Key messages
Why is it important?
Kidney disease is a major health issue for Aboriginal and Torres Strait Islander (First Nations) people who experience disproportionately high levels of kidney disease across all geographic areas, but particularly in remote areas.
Around 1 in 5 First Nations people are likely to develop kidney disease. Chronic Kidney Disease (CKD) often co-occurs with other chronic conditions such as diabetes and high blood pressure, which are also more common in First Nations people. Kidney disease and its treatment significantly impact individuals’ lives including social, emotional, and cultural wellbeing, and can result in financial strain and reduced quality of life. Despite the disease burden, First Nations people are less likely to receive a kidney transplant, which offers better long-term outcomes than dialysis.
Data findings
- Based on the 2022–24 National Aboriginal and Torres Strait Islander Health Measures Survey (NATSIHMS), nearly 1 in 5 (18%) First Nations adults had blood/urine test results showing signs of CKD. Of those, only 13% had reported having the condition and 87% did not know they had it.
- In the 5-year period 2019–2023 in 5 jurisdictions combined, there were 396 deaths of First Nations people due to kidney disease (including acute and chronic kidney disease), corresponding to a rate of 9.2 deaths per 100,000 population.
- From 2016 to 2021, the age-standardised death rate due to kidney diseases (including acute and chronic conditions) as the underlying cause of death did not change significantly, fluctuating between 10 deaths per 100,000 population (in 2017) and 25 deaths per 100,000 (in 2020).
- 1,055 First Nations people started kidney replacement therapy (either a kidney transplant or dialysis) in 2020–2022, corresponding to an incidence rate of 36 new cases of kidney failure with replacement therapy per 100,000 population.
- In 2020–2022, the incidence of kidney failure with replacement therapy was 5.3 times as high for First Nations people as for non-Indigenous Australians nationally, and 17 times as high in Remote and very remote areas.
- As at 31 December 2022, there were 2,625 First Nations people receiving kidney replacement therapy (either dialysis, or a kidney transplant). Among First Nations patients, 84% (2,204 patients) were on dialysis and 16% (421 patients) had a functioning kidney transplant.
- First Nations people were less likely than non-Indigenous Australians to receive a kidney transplant. Among non-Indigenous Australians receiving kidney replacement therapy as at 31 December 2022, 48% (12,113 of 25,120 patients) had a functioning kidney transplant, compared with 16% (421 of 2,625 patients) of First Nations people.
Research and evaluation findings
-
First Nations patients are less likely to be wait-listed for transplantation than non-Indigenous Australians. Barriers include systemic factors (e.g. referral practices for transplant evaluation, service availability), cultural bias and comorbidities.
-
Reducing the CKD burden requires life-course interventions starting before birth, addressing social determinants, and early detection and better disease management.
-
Well run screening and treatment programs for CKD have shown dramatic reductions in mortality and are cost-effective.
-
Mobile dialysis units can provide short-term care that supports cultural connection for First Nations dialysis patients, but do not address long-term relocation needs. Fixed dialysis infrastructure, like the community-controlled clinics run by Purple House, remains essential to enabling First Nations people to stay on Country and receive ongoing care.
Implications
Despite First Nations people having an age-adjusted incidence rate of kidney failure with replacement therapy 5.3 times higher than non-Indigenous Australians, barriers to appropriate treatment and transplantation remain, including limited access to services, financial and travel burdens, and a biomedical model of care that often lacks cultural appropriateness. The absence of First Nations specific CKD prevention, screening and care policies further compounds inequities.
While initiatives such as the Better Renal Services for First Nations Peoples and the National Strategic Action Plan for Kidney Disease have begun to address these gaps, sustained investment in community-led, culturally safe models of care remains essential. Programs like Purple House and the First Nations Health Worker Traineeship demonstrate the value of embedding care within communities, promoting self-determination, and strengthening the First Nations health workforce. However, broader systemic reforms are needed to ensure equitable access to kidney health services across the care continuum.
Why is it important?
Kidneys are crucial to overall health, playing a vital role in cleaning the blood, removing waste and extra fluid from the body, managing Vitamin D production which is crucial for maintaining strong bones and producing red blood cells that carry oxygen around your body, and regulating blood pressure. Aboriginal and Torres Strait Islander (First Nations) people experience disproportionate levels of kidney disease, regardless of whether they live in urban, regional or rural areas (Kidney Health Australia 2025). The incidence of kidney failure requiring dialysis or transplant is much higher among First Nations people than non-Indigenous Australians, and the risk is greatest for those living in remote areas. Kidney Health Australia’s First Nations Client Resources highlights that kidney disease is very common in First Nations people with 1 in 5 likely to develop kidney disease. Reduced kidney function often happens together with diabetes and high blood pressure, which is also common in First Nations people (see measures 1.09 Diabetes and 1.07 High blood pressure).
If the kidneys cease functioning adequately (known as kidney failure or end-stage kidney disease), waste products and excess water build up rapidly in the body, requiring dialysis or a kidney transplant to survive. Despite facing higher rates of kidney disease, First Nations people are significantly less likely to receive kidney transplants than non-Indigenous Australians. Kidney transplantation provides a substantial survival advantage over dialysis, particularly beyond the first-year post-transplant, with dialysis patients experiencing a significantly higher mortality risk. As a result of the disparities in transplantation, many First Nations patients require lifelong dialysis, which impacts their quality of life and social, emotional and cultural wellbeing, particularly due to dislocation from Country and community (Bateman et al. 2024; Khanal et al. 2018; National Kidney Foundation 2023).
Kidney disease can also contribute to, or be impacted by, chronic diseases including high blood pressure, cardiovascular (circulatory) disease, and diabetes (AIHW 2024a). Cardiovascular disease, diabetes and kidney disease share a number of common behavioural risk factors such as tobacco smoking, overweight and obesity, insufficient physical activity, and alcohol consumption. First Nations people have higher levels of risk factors associated with chronic diseases and are at a greater risk of developing chronic kidney disease (CKD), particularly those in lower socioeconomic areas, and remote areas. In many cases CKD is preventable, as several key risk factors are potentially modifiable (AIHW 2024a).
Modifiable risk factors for kidney disease, such as diet and physical activity, are not always easily addressed. Intergenerational trauma, colonisation and systemic disadvantage have disrupted traditional healthy practices and created barriers. This includes food insecurity, socioeconomic disadvantage and stigma that make behavioural change more complex than individual choice alone (Brimblecombe et al. 2014; Brimblecombe and O'Dea 2009; Hunt et al. 2008; Lee and Ride 2018) (see measures 2.18 Physical activity and 2.19 Dietary behaviour). Research has shown that socioeconomic disadvantage leads to worse kidney function (Ritte et al. 2020). The relatively high burden of CKD among First Nations people reflects this social gradient in which those at the greatest disadvantage experience the highest incidence, prevalence, and impacts of disease (AIHW 2019, 2024c, 2025; Marmot 2006; Morton et al. 2016).
CARI (Caring for Australian and New Zealanders with Kidney Impairment) guidelines provide recommendations on clinical best practice for the management of CKD in Australia and New Zealand, including care based on the best available evidence, and including specific recommendations for First Nations people (Tunnicliffe et al. 2022). Current guidelines recommend that all First Nations people aged 18 and over should get an annual Kidney Health Check to identify CKD and it is included in the bulk billed Aboriginal and Torres Strait Islander Peoples Health Assessment. First Nations children under 18 years of age should be screened for potential risk factors for CKD and then have a Kidney Health Check if needed (AIHW 2024a; Tunnicliffe et al. 2022).
Burden of disease
Burden of disease analysis is a way of measuring the impact of both living with poor health (the non-fatal burden of disease) and dying prematurely (fatal burden). It is measured using ‘disability-adjusted life years’ (DALY), where 1 DALY represents 1 year of healthy life lost, either through premature death (‘years of life lost’ or YLL) or from living with an illness or injury (‘years lived with disability’ or YLD).
Among all Indigenous Australians in 2018, chronic kidney disease accounted for:
- 2.5% (6,067 DALY) of the total Indigenous disease burden (239,942 DALY)
- 3.9% (4,416 YLL) of the total Indigenous fatal burden (premature death) (113,445 YLL), and
- 1.3% (1,651 YLD) of the total Indigenous non-fatal burden (years lived in ill health or with disability) (126,496) (AIHW 2022).
In 2018, of the total burden attributable to chronic kidney disease (6,067 DALY) for Indigenous Australians, almost three-quarters (73% or 4,416 YLL) was fatal and just over one-quarter (27% or 1,651 YLD) was non-fatal.
After adjusting for differences in the age-structure between the two populations, the rate of burden due to chronic kidney disease for Indigenous Australians was 8 times the rate for non-Indigenous Australians (13 and 1.7 DALY per 1,000 people, respectively). Based on age-standardised rates, chronic kidney disease was the second leading cause of the gap between Indigenous and non-Indigenous females (6.5% of the gap), and was the sixth leading cause for males (4.0%).
These results exclude the indirect effects of chronic kidney disease. Chronic kidney disease is a risk factor for other diseases such as coronary heart disease, stroke, and dementia and the indirect burden is not accounted for using this approach.
Indirect effects of chronic kidney disease can be estimated in some cases by considering impaired kidney function as a risk factor for other diseases. In 2018, impaired kidney function was estimated to account for 5.0% of the total disease burden for Indigenous Australians, 8.4% of the fatal burden and 1.9% of the non-fatal burden (AIHW 2022).
Data findings
Kidney disease is considerably more likely to be recorded as an additional diagnosis than as the principal diagnosis in hospital separations. In 2021–22, across Australia, there were around 56,800 hospitalisations (excluding dialysis) where CKD was listed as the principal diagnosis and 328,000 hospitalisations where CKD was listed as an additional diagnosis. Similarly, kidney disease is much more likely to be recorded on death certificates as an associated cause of death rather than as the underlying cause (AIHW 2024a). There is also evidence that it may be under-reported as a cause of death, with a study using linked data from Western Australia and New South Wales showing that substantial proportions of people hospitalised with or receiving treatment for kidney failure do not have kidney failure recorded on their death certificate (AIHW 2014; Sypek et al. 2018). Looking only at the principal diagnosis or underlying cause of death therefore under-represents the true impact of CKD. Therefore, this measure also includes data about kidney disease as an additional diagnosis or an associated cause of death.
Death rates for kidney diseases
Deaths data in this measure are sourced from the National Mortality Database. The data are used to report the total number of deaths nationally, which includes Australian residents of all states and territories. However, when reporting death rates, data have been limited to 5 jurisdictions (New South Wales, Queensland, Western Australia, South Australia and the Northern Territory), in which the quality of Indigenous status identification in the deaths data is considered adequate. National death rates are not published due to concerns around the quality of Indigenous status identification in Victoria, Tasmania and the Australian Capital Territory. When reporting death rates by remoteness, data from all jurisdictions has been included.
Kidney disease can be listed as an underlying cause of death, or more commonly, as an associated cause (where another condition is listed on the death certificate as the underlying cause).
Nationally, over the 5-year period 2019–2023, there were 4,203 deaths among First Nations people where kidney diseases were listed as the underlying or associated cause of death, meaning that in this period kidney disease contributed to almost one-fifth (19%) of all First Nations deaths. Based on underlying cause of death, in the period 2019–2023, there were 425 deaths of First Nations people that were due to kidney disease (including acute and chronic kidney disease) (Table D1.23.24b).
The rate of deaths due to kidney disease among First Nations people in Remote and very remote areas was 3.2 times the rate in non-remote areas (Major cities, Inner and Outer regional areas) (Table D1.23.30).
In 2019–2023 in the 5 jurisdictions with adequate Indigenous status identification, there were 3,939 deaths among First Nations people where kidney diseases were listed as the underlying or associated cause of death – 20% of all First Nations deaths (Table D1.23.24a). Considering both underlying and associated causes of death, the rate of deaths related to kidney diseases was 2.9 times as high for First Nations people as for non-Indigenous Australians (Table D1.23.24a).
Based on underlying cause of death, in the period 2019–2023 in the 5 jurisdictions with adequate Indigenous status identification, there were 396 deaths of First Nations people that were due to kidney disease (including acute and chronic kidney disease), corresponding to a rate of 9.2 deaths per 100,000 population. Kidney diseases accounted for 2.0% of First Nations people deaths, of which 58% were attributable to First Nations females (Table D1.23.24a).
In 2019–2023 in the 5 jurisdictions with adequate Indigenous status identification, based on underlying cause of death, the rate of deaths due to kidney disease was higher for First Nations females than First Nations males (10.7 compared with 7.7 per 100,000, respectively) (Table D1.23.24a).
After adjusting for differences in the age structure between the two populations, based on underlying cause of death, deaths due to kidney diseases for First Nations people were 2.6 times the rate for non-Indigenous Australians (Table D1.10.4).
Hospitalisation for chronic kidney disease
Dialysis is an artificial way to remove waste and excess water from the blood and regulate safe levels of circulating agents in the body, a function usually performed by the kidneys. It is most often provided to treat chronic kidney failure but is sometimes needed in cases of acute kidney failure, where the kidneys have been temporarily damaged due to illness or injury. Most people undergoing dialysis attend three sessions per week (ANZDATA Registry 2021).
Between July 2021 and June 2023, there were 539,439 hospitalisations of First Nations people for care of CKD involving dialysis, corresponding to a rate of 269 hospitalisations per 1,000 population (crude rate). Dialysis was the leading cause of hospitalisation for First Nations people (42% of hospitalisations) (Table D1.02.5).
Excluding dialysis, there were 8,104 hospitalisations of First Nations people due to CKD – or 4.0 hospitalisations per 1,000 population (crude rate). Crude rates were twice as high for First Nations females (5.4 per 1,000) than for First Nations males (2.7 per 1,000) (Table D1.10.6).
By age group, between July 2021 and June 2023, the hospitalisation rate for CKD (excluding dialysis) among First Nations people was highest for those aged 55–64 (12 hospitalisations per 1,000 population). For non-Indigenous Australians, rates were highest for those aged 65 and over (5.0 per 1,000) (Table D1.10.6).
For First Nations people, across states and territories, the hospitalisation rate for CKD (excluding dialysis) was lowest in New South Wales and Tasmania (crude rates of 1.9 per 1,000), and highest in the Northern Territory (11.5 per 1,000). Across remoteness areas, the hospitalisation rate for CKD among First Nations people was lowest in Major cities (2.5 per 1,000), and increased with increasing remoteness, with the highest rate in Remote and very remote areas (11.3 per 1,000) (Table D1.10.7, Table D1.10.8).
After adjusting for differences in the age structure between the two populations:
- The rate of hospitalisation for CKD that involved dialysis was 9 times as high for First Nations people as for non-Indigenous Australians (age-standardised rates of 404 and 45 hospitalisations per 1,000 population, respectively).
- The rate of hospitalisation for CKD, excluding dialysis, was 3 times as high for First Nations people as for non-Indigenous Australians (age-standardised rates of 5.4 and 1.8 per 1,000 population, respectively) (Table D1.10.5).
When CKD, excluding dialysis, is considered as either the principal or an additional diagnosis, the age-standardised hospitalisation rate for First Nations people in 2022–23 was 4.7 times that for non-Indigenous Australians, with the difference being greater for females than for males (rate ratios of 6.3 and 3.4, respectively) (Table D1.10.21).
For additional statistics and information relating to the broader Australian context on kidney disease, please see Chronic Kidney Disease: Australian Facts.
Kidney failure with replacement therapy
Kidney failure (also known as end-stage kidney disease) is the most severe form of CKD. It occurs when the kidneys can no longer function adequately on their own. People living with kidney failure require either a kidney transplant or dialysis to maintain the functions normally performed by the kidneys. These treatments are collectively known as ‘kidney replacement therapy’. Note that not all people with kidney failure choose to undergo kidney replacement therapy. Instead, some opt to receive comprehensive conservative care, which focuses on patient care, quality of life and symptom control rather than on efforts to prolong life (AIHW 2023a).
An estimate of the incidence of kidney replacement therapy can be obtained from the Australian and New Zealand Dialysis and Transplant Registry (ANZDATA Registry). This registry includes information on people who have had kidney replacement therapy in the form of dialysis (peritoneal or haemodialysis) or a kidney transplant. It does not contain information on people with kidney failure who do not receive replacement therapy.
During the period 2020–2022, 1,055 First Nations people with kidney failure started kidney replacement therapy – an average of nearly one person a day. This corresponds to an incidence rate of 36 new cases of kidney failure with replacement therapy for every 100,000 First Nations people. The incidence of kidney failure with replacement therapy was higher for First Nations females than for First Nations males (39 per 100,000 compared with 33 per 100,000) (Table D1.10.11).
For both First Nations males and females, the incidence of kidney failure with replacement therapy generally increased with age and was highest for those aged 55–64 (Table D1.10.10, Figure 1.10.1).
The incidence of kidney failure with replacement therapy in 2020–2022 was 5.3 times as high for First Nations people as for non-Indigenous Australians (53 compared with 10 per 100,000 population, based on age-standardised rates). This difference was greater in Remote and very remote areas, where the incidence was 17 times as high for First Nations people as for non-Indigenous Australians (156 compared with 9 per 100,000 population) (Table D1.10.12).
Figure 1.10.1: Incidence (new cases) of kidney failure with replacement therapy, First Nations people, by sex and age group, 2020–2022
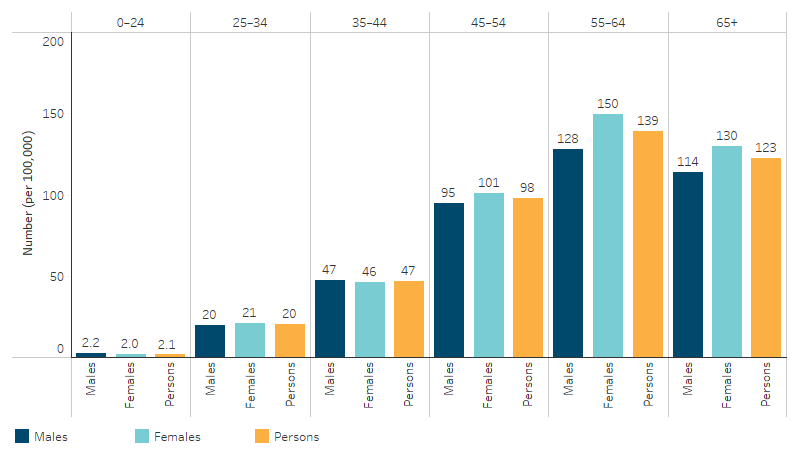
Source: Table D1.10.10. AIHW analysis of the Australia and New Zealand Dialysis and Transplant Registry.
Across states and territories, for the period 2020–2022, the incidence of kidney failure with replacement therapy among First Nations people ranged from 10 new cases per 100,000 population in New South Wales/the Australian Capital Territory combined and 12 new cases per 100,000 population in Victoria/Tasmania, to 135 per 100,000 population in the Northern Territory (Table D1.10.11, Table 1.10-1).
Table 1.10-1: Incidence (new cases) of kidney failure with replacement therapy, First Nations people, by sex and jurisdiction, 2020–2022
|
Jurisdiction |
Male number |
Male rate (per 100,000) |
Female number |
Female rate (per 100,000) |
Persons number |
Persons rate (per 100,000) |
|---|---|---|---|---|---|---|
|
NSW/ACT |
60 |
11.4 | 49 | 9.4 | 109 | 10.4 |
|
Vic/Tas |
18 | 10.6 | 21 | 12.5 | 39 | 11.6 |
|
Qld |
131 | 32.0 | 139 | 33.8 | 270 | 32.9 |
|
WA |
123 | 66.8 | 127 | 72.0 | 250 | 69.4 |
|
SA |
32 | 40.9 | 45 | 57.8 | 77 | 49.3 |
|
NT |
121 | 106.4 | 189 | 163.3 | 310 | 135.1 |
|
Australia |
485 |
32.7 |
570 |
38.7 |
1,055 |
35.7 |
Source: Table D1.10.11. AIHW analysis of the Australia and New Zealand Dialysis and Transplant Registry.
Of the 1,055 new cases of kidney failure among First Nations people who had started replacement therapy in 2020–2022, over one half (533 or 51%) lived in Remote and very remote areas of Australia, 321 (or 31%) lived in Inner and outer regional areas, and 186 (or 18%) lived in Major cities. Adjusting for differences in population size, the incidence of kidney failure with replacement therapy for First Nations people was 7.6 times as high in Remote and very remote areas as in Major cities (118 and 16 new cases per 100,000 population respectively) (Table D1.10.12, Figure 1.10.2).
Figure 1.10.2: Incidence (new cases) rates of kidney failure with replacement therapy, First Nations people, by remoteness, 2020–2022
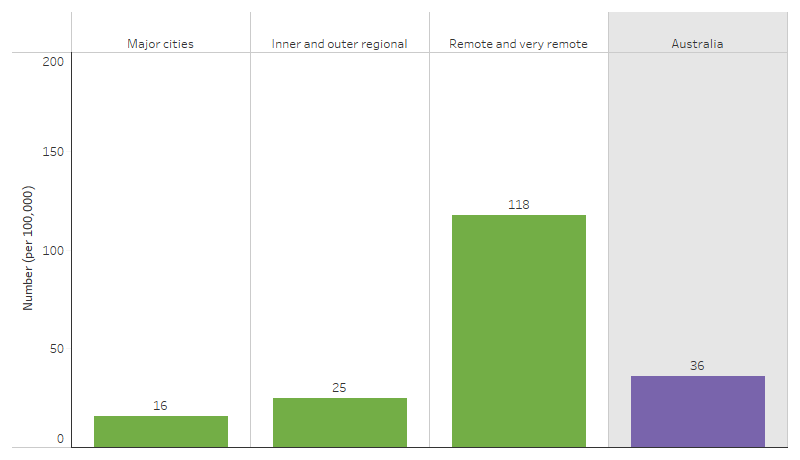
Source: Table D1.10.12. AIHW analysis of Australia and New Zealand Dialysis and Transplant Registry.
In 2020–2022, among First Nations people receiving kidney replacement therapy, the most common type of primary kidney disease was diabetic kidney disease (also known as diabetic nephropathy), which represents 73% (770) of the new 1,055 First Nations kidney replacement therapy patients. This was followed by glomerular disease (90 or 8.5%) and hypertension/renal vascular disease (59 or 5.6%) (Table D1.10.18, Figure 1.10.3).
Figure 1.10.3: Primary kidney disease of new First Nations kidney replacement therapy patients, 2020–2022
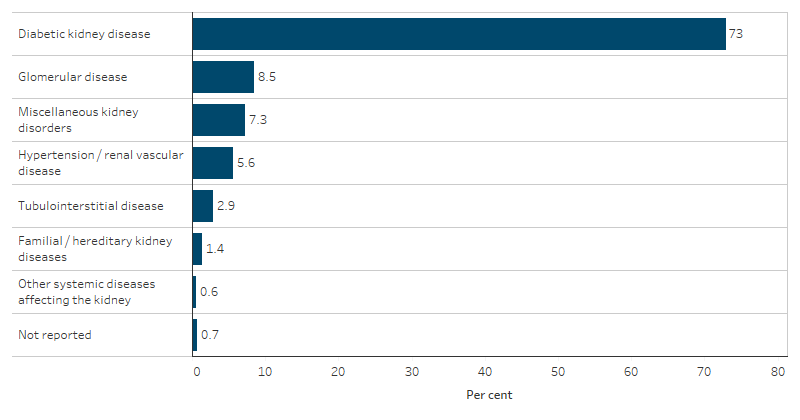
Source: Table D1.10.18. AIHW analysis of the Australia and New Zealand Dialysis and Transplant Registry.
As at 31 December 2022, there was a total of 2,625 First Nations people with kidney failure who were receiving kidney replacement therapy, a prevalence (existing cases) rate of 260 per 100,000 population. Of these cases:
- 2,204 (84%) were reliant on dialysis; and
- 421 (16%) had a functioning kidney transplant (that is, living with a successful kidney transplant, regardless of how long ago they received it) (Table 1.10-2).
Among people receiving kidney replacement therapy, First Nations people were less likely than non-Indigenous Australians to receive a kidney transplant. Among non-Indigenous Australians receiving kidney replacement therapy, 48% (12,113 of 25,120 patients) had a functioning kidney transplant, compared with 16% of First Nations people (421 of 2,625 patients) (Table 1.10-2).
Table 1.10-2: Total patients with kidney failure receiving replacement therapy, by Indigenous status and treatment, 31 December 2022
|
Treatment |
First Nations number |
Non-Indigenous number |
First Nations per cent |
Non-Indigenous per cent |
|---|---|---|---|---|
|
Dialysis |
2,204 |
13,007 | 84.0 | 51.8 |
|
Transplant |
421 | 12,113 | 16.0 | 48.2 |
|
Total |
2,625 |
25,120 |
100.0 |
100.0 |
Source: Table D1.10.14. AIHW analysis of Australia and New Zealand Dialysis and Transplant Registry.
Based on 2023 data, the majority (75%) of First Nations people receiving replacement therapy were treated with facility-based haemodialysis. The remaining 26% were able to access care closer to home – 3% were accessing at home haemodialysis, 5% were utilising long-term peritoneal dialysis and 17% had received a transplant (ANZDATA Registry et al. 2024).
In the 6-year period 2017–2022, 1,510 First Nations people were reliant on dialysis to manage their kidney failure at the time of their death. The primary cause of death in over one-third (587 deaths or 39%) of these cases was due to cardiovascular diseases, a further 23% (350 deaths) was due to withdrawal from dialysis and 12% (187 deaths) was due to infections. Among First Nations people who received a transplant to manage their kidney failure, there were 62 deaths in 2017–2022 – the leading cause of these deaths was cardiovascular disease (18 deaths or 29%), followed by infections (10 deaths or 16%), and cancer (9 deaths or 15%) (Table D1.10.17).
Findings from ABS survey data
Due to the asymptomatic nature of CKD in its early stage, and because diagnosis requires the presence of measured biomedical markers that persist for at least 3 months, people often do not realise they have the disease. As a result, numbers based on self-report are often underestimates of the true number of people living with CKD in Australia. Accurate estimates of the prevalence require large-scale surveys of biomedical markers of kidney function in the population.
The 2022–24 National Aboriginal and Torres Strait Islander Health Measures Survey (NATSIHMS) is the most recent national survey to include biomedical testing of markers for CKD among First Nations people. Based on the 2022–24 NATSIHMS, nearly 1 in 5 First Nations adults (18%, 101,300 people) had blood/urine test results showing signs of CKD. CKD is classified into 5 stages, depending on the level of kidney function. In 2022–24:
- 10% of First Nations adults had biomedical signs of CKD in the earliest stage (stage 1), and 5.2% in stage 2. In these stages there are usually no symptoms
- 2.9% of First Nations adults had biomedical signs of stage 3 CKD
- 0.7% of First Nations adults had biomedical signs of stage 4 or 5 CKD (Table D1.10.22).
In the 2022–24 NATSIHMS, only 13% (13,200 people) of those with signs of CKD reported having the condition, indicating that the majority of First Nations people with CKD did not realise they have it (87%, 88,200 people) (Table D1.10.22). Note however that the point-in-time tests used to identify signs of CKD cannot alone provide a diagnosis, and could indicate the presence of an acute kidney condition or infection instead. CKD can only be confirmed if indicators are persistent for at least 3 months.
Based on the self-reported data from the 2022–23 National Aboriginal and Torres Strait Islander Health Survey (NATSIHS), 2.1% of First Nations adults reported having CKD, with the highest rate for those aged 55 and over, at 5.4% (Table D1.10.23).
First Nations people living in remote areas were twice as likely as those living in non-remote areas to self-report having CKD (3.7% and 1.7%, respectively) (Table D1.10.23).
In 2022–23, First Nations adults who rated their health as fair/poor were 3.5 times as likely to report having CKD compared with those rating their health as excellent/very good/good (4.5% compared with 1.3%). First Nations adults who reported having diabetes were 3.7 times as likely to report having CKD compared with those without diabetes (5.7% compared with 1.6%). First Nations adults reporting cardiovascular problems were 5.1 times as likely to report having CKD compared with those without cardiovascular problems (5.8% compared with 1.1%) (Table D1.10.3).
Based on the 2022–23 NATSIHS, the rate of CKD among First Nations people was 2.5 times the rate for non-Indigenous adults (2.6% compared with 1.0%), after adjusting for differences in the age structure between the two populations (Table D1.10.1).
Change over time
Changes in death
Time series analysis of deaths data in this measure has been limited to the 2016 to 2021 period due to a break in time series for First Nations death statistics in New South Wales after 2021 (for more information see measure 1.22 All-cause age-standardised death rates and Data sources and quality).
From 2016 to 2021, the age-standardised death rate due to kidney diseases (including acute and chronic conditions) as the underlying cause of death fluctuated, ranging between 10 deaths per 100,000 population (in 2017) and 25 deaths per 100,000 (in 2020). Using linear regression to assess the overall trend, there was no statistically significant change in the rate for First Nations people, nor in the gap between First Nations people and non-Indigenous Australians (Table D1.23.23).
Changes in hospitalisations
Based on linear regression estimates, the age-standardised hospitalisation rate for CKD (excluding dialysis) among First Nations people increased by 25% between 2016–17 and 2022–23. The hospitalisation rate increased more for First Nations females than males (29% and 15% over the period, respectively) (Table D1.10.20, Figure 1.10.4).
Among non-Indigenous Australians, the age-standardised rate of hospitalisations for CKD disease (excluding dialysis) increased by 3.4% from 2016–17 to 2022–23, with increases for both males (4.4%) and females (2.3%). The absolute gap between First Nations people and non-Indigenous Australians increased from 2.8 hospitalisations per 1,000 population in 2016–17 to 4.1 per 1,000 in 2022–23 (Table D1.10.20).
Figure 1.10.4: Age-standardised hospitalisation rates for a principal diagnosis of CKD (excluding dialysis) for First Nations people, by sex, Australia, 2016–17 to 2022–23
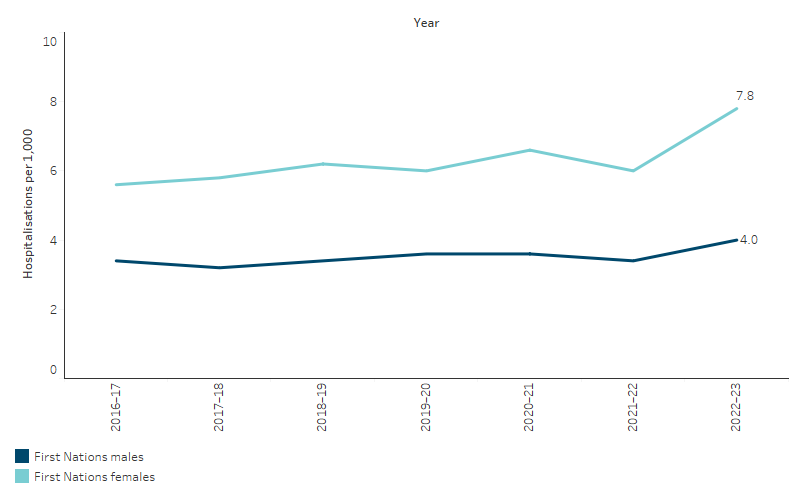
Source: Table D1.10.20 AIHW analysis of National Hospital Morbidity Database
Changes in incidence of replacement therapy
Data from the ANZDATA Registry shows that, over the period from 2016 to 2022, there were not any significant changes in the (age-standardised) incidence of kidney failure with replacement therapy for First Nations people. There were also no significant changes in this incidence rate when categorised by state and territory, nor any significant change in the gap of the rates between First Nations and non-Indigenous Australians (Table D1.10.13, Table D1.10.15, Figure 1.10.5).
Figure 1.10.5: Age-standardised incidence rates of kidney failure with replacement therapy, by Indigenous status, 2016 to 2022
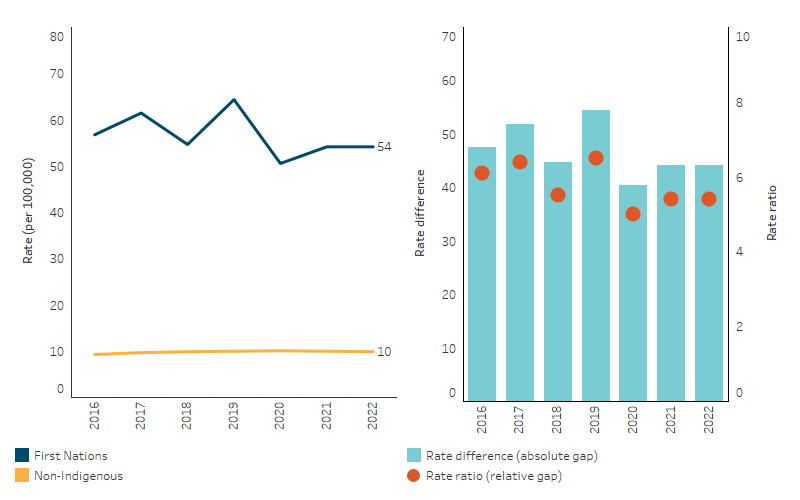
Source: Table D1.10.13. AIHW analysis of the Australia and New Zealand Dialysis and Transplant Registry.
Research and evaluation findings
Literature reviews highlight that kidney disease is influenced by multiple factors including nutritional and developmental disadvantage, low birthweight, childhood infections, family history, and adult-onset chronic diseases like hypertension and diabetes (Hoy 2014; Stumpers and Thomson 2013). However, there are potentially modifiable risk factors such as tobacco smoking, overweight and obesity, and insufficient physical activity (AIHW 2023a). Additionally, environmental factors like overcrowding and limited access to housing and functional facilities can lead to infectious skin conditions, such as post-streptococcal glomerulonephritis, which may result in chronic kidney disease (CKD) (DoH 2021).
Research highlights that interventions to modify high-risk behaviours in Indigenous populations are often ineffective when they fail to account for broader social, cultural, and historical contexts. Evidence shows that before colonisation, Indigenous diets were nutrient-dense and protective against chronic disease, but the introduction of refined cereals, sugars, salts, and fats has created new risk factors for conditions including kidney failure. Barriers such as negative social stereotyping, food insecurity, socioeconomic disadvantage, and disruption of traditional diets reflect structural challenges that shape health behaviours (Brimblecombe et al. 2014; Brimblecombe and O'Dea 2009; Hunt et al. 2008; Lee and Ride 2018) (see measures 2.18 Physical activity and 2.19 Dietary behaviour).
CKD affects First Nations adults at greater rates than for non-Indigenous Australians, and the origins of this disparity may begin early in life. A study found that preterm First Nations infants had significantly impaired kidney function, including higher serum creatinine, sodium excretion, and urine albumin levels, with vulnerability further influenced by antenatal and postnatal exposures. Maternal smoking, remote living, infant morbidities, and medications were all associated with impaired kidney function. Several risk factors, including combined antibiotic treatments, were linked to adverse kidney outcomes only in First Nations infants (Sutherland et al. 2019).
First Nations people experience disadvantage across the full continuum of kidney health, from prevention through to treatment. Before disease onset, systemic inequities in the social determinants of health contribute to higher rates of CKD risk factors, including diabetes and hypertension (AIHW 2024c; NACCHO 2021). These upstream factors are compounded by barriers to preventive health services, such as limited availability of screening, health promotion, and early intervention in remote and regional areas.
Adolescence and young adulthood (12–25 years) represent a critical window for establishing lifelong health behaviours and managing early risk factors for kidney disease. While early childhood and adult-focused interventions are well established, there is a gap in targeted strategies for this age group. Culturally safe health assessments, life skills development, and chronic disease education during this transitional life stage could support early prevention and improve long-term outcomes (AIHW 2024a).
Once kidney disease is established, First Nations people face additional challenges in accessing appropriate care. These include lower rates of transplant referral and evaluation due to reduced investigation, limited patient education, and communication difficulties. Higher rates of comorbidities, transplant incompatibility, and cultural bias further restrict access to transplantation. Geographic isolation exacerbates these disparities, with patients in remote areas significantly less likely to be waitlisted for a transplant – a gap that widens with increasing remoteness (AIHW 2024a).
First Nations patients are significantly less likely to be wait-listed for kidney transplantation compared to non-Indigenous Australians. Research identifies systemic barriers such as restrictive referral practices, limited service availability, cultural bias, and the impact of comorbidities on eligibility (Kelly et al. 2020; Khanal et al. 2018). Institutional racism and discriminatory healthcare environments further discourage engagement with kidney services, contributing to reduced treatment adherence and poorer outcomes (Bateman et al. 2023; Garrard and McDonald 2019; Hughes et al. 2023; Kelly et al. 2020; Khanal et al. 2018; Lakhan et al. 2022; Stumpers and Thomson 2013). These inequities are compounded for First Nations females, who experience the highest incidence of dialysis yet remain the least likely to access home-based or peritoneal dialysis. Contributing factors include increased rates of post-streptococcal glomerulonephritis in childhood, genetic predisposition with lower nephron numbers (resulting in reduced filtering capacity), and higher prevalence of obesity and metabolic syndrome leading to early-onset type 2 diabetes. These biological risks occur alongside systemic inequities such as limited access to primary healthcare, poor housing and sanitation, and socio-economic disadvantage, as well as caregiving responsibilities and exposure to violence, which influence access to and utilisation of health services. Globally, women have higher CKD prevalence but lower access to kidney replacement therapies, while men progress faster and receive transplants more often (McKercher et al. 2017; Wyld et al. 2022).
Systematic reviews show that CKD programs for First Nations people are most effective when integrated into primary care and supported by culturally appropriate approaches. Successful models feature nurse-led or Aboriginal Health Worker-led care, intensive follow-up, and culturally tailored education (Reilly et al. 2016). However, implementation faces barriers such as inadequate resources, workforce shortages, poor coordination, and complex administrative requirements. Broader social determinants such as limited access to healthy food, inadequate housing, transport barriers, and experiences of racism also impede engagement and continuity of care (Yadav et al. 2024; Yadav et al. 2025).
A community-based chronic kidney care model (CYKC) was trialled to improve access to specialist kidney services for First Nations patients in remote areas. The CYKC model addressed systemic barriers by embedding kidney care within primary health services and enabling specialist kidney reviews closer to home. This approach led to an increase in the number of patients with CKD reviewed by nephrologists within the community, with a focus on those at high risk of disease progression. By improving early detection and management, the CYKC model demonstrated a potential to reduce the burden of CKD and improve long-term health outcomes for First Nations people. The study highlights the importance of integrating culturally safe, community-led models of care to address the structural inequities that contribute to poorer kidney health outcomes (Miller et al. 2023).
Evidence supports culturally safe, patient-centred kidney care as a viable alternative to mainstream hospital-based dialysis, improving access and patient outcomes. The Kanggawodli model in Adelaide provided a home-like environment, flexible scheduling, and culturally safe care, enabling patients to maintain social and cultural connections while receiving treatment. Patients reported greater comfort, empowerment, and adherence to dialysis schedules, while providers observed improved health literacy and engagement in care. The model also strengthened provider cultural competency and increased community demand for similar services closer to home, demonstrating the importance of integrating kidney care within existing cultural frameworks (Shearing et al. 2023).
International epidemiological research on CKD among colonised Indigenous populations has traditionally focused on biological causes, particularly type 2 diabetes and cardiovascular disease. However, from 2012 to 2019, studies incorporating Indigenous-led methodologies increasingly identified colonisation, racism, and socioeconomic disparities as key drivers of CKD inequities. Indigenous peoples globally, including Australia, face common barriers, including inadequate health care access, cultural bias in medical care, and geographic isolation. Expanding analyses to include Indigenous perspectives and broader determinants of health is essential for developing effective interventions. Understanding the links between power, colonisation, and resource loss is critical for informing health policy and research (Chaturvedi et al. 2024; Huria et al. 2021).
The albumin-to-creatinine ratio (ACR) is a key marker of kidney disease progression, with higher levels associated with a faster decline in kidney function. A study across urban, regional, and remote sites in Australia found that First Nations people experienced a rate of decline in kidney function – measured by estimated glomerular filtration rate (eGFR) – three times higher than non-Indigenous populations. The eGFR estimates how well kidneys are filtering blood. It is commonly used to monitor the progression of kidney disease over time. The study identified ACR, diabetes, and lower kidney function as strong predictors of CKD progression (Maple-Brown et al. 2016). A study of 492 Tiwi people found that 20.3% had an ACR indicating high risk of CKD, with nearly one in three at severely increased risk. Tiwi people had significantly higher ACR levels than other ethnic groups, independent of glycaemic control, and ACR was found to be highly heritable (52%) in this population. These findings highlight the importance of early detection and population-specific approaches, such as personalised medicines, to improve CKD prevention and treatment for First Nations communities (Arunachalam et al. 2024).
Childhood infections such as streptococcal infections and urinary tract infections (UTIs) can cause kidney damage and long-term kidney disease if untreated. Post-streptococcal glomerulonephritis (PSGN) may develop weeks after an untreated strep throat or skin infection, leading to kidney inflammation and reduced function, particularly in children aged 6–10 years. Untreated UTIs can also cause kidney scarring and, in severe cases, become life-threatening if bacteria enter the bloodstream. Early diagnosis and antibiotic treatment are essential, as some UTIs may indicate underlying conditions like urinary reflux or blockages, which can lead to permanent kidney damage if not addressed (National Kidney Foundation n.d.).
First Nations women in the Northern Territory with gestational diabetes mellitus (GDM) or pre-existing diabetes during pregnancy are at significantly increased risk of developing CKD and end-stage kidney disease (ESKD). A study of First Nations women who gave birth between 2000 and 2016, found that those with GDM were around 4 times as likely to develop CKD and 6 times as likely to develop ESKD compared with those without diabetes in pregnancy. Among women with pre-existing diabetes, nearly 1 in 3 developed CKD, and 1 in 10 developed ESKD, with risks substantially higher than for those without diabetes. Most women with GDM who later developed kidney disease had progressed to type 2 diabetes before onset. While diabetes in pregnancy was the primary focus, other factors such as age, hypertensive disorders of pregnancy, remoteness, and socioeconomic disadvantage also contributed to increased CKD and ESKD risk. These findings highlight pregnancy as a key opportunity to identify and mitigate kidney disease risk, with a need for strategies that address both clinical and social determinants of health (Hare et al. 2023).
A cohort analysis of intensive care unit (ICU) admissions for dialysis-dependent chronic kidney disease (CKD5D) between 2010 and 2017 found that First Nations people were significantly overrepresented, accounting for 11.9% of CKD5D ICU admissions despite comprising only 2.8% of the population. First Nations patients were, on average, 13.5 years younger than non-Indigenous CKD5D patients and more likely to live in very remote (25.4% compared to 1.0%) and socioeconomically disadvantaged areas (33.3% compared to 12.7%). Despite their younger age and fewer comorbidities, First Nations CKD5D patients had a comparable severity of illness on ICU admission and a lower crude hospital mortality rate (12.1% compared to 16.8%). However, after adjusting for age, remoteness, and illness severity, mortality was equivalent between First Nations and non-Indigenous patients, suggesting that systemic disadvantage drives earlier disease onset and ICU admissions rather than inherently worse outcomes (Dunlop et al. 2022).
High rates of First Nations people in remote areas requiring dialysis leads to patients leaving their homes, communities and Country to visit dialysis services in non-remote areas. Research found that almost one quarter (23.9%) of Australian kidney replacement therapy patients between 2005 and 2015 relocated, with patients relocating more frequently and earlier from outer regional, remote and very remote areas towards major cities and inner regional areas (Hassan et al. 2020). This disruption can significantly affect patients’ health, wellbeing, and connection to family and culture.
To address this, dialysis services in remote Australia have been expanding through providers such as the Purple House. In 2024–25, Purple House provided over 11,000 dialysis treatments on Country, supporting 227 patients across 20 remote clinics and through two mobile dialysis units known as the Purple Trucks. These services enable patients to return home for family, cultural, or sorry business, helping to maintain community connection and improve wellbeing (Purple House 2025). An independent review of rural dialysis models found that First Nations-controlled services like Purple House are not only more culturally appropriate but are also more cost-effective than urban-based care, all while improving access, continuity, and patient satisfaction in remote First Nations communities (Agency for Clinical Innovation 2024).
The South Australian Mobile Dialysis Truck allows patients to have dialysis closer to home for one- to two-week periods. A qualitative evaluation on the Country Health SA Dialysis bus found that it improved the social and emotional wellbeing of patients by allowing them to fulfil cultural commitments and improved patient quality of life, as well as build positive relationships and trust between metropolitan nurses and remote patients, contributing to improved cultural competency among health professionals (Conway et al. 2018; Rix et al. 2014) (for more information see measure 2.13 Transport). While mobile dialysis services face logistical challenges, including transport difficulties, accommodation shortages, staff strain, weather disruptions, and mechanical issues, staff have noted that additional support could help overcome these barriers and increase patient participation. Importantly, mobile dialysis units, such as those operated by the South Australian Government and the Purple House, provide short-term care that supports cultural connection, but do not address long-term relocation needs. Therefore, fixed dialysis infrastructure, like the community-controlled clinics run by Purple House, remains essential to enabling First Nations people to stay on Country and receive ongoing care.
A study of First Nations people who commenced dialysis between 2006 and 2020 found that deceased donor kidney transplantation provides a significant survival benefit compared to remaining on dialysis, with benefits similar to those observed in non-Indigenous Australians. Despite this, First Nations people are far less likely to receive transplants. The major barrier to transplantation is being waitlisted, with systemic biases across referral, limiting access to assessment and listing processes. Health professionals and First Nations communities both have important roles in improving equitable access to kidney transplantation. While there is strong community interest in transplantation as a pathway to return home and reconnect with family and Country, systemic barriers persist. Addressing these requires more than just better information – it involves building cultural awareness in the health system, reflecting on institutional biases, and ensuring culturally safe care (Bateman et al. 2024). Aboriginal Community Controlled Health Organisations (ACCHOs), as trusted and community-governed providers, are well placed to lead and support initiatives that promote culturally secure pathways to transplantation. Additionally, the appropriateness of health services strongly influences care uptake among First Nations people, with cultural security identified as essential to effective health care. Without it, First Nations patients may experience emotional and physical discomfort, leading to reduced service use and poorer outcomes (Coffin 2007).
A study of children in Australia and New Zealand who commenced kidney replacement therapy (KRT) between 2000 and 2020 found that peritoneal dialysis (PD) was the most prescribed first treatment and pre-emptive kidney transplantation the least. Outcomes for children receiving KRT were generally positive, with excellent patient survival, technique survival and graft survival rates. Graft survival for those that received kidney transplantation has improved over the last two decades, with 5-year death-censored graft survival increasing from 84.3% (2000–2010) to 88.4% (2011–2020). Despite these improvements, significant disparities exist for Indigenous children, who experience longer durations on dialysis before transplantation, lower rates of pre-emptive kidney transplants, and lower likelihood of receiving a live donor kidney. Factors such as remoteness, language barriers, poor access to transplant services, and health system biases contribute to these inequities, which also impact survival outcomes (Ambarsari et al. 2023).
A cohort study of first-time kidney transplant recipients (2005–2018) found that First Nations people had a two-fold higher risk of allograft loss – that is, loss of the transplanted kidney’s function, typically resulting in a return to dialysis or the need for another transplant – and a three-fold higher risk of infection-related death compared to non-Indigenous Australians. While acute rejection partially explained the disparity in graft loss, infection-related deaths occurred independently of this factor. The study suggests that social and structural determinants likely contribute to these survival disparities, highlighting the complex and multifactorial nature of post-transplant outcomes (Van Loon et al. 2020; Zheng et al. 2022).
The National Indigenous Kidney Transplantation Taskforce (NIKTT) was established in 2019 following a Commonwealth-funded expert panel review that identified critical barriers to kidney transplantation for First Nations people. The NIKTT focused on four key areas:
- Establish a national network of collaborators
- Enhance data collection to improve understanding of waitlisting barriers
- Pilot initiatives to increase transplant access
- Address cultural bias in kidney care.
The NIKTT Final Report (2019–2022) highlights key findings, including that only 2% of First Nations dialysis patients were waitlisted in 2020, compared with 8% of non-Indigenous patients, though waitlisting rates have improved since NIKTT initiatives began. Successful models of care – such as Outreach Assessment Clinics, patient navigator programs, and tailored education resources – demonstrated improved waitlist access, but challenges remain in workforce recruitment and administrative burdens. The Cultural Bias Report outlined four domains for action and 14 recommendations, with priority actions including establishing Indigenous Reference Groups in transplant units, increasing First Nations kidney health workforce capacity, and implementing patient navigator roles. In 2022, the NIKTT endorsed a Position Statement, sent to state, territory, and federal ministers, advocating for structural reforms. The Taskforce presented three key recommendations: (1) sustainable funding for First Nations-led kidney care initiatives, (2) establishment of a NIKTT Secretariat to monitor progress for at least three years, and (3) investigation into systemic inequities beyond waitlisting to improve transplantation outcomes. These recommendations were presented to the Jurisdictional Organ and Tissue Steering Committee (JOTSC) in 2022–2023 for inclusion in the national transplant strategy (Cundale et al. 2023).
Implications
Historically, Commonwealth, state, and territory governments have tried to present policies in addressing chronic kidney disease (CKD) disparities for First Nations people and rural and remote communities. From 2020 to 2022, the incidence of First Nations patients with kidney failure requiring kidney replacement therapy was more than 7 times as high in Remote and very remote areas as in Major cities. Despite First Nations people having a higher incidence rate of kidney failure with replacement therapy than non-Indigenous Australians, research on policies up to March 2022 revealed a lack of policies specifically addressing improved access to CKD care for First Nations people. Barriers to treatment include limited access to healthcare services, financial and travel burdens, and a biomedical model of care that does not incorporate culturally appropriate approaches. The lack of prevention and screening policies further compounds inequities, particularly for First Nations people, who experience unequal rates of transplantation and home dialysis (DoHAC 2020; Recabarren et al. 2024).
Kidney disease presents a significant burden for both individuals and the health system. For patients, living with CKD often involves ongoing dialysis, frequent travel for treatment, dietary restrictions, fatigue, and disruptions to family, cultural, and community life. These challenges can lead to emotional distress, financial strain, and reduced quality of life. At the system level, CKD accounted for an estimated $1.9 billion in health expenditure in 2020–21, representing 1.2% of the total disease expenditure in Australia. Of this, $1.7 billion (89% of the total expenditure for CKD) was spent on hospital services: $1.2 billion on admitted patient care in public hospitals, $261.6 million on private hospital services, and $158.1 million on public hospital outpatient care (AIHW 2023a, 2024b).
The National Strategic Action Plan for Kidney Disease (the Action Plan) provides a coordinated, long-term approach to preventing kidney disease, improving care for those affected, and advancing research to enhance treatment outcomes. It acknowledges the disproportionate burden of kidney disease among First Nations people and includes targeted strategies to address these inequities. Objective 2.4 focuses on ‘reducing the disproportionate burden of kidney disease in Aboriginal and Torres Strait Islander communities’, with additional actions supporting First Nations health outcomes embedded throughout the priority areas. A key overarching recommendation is ensuring First Nations people are actively involved in policy development, program implementation, research, and healthcare service delivery. The Action Plan highlights the importance of cultural safety and self-determination, ensuring all initiatives are community-led and culturally responsive.
Mainstream service providers and specialists must ensure culturally safe practices to better help First Nations people, particularly from remote areas, to navigate the kidney disease continuum. The CARI guidelines: Recommendations for Culturally Safe and Clinical Kidney Care for First Nations Australians recommend that institutional racism could be addressed through actively decolonising services by starting with increasing self-determination and empowerment of patients, families, and communities that need to engage with mainstream kidney health services (Tunnicliffe et al. 2022).
The Cultural Respect Framework 2016–2026 reaffirms the Australian Government’s longstanding commitment to embedding cultural respect in the health system, ensuring equitable access and improved health outcomes for First Nations people (National Aboriginal and Torres Strait Islander Health Standing Committee 2017). The Aboriginal and Torres Strait Islander Health Performance Framework plays a role in monitoring this commitment across several measures (see measure 3.08 Cultural competency). Monitoring is also supported by the Cultural safety in health care for Indigenous Australians: monitoring framework which covers three domains: how health-care services are provided, First Nations patients’ experience of health care, and measures regarding access to health care (AIHW 2023b). The 2023 cultural safety report showed whether First Nations-specific health care organisations and maternal/child health services had a formal commitment to achieving culturally safe health care. From 2012–13 to 2017–18 the proportion of these services with a formal commitment increased from 86% to 95%. However, the lack of data on mainstream health services presents a challenge to ensuring culturally safe and effective health services for First Nations people (AIHW 2023b).
The Australian Government is addressing disparities in kidney health care for First Nations people by increasing access to dialysis services in remote communities. Through the Better Renal Services for First Nations Peoples initiative, the Government is funding the establishment of dialysis units in areas where access to treatment is limited, reducing the burden of travel and enabling patients to receive care while staying on Country. Under the initiative, three new renal dialysis units are being established in remote Queensland and Western Australia, while a further seven remote communities in the Northern Territory, Queensland, and Western Australia will receive new dialysis units in the third funding round. These communities were selected based on high demand, significant distance from existing services, and strong community support. In addition to expanding dialysis access, the initiative is improving water security through the National Water Grid Fund, ensuring communities have a safe and reliable water supply for dialysis treatment. The expansion of remote dialysis services is expected to improve health outcomes, treatment adherence, and quality of life for First Nations people, addressing a critical gap in kidney care (Kearney 2024; McCarthy 2024; Morse 2024).
Purple House is an Aboriginal community-controlled organisation, which provides culturally safe dialysis services in remote First Nations communities, enabling patients to receive care on Country while maintaining vital social and cultural connections. Their model includes dialysis treatment, aged care, disability services, social support programs, and initiatives such as the Return to Country program. Purple House promotes First Nations employment, with one-third of its staff being First Nations people, including Patient Preceptors who bridge gaps between communities and mainstream health care services. Through these efforts, Purple House enhances First Nations leadership, supports self-determination, and ensures that care aligns with cultural priorities and needs, contributing to broader systemic improvements in kidney health equity (Purple House 2025).
The National Aboriginal and Torres Strait Islander Health Plan 2021–2031 (The Health Plan) emphasises the need for culturally safe and community-led approaches that integrate structural, environmental, and lifestyle factors affecting kidney health. It prioritises early and equitable access to comprehensive primary health care through community-controlled health services, aiming to prevent hospitalisation and improve early intervention for chronic disease. The plan includes a long-term vision to eliminate racism in the health system, with immediate actions to address systemic bias and ensure culturally safe and responsive care. This aligns with Priority Reform 3 of the National Agreement on Closing the Gap, focusing on transforming government organisations to be culturally safe and more responsive to the needs of First Nations people.
In September 2022, the Australian Government expanded the Pharmaceutical Benefits Scheme listing of clinical indications for the drug treatment dapagliflozin to improve or maintain kidney function independent of diabetic control and help reduce the risk of progressive decline in kidney function. This expansion was expected to benefit thousands of Australians, including First Nations people who are disproportionately affected by CKD.
The NT Health Kidney Plan 2024–2029 outlines a strategic approach to addressing the high burden of kidney disease in the Northern Territory, with a focus on improving prevention, detection, and treatment. It emphasises community-led initiatives, expanded models of care, and enhanced workforce capacity to improve health outcomes, particularly for First Nations people who experience disproportionately high rates of CKD. Key actions include increasing access to culturally safe care, strengthening renal workforce training, expanding remote dialysis options, and enhancing data collection for service planning. The plan also prioritises improved pathways for kidney transplantation and partnerships with Aboriginal Community Controlled Health Organisations (ACCHOs) to provide holistic, culturally competent care (Northern Territory Government 2024). These efforts are bolstered by the introduction of the First Nations Health Worker Traineeship (FNHWT) program, developed by First Nations organisations in partnership with government and coordinated through the National Aboriginal Community Controlled Health Organisation (NACCHO). This program will certify up to 500 First Nations people as First Nations Health Workers or Practitioners by 2027. Delivered through on-the-job training by Aboriginal Community Controlled Health Registered Training Organisations (ACCHRTOs), the program aims to strengthen the First Nations health workforce by building culturally safe, community-based care and addressing critical workforce shortages in ACCHOs (NACCHO 2024).
References
- Agency for Clinical Innovation (2024) Evidence brief: rural renal dialysis models of care, Critical Intelligence Unit‚ NSW Government.
-
AIHW (Australian Institute of Health and Welfare) (2014) Assessment of the coding of ESKD in deaths and hospitalisation data: a working paper using linked hospitalisation and deaths data from Western Australia and New South Wales, AIHW, Australian Government.
-
AIHW (2019) Indicators of socioeconomic inequalities in cardiovascular disease, diabetes and chronic kidney disease, AIHW, Australian Government, doi:10.25816/5ebca9d1fa7e0.
-
AIHW (2022) Impact and causes of illness and death in Aboriginal and Torres Strait Islander people 2018, Australian Burden of Disease Study, AIHW, Australian Government, doi:10.25816/xd60-4366.
-
AIHW (2023a) Chronic kidney disease: Australian facts, AIHW, Australian Government, accessed 29 September 2025.
-
AIHW (2023b) Cultural safety in health care for Indigenous Australians: monitoring framework, AIHW, Australian Government, accessed 22 August 2025.
-
AIHW (2024a) Chronic kidney disease: Australian facts, AIHW, Australian Government, accessed 20 October 2025.
-
AIHW (2024b) Chronic kidney disease: Australian facts [data set], AIHW website, accessed 29 September 2025.
-
AIHW (2024c) Determinants of health for First Nations people, AIHW, Australian Government.
-
AIHW (2025) Closing the Gap targets: key findings and implications, AIHW, Australian Government, doi:10.25816/gqtf-2k57.
-
Ambarsari CG, Cho Y, Milanzi E, Francis A, Koh LJ, Lalji R and Johnson DW (2023) 'Epidemiology and outcomes of children with kidney failure receiving kidney replacement therapy in Australia and New Zealand', Kidney International Reports, 8(10):1951–1964, doi:10.1016/j.ekir.2023.07.006.
-
ANZDATA Registry (2021) 'Haemodialysis: reporting the incidence, prevalence, and survival of haemodialysis patients in Australia and New Zealand; summarising dialysis prescriptions, laboratory results, dialysis adequacy, vascular access, and rates of home haemodialysis treatment', in ANZDATA 44th Annual Report 2021, Australia and New Zealand Dialysis and Transplant Registry, Adelaide.
-
ANZDATA Registry, Bateman S, Solomon B, Davies C, Au E, Chen J, Clayton P, Hurst K, Kholmurodova F, Lee D, McCarthy H, McDonald S, Mulley W, Roberts M, Sun T and Iris G (2024) 'Kidney failure in Aboriginal and Torres Strait Islander Australians: reporting the incidence, prevalence and survival of Aboriginal and Torres Strait Islander Australians receiving kidney replacement therapy', in ANZDATA 47th Annual Report 2024, Australia and New Zealand Dialysis and Transplant Registry, Adelaide.
-
Arunachalam V, Lea R, Hoy W, Lee S, Mott S, Savige J, Mathews JD, McMorran BJ and Nagaraj SH (2024) 'Novel genetic markers for chronic kidney disease in a geographically isolated population of Indigenous Australians: individual and multiple phenotype genome-wide association study', Genome Medicine, 16(1):29, doi:10.1186/s13073-024-01299-3.
-
Bateman S, Owen K, Lester R, Pearson O, Lawton P, McDonald S, Jesudason S and Clayton PA (2024) 'The survival benefit of deceased donor kidney transplantation for Aboriginal and Torres Strait Islander people, 2006–20: a retrospective national cohort study', Medical Journal of Australia, 221(2):111–116, doi:10.5694/mja2.52361.
-
Bateman S, Riceman M, Owen K, Pearson O, Lester R, Sinclair N, McDonald S, Howell M, Tunnicliffe D and Jesudason S (2023) 'Models of care to address disparities in kidney health outcomes for First Nations people', Kidney International, 104(4):681–689, doi:10.1016/j.kint.2023.06.026.
-
Brimblecombe J, Maypilama E, Colles S, Scarlett M, Dhurrkay J, Ritchie J and O’Dea K (2014) 'Factors influencing food choice in an Australian Aboriginal community', Qualitative Health Research, 24(3):387–400, doi:10.1177/1049732314521901.
-
Brimblecombe JK and O'Dea K (2009) 'The role of energy cost in food choices for an Aboriginal population in northern Australia', Medical Journal of Australia, 190(10):549–551, doi:10.5694/j.1326-5377.2009.tb02560.x.
-
Chaturvedi S, Victoria Bianchi ME, Bello A, Crowshoe H and Hughes JT (2024) 'Barriers to optimal kidney health among Indigenous peoples', Kidney International Reports, 9(3):508–511, doi:10.1016/j.ekir.2024.01.038.
-
Coffin J (2007) 'Rising to the challenge in Aboriginal health by creating cultural security', Aboriginal and Islander Health Worker Journal, 31(3):22–24.
-
Conway J, Lawn S, Crail S and McDonald S (2018) 'Indigenous patient experiences of returning to country: a qualitative evaluation on the Country Health SA Dialysis Bus', BMC Health Services Research, 18(1):1010, doi:10.1186/s12913-018-3849-4.
-
Cundale K, Hughes J, Owen K and McDonald S (2023) Final report: National Indigenous Kidney Transplantation Taskforce, National Indigenous Kidney Transplantation Taskforce, accessed 19 March 2025.
-
DoH (Department of Health) (2021) National Aboriginal and Torres Strait Islander Health Plan 2021–2031, DoH, Australian Government, accessed 2 May 2025.
-
DoHAC (Department of Health and Aged Care) (2020) What we're doing about kidney disease, DoHAC website, accessed 18 February 2025.
-
Dunlop WA, Secombe PJ, Agostino JW and van Haren FMP (2022) 'Characteristics and outcomes of Aboriginal and Torres Strait Islander patients with dialysis-dependent kidney disease in Australian intensive care units', Internal Medicine Journal, 52(3):458–467, doi:10.1111/imj.15077.
-
Garrard E and McDonald S (2019) Improving access to and outcomes of kidney transplantation for Aboriginal and Torres Strait Islander people in Australia: performance report, Transplantation Society of Australia and New Zealand.
-
Hare MJL, Maple-Brown LJ, Shaw JE, Boyle JA, Lawton PD, Barr ELM, Guthridge S, Webster V, Hampton D, Singh G, Dyck RF and Barzi F (2023) 'Risk of kidney disease following a pregnancy complicated by diabetes: a longitudinal, population-based data-linkage study among Aboriginal women in the Northern Territory, Australia', Diabetologia, 66(5):837–846, doi:10.1007/s00125-023-05868-w.
-
Hassan HIC, Chen JH and Murali K (2020) 'Incidence and factors associated with geographical relocation in patients receiving renal replacement therapy', BMC Nephrology, 21(1):249, doi:10.1186/s12882-020-01887-6.
-
Hoy WE (2014) 'Kidney disease in Aboriginal Australians: a perspective from the Northern Territory', Clinical Kidney Journal, 7(6):524–530, doi:10.1093/ckj/sfu109.
-
Hughes JT, Cundale K, Webster A, Owen KJ and McDonald SP (2023) 'Towards equity in kidney transplantation: the next steps', Medical Journal of Australia, 219(S8):S19–S22, doi:10.5694/mja2.52111.
-
Hunt J, Marshall AL and Jenkins D (2008) 'Exploring the meaning of, the barriers to and potential strategies for promoting physical activity among urban Indigenous Australians', Health Promotion Journal of Australia, 19(2):102–108, doi:10.1071/he08102.
-
Huria T, Pitama SG, Beckert L, Hughes J, Monk N, Lacey C and Palmer SC (2021) 'Reported sources of health inequities in Indigenous Peoples with chronic kidney disease: a systematic review of quantitative studies', BMC Public Health, 21:1447, doi:10.1186/s12889-021-11180-2.
-
Kearney G (13 November 2024) More dialysis units for remote communities [media release], Office of the Hon Ged Kearney, Former Assistant Minister for Indigenous Health, Former Assistant Minister for Health and Aged Care, Department of Health and Aged Care, Australian Government, accessed 20 March 2025.
-
Kelly J, Dent P, Owen K, Schwartzkopff K and O’Donnell K (2020) Cultural bias Indigenous kidney care and kidney transplantation report, report to National Indigenous Kidney Transplantation Taskforce, The University of Adelaide, Lowitja Institute.
-
Khanal N, Lawton PD, Cass A and McDonald SP (2018) 'Disparity of access to kidney transplantation by Indigenous and non‐Indigenous Australians', Medical Journal of Australia, 209(6):261–266, doi:10.5694/mja18.00304.
-
Kidney Health Australia (2025) Aboriginal and Torres Strait Islander peoples, Kidney Health Australia website, accessed 24 February 2025.
-
Lakhan P, Cooney A, Palamuthusingam D, Torrens G, Spurling G, Martinez A and Johnson D (2022) 'Challenges of conducting kidney health checks among patients at risk of chronic kidney disease and attending an urban Aboriginal and Torres Strait Islander primary healthcare service', Australian Journal of Primary Health, 28(5):371–379, doi:10.1071/PY21248.
-
Lee A and Ride K (2018) 'Review of nutrition among Aboriginal and Torres Strait Islander people', Australian Indigenous Health Bulletin, 18(1).
-
Levey AS, Eckardt KU, Dorman NM, Christiansen SL, Hoorn EJ, Ingelfinger JR, Inker LA, Levin A, Mehrotra R, Palevsky PM, Perazella MA, Tong A, Allison SJ, Bockenhauer D, Briggs JP, Bromberg JS, Davenport A, Feldman HI, Fouque D, Gansevoort RT, Gill JS, Greene EL, Hemmelgarn BR, Kretzler M, Lambie M, Lane PH, Laycock J, Leventhal SE, Mittelman M, Morrissey P, Ostermann M, Rees L, Ronco P, Schaefer F, St Clair Russell J, Vinck C, Walsh SB, Weiner DE, Cheung M, Jadoul M and Winkelmayer WC (2020) 'Nomenclature for kidney function and disease: report of a Kidney Disease: Improving Global Outcomes (KDIGO) consensus conference', Kidney International, 97(6):1117–1129, doi:10.1016/j.kint.2020.02.010.
-
Maple-Brown LJ, Hughes JT, Ritte R, Barzi F, Hoy WE, Lawton PD, Jones GRD, Death E, Simmonds A, Sinha AK, Cherian S, Thomas MAB, McDermott R, Brown ADH, O'Dea K, Jerums G, Cass A and MacIssac RJ (2016) 'Progression of kidney disease in Indigenous Australians: the eGFR follow-up study', Clinical Journal of the American Society of Nephrology, 11(6):993–1004, doi:10.2215/CJN.09770915.
-
Marmot MG (2006) 'Status syndrome: a challenge to medicine', JAMA, 295(11):1304–1307, doi:10.1001/jama.295.11.1304.
-
McCarthy M (19 July 2024) Three new renal units to open in remote Queensland and Western Australia [media release], Office of the Hon Malarndirri McCarthy, Department of Health and Aged Care, Australian Government, accessed 20 March 2025.
-
McKercher C, Jose MD, Grace B, Clayton PA and Walter M (2017) 'Gender differences in the dialysis treatment of Indigenous and non‐Indigenous Australians', Australian and New Zealand Journal of Public Health, 41(1):15–20, doi:10.1111/1753-6405.12621.
-
Miller A, Brown L, Tamu C and Cairns A (2023) 'Cape York Kidney Care: service description and baseline characteristics of a client-centred multidisciplinary specialist kidney health service in remote Australia', BMC Health Services Reseach, 23:907, doi:10.1186/s12913-023-09887-6.
-
Morse C (2024) 'Essential, lifesaving treatment: more dialysis units on the way to remote First Nations communities', National Indigenous Times.
-
Morton RL, Schlackow I, Mihaylova B, Staplin ND, Gray A and Cass A (2016) 'The impact of social disadvantage in moderate-to-severe chronic kidney disease: an equity-focused systematic review', Nephrology Dialysis Transplantation, 31(1):46–56, doi:10.1093/ndt/gfu394.
-
NACCHO (National Aboriginal Community Controlled Health Organisation) (2021) Core Services and Outcomes Framework: the Model of Aboriginal and Torres Strait Islander Community-Controlled Comprehensive Primary Health Care, NACCHO.
-
NACCHO (7 March 2024) First Nations Health Worker Traineeship Program (FNHWTP) [media release], NACCHO, accessed 5 May 2025.
-
National Aboriginal and Torres Strait Islander Health Standing Committee (2017) Cultural Respect Framework 2016–2026 for Aboriginal and Torres Strait Islander health, Australian Health Ministers' Advisory Council.
-
National Kidney Foundation (2023) Kidney failure, National Kidney Foundation website, accessed 19 March 2025.
-
National Kidney Foundation (n.d.) Childhood infections & kidney disease, National Kidney Foundation website, accessed 18 February 2025.
-
Northern Territory Government (2024) Supporting people living with kidney disease, Northern Territory Government website, accessed 20 March 2024.
-
Purple House (2025) Social impact report 2024–2025, Social Impact Report Series, Western Desert Nganampa Walytja Palyantjaku Tjutaku Aboriginal Corporation.
-
Recabarren J, Dominello A, Scholes-Robertson N, Jaure A, Wong G, Craig JC and Howell M (2024) 'It matters who you are and where you live: Commonwealth, state and territory policies for access to care for Australians with chronic kidney disease and their caregivers', Australian and New Zealand Journal of Public Health, 48(2):100131, doi:10.1016/j.anzjph.2024.100131.
-
Reilly R, Evans K, Gomersall J, Gorham G, Peters MDJ, Warren S, O’Shea R, Cass A and Brown A (2016) 'Effectiveness, cost effectiveness, acceptability and implementation barriers/enablers of chronic kidney disease management programs for Indigenous people in Australia, New Zealand and Canada: a systematic review of mixed evidence', BMC Health Services Research, 16:119, doi:10.1186/s12913-016-1363-0.
-
Ritte RE, Lawton P, Hughes JT, Barzi F, Brown A, Mills P, Hoy W, O'Dea K, Cass A and Maple-Brown L (2020) 'Chronic kidney disease and socio-economic status: a cross sectional study', Ethnicity & Health, 25(1):93–109, doi:10.1080/13557858.2017.1395814.
-
Rix EF, Barclay L, Stirling J, Tong A and Wilson S (2014) ''Beats the alternative but is messes up your life': Aboriginal people's experience of haemodialysis in rural Australia', BMJ Open, 4(9):e005945, doi:10.1136/bmjopen-2014-005945.
-
Shearing T, Sivak L, Mejia G, Clinch N, O’Donnell K, Sinclair N, Kartinyeri J, Owen K, Clinch D and Morey K (2023) 'A pilot place-based renal dialysis model of care responding to Aboriginal and Torres Strait Islander priorities in South Australia', Australian and New Zealand Journal of Public Health, 47(6):100107, doi:10.1016/j.anzjph.2023.100107.
-
Stumpers SA and Thomson NJ (2013) 'Review of kidney disease among Indigenous people', Australian Indigenous Health Bulletin, 13(2).
-
Sutherland MR, Chatfield MD, Davison B, Vojisavljevic D, Kent AL, Hoy WE, Singh GR and Black MJ (2019) 'Renal dysfunction is already evident within the first month of life in Australian Indigenous infants born preterm', Kidney International, 96(5):1205–1216, doi:10.1016/j.kint.2019.07.015.
-
Sypek MP, Dansie KB, Clayton P, Webster AC and McDonald S (2018) 'Comparison of cause of death between Australian and New Zealand Dialysis and Transplant Registry and the Australian National Death Index', Nephrology, 24(3):322–329, doi:10.1111/nep.13250.
-
Tunnicliffe D, Bateman S, Arnold-Chamney M, Dwyer K, Howell M, Gebadi A, Jesudason S, Kelly J, Lambert K, Majoni S, Olivia D, Owen K, Pearson O, Rix E, Roberts I, Stirling K, Wittert G, Widders K, Yip A, Craig J and Phoon R (2022) Recommendations for culturally safe and clinical kidney care for First Nations Australians, CARI Guidelines, Caring for Australian and New Zealanders with Kidney Impairment.
-
Van Loon E, Senev A, Lerut E, Coemans M, Callemeyn J, Van Keer JM, Daniëls L, Kuypers D, Sprangers B, Emonds M-P and Naesens M (2020) 'Assessing the complex causes of kidney allograft loss', Transplantation, 104(12):2557–2566, doi:10.1097/tp.0000000000003192.
-
Wyld MLR, Mata NLDL, Viecelli A, Swaminathan R, O'Sullivan KM, O'Lone E, Rowlandson M, Francis A, Wyburn K and Webster AC (2022) 'Sex-based differences in risk factors and complications of chronic kidney disease', Seminars in Nephrology, 42(2):153–169, doi:10.1016/j.semnephrol.2022.04.006.
-
Yadav UN, Davis JM, Bennett-Brook K, Coombes J, Wyber R and Pearson O (2024) 'A rapid review to inform the policy and practice for the implementation of chronic disease prevention and management programs for Aboriginal and Torres Strait Islander people in primary care', Health Research Policy and Systems, 22:34, doi:10.1186/s12961-024-01121-x.
-
Yadav UN, Thottunkal S, Agostino J, Sinka V, Wyber R, Hammond B, Butler DC, Belfrage M, Freeman K, Passey M, Walke E, Smith M, Jones B, Lovett R and Douglas KA (2025) 'What influences the implementation of health checks in the prevention and early detection of chronic diseases among Aboriginal and Torres Strait Islander people in Australian primary health care? Findings from an evidence mapping review', Health Research Policy and Systems, 23:70, doi:10.1186/s12961-025-01325-9.
-
Zheng C, Teixeira-Pinto A, Hughes JT, Sinka V, van Zwieten A, Lim WH and Wong G (2022) 'Acute rejection, overall graft loss, and infection-related deaths after kidney transplantation in Indigenous Australians', Kidney International Reports, 7(11):2495–2504, doi:10.1016/j.ekir.2022.08.027.

