Key messages
Why is it important?
Understanding the leading causes of death among Aboriginal and Torres Strait Islander (First Nations) people provides critical insight into health disparities and helps identify where targeted policy and service responses are needed. These insights support the development of culturally safe, community led health programs and inform progress against key Closing the Gap targets, particularly for life expectancy and suicide.
Data findings
- Nationally, over the 5-year period 2019–2023, there were 22,275 deaths of First Nations people. In the same 5-year period for the 5 jurisdictions with adequate Indigenous status identification, there were 19,993 deaths of First Nations people.
- The leading 5 broad causes of death for First Nations people in the 5-year period 2019–2023 were cancer and other neoplasms (24% of deaths), cardiovascular disease (21%), injury and poisoning (14%), respiratory disease (9.4%) and endocrine, nutritional and metabolic diseases (8.8%).
- The leading broad causes of death differed by age. For First Nations people aged 0–14, conditions originating in the perinatal period was the leading cause of death while for those aged 15–44 it was injury and poisoning. For those aged 45–54 cardiovascular disease was the leading cause of death while for those aged 55 and over cancer and other neoplasms was the leading broad cause.
- In 2019–2023, death rates for First Nations males were higher than for First Nations females across most broad causes of death. The largest relative difference in death rates between First Nations males and females was for injury and poisoning, where the rate for males was 2.2 times as high as the rate for females.
- In 2019–2023, the top 5 specific causes of death for First Nations people were coronary heart disease (11% of deaths), diabetes (7.3%), chronic obstructive pulmonary disease (6.4%), lung cancer (6.0%) and intentional self-harm (5.2%).
- After adjusting for differences in the age structure of the two populations, death rates were between 1.4 and 3.6 times as high for First Nations people as for non-Indigenous Australians across all broad causes of death except one. The exception was for nervous system diseases, where the age-standardised rates were similar.
- Cardiovascular disease accounted for the largest gap in death rates between First Nations people and non-Indigenous Australians in 2019–2023 (77 more deaths per 100,000 population for First Nations people), followed by cancer and other neoplasms (72 per 100,000), and endocrine, nutritional and metabolic diseases (60 per 100,000).
- Over the period from 2016 to 2021, the age-standardised death rates for First Nations people due to cardiovascular disease and injury and poisoning did not change significantly, nor did the absolute difference in rates between First Nations people and non-Indigenous Australians. Age-standardised rates for deaths due to cancer and other neoplasms increased by 15% for First Nations people and the absolute difference in rates between the two populations widened.
Research and evaluation findings
- Multimorbidity is more prevalent among First Nations people and is a key factor contributing to higher death rates.
- A large proportion of the improvement in First Nations life expectancy in the Northern Territory between 1999 and 2018 was attributable to fewer years of life being lost due to cancer, injuries and chronic disease.
- Since the introduction of the Better Cardiac Care project there have been improvements in the level of access to cardiac-related health services, increased proportion of First Nations people who received Medicare-funded health assessments and reductions in the death rate due to cardiac conditions.
- Diabetes-related deaths are significantly higher in remote areas, and better access to primary care is linked to improved management and fewer hospitalisations.
- The Tackling Indigenous Smoking (TIS) program is associated with reduced smoking rates and increased use of cessation services.
Implications
The leading causes of death among First Nations people highlight the need for improved access to culturally safe and well-resourced primary health care and specialist services, particularly for early detection and management of chronic conditions. Programs delivered through Aboriginal Community Controlled Health Organisations, such as Deadly Choices, Culture Care Connect, and cancer screening initiatives, support targeted responses to coronary heart disease, diabetes, cancer, suicide, and respiratory disease. Continued investment in prevention, early intervention, and service coordination is required to reduce avoidable deaths and contribute to Closing the Gap targets. Addressing the upstream modifiable risk factors and social determinants of health are crucial but need to be understood in the context of the ongoing impacts of colonisation, including intergenerational trauma, systemic and interpersonal racism, and the disruption of cultural, social, and economic systems. The broader heath system has its role to play by eliminating racism, adapting services to more appropriately meet the needs of First Nations people, and working in partnership with First Nations people.
Why is it important?
Analysis of leading causes of death can provide insights into the overall health status of different populations, as well as a better understanding of the contributing factors, and indicate areas needing policy focus. Disparities in mortality within the Aboriginal and Torres Strait Islander (First Nations) population and between First Nations people and non-Indigenous Australians for particular causes of death can provide insight into where policy attention is needed to close the gap. As the health status of First Nations people improves, the rate of premature deaths is expected to decrease over time.
Understanding the leading causes of death is particularly important for the health and wellbeing of First Nations people as it enables the development of targeted interventions and the allocation of resources to where they are most needed, and to the services best equipped to provide appropriate care. Working with communities to identify leading causes of death can empower them to take proactive steps in improving their health and wellbeing.
This measure provides a high-level exploration of leading causes of death which are explored in further detail in the subject specific measures within Tier 1 of the Health Performance Framework. The types of diseases causing the most deaths for both First Nations people and non-Indigenous Australians are somewhat similar, although occurring at different rates and different ages. However, there have been different patterns in the trends for specific causes over time. There are also differences in the leading causes of death between different subgroups of the First Nations population. Identifying these differences allows for targeted analysis and intervention to reduce mortality.
The National Agreement on Closing the Gap (the National Agreement), was developed in partnership between Australian governments and the Coalition of Aboriginal and Torres Strait Islander Peak Organisations. It is built around 4 Priority Reforms directly informed by First Nations people. These reforms aim to change how governments work with First Nations people by fostering partnership and shared decision-making, building the Aboriginal community-controlled sector, transforming government organisations, and improving and sharing access to data and information to enable informed decision making by First Nations communities. The National Agreement has identified the importance of making sure First Nations people enjoy long and healthy lives, children are born healthy and strong, and that First Nations people enjoy high levels of social and emotional wellbeing. To achieve these outcomes the National Agreement specifically outlines the following targets to direct policy attention and monitor progress:
- Target 1– Close the Gap in life expectancy within a generation, by 2031 (with leading causes of death as a supporting indicator).
- Target 2 – By 2031, increase the proportion of Aboriginal and Torres Strait Islander babies with a healthy birthweight to 91 per cent.
- Target 14 – Significant and sustained reduction in suicide of Aboriginal and Torres Strait Islander people towards zero.
These targets are part of a broader framework aimed at addressing various socioeconomic and health disparities faced by First Nations communities.
For the latest data on the Closing the Gap targets, see the Closing the Gap Information Repository.
As life expectancy estimates for First Nations people are published every 5 years by the Australian Bureau of Statistics (ABS), the National Agreement also identified several supporting indicators, which may be used to direct policy attention and provide proxy information for monitoring progress towards the target in the intervening years (Productivity Commission 2021). One of the supporting indicators for this target is leading causes of death (the focus of this HPF measure). Other supporting indicators that draw on deaths data are all-cause mortality and potentially avoidable death rates (see measures 1.22 All-cause age-standardised death rates and 1.24 Avoidable and preventable deaths, respectively, for information on these topics).
The National Aboriginal and Torres Strait Islander Health Plan 2021–2031 (the Health Plan) provides a strong overarching policy framework for First Nations health and wellbeing and is the first national health document to address the health targets and priority reforms of the National Agreement.
The vision of the Health Plan is that First Nations people enjoy long, healthy lives centred in culture, with access to services that are prevention-focused, culturally safe and responsive, equitable, and free of racism.
Priority 9 of the Health Plan focuses on improving access to person-centred and family-centred care. Early access to responsive primary care, and addressing barriers to accessing care, are identified by the Health Plan as key to addressing high hospitalisation rates of First Nations people, where presentation often occurs at a later stage of disease.
Both the National Agreement and the Health Plan are discussed further in the Implications section of this measure.
Burden of disease
Burden of disease analysis combines the years of healthy life lost due to living with ill health (non-fatal burden) with the years of life lost due to dying prematurely (fatal burden).
In 2018, First Nations people lost 113,445 years of life due to dying prematurely, equivalent to 137 years of life lost per 1,000 people.
Four disease groups accounted for over two-thirds of fatal burden that First Nations people experienced in 2018: injuries (23%), cancer (20%), cardiovascular (or circulatory) diseases (19%) and infant and congenital conditions (9%).
For First Nations children aged under 1, infant and congenital conditions were responsible for the majority of fatal burden in 2018 (82%). For First Nations people aged under 45 (excluding infants), injuries were the leading cause of fatal burden (47% of fatal burden among those aged 1–14, and 80% for those aged 15–24). Among First Nations people aged 45 and over, chronic diseases were the main contributors to fatal burden (with cancer and cardiovascular (or circulatory) diseases contributing 30% and 25%, respectively) (AIHW 2022a).
Data findings
Deaths data in this measure are sourced from the National Mortality Database (NMD). The data are used to report the total number of deaths in Australia (nationally), which includes Australian residents of all states and territories. However, when reporting death rates, data are limited to 5 jurisdictions (New South Wales, Queensland, Western Australia, South Australia and the Northern Territory), in which the quality of Indigenous status identification in the deaths data is considered adequate. National death rates are not published due to concerns around the quality of Indigenous status identification in Victoria, Tasmania and the Australian Capital Territory. Data held within the NMD are supplied from the ABS Causes of Death collection. Currently, the ABS is undertaking significant work to improve the identification of First Nations people in this collection by working directly with the Registries of Births, Deaths and Marriages in each state and territory (ABS 2023a).
When reporting death rates by remoteness, data from all jurisdictions are included.
Nationally, over the 5-year period 2019–2023, there were 22,275 deaths of First Nations people.
In the same 5-year period for the 5 jurisdictions with adequate Indigenous status identification, there were 19,993 deaths of First Nations people, corresponding to a crude rate of 464 per 100,000 population. The top 5 broad leading causes of death were:
- cancer and other neoplasms, accounting for almost one-quarter (24% or 4,773 deaths) of all deaths
- cardiovascular diseases (21%, 4,283 deaths) - for example, heart attack
- injury and poisoning (14%, 2,739 deaths), including suicide (intentional self-harm)
- respiratory diseases (9.4%, 1,871 deaths), including chronic obstructive pulmonary disease
- endocrine, nutritional and metabolic diseases (8.8%, 1,758 deaths), including diabetes (Table D1.23.1, Figure 1.23.1).
Figure 1.23.1: Leading broad causes of death for First Nations people, NSW, Qld, WA, SA and NT, 2019–2023
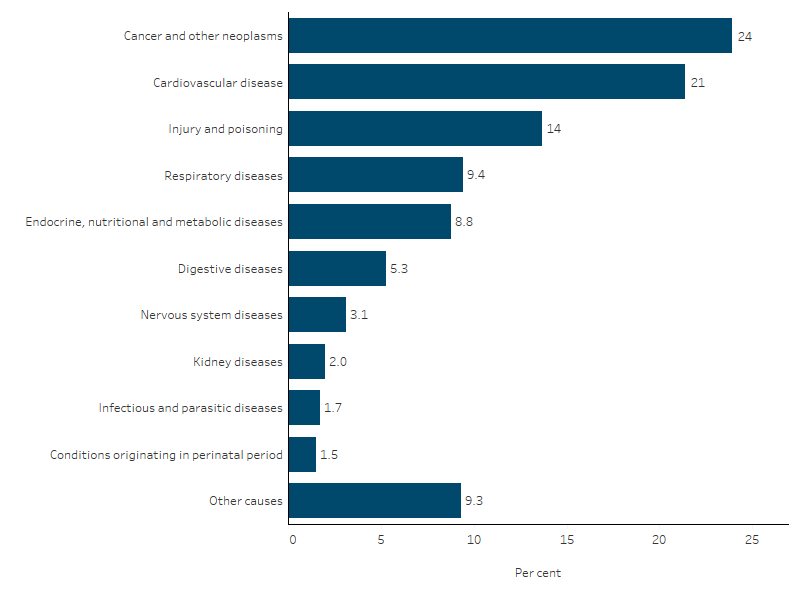
Note: ‘Other causes’ include diseases of blood and blood-forming organs; mental and behavioural disorders; diseases of the eye and adnexa; diseases of the ear and mastoid process; diseases of the skin and subcutaneous tissue; diseases of the musculoskeletal system and connective tissue; diseases of the genitourinary system (excluding kidney diseases); pregnancy, childbirth and the puerperium; congenital malformations, deformations and chromosomal abnormalities; symptoms, signs and abnormal clinical findings not elsewhere classified; codes for special purposes. See table D1.23.1 for a full list of ICD-10 codes.
Source: Table D1.23.1. AIHW National Mortality Database.
Leading broad cause by sex and age
In 2019–2023, among First Nations people in New South Wales, Queensland, Western Australia, South Australia and the Northern Territory:
- Cancer and other neoplasms was the leading broad cause of death for both males and females, accounting for 23% (2,525 deaths) and 25% (2,248 deaths) of all deaths, respectively.
- Cardiovascular diseases was the second leading broad cause of death for both males and females, accounting for 22% (2,387 deaths) and 21% (1,896 deaths), respectively.
- For males, injury and poisoning was the third leading broad cause of death (17% or 1,897 deaths), while for females it was endocrine, nutritional and metabolic diseases (11% or 965 deaths) (Table D1.23.1, Figure 1.23.2).
In 2019–2023, death rates for First Nations males were higher than for First Nations females across most broad causes of death, with the exception of endocrine, nutritional and metabolic diseases (37 compared with 45 deaths per 100,000 population, respectively) and kidney diseases (7.7 compared with 11 per 100,000, respectively), where rates were higher for females. The largest relative difference in death rates between First Nations males and females was for injury and poisoning, where the rate for males was 2.2 times as high as the rate for females. Deaths due to injury and poisoning also accounted for the largest absolute difference in death rates between First Nations males and females, with a difference of 49 deaths per 100,000 population (88 compared with 39 per 100,000, respectively) (Table D1.23.1).
Figure 1.23.2: Leading broad causes of death for First Nations people, by sex, NSW, Qld, WA, SA and NT, 2019–2023
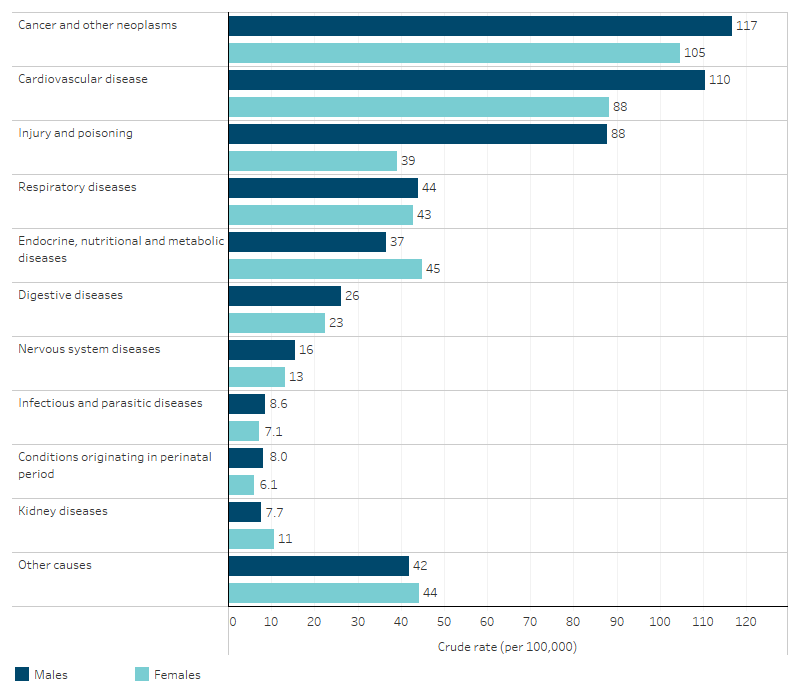
Note: ‘Other causes’ includes diseases of blood and blood-forming organs; mental and behavioural disorders; diseases of the eye and adnexa; diseases of the ear and mastoid process; diseases of the skin and subcutaneous tissue; diseases of the musculoskeletal system and connective tissue; diseases of the genitourinary system (excluding kidney diseases); pregnancy, childbirth and the puerperium; congenital malformations, deformations and chromosomal abnormalities; symptoms, signs and abnormal clinical findings not elsewhere classified; codes for special purposes. See table D1.23.1 for a full list of ICD-10 codes.
Source: Table D1.23.1. AIHW National Mortality Database.
In 2019–2023, the leading broad causes of death differed by age:
- For First Nations people aged 0–14, conditions originating in the perinatal period was the leading broad cause of death (21 deaths per 100,000).
- For First Nations people aged 15–24, 25–34 and 35–44 the leading broad cause of death was injury and poisoning (63, 94 and 120 deaths per 100,000, respectively).
- For First Nations people aged 45–54 cardiovascular disease was the leading broad cause of death (182 deaths per 100,000).
- For First Nations people aged 55–64, 65–74 and 75 and over, cancer and other neoplasms was the leading broad cause of death (409, 860 and 1,744 deaths per 100,000, respectively) (Table D1.23.3).
Leading broad cause by states and territories
Across the 5 jurisdictions with adequate Indigenous status identification in 2019–2023, there were differences in the leading broad cause of death among First Nations people:
- In New South Wales and Queensland, cancer and other neoplasms was the leading cause accounting for 27% (1,876 deaths) and 26% (1,501 deaths) of all deaths, respectively.
- In Western Australia, South Australia and the Northern Territory, cardiovascular disease was the leading cause, accounting for 761, 284 and 608 deaths respectively, or around 22% of all deaths.
- Injury and poisoning accounted for a higher proportion of deaths in Western Australia (18% or 578 deaths) than in the other 4 jurisdictions (between 13% and 14% of deaths).
- The proportion of total deaths due to respiratory disease was higher in New South Wales and South Australia (both 11% of deaths, 790 and 137 deaths respectively), compared with the other 3 jurisdictions (7–9% of deaths).
- The proportion of total deaths due to endocrine, nutritional and metabolic diseases – which includes diabetes – was higher in the Northern Territory (14%, 379 deaths, compared with 7–10% in the other 4 jurisdictions) (Table D1.23.2, Figure 1.23.3).
Figure 1.23.3: Leading broad causes of death for First Nations people, by jurisdiction, NSW, Qld, WA, SA and NT, 2019–2023
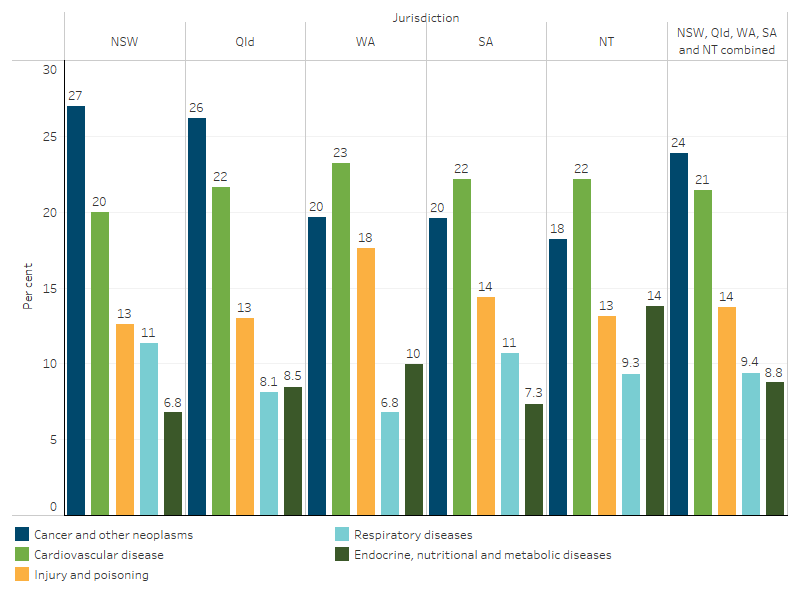
Source: Table D1.23.2. AIHW National Mortality Database.
Leading broad causes by remoteness
During 2019–2023, for First Nations people, the relative contribution of different broad leading causes of death in non-remote areas (Major cities, Inner regional and Outer regional areas combined) differed from that in remote areas (Remote and Very remote areas combined):
- In non-remote areas, cancer and other neoplasms accounted for the highest proportion of deaths (26% or 3,259 deaths), followed by cardiovascular disease (21% or 2,632), injury and poisoning (14% or 1,821), respiratory diseases (9.5% or 1,199), and endocrine, nutritional and metabolic diseases (7.3% or 925).
- In remote areas, cardiovascular disease was the leading broad cause of death (24% or 960), followed by cancer and other neoplasms (20% or 812), injury and poisoning (14% or 558), endocrine, nutritional and metabolic diseases (12% or 497), and respiratory diseases (8.3% or 334).
Among First Nations people, death rates for the 5 broad leading causes were higher for those living in remote areas than for those in non-remote areas. The largest relative difference was for endocrine, nutritional and metabolic diseases, where the rate was 3 times as high for those living in remote areas compared with those in non-remote areas (66 compared with 22 per 100,000 population) (Table D1.23.30, Figure 1.23.4).
Figure 1.23.4: Leading broad causes of death for First Nations people, by remoteness, Australia, 2019–2023
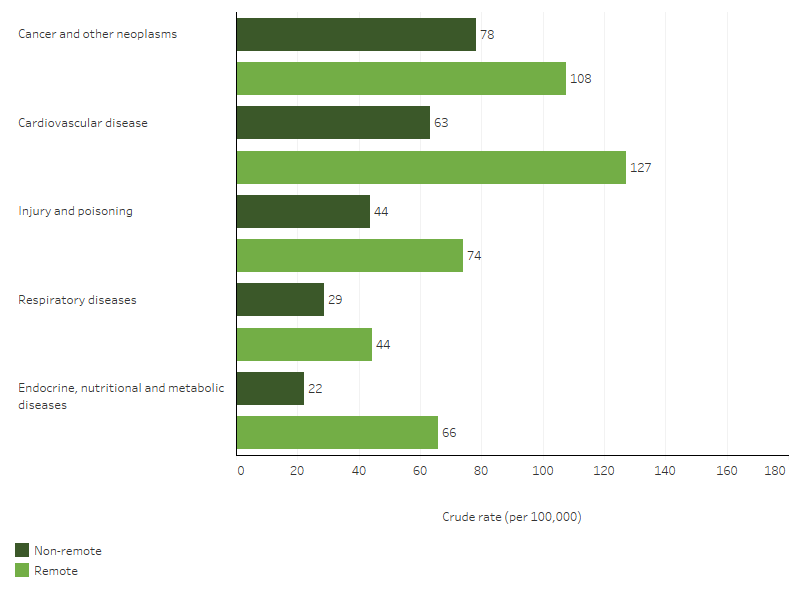
Source: Table D1.23.30. AIHW National Mortality Database.
Leading specific causes of death
This section focuses on the specific leading causes of death. That is, individual diseases, conditions or injuries which accounted for the most deaths of First Nations people. It first looks at the leading specific causes independent of broad cause and then the specific causes of death within the 3 leading broad causes of death (ICD-10 chapter). This section is limited to the 5 jurisdictions with adequate Indigenous status identification over the time period presented.
Among First Nations people, in 2019–2023 and irrespective of ICD-10 chapter, the top 5 specific leading causes of death were:
- coronary heart disease (11% or 2,259 of 19,993 deaths), with a rate of 52 coronary heart disease deaths per 100,000 population
- diabetes (7.3% or 1,452 deaths), with a rate of 34 deaths per 100,000
- chronic obstructive pulmonary diseases (6.4% or 1,270 deaths), with a rate of 29 deaths per 100,000
- lung cancer (6.0% or 1,194 deaths), with a rate of 28 deaths per 100,000
- intentional self-harm (5.2% or 1,046 deaths), with a rate of 24 deaths per 100,000 (Table D1.23.33)
Over the same 5-year period (2019–2023), for First Nations people, specific leading causes of death differed by age:
- For First Nations children aged 0–4, the leading cause of death was due to perinatal and congenital conditions (this includes conditions originating in the perinatal period, congenital malformations, deformations and chromosomal abnormalities) which accounted for 60% (403 deaths) of all deaths, at a rate of 85 deaths per 100,000.
- For those aged 5–14 the leading cause of death was due to land transport accidents which accounted for just over one-quarter of deaths (26% or 43 deaths), with a rate of 8.9 per 100,000.
- Intentional self-harm was the leading cause of death for First Nations people aged 15–44, accounting for one-quarter of deaths for this age group (25% or 825 deaths) with the rate highest among those aged 25–34 (105 deaths per 100,000).
- Coronary heart disease was the leading cause for those aged 45–74, accounting for 13% (1,475) of deaths, and peaking at a rate of 748 deaths per 100,000 for those aged 65–74.
- For those aged 75 and over, dementia (including Alzheimer’s disease) was the leading cause accounting for more than 1 in 10 deaths (11% or 540 deaths), at a rate of 820 deaths per 100,000 (Table D1.23.34, Figure 1.23.5).
Figure 1.23.5: Leading specific causes of death for First Nations people by age group, NSW, Qld, WA, SA and NT, 2019–2023
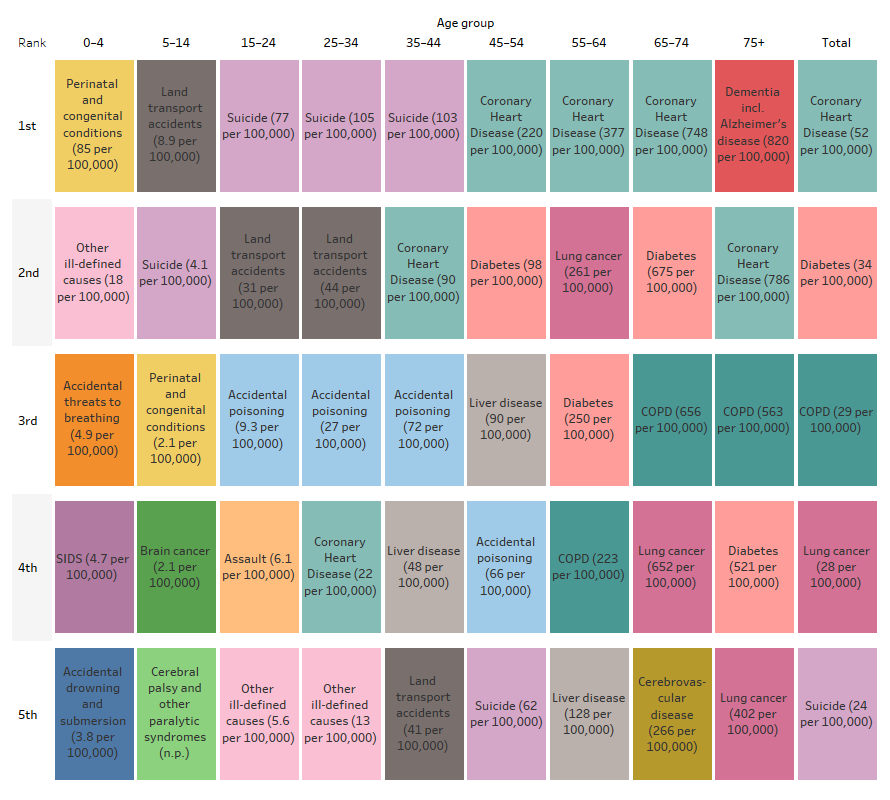
Note: SIDS Sudden infant death Syndrome; COPD Chronic obstructive pulmonary disease; Certain conditions originating in the perinatal period, congenital malformations, deformations and chromosomal abnormalities abbreviated as Perinatal and congenital conditions.
Source: Table D1.23.34. AIHW National Mortality Database.
Specific causes contributing to the top 3 leading broad causes of death
Deaths due to cancer and other neoplasms
In 2019–2023, nearly one quarter (24%, 4,773 deaths) of deaths among First Nations people were due to cancer and other neoplasms at a rate of 111 deaths per 100,000 population (Table D1.23.1). Of all cancer and other neoplasms deaths, the leading specific causes were:
- lung cancer, accounting for 25% (1,194) of these deaths, at a rate of 28 deaths per 100,000 population
- colorectal (bowel) cancer (7.8% or 371 deaths) at a rate of 8.6 per 100,000
- liver cancer (7.7% or 367 deaths) at a rate of 8.5 per 100,000 (Table D1.23.12, Figure 1.23.6).
While the proportion of cancer and other neoplasms deaths that were due to lung and colorectal cancer was similar between First Nations males and females (25% compared with 26% and 7.9% compared with 7.6%), breast cancer was the second specific leading cause of cancer death for females while liver cancer was the second leading cause of cancer death among males (Table D1.23.12). See measure 1.08 Cancer for more information.
Figure 1.23.6: Top 3 broad leading causes of death for First Nations people, by specific cause, NSW, Qld, WA, SA and NT, 2019–2023
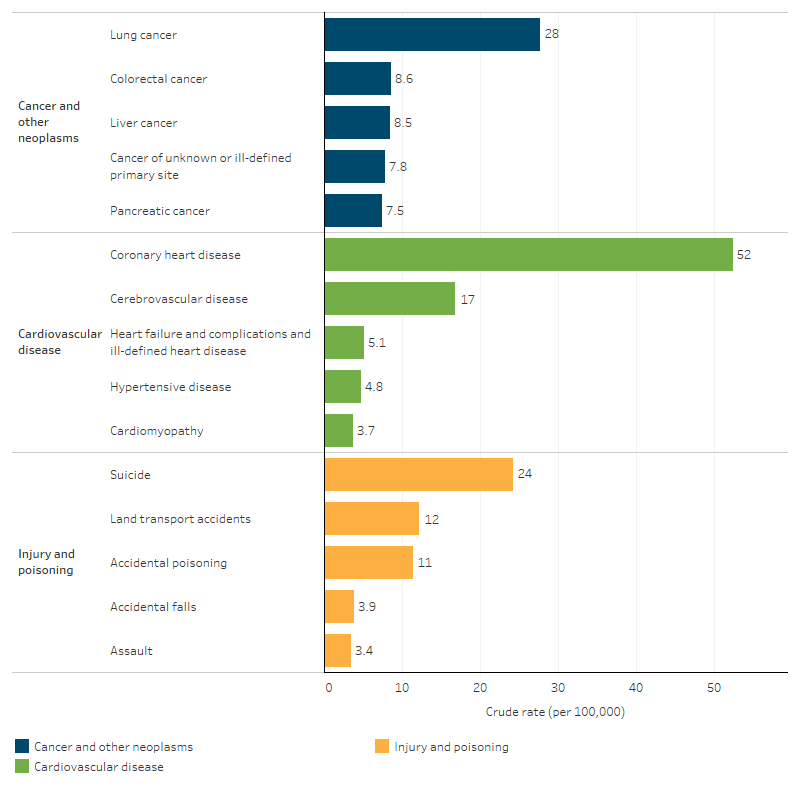
Sources: Tables D1.23.8, D1.23.10, D1.23.12. AIHW National Mortality Database.
Deaths due to cardiovascular disease
For First Nations people, in 2019–2023, 21% of all deaths were due to cardiovascular disease (4,283 deaths), corresponding to a rate of 99 deaths per 100,000 population (Table D1.23.1). The leading specific causes of cardiovascular disease deaths were:
- coronary heart disease (also known as ischaemic heart disease), accounting for over half (53% or 2,259 deaths) of all cardiovascular disease deaths at a rate of 52 deaths per 100,000 population
- cerebrovascular disease (17% or 723 deaths) at a rate of 17 per 100,000
- heart failure and complications and ill-defined heart disease (5.1% or 219 deaths) at a rate of 5.1 deaths per 100,000.
For deaths due to coronary heart disease, people aged 55–64 accounted for a higher proportion of deaths than those aged 75 and over (24% compared with 23%). For deaths due to cerebrovascular disease, the reverse was true, with people aged 75 and over accounting for a higher proportion of the deaths (22% compared with 33%) (Table D1.23.9). See measure 1.05 Cardiovascular disease for more information.
Deaths due to injury and poisoning
During 2019–2023, for First Nations people, 2,739 deaths (14% of all deaths) were due to injury and poisoning at a rate of 64 deaths per 100,000 population (Table D1.23.1). The leading specific causes of injury and poisoning deaths were:
- intentional self-harm (suicide), accounting for 38% (1,046 deaths) of all injury and poisoning deaths. The rate of deaths due to intentional self-harm was 24 deaths per 100,000 population
- land transport accidents (19% or 527 deaths) at a rate of 12 deaths per 100,000
- accidental poisoning (18% or 492 deaths) at a rate of 11 deaths per 100,000.
The leading cause of deaths due to injury and poisoning differed by age. For those aged 0–14 the leading cause was land transport accidents, which accounted for over one-third (34%) of injury and poisoning deaths. For those aged 15–44 the leading cause of death was intentional self-harm, accounting for 50% of injury and poisoning deaths. The leading cause of death for those aged 45–64 was accidental poisoning (29% of deaths), while for those aged 65 and over it was accidental falls (42% of deaths) (Table D1.23.11). See measures 1.03 Injury and poisoning and 1.18 Social and emotional wellbeing for more information.
Comparison with non-Indigenous Australians
Differences in broad causes of death
After adjusting for differences in the age structure of the two populations, in 2019–2023 in the 5 jurisdictions with adequate Indigenous status identification, death rates were between 1.4 and 3.6 times as high for First Nations people as for non-Indigenous Australians across all broad causes of death except one. The exception was for nervous system diseases, where the age-standardised rates were similar (ratio of 1.0) (Table D1.23.1).
Cardiovascular disease accounted for the largest gap in death rates between First Nations and non-Indigenous Australians (rate difference of 77 deaths per 100,000 population, based on age-standardised data). This was followed by cancer and other neoplasms (gap of 72 per 100,000); endocrine, nutritional and metabolic diseases (including diabetes) (gap of 60 per 100,000); and respiratory diseases (gap of 52 per 100,000) (Table D1.23.1, Figure 1.23.7).
Figure 1.23.7: Gap in age-standardised death rates for broad leading causes between First Nations people and non-Indigenous Australians, NSW, Qld, WA, SA and NT, 2019–2023
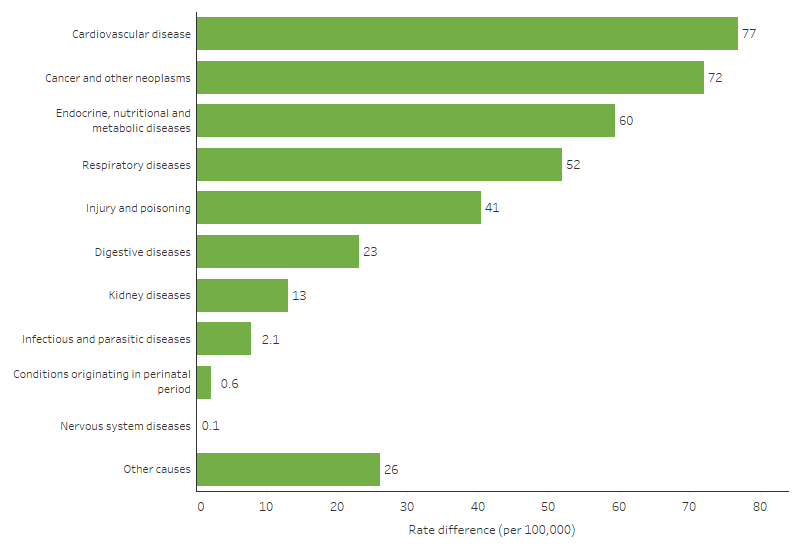
Note: ‘Other causes’ diseases of blood and blood-forming organs; mental and behavioural disorders; diseases of the eye and adnexa; diseases of the ear and mastoid process; diseases of the skin and subcutaneous tissue; diseases of the musculoskeletal system and connective tissue; diseases of the genitourinary system (excluding kidney diseases); pregnancy, childbirth and the puerperium; congenital malformations, deformations and chromosomal abnormalities; symptoms, signs and abnormal clinical findings not elsewhere classified; codes for special purposes. See table D1.23.1 for a full list of ICD-10 codes.
Source: Table D1.23.1. AIHW National Mortality Database.
In Western Australia, South Australia and the Northern Territory, cardiovascular disease was the leading contributor to the gap (a gap of 153, 104 and 210 per 100,000, respectively). In New South Wales and Queensland, the leading broad cause contributing to the gap was cancer and other neoplasms (a gap of 60 and 71 per 100,000, respectively) (Table D1.23.2).
In Remote and Very remote areas combined, cardiovascular disease accounted for the largest gap in death rates between First Nations people and non-Indigenous Australians (gap of 134 per 100,000). In non-remote areas, cancer and other neoplasms was the biggest contributor to the gap (gap of 39 per 100,000) (Table D1.23.30).
Differences in specific leading causes of death
After adjusting for differences in the age structure of the two populations in the 5 jurisdictions in 2019–2023, death rates were between 1.3 and 4.4 times as high for First Nations people as for non-Indigenous Australians across the 10 leading specific causes of death.
The highest gaps were for:
- diabetes (rate difference of 53 deaths per 100,000 population, based on age-standardised data)
- coronary heart disease (rate difference of 52 deaths per 100,000 population)
- chronic obstructive pulmonary diseases (rate difference of 44 deaths per 100,000 population)
- lung cancer (rate difference of 31 deaths per 100,000 population), and
- intentional self-harm (rate difference of 15 deaths per 100,000 population) (Table D1.23.33).
Changes over time
Based on age-standardised rates in the 5 jurisdictions with adequate Indigenous status identification, cancer and other neoplasms was the broad leading cause of death among First Nations people for the majority of the period from 2016 to 2023, the exception being for 2016, where cardiovascular disease was the leading cause of death. For non-Indigenous Australians, cancer and other neoplasms was the leading cause of death in all years for which data are available.
Between 2016 and 2021, the age-standardised death rate for cancer and other neoplasms increased by 15% for First Nations people while the rate decreased by 7% for non-Indigenous Australians. This resulted in the absolute gap (rate difference) between First Nations people and non-Indigenous Australians widening. The relative difference (rate ratio) in the rates of death due to cancer and other neoplasms was higher for First Nations people across all years for which data are available and peaked at 1.5 times the rate of non-Indigenous Australians in 2021 (Table D1.23.20, Figure 1.23.8).
There was no significant change in the age-standardised rates for deaths due to cardiovascular disease between 2016 and 2021 for First Nations people. There was also no significant change in the absolute gap between First Nations people and non-Indigenous Australians (assessed using linear regression). Over this period, the relative difference in rates fluctuated between 1.2 times as high for First Nations people in 2017 and 1.6 times as high in 2020 (Table D1.23.18, Figure 1.23.8).
The rate of deaths due to injury and poisoning among First Nations people did not change significantly between 2016 and 2021, and nor did the gap (rate difference). The relative difference in the rates was higher for First Nations people across the time period, varying between 1.6 and 1.9 times the rate of non-Indigenous Australians with no trend evident (Table D1.23.19, Figure 1.23.8).
Figure 1.23.8: Age-standardised death rates for the top 3 broad leading causes of death, by Indigenous status, NSW, Qld, WA, SA and NT, 2016 to 2023
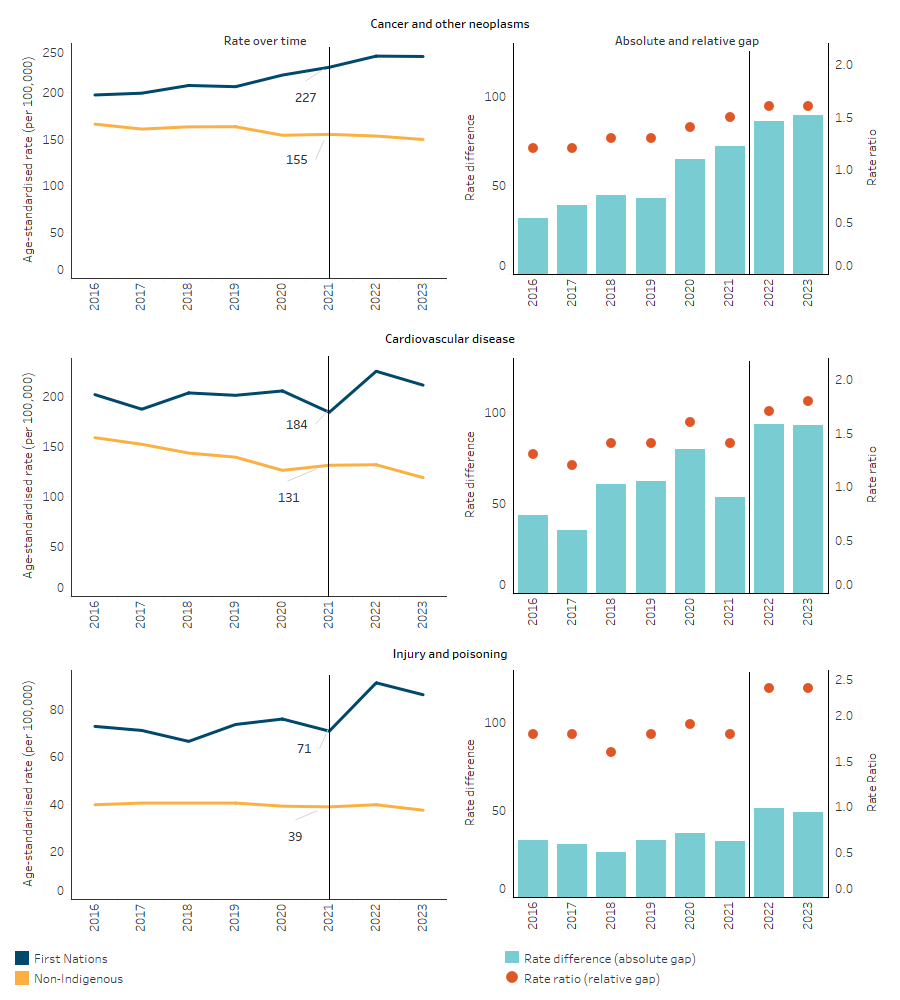
Note: The vertical line indicates a break in series in 2022 due to changes in Indigenous identification method in New South Wales. Caution should be used when interpreting changes in death rates over time (see Box 1.23.2 for more information).
Sources: Tables D1.23.18, D1.23.19, D1.23.20. AIHW National Mortality Database.
Research and evaluation findings
The research literature provides a number of insights into the determinants of mortality among First Nations people. It highlights improvements that can be made to the health system, and the social determinants, to reduce disease-specific death rates.
Findings show that improved management of chronic diseases can prevent the development of life-threatening complications (Hyun et al. 2023). For example, a study of incidence and survival of acute myocardial infarction found that improvement in survival for First Nations people in the Northern Territory was associated with pre-hospital management of conditions. Specialised coronary care services within hospitals placed a greater emphasis on post-hospital management, which led to improved survival rates of patients (You et al. 2009). A tertiary hospital study in Queensland found that after receiving a culturally informed multidisciplinary model of care, First Nations patients with acute coronary syndrome had experienced fewer subsequent events (death, acute myocardial infarction, unplanned revascularisation, or cardiac readmission) by the endpoint of 90 days after initial hospital admission, compared with patients prior to implementation of the model of care (20% and 34% respectively). This was largely driven by a reduction in unplanned cardiac readmissions (Harrop et al. 2024) (see measure 3.05 Chronic disease management).
A systematic review found that multimorbidity was associated with increased mortality (Nunes et al. 2016) and prevalence of multimorbidity is higher among First Nations people than non-Indigenous Australians:
- A study using the Household, Income and Labour Dynamics in Australia (HILDA) Survey, found First Nations adults reported a higher prevalence of multimorbidity (24.2%) compared with non-Indigenous Australians (20.7%), and the prevalence of physical–mental multimorbidity was almost twice as high (16.1% compared to 8.1%). Multimorbidity was associated with increased health service use, reduced employment productivity, and poorer self-reported health status (Carman et al. 2022).
- In New South Wales, analysis of linked hospital and death data showed that after adjusting for age, sex, and socioeconomic status, the prevalence of multimorbidity among First Nations people was 2.6 times that of non-Indigenous Australians. This difference accounted for a large proportion of the difference in death rates between the 2 groups of patients (Randall et al. 2018).
- In Western Australia, among adults aged 25–59 hospitalised with atherothrombotic disease, 79% of First Nations patients had multimorbidity compared to 39% of non-Indigenous patients, highlighting the complexity of care needs (Hussain et al. 2018).
A study in the Northern Territory found that the largest decreases for the First Nations population in avoidable mortality between 1985 and 2004 were for conditions amenable to medical care such as asthma, pneumonia and breast cancer. However, there was only a marginal change for potentially preventable conditions, such as lung cancer, chronic liver disease and cirrhosis, and motor vehicle accidents (Li et al. 2009). A more recent Northern Territory study of improvements in First Nations life expectancy between 1999 and 2018 found that a large proportion of the improvement during this period was attributable to fewer years of life being lost due to cancer, injuries and chronic disease (Zhao et al. 2022). Another study in the Northern Territory found that socioeconomic disadvantage was the leading determinant for gaps in life expectancy between First Nations people and non-Indigenous Australians, accounting for one-third to one-half of the gap (Zhao et al. 2013).
Socioeconomic disadvantage is multi-faceted and is influenced by factors like access to education, employment and housing (see measures 2.01 Housing, 2.04 Literacy and numeracy, 2.06 Educational participation and attainment of adults, 2.07 Employment, 2.09 Socioeconomic indexes).
The Deadly Choices program is an education initiative which aims to increase the number of First Nations people accessing their local Community Controlled Health Services to undertake comprehensive health assessments. An evaluation of the program found that it improved knowledge, attitudes, self-efficacy, and behaviours related to chronic disease prevention and healthy living among participants, and that the program facilitated the uptake of Aboriginal and Torres Strait Islander Health Checks for participants (Malseed 2013).
Research on selected leading causes
Cancer death rates are higher for First Nations people than for non-Indigenous Australians, even after accounting for more advanced stages of cancer and competing causes of death (Condon et al. 2014; Tervonen et al. 2017). First Nations people diagnosed with cancer have a higher probability of dying from cancer within the first 5 years of diagnosis across a range of cancer types (Dasgupta et al. 2022) (see measure 1.08 Cancer).
Some progress has been made on death rates from cardiac conditions since the introduction of the Better Cardiac Care project, which aims to reduce mortality and morbidity from cardiac conditions among First Nations people by increasing access to services, better managing risk factors and treatment, and improving coordination of care. Improvements include:
- The level of access for cardiac-related health services has improved.
- There have been increases in the proportion of First Nations people who received: Medicare-funded health assessments; and the recommended intervention following hospitalisation for a severe heart attack.
- The death rate from cardiac conditions for First Nations people declined by 35% between 2006 and 2021 (AIHW 2024a; Timothy et al. 2020).
The Lighthouse Hospital Project aims to improve the patient journey for First Nations people with heart disease and reduce the impact and incidence of discharge against medical advice. Since the launch of the project in 2012, better in-hospital and post-hospital cardiac care has been provided through improved hospital systems and fostering cultural safety in acute care (for more information see measures 1.05 Cardiovascular disease, 3.08 Cultural competency and 3.09 Self-discharge from hospital).
Rheumatic Heart Disease (RHD) Control Programs have led to better management and prevention of RHD and acute rheumatic fever, reducing the overall disease burden. These programs significantly improved the delivery of secondary prophylaxis, protecting against the progression from mild RHD to severe RHD and death (Stacey et al. 2023).
For First Nations children in Australia, it has been well documented that injuries resulting from external causes are major causes of death. Research has found that Indigenous children across different communities around the world experience a significantly higher burden of illness and death from unintentional injuries. Most of these injuries, such as burns, poisoning and transport injuries, are highly preventable. The risks of these injuries are increased by high exposure to hazards in the living environment, socioeconomic disadvantage, lack of means of protection, and living in remote areas (Lee et al. 2018; Möller et al. 2016a; Möller et al. 2017; Möller et al. 2016b; Möller et al. 2015; Möller et al. 2019) (see measure 1.20 Infant and child mortality).
A key contributor to injury deaths for First Nations young people and adults under 45 years of age is suicide. A literature review on protective and risk factors for suicide among First Nations people summarised findings from 214 reports, research articles and systematic reviews, and concluded 17 critical protective and risk factors associated with an individual’s intention to commit suicide. Factors that affect both First Nations and non-Indigenous Australians include: age, sex, location of residence, housing, employment, substance use and incarceration. The review also highlights the unique factors that may be particularly important for First Nations people: cultural continuity, spirit, language and cultural understandings of wellbeing (AIHW 2022c) (see measure 1.18 Social and emotional wellbeing).
Based on consultation and research, a report by the AIHW sought to further understand the sources of data that can inform progress to reduce First Nations suicide rates, supporting the need for accurate and timely data about suicide deaths and non-lethal intentional self-harm (AIHW 2022b). The report:
- provides a detailed description of the key players and stages in the identification and recording of suicide and non-lethal intentional self-harm incidents among First Nations people
- brings together information on suicide-relevant data collections with national, state or territory coverage: including their purpose; their Indigenous status derivation; and their limitations
- identifies the sources of error in the classification of Indigenous status; of suicide as a cause of death; and of suicidal intent in cases of self-harm
- describes the work already underway to enhance the quality, consistency and timeliness of data collection and reporting, and work that needs to be undertaken (AIHW 2022b).
High rates of respiratory diseases, such as asthma, chronic obstructive pulmonary disease (COPD), pneumonia and invasive pneumococcal disease are a major cause of death for First Nations people (see measure 1.04 Respiratory disease). The social determinants of respiratory health significantly impact outcomes from birth and throughout life. Adverse exposures before conception, during pregnancy, and in early childhood have lasting effects on lung function, contributing to diseases like COPD, bronchiectasis, and early mortality. These issues disproportionately affect populations of lower socioeconomic status, including First Nations people in Australia. Factors such as passive tobacco exposure, air pollution, poor housing conditions, and limited access to affordable medications contribute to lung health disparities. Climate change further exacerbates respiratory health issues for disadvantaged children. Early-life lung function impairment is linked to intergenerational effects, with parental lung function influencing child respiratory health (Bush et al. 2024). A study in the Northern Territory found that First Nations patients referred to respiratory specialist outreach teams in remote and rural communities have a significantly higher rate of smoking and COPD compared with non-Indigenous patients referred to this service. Bronchiectasis is also more common among First Nations patients (Kruavit et al. 2017). The study suggested there is a need to focus resources on reducing the rate of smoking in these areas, and further improve the quality of health care with a focus on primary health care. In addition to education provided by the respiratory outreach team, Aboriginal health workers could provide information on tobacco and ‘quit support’ to the community.
Evaluation of the Tackling Indigenous Smoking (TIS) Program has highlighted a decline in smoking rates among First Nations people. The TIS Program is a key part of the effort to increase life expectancy over time (DoHAC 2024). An analysis of Quitline usage in TIS and non-TIS areas found that usage of Quitline was higher in areas which had TIS teams, suggesting that programs like TIS are an important way to encourage the use of smoking cessation services (Colonna et al. 2024). Living in a TIS area is also associated with a lower prevalence of smoking in the home, and a lower prevalence of high smoking intensity (Cohen et al. 2021).
Diabetes does not often lead directly to death, rather it contributes to deaths from other causes (for example, cardiovascular (circulatory) disease or kidney disease). This is referred to as associated cause of deaths (AIHW 2017). In 2022, there were approximately 1,100 deaths among First Nations people where diabetes was listed as an underlying or associated cause. This represents a significant burden, especially considering that the age-standardised diabetes death rate among First Nations people was 4.6 times higher than that of non-Indigenous Australians (AIHW 2024b). Diabetes has consistently been ranked among the top causes of death for First Nations people in recent years (ABS 2025a) (see measure 1.09 Diabetes).
The rate of First Nations people with diabetes is higher in remote areas than in urban areas and First Nations people are also at greater risk of complications, for example kidney failure (Minges et al. 2011; Shaw and Tanamas 2012). The underlying causes are multifaceted. Firstly, diabetes is a chronic condition that requires complex medical care and often involves multiple health care providers. An observational study of remote First Nations patients with diabetes in the Northern Territory has found patients who had adequate levels of access to primary health care had better diabetes management and a lower level of hospitalisations, compared with those with fewer primary health care visits (Zhao et al. 2015). With less health service options available, self-management of diabetes is more necessary for remote residents than others who live in urban areas (Sav et al. 2015). However, living remotely poses barriers to accessing diabetes education resources. Moreover, people living in rural and remote areas are less likely to have completed Year 12 or equivalent education, have fewer employment opportunities, and have lower incomes while bearing higher costs for goods and services than urban residents (AIHW 2024c).
Implications
These findings emphasise the need for significant and concerted efforts to continue improving First Nations people’s health outcomes, both directly through health interventions and services, and by addressing the cultural and social determinants of health. Addressing the upstream modifiable risk factors and social determinants of health are crucial but need to be understood in the context of the ongoing impacts of colonisation, including intergenerational trauma, systemic and interpersonal racism, and the disruption of cultural, social, and economic systems. The health system can contribute to sustained improvements by partnering with First Nations people to better identify their needs, enhance their access to services, and improve attendance.
Access to effective, culturally safe primary health care, and also to medical specialists, is vital for meeting the health needs of First Nations people, particularly for detecting and managing health conditions so as to prevent hospitalisation and death. Improved management of chronic diseases can prevent the development of life-threatening complications but cannot cure these diseases. Chronic diseases can be prevented through modifying health risk behaviours, such as increased physical exercise (see measure 2.18 Physical activity), reduced consumption of alcohol (see measure 2.16 Risky alcohol consumption), smoking cessation (see measure 2.15 Tobacco use), and better nutrition (see measure 2.19 Dietary behaviours).
The Australian Government funds a number of evidence-based preventive health programs. It is expanding the Deadly Choices program to increase the number of First Nations people accessing health assessments (Butler 2024). It continues to fund the Tackling Indigenous Smoking (TIS) Program, which is delivered in strong partnership with First Nations people (DoHAC 2024). The Australian Government also funds RHD control programs in Queensland, Western Australia, South Australia and the Northern Territory (AIHW 2025).
Partnerships with First Nations organisations that emphasise shared decision-making are also important to addressing preventable chronic diseases such as RHD. The Australian Government has formed a partnership with the National Aboriginal Community Controlled Health Organisation (NACCHO) to deliver the Rheumatic Fever Strategy, to establish a national coordinated approach, support community-led and place-based approaches and enhance prevention and management efforts in high-burden areas (Federal Financial Relations 2024; NACCHO 2025).
In addition to Deadly Choices, Aboriginal Community Controlled Health Organisations (ACCHOs) deliver a range of impactful programs tailored to community needs. NACCHO coordinates the Improving First Nations Cancer Outcomes Program, supporting ACCHOs to deliver culturally safe cancer prevention, screening, diagnosis, and treatment services. This also includes initiatives such as the National Lung Cancer Screening Program, bowel cancer screening, and cervical screening, which are tailored to local contexts and supported by community-led health promotion campaigns) (NACCHO 2023a, 2023b). The Culture Care Connect program, coordinated by NACCHO, is a national suicide prevention and aftercare initiative that integrates cultural safety, trauma-aware care, and community empowerment. Operating across more than 30 ACCHOs, it supports localised suicide prevention planning and aftercare services, with a strong emphasis on cultural connection and healing (NACCHO 2022).
High levels of intentional self-harm highlight the need for cross-sectoral approaches to health, self-esteem and social and emotional wellbeing (see measure 1.18 Social and emotional wellbeing).
The National Aboriginal and Torres Strait Islander Suicide Prevention Strategy (2025–2035) aims to achieve a significant and sustained reduction in suicide and self-harm of First Nations people towards zero through First Nations community leadership and governance, with key priorities on self-determination, support for communities to thrive and be informed, with culturally safe care and a responsive workforce (Department of Health and Aged Care and Gayaa Dhuwi (Proud Spirit) Australia 2024).
The National Agreement on Closing the Gap was developed in partnership between all Australian governments and the Coalition of Aboriginal and Torres Strait Islander Peak Organisations. Each party to the National Agreement has developed their own Implementation Plan and will report annually on their actions to achieve the outcomes of the Agreement.
The National Aboriginal and Torres Strait Islander Health Plan 2021–2031 (the Health Plan), released in December 2021, is the overarching policy framework to drive progress against the Closing the Gap health targets and priority reforms. The Australian Government is responsible for implementing the Health Plan at a national level. States, territories and other implementation partners, while also responsible for its implementation, can take flexible approaches to implementing Health Plan priorities. Their approaches will depend on local needs and priorities, led by First Nations people and communities.
Implementation of the Health Plan aims to drive structural reform towards models of care that are prevention and early intervention focused, with greater integration of care systems and pathways across primary, secondary and tertiary care. It also emphasises the need for mainstream services to address racism and provide culturally safe and responsive care, and be accountable to First Nations people and communities. The Health Plan also calls on acute care settings to be accessible, culturally safe and responsive.
References
-
ABS (Australian Bureau of Statistics) (2023a) Causes of death, Australia methodology (2022), ABS website, accessed 27 January 2026.
-
ABS (2023b) Understanding change in counts of Aboriginal and Torres Strait Islander Australians: Census (2021), ABS website, accessed 27 January 2026.
-
ABS (2024) Causes of death, Australia methodology (2023), ABS website, accessed 27 January 2026.
-
ABS (2025a) Causes of death, Australia (2024), ABS website, accessed 6 February 2026.
-
ABS (2025b) Excess mortality by selected causes of death, 2020–23, ABS website, accessed 27 January 2026.
-
AIHW (Australian Institute of Health and Welfare) (2017) Deaths among people with diabetes in Australia, 2009–2014, AIHW, Australian Government.
-
AIHW (2022a) Impact and causes of illness and death in Aboriginal and Torres Strait Islander people 2018, Australian Burden of Disease Study, AIHW, Australian Government, doi:10.25816/xd60-4366.
-
AIHW (2022b) Investigating enhancements of Indigenous data in suicide-relevant data sets, AIHW, Australian Government, doi:10.25816/mhh2-5r51.
-
AIHW (2022c) Protective and risk factors for suicide among Indigenous Australians, AIHW, Australian Government, doi:10.25816/vnrs-v647.
-
AIHW (2024a) Better Cardiac Care measures for Aboriginal and Torres Strait Islander people: eighth national report 2023, AIHW, Australian Government.
-
AIHW (2024b) Diabetes: Australian facts, AIHW website, accessed 4 June 2025.
-
AIHW (2024c) Rural and remote health, AIHW website, accessed 4 June 2025.
-
AIHW (2025) Acute rheumatic fever and rheumatic heart disease in Australia, AIHW, Australian Government, accessed June 2025.
-
Becker R, Silvi J, Ma Fat D, L’Hours A and Laurenti R (2006) 'A method for deriving leading causes of death', Bulletin of the World Health Organization 84(4):297–304, doi:10.2471/blt.05.028670.
-
Bush A, Byrnes CA, Chan KC, Chang AB, Ferreira JC, Holden KA, Lovinsky-Desir S, Redding G, Singh V, Sinha IP and Zar HJ (2024) 'Social determinants of respiratory health from birth: still of concern in the 21st century?', European Respiratory Review, 33(172):230222, doi:10.1183/16000617.0222-2023.
-
Butler M (26 September 2024) Government backs “Deadly Choices” preventative health program [media release], Office of the Hon Mark Butler, Minister for Health and Ageing, Minister for Disability and the National Disability Insurance Scheme, Department of Health and Aged Care, Australian Government.
-
Carman W, Ishida M, Trounson JS, Mercer SW, Anindya K, Sum G, Armstrong G, Oldenburg B, McPake B and Lee JT (2022) 'Epidemiology of physical-mental multimorbidity and its impact among Aboriginal and Torres Strait Islander in Australia: a cross-sectional analysis of a nationally representative sample', BMJ Open, 12(10):e05999, doi:10.1136/bmjopen-2021-054999.
-
Cohen R, Maddox R, Sedgwick M, Thurber K, Brinckley M-M, Barrett E and Lovett R (2021) 'Tobacco related attitudes and behaviours in relation to exposure to the Tackling Indigenous Smoking Program: evidence from the Mayi Kuwayu Study', International Journal of Environmental Research and Public Health, 18(20):10962, doi:10.3390/ijerph182010962.
-
Colonna E, Heris C, Barrett EM, Wells S and Maddox R (2024) 'Aboriginal and Torres Strait Islander peoples' Quitline use and the Tackling Indigenous Smoking program', Public Health Research & Practice, 34(3):e34012403, doi:10.17061/phrp34012403.
-
Condon J, Zhang X, Baade P, Griffiths K, Cunningham J, Roder D, Coory M, Jelfs P and Threlfall T (2014) 'Cancer survival for Aboriginal and Torres Strait Islander Australians: a national study of survival rates and excess mortality', Population Health Metrics, 12:1, doi:10.1186/1478-7954-12-1.
-
Dasgupta P, Garvey G and Baade PD (2022) 'Quantifying the number of deaths among Aboriginal and Torres Strait Islander cancer patients that could be avoided by removing survival inequalities, Australia 2005–2016', PloS One, 17(8):e0273244, doi:10.1371/journal.pone.0273244.
-
Department of Health and Aged Care and Gayaa Dhuwi (Proud Spirit) Australia (2024) National Aboriginal and Torres Strait Islander Suicide Prevention Strategy 2025–2035, DoHAC, Australian Government.
-
DoHAC (Department of Health and Aged Care) (2024) Tackling Indigenous Smoking, DoHAC website, accessed 4 June 2025.
-
Federal Financial Relations (2024) Rheumatic Fever Strategy: federation funding agreement – health, Federal Financial Relations, Australian Government.
-
Harrop DL, Bryce V, Kitchener T, Grugan S, Renouf S, Mitchell S, Hasking G, Pauza D, Richards G, Ng ACT and Wang WYS (2024) 'Effects of a culturally informed model of care for Aboriginal and Torres Strait Islander patients with acute coronary syndrome in a tertiary hospital in Australia: a pre-post, quasi-experimental, interventional study', The Lancet Global Health, 12(4):623–630, doi:10.1016/S2214-109X(23)00601-0.
-
Hussain M, Katzenellenbogen J, Sanfilippo F, Murray K and Thompson S (2018) 'Complexity in disease management: a linked data analysis of multimorbidity in Aboriginal and non-Aboriginal patients hospitalised with atherothrombotic disease in Western Australia', PloS One, 3(8):e0201496, doi:10.1371/journal.pone.0201496.
-
Hyun M, Lee J and Ko S (2023) 'Chronic disease management program applied to type 2 diabetes patients and prevention of diabetic complications: a retrospective cohort study using nationwide data', BMC Public Health, 23:928, doi:10.1186/s12889-023-15763-z.
-
Kruavit A, Fox M, Pearson R and Heraganahally S (2017) 'Chronic respiratory disease in the regional and remote population of the Northern Territory Top End: a perspective from the specialist respiratory outreach service', Australian Journal of Rural Health, 25(5):275–284, doi:10.1111/ajr.12349.
-
Lee C, Hanly M, Larter N, Zwi K, Woolfenden S and Jorm L (2018) 'Demographic and clinical characteristics of hospitalised unintentional poisoning in Aboriginal and non-Aboriginal preschool children in New South Wales, Australia: a population data linkage study', BMJ Open, 9:e022633, doi:10.1136/bmjopen-2018-022633.
-
Li SQ, Gray N, Guthridge S, Pircher S, Wang Z and Zhao Y (2009) 'Avoidable mortality trends in Aboriginal and non‐Aboriginal populations in the Northern Territory, 1985‐2004', Australian and New Zealand Journal of Public Health, 33(6):544–550, doi:10.1111/j.1753-6405.2009.00451.x.
-
Malseed C (2013) Deadly Choices health promotion initiative evaluation report January 1 – December 31, 2013, The Lowitja Institute, the Institute for Urban Indigenous Health, The University of Queensland.
-
Minges KE, Zimmet P, Magliano DJ, Dunstan DW, Brown A and Shaw JE (2011) 'Diabetes prevalence and determinants in Indigenous Australian populations: a systematic review', Diabetes Research and Clinical Practice, 93(2):139–149, doi:10.1016/j.diabres.2011.06.012.
-
Möller H, Falster K, Ivers R, Falster M, Randall D, Clapham K and L J (2016a) 'Inequalities in hospitalized unintentional injury between Aboriginal and non-Aboriginal children in New South Wales, Australia', American Journal of Public Health, 106(5):899–905, doi:10.2105/AJPH.2015.303022.
-
Möller H, Falster K, Ivers R, Falster MO, Clapham K and L J (2017) 'Closing the Aboriginal child injury gap: targets for injury prevention', Australian and New Zealand Journal of Public Health, 41(1):8–14, doi:10.1111/1753-6405.12591.
-
Möller H, Falster K, Ivers R, Falster M, Randall D, Clapham K and Jorm L (2016b) 'Inequalities in unintentional injury hospitalisation between Aboriginal and non-Aboriginal children in New South Wales, Australia', American Journal of Public Health, doi:10.2105/ajph.2015.303022.
-
Möller H, Falster K, Ivers R and Jorm L (2015) 'Inequalities in unintentional injuries between Indigenous and non-Indigenous children: a systematic review', Injury Prevention, 21:e144–e152, doi:10.1136/injuryprev-2013-041133.
-
Möller H, Ivers R, Clapham K and Jorm L (2019) 'Are we closing the Aboriginal child injury gap? A cohort study', Australian and New Zealand Journal of Public Health, 43(1):15–17, doi:10.1111/1753-6405.12866.
-
NACCHO (National Aboriginal Community Controlled Health Organisation) (2022) Culture care connect, NACCHO website, accessed September 2025.
-
NACCHO (2023a) Cancer program – improving First Nations cancer outcomes, NACCHO website, accessed September 2025.
-
NACCHO (2023b) National lung cancer screening program, NACCHO website, accessed September 2025.
-
NACCHO (2025) Acute rheumatic fever and rheumatic heart disease, accessed March 2025.
-
Nunes B, Flores T, Mielke G, Thumé E and Facchini L (2016) 'Multimorbidity and mortality in older adults: a systematic review and meta-analysis', Archives of Gerontology and Geriatrics, 67:130–138, doi:10.1016/j.archger.2016.07.008.
-
Productivity Commission (2021) Closing the Gap annual data compilation report July 2021, Annual Data Compilation Report Series, Productivity Commission, Australian Government, accessed 28 September 2025.
-
Randall D, Lujic S, Havard A, Eades SJ and Jorm L (2018) 'Multimorbidity among Aboriginal people in New South Wales contributes significantly to their higher mortality', Medical Journal of Australia, 209(1):19–23, doi:10.5694/mja17.00878.
-
Sav A, King MA, Kelly F, McMillan SS, Kendall E, Whitty JA and Wheeler AJ (2015) 'Self-management of chronic conditions in a rural and remote context', Australian Journal of Primary Health, 21(1):90–95, doi:10.1071/PY13084.
-
Shaw J and Tanamas S (2012) Diabetes: the silent pandemic and its impact on Australia, Baker IDI Heart and Diabetes Institute.
-
Stacey I, Ralph A, de Dassel J, Nedkoff L, Wade V, Francia C, Wyber R, Murray K, Hung J and Katzenellenbogen J (2023) 'The evidence that rheumatic heart disease control programs in Australia are making an impact', Australian and New Zealand Journal of Public Health, 47(4):100071, doi:10.1016/j.anzjph.2023.100071.
-
Tervonen HE, Walton R, You H, Baker D, Roder D, Currow D and Aranda S (2017) 'After accounting for competing causes of death and more advanced stage, do Aboriginal and Torres Strait Islander peoples with cancer still have worse survival? A population-based cohort study in New South Wales', BMC Cancer, 17:398, doi:10.1186/s12885-017-3374-6.
-
Timothy A, Wong D, Anderson K and Agostino J (2020) Cardiovascular disease risk communication with Aboriginal and Torres Strait Islander Peoples: toolkit for health professionals, Department of Health, Australian Government.
-
You J, Condon JR, Zhao Y and Guthridge S (2009) 'Incidence and survival after acute myocardial infarction in Indigenous and non-Indigenous people in the Northern Territory, 1992–2004', Medical Journal of Australia, 190(6):298–302, doi:10.5694/j.1326-5377.2009.tb02416.x.
-
Zhao Y, Connors C, Lee AH and Liang W (2015) 'Relationship between primary care visits and hospital admissions in remote Indigenous patients with diabetes: a multivariate spline regression model', Diabetes Research and Clinical Practice, 108(1):106–112, doi:10.1016/j.diabres.2015.01.013.
-
Zhao Y, Li S, Wilson T and Burgess P (2022) 'Improved life expectancy for Indigenous and non‐Indigenous people in the Northern Territory, 1999–2018: overall and by underlying cause of death', Medical Journal of Australia, 217:30–35, doi:10.5694/mja2.51553.
-
Zhao Y, Wright J, Begg S and Guthridge S (2013) 'Decomposing Indigenous life expectancy gap by risk factors: a life table analysis', Population Health Metrics, 11:1, doi:10.1186/1478-7954-11-1.

