous Australians (age-standardised rates of 38.8 and 15.8 DALY per 1,000 people, respectively). Injuries accounted for 10% of the gap in disease burden between First Nations people and non-Indigenous Australians.
- For First Nations people in the 5 jurisdictions with adequate Indigenous status identification, suicide was the leading cause of death due to injury and poisoning (38% or 1,046 deaths) in 2019–2023. It was followed by land transport accidents (19% or 527 deaths), and accidental poisoning (18% or 492 deaths).
- In 2019–2023, of all deaths from injury and poisoning, land transport accidents were the most common cause for those aged under 15 (34% of injury and poisoning deaths in that age group) while suicide was the leading cause for those aged 15–44, accounting for 49% of injury and poisoning deaths in that age group.
- For First Nations males, the rate of deaths from suicide was 2.7 times the rate for First Nations females. For land transport accidents, the rate for First Nations males was 2.4 times the rate for First Nations females.
- Over the period 2016 to 2021, there was no significant change in the age-standardised death rate due to injury and poisoning for First Nations people or non-Indigenous Australians, and no significant change in the gap.
- Between July 2021 and June 2023, there were 83,503 (42 per 1,000) hospitalisations due to injury and poisoning for First Nations people.
- Falls were the leading cause of hospitalisation due to injury and poisoning for First Nations males (20% of injury and poisoning hospitalisations) and females (23%). Exposure to inanimate mechanical forces was the second leading cause of hospitalisation due to injury and poisoning for First Nations males (16%) while assault was the second leading cause for First Nations females (20%).
- First Nations people were 1.8 times as likely as non-Indigenous Australians to be hospitalised for injury and poisoning between July 2021 and June 2023. The age-standardised rate of injury and poisoning hospitalisations increased faster for First Nations people compared with non-Indigenous Australians over the period from 2018–19 to 2022–23 resulting in a widening of the gap from 16 per 1,000 in 2016–17 to 23 per 1,000 in 2022–23.
- For First Nations females, age-standardised rates of non-fatal hospitalisation for family violence-related assaults were 30 times the rate for non-Indigenous females between July 2021 and June 2023.
Research and evaluation findings
- Evidence shows that family and community wellbeing are protective against child injury, with programs and services to support caregivers’ wellbeing leading to improvement in injury prevention for the child.
- Transport-related injuries and road trauma is disproportionately high among First Nations people, particularly in remote areas, due to systemic barriers such as poor infrastructure, low licensing rates, and limited transport options, but also behavioural risks such as low seat belt use, speeding, vehicle overcrowding, driver distraction and alcohol use.
- Alcohol and substance use contribute significantly to injury – including assault, self-harm, and transport accidents. In the Northern Territory, alcohol-related injuries accounted for 32.6% of all injury hospitalisations among First Nations people.
- High suicide rates should be understood in the context of the impacts of colonisation, intergenerational trauma, contemporary disadvantage, and discrimination which weaken protective factors such as family, community, and cultural resilience. Suicide clusters have occurred in Australia and internationally with young people particularly vulnerable, where the loss of one individual can deeply affect others and increase vulnerability to further suicides. This highlights the need for timely and culturally safe postvention.
Implications
Addressing injury and poisoning among First Nations people requires evidence-based, culturally safe, and community-led strategies that respond to local conditions and systemic disadvantage. The National Aboriginal and Torres Strait Islander Safety Promotion Strategy still provides a framework for holistic injury prevention, emphasising the importance of community leadership, improved data systems, and culturally responsive approaches. Integration with broader frameworks – such as the National Aboriginal and Torres Strait Islander Health Plan 2021–2031, the National Road Safety Strategy 2021–2030, and the National Aboriginal and Torres Strait Islander Suicide Prevention Strategy 2025–2035 – will be critical to ensuring coordinated, effective action that supports First Nations communities.
Why is it important?
For Aboriginal and Torres Strait Islander (First Nations) people, external causes (injury and poisoning) are among the leading causes of death, and death rates are twice as high as rates for non-Indigenous Australians. Suicide (intentional self-harm) is the leading cause of death from external causes followed by transport accidents (see measures 1.23 Leading causes of death and 1.18 Social and emotional wellbeing).
Research identifies key contributing factors across various injury types such as alcohol use, socioeconomic disadvantage, and remoteness. Transport-related injuries are linked to low seat belt use, speeding, low licensing levels, and inadequate access to roadworthy vehicles and infrastructure, particularly in remote areas. Violence-related injuries are associated with social stressors, including lone parenthood, disability, previous exposure to violence, neighbourhood issues, family conflict, interracial tension, and policing practices. Overcrowded housing has been shown to exacerbate stress, reduce privacy, and contribute to family strain and child safety concerns, which may heighten vulnerability to injury and poor health outcomes (Dockery et al. 2022). Suicide risk factors include the death of someone close, relationship issues, unemployment, financial and legal stress, homelessness, history of self-harm, and limited access to culturally appropriate counselling and healthcare services (Boufous et al. 2010; AIHW 2025). These risks also need to be understood within the historical, social and cultural context in which First Nations people live – contexts that shape both systemic barriers and protective factors for injury prevention, not all of which are adequately measured or monitored. Suicide clustering – where suicidal behaviour becomes ‘socially contagious’ – has been observed among First Nations and non-Indigenous Australian communities and internationally, particularly among young people, prompting greater policy emphasis on early intervention and building community capacities to respond to suicide (Silburn et al. 2014).
The impact of injuries can extend beyond immediate health consequences, sometimes leading to long-term disability affecting education and employment, economic outcomes, communication and the need for additional caring supports (Boufous et al. 2010; Stephens et al. 2014). Injuries can also contribute to emotional distress, social withdrawal, increased alcohol use, stigma, and challenges with mobility and access to services. Evidence also shows that acquired brain injury leading to cognitive impairment is associated with contact with the criminal justice system (Haysom et al. 2014). In cases of fatal injury, the effects can be deeply felt within communities for years. Injury is a significant health issue for First Nations people and rates of injury for specific causes are many times those for non-Indigenous Australians (AIHW and Pointer SC 2019). First Nations children suffer a disproportionately high burden of unintentional injury (Möller et al. 2017).
The National Aboriginal and Torres Strait Islander Health Plan 2021–2031 (the Health Plan), released in December 2021, provides a strong overarching policy framework for First Nations health and wellbeing and is the first national health document to address the health targets and priority reforms of the National Agreement on Closing the Gap.
Priority 4 of the Health Plan, Health promotion, is about enabling people to be in control of their health. Health promotion, literacy and prevention approaches recognise culture as a protective factor and prioritise strategies that drive improved outcomes across the cultural determinants and social determinants of health. Health promotion also involves strengths-based harm reduction policies and programs, including those that address the risk factors associated with injury. One particular objective of Priority 4 addresses injury prevention:
- Objective 4.7. Deliver targeted, culturally safe and responsive injury prevention activities.
Priority 10 of the Health Plan focuses on mental health and suicide prevention. A number of objectives focus on suicide prevention, including strengthening suicide prevention services and implementing key reforms to First Nations mental health and suicide prevention policy.
Burden of disease
In 2018, injuries were the second leading cause (12%) of the total disease burden for Indigenous Australians, behind mental and substance use disorders (23%). Most of the injury burden (89%) was due to premature death (fatal burden (YLL)), with only 11% due to years lived in ill health or with disability (non-fatal burden (YLD)).
Injuries were the leading cause of the fatal burden in 2018 (23% of fatal burden), particularly at younger ages – injuries were the leading cause of fatal burden for First Nations children aged 1–14 and First Nations young people aged 15–24 (47% and 80% of the fatal burden, respectively) (AIHW 2022).
Just over two-thirds (69%) of the total burden (DALY) due to injuries was experienced by First Nations males (with the remaining 31% experienced by First Nations females). Among First Nations males, 16% of total burden was due to injuries, compared with 8.3% for First Nations females.
The leading causes of injury burden were suicide and self-inflicted injuries (37% of total injury burden), and poisoning (such as the toxic effects of medicinal or other substances) (17% of injury burden).
In 2018, the age-standardised rate of burden due to injuries for First Nations people was 2.4 times the rate for non-Indigenous Australians (age-standardised rates of 38.8 and 15.8 DALY per 1,000 people, respectively). Injuries accounted for 10% of the gap in disease burden between First Nations people and non-Indigenous Australians (AIHW 2022).
Data findings
Death due to injury and poisoning
Deaths data in this measure are sourced from the National Mortality Database. The data are used to report the total number of deaths nationally, which includes Australian residents of all states and territories. However, when reporting death rates, data have been limited to 5 jurisdictions (New South Wales, Queensland, Western Australia, South Australia and the Northern Territory), in which the quality of Indigenous status identification in the deaths data is considered adequate. National death rates are not published due to concerns around the quality of Indigenous status identification in Victoria, Tasmania and the Australian Capital Territory.
When reporting death rates by remoteness, data from all jurisdictions has been included.
Nationally, over the 5-year period 2019–2023, there were 3,112 deaths of First Nations people that were due to injury and poisoning. Of these 2,162 (69%) were deaths of First Nations males and 950 (31%) were deaths of First Nations females (Table D1.03.1b).
- In 2019–2023 nationally, the rate of death due to injury and poisoning in remote areas (Remote and Very remote areas combined) was 1.7 times the rate in non-remote areas (Major cities, Inner regional and Outer regional areas combined) (74 and 44 per 100,000, respectively) (Table D1.23.30).
In the 5 jurisdictions with adequate Indigenous status identification, over the 5-year period 2019–2023, there were 2,739 deaths of First Nations people that were due to injury and poisoning. Of these 1,897 (69%) were deaths of First Nations males and 842 (31%) were deaths of First Nations females (Table D1.03.1a).
In the 5 jurisdictions with adequate Indigenous status identification, among First Nations people, over the period 2019–2023:
- Looking at broad causes of death, injury and poisoning was the third leading cause of death, accounting for 14% (2,739) of all deaths – following cancer and other neoplasms (24%, 4,773 deaths) and circulatory diseases (21%, 4,283 deaths) (Table D1.23.1).
- Looking at specific causes of death within the injury and poisoning chapter, suicide (intentional self-harm) was the leading cause of death, accounting for 38% (1,046 deaths) of all injury and poisoning deaths. This was followed by land transport accidents (19% or 527 deaths) and accidental poisoning (18% or 492 deaths). The top three leading specific causes of death were the same for males and females and accounted for 77% and 71% of all injury and poisoning deaths, respectively (Table D1.23.10).
- The rate of death due to injury and poisoning was 64 deaths per 100,000 population with a rate 2.2 times as high for males as females (88 compared with 39 per 100,000). The largest relative difference between the sexes was for deaths due to suicide, with the rate for males 2.7 times as high as the rate for females (35 compared with 13 per 100,000). This was followed by land transport accidents where the rate for males was 2.4 times as high as the rate for females (17 compared with 7 per 100,000) (Table D1.03.1a, Figure 1.03.1).
Figure 1.03.1 Death rates for injury and poisoning (external causes) for First Nations people, by external cause and sex, NSW, Qld, WA, SA and NT, 2019–2023
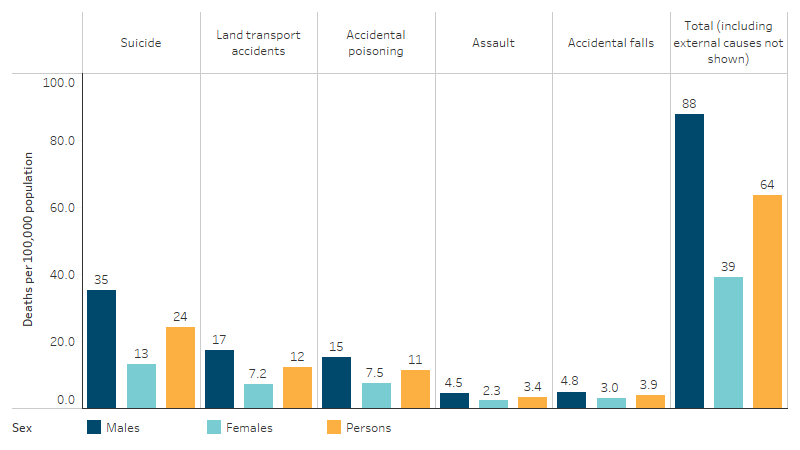
Source: Table D1.03.1a AIHW National Mortality Database.
In the 5 jurisdictions with adequate Indigenous status identification, in 2019–2023, injury and poisoning was the leading cause of death for First Nations people aged between 15 and 44. Over half (61%) of all injury and poisoning deaths occurred in these age groups (Table D1.23.3).
- For those aged under 15 the leading cause of injury and poisoning deaths was land transport accidents (34% of injury and poisoning deaths in that age group).
- For those aged between 15 and 44, the leading cause of injury and poisoning deaths was suicide, accounting for just under half (49%) of all injury and poisoning deaths in that age group.
- Accidental poisoning was the leading cause of death for those aged 45 to 64 (29%) while accidental falls was the leading cause for those over 65 (7%) (Table D1.23.11).
Hospitalisation for injury and poisoning
Injury is one of the major causes of hospitalisation. Only a small proportion of all incidents of injury result in admission to a hospital. For each hospital admission, many more cases present to hospital emergency departments but are not admitted, or are seen by a general practitioner instead. A larger number of generally minor injuries do not receive any medical treatment.
From July 2021 to June 2023, there were 83,503 hospitalisations due to injury and poisoning for First Nations people – a rate of 42 per 1,000 population (Table D1.02.5).
Excluding care involving dialysis, injury and poisoning was the leading cause of hospitalisation based on principal diagnosis for First Nations people (11% of hospitalisations excluding dialysis, or 6.5% of all hospitalisations).
Age and sex
The hospitalisation rate for injury and poisoning for First Nations people generally increased with age, ranging from 19 per 1,000 for First Nations people aged 5–14 to 67 per 1,000 for First Nations people aged over 65. The hospitalisation rate for injury and poisoning was higher for First Nations males than females in all age groups except for over 65, where First Nations women had a slightly higher rate of hospitalisation (68 compared with 66 per 1,000 population) (Table D1.03.2, Figure 1.03.2).
Figure 1.03.2: Age-specific hospitalisation rates for a principal diagnosis of injury and poisoning, by Indigenous status and sex, Australia, July 2021 to June 2023
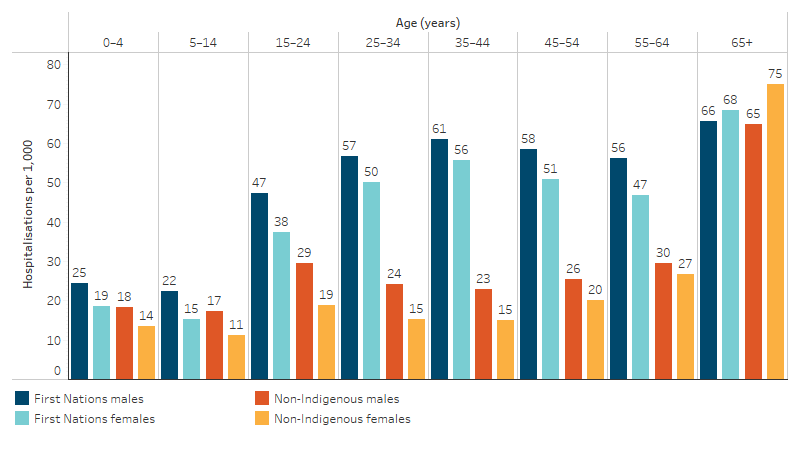
Source: Table D1.03.2. AIHW analysis of National Hospital Morbidity Database.
Jurisdiction and remoteness
Some jurisdictions have slightly different approaches to the collection of the standard Indigenous status question and categories in their hospital collections. As such comparisons by jurisdiction should be interpreted with caution. See Data sources and quality for additional information on this data collection.
Looking at rates of injury and poisoning by state and territory, for First Nations people, the rate was lowest for those living in Tasmania (25 per 1,000 population), and highest for those living in the Northern Territory (86 per 1,000) (Table D1.03.3, Figure 1.03.3).
Figure 1.03.3: Hospitalisation rates for First Nations people for a principal diagnosis of injury and poisoning, by jurisdiction, Australia, July 2021 to June 2023
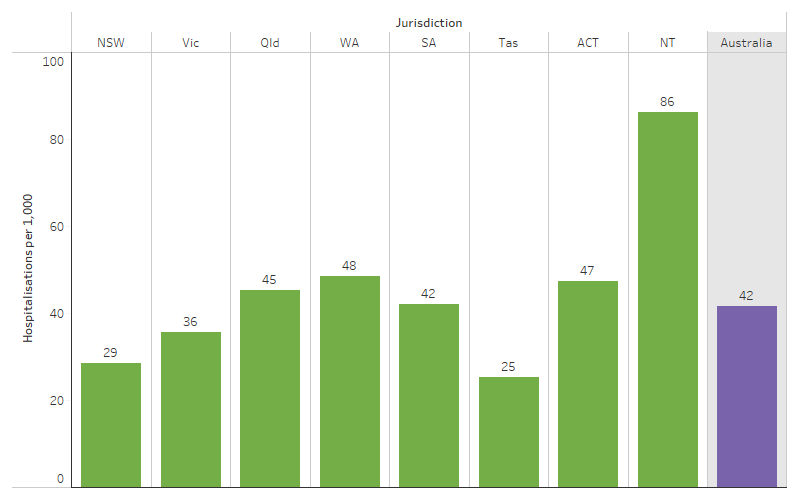
Source: Table D1.03.3. AIHW analysis of National Hospital Morbidity Database.
The hospitalisation rates for injury and poisoning were higher for First Nations people living in Remote and very remote areas (74 per 1,000 population), than in non-remote areas (35 per 1,000 in both Major cities, and in Inner and outer regional areas) (Table D1.03.4).
External cause of Injury hospitalisation
For First Nations males, falls were the leading cause of hospitalisation due to injury and poisoning (20% of injury and poisoning hospitalisations) followed by exposure to inanimate mechanical forces (16%). For First Nations females, falls was the leading cause (23%), followed by assault (20%). Hospitalisations for intentional self-harm represented 9.4% of hospitalisations of First Nations females, nearly twice as high as for First Nations males (4.9%) (Table D1.03.7, Figure 1.03.4).
Figure 1.03.4: First reported external causes for hospitalisations for a principal diagnosis of injury and poisoning for First Nations people, by sex, July 2021 to June 2023
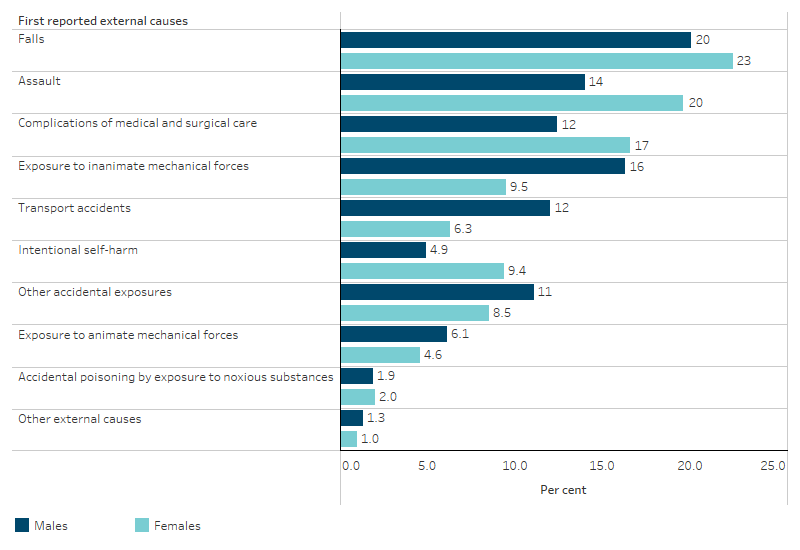
Source: Table D1.03.7. AIHW analysis of National Hospital Morbidity Database.
The first reported external cause of hospitalisation for injury and poisoning for First Nations people varied by age:
- For those aged 0–4 and 5–14, the most common first reported external cause of hospitalisation was falls (6.4 and 5.9 per 1,000 population respectively).
- For those aged 15–24, 25–34 and 35–44, the most common first reported external cause of hospitalisation was assault (7.4, 14 and 16 per 1,000 population respectively).
- For those aged 45–54, the most common first reported external cause of hospitalisation was complications of medical and surgical care (12 per 1,000 population). These can include adverse effects from medicines, and problems arising during surgical and medical care.
- For those aged 55–64 and 65 and over, the most common first reported external cause of hospitalisation was falls (16 and 35 per 1,000 population respectively) (Table D1.03.15).
For First Nations people living in non-remote areas, falls were the most reported external cause of hospitalisation for both same-day and overnight hospitalisations (3.0 and 5.0 per 1,000). In remote areas (Remote and Very remote areas combined), the leading cause was assault (10 and 14 per 1,000, for same-day and overnight hospitalisations respectively) (Table D1.03.17).
Rates of hospitalisation due to assault for First Nations people were highest in Remote and very remote areas (2,351 per 100,000), and lowest in Major cities (321 per 100,000) (Table D2.10.6; see measure 2.10 Community safety).
Comparisons with non-Indigenous Australians
Deaths
In 2019–2023, after adjusting for differences in the age structure between the two populations, in the 5 jurisdictions with adequate Indigenous status identification First Nations people died from injury and poisoning at 2.0 times the rate of non-Indigenous Australians, or an additional 41 deaths per 100,000 population. The largest absolute differences in age-standardised death rates between the two populations were for:
- suicide – 27 deaths per 100,000 First Nations population compared with 12 per 100,000 non-Indigenous population (rate difference of 15 per 100,000 and rate ratio of 2.2)
- accidental poisoning – 15 deaths per 100,000 First Nations population compared with 4.8 per 100,000 non-Indigenous population (rate difference of 9.9 per 100,000 and rate ratio of 3.1)
- land transport accidents – 13 deaths per 100,000 First Nations population compared with 4.8 per 100,000 non-Indigenous population (rate difference of 8.5 per 100,000 and rate ratio of 2.8) (Table D1.23.10).
Hospitalisations
Between July 2021 to June 2023, the hospitalisation rate for injury and poisoning for First Nations people was higher than for non-Indigenous Australians across all age groups except 65 and over. The largest relative differences were in the 25–34, 35–44 and 45–54 age groups:
- For First Nations people aged 25–34, the hospitalisation rate for injury and poisoning was 53 per 1,000, which was 2.7 times the rate for non-Indigenous Australians (20 per 1,000).
- For First Nations people aged 35–44, the hospitalisation rate for injury and poisoning was 58 per 1,000, which was 3.1 times the rate for non-Indigenous Australians (19 per 1,000), the highest relative difference across all age groups.
- For First Nations people aged 45–54, the hospitalisation rate for injury and poisoning was 55 per 1,000, which was 2.4 times the rate for non-Indigenous Australians (23 per 1,000).
These differences were primarily due to the higher rates of hospitalisations due to assault for First Nations people in these age groups – 14, 19 and 17 times as high respectively for First Nations people as for non-Indigenous Australians (Table D1.03.15).
For both First Nations people and non-Indigenous Australians, hospitalisation rates for injury and poisoning were highest for those aged 65 and over, reflecting the higher number of falls among older people (Table D1.03.2, Figure 1.03.2). The hospitalisation rate for falls was higher for non-Indigenous Australians than for First Nations people aged 65 and over (45 and 35 hospitalisations per 1,000 population respectively). Conversely, First Nations people in this age group experienced a higher rate of hospitalisation for complications of medical and surgical care than non-Indigenous Australians (20 and 13 hospitalisations per 1,000 population respectively) (Table D1.03.15).
After adjusting for differences in the age structure between the two populations, First Nations people were 1.8 times as likely as non-Indigenous Australians to be hospitalised for injury and poisoning (Table D1.03.7).
The largest difference was for hospitalisations due to assault, with First Nations people experiencing an age-standardised rate of 7.8 per 1,000 which was 13 times the rate for non-Indigenous Australians (0.6 per 1,000) (Table D1.03.7, Figure 1.03.5).
For First Nations females, age-standardised rates of non-fatal hospitalisation for family violence-related assaults were 30 times the rate for non-Indigenous females (see also measure 2.10 Community safety) (Table D2.10.35).
Figure 1.03.5: Age-standardised hospitalisation rates for a principal diagnosis of injury and poisoning, by first reported external cause and Indigenous status, July 2021 to June 2023
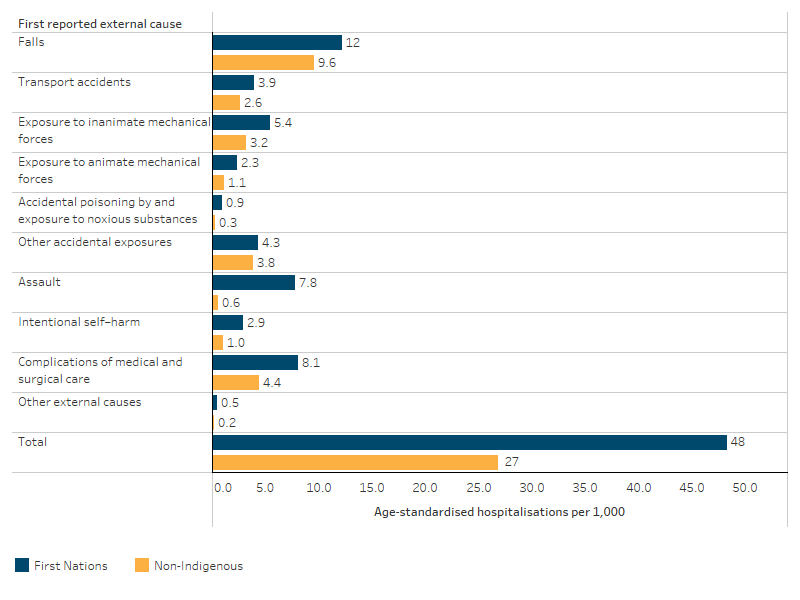
Source: Table D1.03.7. AIHW analysis of National Hospital Morbidity Database.
After adjusting for differences in age structure, hospitalisation rates for injury and poisoning were higher for First Nations people than non-Indigenous Australians in all jurisdictions (Table D1.03.3). The largest difference was for those living in the Northern Territory where the rate for First Nations people was 2.6 times as high as for non-Indigenous Australians.
Changes over time
Changes in deaths
Time series analysis of deaths data has been limited to the 2016 to 2021 period due to a break in time series for First Nations death statistics in New South Wales from 2022 (for more information see measure 1.22 All-cause age-standardised death rates and Data Sources and Quality).
Over the period 2016 to 2021 in the 5 jurisdictions with adequate Indigenous status identification, based on age-standardised rates, there was no significant change in the death rates due to injury and poisoning for First Nations people or non-Indigenous Australians. Over the same period, there were no significant changes in the absolute gap in death rates between the two populations (Table D1.23.19).
Changes in hospitalisations
The age-standardised hospitalisation rate for injury and poisoning increased by 8.8% for First Nations people and decreased by 8.4% for non-Indigenous Australians from 2016–17 to 2022–23. This resulted in a widening of the absolute gap from a difference of 16 per 1,000 in 2016–17 to 23 per 1,000 in 2022–23 (Table D1.03.5, Figure 1.03.6).
Note that some of the changes over time are affected by changes in coding practices. In particular, in New South Wales, from 2017–18, episodes of care delivered entirely within a designated emergency department or urgent care centre are no longer categorised as an admission regardless of the amount of time spent in hospital. This resulted in a reduction in the number of hospitalisations due to injury and poisoning in New South Wales (and nationally) between 2016–17 and 2017–18.
Figure 1.03.6: Age-standardised hospitalisation rates for a principal diagnosis of injury and poisoning, by Indigenous status, Australia, 2016–17 to 2022–23
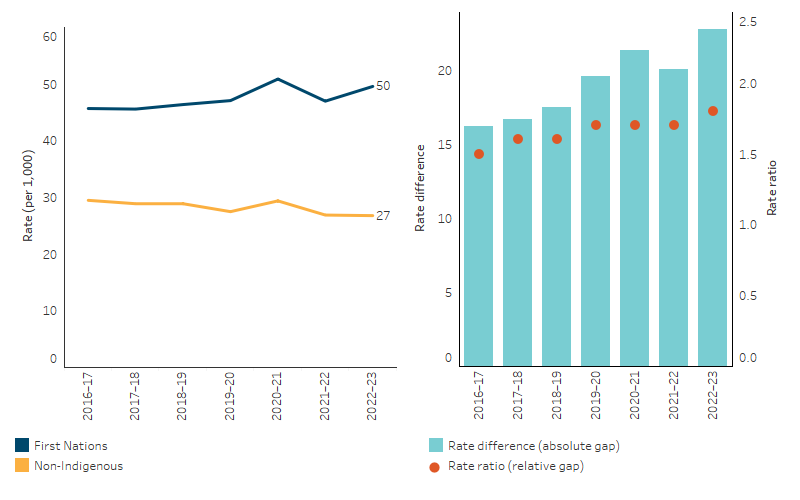
Notes:
1. A change in coding practices contributed to a decrease in the rate of hospitalisations between 2016–17 and 2017–18. See footnotes to Table D1.03.5 for details.
2. Rate difference is the age-standardised rate (per 1,000) for First Nations people minus the age-standardised rate (per 1,000) for non-Indigenous Australians. Rate ratio is the age-standardised rate for First Nations people divided by the age-standardised rate for non-Indigenous Australians.
Source: Table D1.03.5. AIHW analysis of National Hospital Morbidity Database.
Research and evaluation findings
Child injury
First Nations children disproportionately experience higher mortality and hospitalisation rates for some injury types. Evidence shows that family and community wellbeing are protective against child injury, with programs and services to support caregivers’ wellbeing leading to improvement in injury prevention for the child (Thurber et al. 2018) (see measure 1.13 Community functioning).
Over the period 2019–2023, among First Nations children aged 1–4, almost half of all deaths (46%) were due to injury and poisoning, including transport accidents and other accidents and injuries such as accidental drowning (in New South Wales, Queensland, Western Australia, South Australia and the Northern Territory combined) (Table D1.20.14) (see measure 1.20 Infant and child mortality).
A study using linked hospital data to construct cohorts of children born in New South Wales hospitals between 2003–07 and 2008–12 found that, in both cohorts, falls were the leading cause of injury followed by burns and poisoning for both First Nations and non-Indigenous children. While rates of injury in First Nations children caused by burns, poisoning and traffic were lower in the later cohort compared with the early cohort, overall rates of hospitalisation caused by unintentional injury remained similar in both cohorts. Injury hospitalisation inequalities between First Nations and non-Indigenous children remained similar across the period, with First Nations children almost twice as likely to suffer unintentional injury as non-Indigenous children (Möller et al. 2019).
A study of 21,189 children born in the Northern Territory (2000–2010) found that First Nations children had a 28.6% higher rate of unintentional injury hospitalisation (UIH) than non-Indigenous children (28.8 compared to 22.4 per 1,000 person-years). Falls were the most common cause of UIH, but First Nations children had higher rates of transport-related injuries (1.6 times), struck by or against objects (1.6 times), cut/pierce injuries (2.2 times), natural or environmental causes (1.5 times), and contact with fire or heat (2.6 times) compared to non-Indigenous children. Risk factors for UIH included being male (1.3 times), living in Remote (1.3 times) or Very remote areas (1.4 times), and having a notification (1.4 times) or substantiated notification for abuse (1.6 times) or neglect (1.3 times) (Su et al. 2024).
First Nations children aged 0–4 had approximately 3 times higher rates of hospitalised poisoning (1.3%) compared with non-Indigenous children (0.4%). Poisoning incidence peaked at 2–3 years of age and the primary outcome was hospitalisation for unintentional poisoning. Gender (male), socioeconomic disadvantage and geographical remoteness were associated with higher odds of poisoning hospitalisation for both First Nations and non-Indigenous children. This study highlights a need to develop culturally safe poisoning prevention strategies and policies (Lee et al. 2019).
Falls
Henry et al. (2025) surveyed 250 Torres Strait Islander adults aged 45 years and over (mean age 64 years) and found that 22% had experienced at least one fall in the past year, while 9% reported multiple falls. Among those who fell, 66% sustained an injury. Participants with poor mobility were 2.9 times more likely to have experienced a fall, and those with urinary incontinence were 2.5 times more likely to fall. Lukaszyk et al. (2017) used Yarning Circles across 6 sites in New South Wales to explore the perceptions of older First Nations people (aged 45 years and over) and found that falls were associated with physical disability, emotional distress, and reduced social connection, with fear of falling leading to withdrawal from daily activities. Many participants were unaware of existing fall prevention programs, citing limited availability, lack of healthcare provider referrals, and accessibility challenges as key barriers. Participants preferred ongoing, First Nations-specific, group-based programs delivered in a culturally safe setting, with transport support to improve accessibility and to better meet community needs.
Alcohol, substance use, and related self-harm
Alcohol and substance use are known risk factors in suicide (Robinson et al. 2011), transport accidents (West et al. 2014b; Fitts et al. 2017) as well as assault (Mitchell 2011) (see measures 2.16 Risky consumption of alcohol and 2.17 Drug and other substance use).
A study analysing 36,469 alcohol-related injury (ARI) hospitalisations in the Northern Territory across 2007–2022 found that First Nations people accounted for 82% of ARI hospitalisations. Alcohol use was associated with 32.6% of all injury hospitalisations among First Nations people, with an age-standardised ARI hospitalisation rate of 2,868 per 100,000, this was 11.5 times higher than for non-Indigenous people. Assault was the leading cause of alcohol-related injuries, accounting for 44% of hospitalisations among First Nations males and 61% among First Nations females, followed by falls, intentional self-harm, transport-related injuries, and contact with objects.
ARI hospitalisations in the Northern Territory among both First Nations and non-Indigenous Australians were higher than national estimates suggesting that risky drinking is an issue affecting both populations within the Northern Territory (Chen et al. 2025).
A study examining intensive care unit (ICU) admissions due to drug overdose (OD) in Australia and New Zealand from 2005 to 2013 found a significant increase among First Nations people. The rate of overdose-related ICU admissions for First Nations people rose more than tenfold, from 31 per million in 2005 to 436 per million in 2013, peaking at 553 per million in 2012. The proportion of First Nations ICU admissions that were due to OD also increased from 0.6% in 2005 to 2.6% in 2013. The study highlights that drug overdose is an increasing source of illness and death, particularly in younger and otherwise healthy individuals. The rising incidence of OD among First Nations people is a growing concern, with substantial loss of life-years (Cioccari et al. 2017).
A study in New South Wales found that First Nations patients had at least double the rate of hospital-treated deliberate self-poisoning compared with non-Indigenous Australians, with rising rates among young First Nations females since 2005. First Nations patients were also less likely to be discharged to a psychiatric hospital, which may reflect barriers in care or preferences for less restrictive, community-based support. Further investigation is needed to explore culturally inclusive, community-based aftercare models that improve support for First Nations people following hospital-treated self-harm (McGill et al. 2022).
Road injury
A number of factors contribute to the higher rates of injury in remote areas, where higher proportions of First Nations people than non-Indigenous Australians live. Risk factors include greater distances travelled, higher speed limits, poor condition of roads, poor availability of transport services, greater diversity in vehicle condition and delay in accessing medical treatment (Thomson et al. 2009).
A study examining road user behaviour and barriers to road safety among First Nations people in urban, regional and remote communities located in New South Wales and South Australia identified key risk behaviours contributing to transport-related injury. Of the 625 participants, 7% reported being involved in a car crash in the past 12 months, with 68% of those involved being the driver at the time, and 13% of drivers in crashes reported not holding a licence. While most participants reported consistent seatbelt use in the front seat (98%), compliance was lower for rear seatbelts (86%), particularly among younger people (80% among those aged 16–24). Some drivers (11%) reported regularly driving 10 km/h over the speed limit. Alcohol use and driving was uncommon, with 96% of drivers reporting it was unlikely they had driven over the legal blood alcohol limit in the past year, though 3.8% indicated they may have done so. Barriers to road safety, particularly in remote communities, included limited transport options, vehicle overcrowding, and unsafe driving practices (Cullen et al. 2020).
A broader analysis found that First Nations people experience disproportionately high rates of road trauma, with road traffic accidents being a leading cause of death and serious injury. They are up to 6 times more likely to be involved in a crash than non-Indigenous Australians, 2.7 times more likely to die in a vehicle accident, and 1.4 times more likely to sustain serious injuries. Passenger fatalities are particularly high, accounting for 61% of First Nations transport-related deaths, with First Nations passengers being 3 times more likely to be fatally injured than non-Indigenous passengers. Seatbelt non-use is a significant contributing factor, with 21% of First Nations motor vehicle occupants killed in crashes not wearing a seatbelt, and in the Northern Territory, 68% of First Nations’ road fatalities were attributed to lack of seatbelt use. First Nations children are at greater risk, being 4 times more likely to sustain serious injuries in car accidents, with 92% of those killed or seriously injured in the Northern Territory not properly restrained. Unlicensed driving remains a challenge, with financial, literacy, and systemic barriers limiting access to driver licensing. Alcohol-related crashes account for 66% of First Nations’ road fatalities, while driver distraction contributes to 35.4% of crashes in Northern Queensland. These findings highlight the need for targeted road safety interventions that address systemic factors contributing to the disproportionate rates of road injury and fatality among First Nations people (Pammer et al. 2021).
Suicide and self-harm
The suicide rate for First Nations people is twice that of non-Indigenous Australians, with young people under 18 significantly over-represented. These higher rates are linked to the impacts of colonisation, intergenerational trauma, contemporary disadvantage, and discrimination, which weaken protective factors such as family, community, and cultural resilience, and limit access to culturally appropriate services (Dudgeon et al. 2017). Suicide contagion in First Nations communities further compounds risk, as imitation and repetition of suicide within families, kinship groups, and close-knit networks lead to clusters and echo clusters of further suicides. This contagion effect has been especially pronounced among youth and young adults (Hanssens 2016).
First Nations young people in Australia experience suicide rates many times higher than their non-Indigenous peers. Higher prevalence of self-harm and suicidal ideation has been linked to incarceration, racial discrimination, emotional and social distress, and living in regional or remote areas (Dickson et al. 2019). Evidence from Queensland further shows that suicide rates among First Nations young people are more than 4 times higher than for non-Indigenous youth, with especially high rates among children under 15 and those in regional and remote areas. Rates were higher in communities with low cultural social capital and high levels of reported discrimination, highlighting the protective role of cultural connectedness and reduced discrimination as community-level strategies for suicide prevention (Gibson et al. 2021).
A systematic review found that while non-suicidal self-injury (NSSI) in First Nations populations has received limited research attention, existing evidence indicates that NSSI is linked to younger age, incarceration, and alcohol use. Prevalence estimates varied widely from: 0.9% in non-drinkers; to 14.3% in heavy or recently abstinent drinkers; and up to 22.5% in incarcerated youth. However, several studies found that NSSI rates in First Nations populations were not significantly higher than non-Indigenous Australians. The review also noted a lack of validated NSSI measures adapted for Indigenous populations (Black and Kisely 2018).
Implications
Injury is a leading cause of preventable death and disability in Australia, with most injuries avoidable by identifying risks and reducing exposure. This measure on injury and poisoning covers a broad range of policy, service delivery and health promotion issues such as suicide and self-harm, transport safety, accidental injury and community safety. Policy responses aimed at addressing injury prevention need to be evidence-based, multi-dimensional, place-based, culturally safe and address systemic issues that reduce people's capacity to make health-enhancing choices (Anderson 2008; Berger et al. 2009; Berry et al. 2009). Alcohol and substance use have been found to be a factor in suicide and transport accidents as well as assault (Mitchell 2011; Robinson et al. 2011; West et al. 2014a; Fitts et al. 2017). Strategies to prevent injuries should address road safety, child car safety and alcohol abuse.
In keeping with the holistic conceptualisation of health and wellbeing for First Nations people, safety promotion and injury prevention activities should also address the social, cultural and geographic context in which First Nations people live. Over the past decade, efforts to reduce First Nations child (0–4 years) death rates have focussed on reducing risk factors and improving maternal and child health particularly during pregnancy and infancy, as these factors have the most potential to affect child death rates. More research is needed to understand why improvements in health risk factors are not translating into stronger improvements in First Nations child (0–4) death rates (PM&C 2020). The high proportion of injury related deaths among First Nations children (1–4) may warrant more attention. Although these represent a smaller contribution to the overall number of deaths among First Nations children (0–4) they also represent an opportunity to address risks that are largely preventable such as transport accidents and drowning.
The National Aboriginal and Torres Strait Islander Safety Promotion Strategy highlights the need for culturally responsive approaches that address the unique social, emotional, and spiritual dimensions of injury in First Nations communities. It emphasises the importance of community-led action, improved data systems, and holistic safety promotion that builds on existing strengths and addresses systemic disadvantage.
First Nations people experience disproportionately higher rates of road trauma and road fatalities, than non-Indigenous Australians. The National Road Safety Strategy 2021–30 recognises the need for community-led, culturally appropriate approaches to improve safety outcomes. Effective initiatives such as child seat restraint programs, alternative transport options, and targeted safety interventions highlight the importance of tailored solutions. The strategy commits to stronger partnerships with First Nations communities to co-design road safety initiatives, ensuring alignment with the National Agreement on Closing the Gap Priority Reform One, and addressing barriers such as limited access to driver licensing and transport assistance. The National Road Safety Action Plan 2023–25 is the first implementation plan under the strategy, identifying First Nations people as a priority population. It focuses on enhancing road safety education, improving licensing access, and developing culturally appropriate countermeasures in collaboration with First Nations communities. Additionally, it commits to establishing baseline fatality data to inform targeted interventions and measure progress. Success will be evaluated through reductions in deaths and serious injuries, using data-driven insights to shape future road safety policies.
The National Disability Insurance Scheme (NDIS) provides funding for long-term, individualised care and support for people with permanent disabilities that significantly impact their communication, mobility, self-care, or self-management. It also connects all people with disability to community services, health care, education, and state and territory support programs. The NDIS First Nations Strategy 2025–2030 embeds the knowledge and experiences of First Nations people and reflects First Nations concepts of disability and wellbeing. It will guide actions to make the NDIS more equitable, culturally safe, community-centred and coordinated for First Nations people. An Implementation Plan to support the delivery of the strategy will be developed with the community in 2025 (see measure 1.14 Disability for more information).
The National Plan to End Violence against Women and Children 2022–2032 is a whole-of-government framework aimed at eliminating gender-based violence within one generation through prevention, early intervention, response, and recovery strategies. First Nations women and children experience disproportionately high rates of violence, driven by systemic disadvantage, intergenerational trauma, and barriers to accessing culturally safe services. To address these issues, the Aboriginal and Torres Strait Islander Action Plan 2023–2025 (Action Plan) provides a dedicated framework aligned with the National Agreement on Closing the Gap (National Agreement) Target 13-Family Safety, to reduce all forms of violence against Aboriginal and Torres Strait Islander women and children by at least 50% by 2031, as progress towards zero. Implementation of the Action Plan includes priority grants that are being rolled out across Australia based on community needs. Examples of grants include:
• Community-led Men’s Wellness Centres for Aboriginal and Torres Strait Islander peoples
• Family, domestic and sexual violence programs in Aboriginal and Torres Strait Islander community-controlled organisations (see measure 2.10 Community safety for more information).
The National Aboriginal and Torres Strait Islander Suicide Prevention Strategy 2025–2035 provides a community-led framework to achieve a significant and sustained reduction in suicide and self-harm among First Nations people towards zero. Grounded in leadership, cultural safety, and self-determination, it aligns with the National Agreement commitments and builds on key frameworks, including the Aboriginal and Torres Strait Islander Suicide Prevention Evaluation Project (ATSISPEP). The strategy emphasises culturally informed, strengths-based approaches that integrate social and emotional wellbeing, mental health, and suicide prevention. By embedding culturally safe, community-driven approaches into the broader mental health system, the strategy is a critical step towards zero suicide in First Nations communities (see measure 1.18 Social and emotional wellbeing for more information).
The Australian Government provides guidance on the Safe use of medicines, emphasising the importance of using medicines as directed, understanding their effects, and tracking usage to prevent misuse. Safe medicine practices help reduce the risks of overdose, addiction, adverse interactions, and the safe disposal of expired or unused medicines to prevent accidental poisoning or misuse. The National Return and Disposal of Unwanted Medicines Program (NatRUM) allows for environmentally safe disposal, reducing the risk of unintended harm.
References
-
AIHW (Australian Institute of Health and Welfare) (2022) 'Impact and causes of illness and death in Aboriginal and Torres Strait Islander people 2018', Australian Burden of Disease Study, AIHW, Australian Government, doi:10.25816/xd60-4366.
-
AIHW (2025) Suicide & self-harm monitoring, accessed 18 October 2025.
-
AIHW and Pointer SC (2019) 'Hospitalised injury among Aboriginal and Torres Strait Islander people, 2011–12 to 2015–16', Injury Research and Statistics, AIHW, Australian Government.
-
Anderson I (2008) 'An analysis of national health strategies addressing Indigenous injury: consistencies and gaps', Injury, 39:S55–S60, doi:10.1016/S0020-1383(08)70029-9.
-
Berger LR, Wallace LD and Bill NM (2009) 'Injuries and injury prevention among Indigenous children and young people', Pediatric Clinics, 56(6):1519–1537, doi:10.1016/j.pcl.2009.09.016.
-
Berry JG, Harrison JE and Ryan P (2009) 'Hospital admissions of Indigenous and non-Indigenous Australians due to interpersonal violence, July 1999 to June 2004', Australian and New Zealand Journal of Public Health, 33(3):215–222, doi:10.1111/j.1753-6405.2009.00378.x.
-
Black EB and Kisely S (2018) 'A systematic review: non-suicidal self-injury in Australia and New Zealand's indigenous populations', Australian Psychological Society, 53(1):3–12, doi:10.1111/ap.12274.
-
Boufous S, Ivers R, Senserrick T, Martiniuk A and Clapham K (2010), Underlying causes and effects of injury in Australian Aboriginal populations: a rapid review, report to the Department of Health, New South Wales Government, The Sax Institute.
-
Chen J, Zhang X, Draper A, Kaur G, Field E and Boffa J (2025) 'Alcohol-related injury hospitalisations in relation to alcohol policy changes, Northern Territory, Australia, 2007–2022: a joinpoint regression analysis', Drug and Alcohol Review, 44(1):324–335, doi:10.1111/dar.13976.
-
Cioccari L, Luethi N, Bailey M, Pilcher D and Bellomo R (2017) 'Characteristics and outcomes of critically ill patients with drug overdose in Australia and New Zealand', Critical Care and Resuscitation, 19(1):14–22, doi:10.1016/S1441-2772(23)00738-X.
-
Cullen P, Hunter K, Clapham K, Senserrick T, Rogers K, Harrison JE and Ivers RQ (2020) 'Road user behaviour, attitudes and crashes: a survey of Aboriginal and Torres Strait Islander people in Australia', Injury Prevention, 26(2):123–128, doi:10.1136/injuryprev-2018-043011.
-
Dickson JM, Cruise K, McCall CA and Taylor PJ (2019) 'A systematic review of the antecedents and prevalence of suicide, self-harm and suicide ideation in Australian Aboriginal and Torres Strait Islander youth', International Journal of Environmental Research and Public Health, 16(17):3154, doi:10.3390/ijerph16173154.
-
Dockery M, Moskos M, Isherwood L and Harris M (2022), How many in a crowd? Assessing overcrowding measures in Australian housing, Australian Housing and Urban Research Institute Limited, doi:10.18408/ahuri8123401.
-
Dudgeon P, Calma T and Holland C (2017) 'The context and causes of the suicide of Indigenous people in Australia', Journal of Indigenous Wellbeing: Te Mauri – Pimatisiwin, 2(2):5–15.
-
Fitts MS, Palk GR, Lennon AJ and Clough AR (2017) 'The characteristics of young Indigenous drink drivers in Queensland, Australia', Traffic Injury Prevention, 18(3):237–243, doi:10.1080/15389588.2016.1186273.
-
Gibson M, Stuart J, Leske S, Ward R and Tanton R (2021) 'Suicide rates for young Aboriginal and Torres Strait Islander people: the influence of community level cultural connectedness', Medical Journal of Australia, 214:514–518, doi:10.5694/mja2.51084.
-
Hanssens L (2016) 'The impact of suicide contagion and intergenerational segregation on youth and young adults in remote Indigenous communities in Northern Territory, Australia', Aboriginal and Islander Health Worker Journal, 40:38–47.
-
Haysom L, Indig D, Moore E and Gaskin C (2014) 'Intellectual disability in young people in custody in New South Wales, Australia–prevalence and markers', Journal of Intellectual Disability Research, 58(11):1004–1014, doi:10.1111/jir.12109.
-
Henry R, Sagigi B, Miller G, Russell SG, Thompson F, Quigley R and Strivens E (2025) 'The prevalence of falls and associated factors in older adults of the Torres Strait', Australasian Journal on Ageing, 44(1), doi:10.1111/ajag.13383.
-
Lee C, Hanly M, Larter N, Zwi K, Woolfenden S and Jorm L (2019) 'Demographic and clinical characteristics of hospitalised unintentional poisoning in Aboriginal and non-Aboriginal preschool children in New South Wales, Australia: a population data linkage study', BMJ Open, 9(1):e022633, doi:10.1136/bmjopen-2018-022633.
-
Lukaszyk C, Coombes J, Turner NJ, Hillmann E, Keay L, Tiedemann A, Sherrington C and Ivers R (2017) 'Yarning about fall prevention: community consultation to discuss falls and appropriate approaches to fall prevention with older Aboriginal and Torres Strait Islander people', BMC Public Health, 18(1):77, doi:10.1186/s12889-017-4628-6.
-
McGill K, Salem A, Hanstock TL, Heard TR, Garvey L, Leckning B, Whyte I, Page A and Carter G (2022) 'Indigeneity and likelihood of discharge to psychiatric hospital in an Australian deliberate self-poisoning hospital-treated cohort', International Journal of Environmental Research and Public Health, 19(19):12238, doi:10.3390/ijerph191912238.
-
Mitchell L (2011) 'Domestic violence in Australia: an overview of the issues', Department of Parliamentary Services, Australian Government.
-
Möller H, Falster K, Ivers R, Falster M, Clapham K and Jorm L (2017) 'Closing the Aboriginal child injury gap: targets for injury prevention', Australian and New Zealand Journal of Public Health, 41(1):8–14, doi:10.1111/1753-6405.12591.
-
Möller H, Ivers R, Clapham K and Jorm L (2019) 'Are we closing the Aboriginal child injury gap? A cohort study', Australian and New Zealand Journal of Public Health, 43(1):15–17.
-
Pammer K, Freire M, Gauld C and Towney N (2021) 'Keeping safe on Australian roads: overview of key determinants of risky driving, passenger injury, and fatalities for Indigenous populations', International Journal of Environmental Research and Public Health, 18(5):2446, doi:10.3390/ijerph18052446.
-
PM&C (Department of the Prime Minister and Cabinet) (2020) 'Closing the Gap report 2020', Closing the Gap, PM&C, Australian Government.
-
Robinson G, Silburn S and Leckning B (2011), Suicide of children and youth in the NT 2006–2010: public release report for the Child Deaths Review and Prevention Committee, Menzies Centre for Child Development and Education, Menzies School of Health Research, Darwin, doi:10.13140/RG.2.1.2364.3766.
-
Silburn S, Robinson G, Leckning B, Henry D, Cox A and Kickett D (2014) 'Preventing suicide among Aboriginal Australians', in Dudgeon P, Milroy H and Walker R (eds) Working together: Aboriginal and Torres Strait Islander mental health and wellbeing principles and practice, 2nd edn, Telethon Institute for Child Health Research, Kulunga Research Network, The University of Western Australia, The Department of Prime Minister and Cabinet, Australian Government.
-
Stephens A, Cullen J, Massey L and Bohanna I (2014) 'Will the National Disability Insurance Scheme improve the lives of those most in need? Effective service delivery for people with Acquired Brain Injury and other disabilities in remote Aboriginal and Torres Strait Islander communities', Australian Journal of Public Administration, 73(2):260–270, doi:10.1111/1467-8500.12073.
-
Su J, He V, Lithgow A and Guthridge S (2024) 'Risk factors for unintentional injury hospitalisation among Aboriginal and non-Aboriginal children in Australia’s Northern Territory: a data linkage study', PLoS One, 19(11):e0311586, doi:10.1371/journal.pone.0311586.
-
Thomson N, Krom I and Ride K (2009), Summary of road safety among Indigenous peoples, Australian Indigenous HealthInfoNet.
-
Thurber K, Burgess L, Falster K, Banks E, Möller H, Ivers R, Cowell C, Isaac V, Kalucy D and Fernando P (2018) 'Relation of child, caregiver, and environmental characteristics to childhood injury in an urban Aboriginal cohort in New South Wales, Australia', Australian and New Zealand Journal of Public Health, 42(2):157–165, doi:10.1111/1753-6405.12747.
-
West C, Usher K and Clough A (2014a) 'Study protocol - resilience in individuals and families coping with the impacts of alcohol related injuries in remote Indigenous communities: a mixed method study', BMC Public Health, 14:479, doi:10.1186/1471-2458-14-479.
-
West R, Usher K, Foster K and Stewart L (2014b) 'Academic staff perceptions of factors underlying program completion by Australian Indigenous nursing students', The Qualitative Report, 19(12):2, doi:10.46743/2160-3715/2014.1257.

