Key messages
Why is it important?
Hospitalisation rates for Aboriginal and Torres Strait Islander (First Nations) people are influenced by access to primary care and other health-care services, the burden of disease in the population, and the social determinants and risk factors that drive or exacerbate ill health. Systemic inequities affect the accessibility, affordability and appropriateness of health care.
Hospitalisation rates for First Nations people are significantly higher than for non-Indigenous Australians for conditions like kidney disease, digestive system diseases, respiratory illness, and diabetes, yet access to culturally safe, continuous, and affordable primary care remains limited. Despite experiencing poorer health outcomes, First Nations people often underutilise health services, highlighting gaps in equity and service delivery. Barriers such as cost, transport, communication, and continuity of care contribute to preventable hospitalisations.
Data findings
- The hospitalisation rate was higher for First Nations females than First Nations males between the age groups 15–24 to 45–54 and was otherwise similar or slightly higher for First Nations males.
- For First Nations children aged 0–4, respiratory diseases were the leading reason for hospitalisation (22% of hospitalisations). For First Nations children aged 5–14, injury and poisoning was the leading reason for hospitalisation (18% of hospitalisations).
- Between July 2021 and June 2023, across states and territories, the highest hospitalisation rate for First Nations people was in the Northern Territory (545 per 1,000 population) and the lowest was in New South Wales (283 per 1,000).
- Between July 2021 and June 2023, hospitalisation rates for First Nations people (excluding dialysis) were highest in Remote and very remote areas, at 1.5 times the rate in non-remote areas.
- Between July 2021 and June 2023, after adjusting for differences in the age structure between the two populations, First Nations people were hospitalised at 2.2 times the rate of non-Indigenous Australians when care involving dialysis was included, and 1.3 times the rate of non-Indigenous Australians when dialysis was excluded.
- After adjusting for differences in the age structure across the period, the hospitalisation rate (excluding dialysis) for First Nations people increased by an average of 11 hospitalisations per 1,000 population each year from 2016–17 to 2022–23.
Research and evaluation findings
- Primary health care can play a pivotal role in helping to reduce health inequalities and hospitalisation rates as well as providing critical continuity of care and follow-up care. Research shows that optimal primary health care access in the Northern Territory has reduced hospitalisation significantly. Primary care in remote First Nations communities was associated with cost-savings to public hospitals and health benefits to individual patients.
- Dialysis is a major driver of the high hospitalisation rates for First Nations people. Innovative solutions to improve access to dialysis in remote areas can improve outcomes for patients.
- Medication-related hospitalisations are preventable; research has shown over one-third of cardiovascular disease hospitalisations were linked to inadequate medication management.
- Multimorbidity is more frequent among First Nations people, contributing to higher hospitalisation and death rates.
Implications
Disproportionately high hospitalisation rates among First Nations people highlight the urgent need for culturally safe, accessible, and integrated health care. Expanding the reach of Aboriginal Community Controlled Health Organisations, increasing disease screening and early detection, and improving access to specialist care are critical to reducing preventable hospital admissions. Improving the appropriateness of the acute care system for First Nations people, and tackling social determinants and risk factors are essential to improving health outcomes.
Why is it important?
Hospitalisation rates show how often people in a population experience serious illnesses or conditions that require hospital care, as well as how hospital services are accessed and used. However, these rates do not directly reflect the prevalence of disease in the population. Hospitalisation rates are influenced by access to primary care and other healthcare services, and provide insights into both health care need and system performance (see measure 3.07 Selected potentially preventable hospital admissions).
High rates of hospitalisation for preventable conditions, such as diabetes complications and respiratory disease, may indicate barriers to appropriate, timely and effective primary care, including availability, accessibility, affordability, and cultural safety. However, in some cases, higher hospitalisation rates may reflect appropriate service use in response to greater need (Beckwith and Glover 2018).
For Aboriginal and Torres Strait Islander (First Nations) people, hospitalisation rates for conditions such as kidney disease, digestive system diseases, respiratory disease, and type 2 diabetes remain significantly higher than for non-Indigenous Australians, highlighting the ongoing need to ensure equitable access to healthcare (see measure 1.04 Respiratory disease, 1.09 Diabetes, and 1.10 Kidney disease). These conditions and other chronic diseases are often associated with social determinants of health, including inadequate housing, education, income and employment, limited access to healthcare services, and higher rates of risk factors such as smoking and poor diet (see measure 2.01 Housing, 2.15 Tobacco use, and 2.19 Dietary behaviour). Addressing these underlying determinants and risk factors is critical to improving health outcomes and achieving health equity for First Nations communities.
Hospitalisation data feature across multiple measures within the Aboriginal and Torres Strait Islander Health Performance Framework. This measure provides an overview of hospital admissions for First Nations people to serve as an introduction to other measures which provide more detail on the interaction between First Nations people and the hospital sector. Tier 3 measures on health system performance (such as measure 3.06 Access to hospital procedures, measure 3.07 Selected potentially preventable hospital admissions, measure 3.09 Self-discharge from hospital and measure 3.14 Access to services compared with need) provide further insight into First Nations people’s access to the hospital sector, experience within the sector and barriers to accessing specific health and hospital services.
Hospitalisation trends also reflect broader systemic issues, including the need for secondary care of chronic conditions, environmental factors, and gaps in primary healthcare. Overcrowding, remoteness, food insecurity, and limited access to culturally safe and continuous care contribute to higher rates of potentially preventable hospitalisations. These barriers are examined in Tier 3 measures of health system performance and point to the need for integrated, cross-sectoral policy responses to reduce avoidable admissions and improve healthcare access for First Nations people.
Interpretation of the gap in hospitalisation rates between First Nations people and non-Indigenous Australians should be treated with caution. For hospitalisation data, this gap can be useful in understanding and comparing access to services. However, unlike many health outcomes, this gap does not necessarily reflect a disparity that needs to be closed in the short to medium term, particularly if it reflects where services are better addressing previously unmet need for care.
Experiences of discrimination and racism in the health system contribute to mistrust, hospital avoidance, and delayed care-seeking among First Nations people, and constitute significant barriers to accessing care (Australians for Native Title and Reconciliation 2021; AIHW 2023). Ensuring culturally safe and responsive hospital services is essential to improving health outcomes and reducing preventable hospitalisations. Other barriers include, but are not limited to, cost, transport, communication pathways, continuity of care, service infrastructure, and information capability. Self-discharge rates are disproportionately high among First Nations patients, often reflecting issues such as systemic racism, inadequate cultural safety, poor communication, and past negative healthcare experiences (see measure 3.09 Self-discharge from hospital).
The National Agreement on Closing the Gap (National Agreement) aims to ensure First Nations people enjoy long and healthy lives, with Target 1 aiming to close the life expectancy gap by 2031. Hospitalisation data provides important insights into the health burden and issues with access to care for First Nations people, which influence life expectancy. Addressing disparities in hospitalisation rates, preventable hospital admissions, and barriers to culturally safe care will be critical to achieving this target.
In line with this, the National Aboriginal and Torres Strait Islander Health Plan 2021–2031 (the Health Plan) provides the framework for progress towards the Closing the Gap health targets, emphasising prevention, early intervention, and integrated care systems. It calls for mainstream services to address racism, provide culturally safe care, be centred in culture and be accountable to First Nations people and communities.
Both the National Agreement and the Health Plan are discussed further in the Implications section of this measure.
Data findings
In Australia, hospital services are provided by both public and private hospitals. Hospitals provide a range of services for admitted patients such as elective care, maternity services and medical and surgical services. Non-admitted patient services are mostly located in public hospitals and include emergency department services and outpatient clinics (AIHW 2025a).
Between July 2021 and June 2023, there were 1,276,527 hospitalisations for First Nations people (including dialysis) – an average of about 638,000 hospitalisations annually – corresponding to a rate of 637 per 1,000 population (Table D1.02.5). Excluding dialysis, there were 736,105 hospitalisations for First Nations people, a rate of 367 per 1,000 (Table D1.02.1).
Top reasons for total hospitalisations
Between July 2021 and June 2023, the leading cause of hospitalisation was care involving dialysis (540,422 hospitalisations), which accounted for 42% of all hospitalisations for First Nations people (compared with 13% for non-Indigenous Australians) (Table D1.02.5).
Dialysis is an artificial way to remove waste and excess water from the blood and regulate safe levels of circulating agents in the body, a function usually performed by the kidneys. It is most often provided to treat chronic kidney failure but is sometimes needed in cases of acute kidney failure, where the kidneys have been temporarily damaged due to illness or injury. Most people undergoing dialysis attend three sessions per week (ANZDATA Registry 2021: Table 4.9). See also measure 1.10 Kidney disease.
Among First Nations people, after care involving dialysis, the next four leading reasons for hospitalisation were:
- Injury and poisoning (83,503, 6.5% of all hospitalisations for First Nations people, or 11% of hospitalisations excluding dialysis): for example, falls, exposure to inanimate mechanical forces and assault. See also measure 1.03 Injury and poisoning.
- Symptoms, signs and abnormal findings not elsewhere classified (80,229, 6.3% of all hospitalisations or 11% excluding dialysis): this includes symptoms such as abnormalities of heartbeat, abnormalities of breathing, chest pain, nausea and vomiting, headache, and convulsions that are not attributable to a specific diagnosis based on the information available at the time of the care.
- Pregnancy, childbirth and the puerperium (68,166, 5.3% of all hospitalisations or 9.3% excluding dialysis).
- Digestive system diseases (66,842, 5.2% of all hospitalisations or 9.1% excluding dialysis) (Table D1.02.5, Figure 1.02.1).
Figure 1.02.1: Hospitalisations for First Nations people, by principal diagnosis, Australia, July 2021 to June 2023
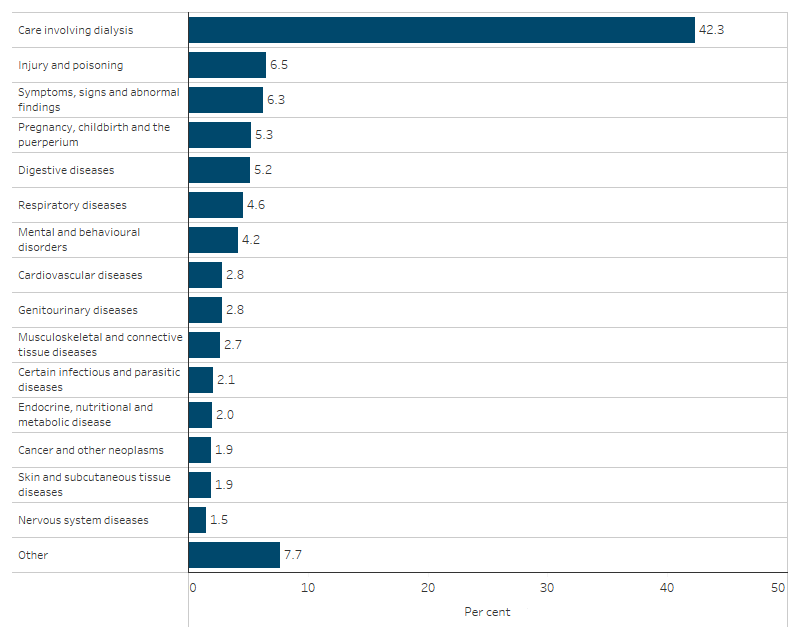
Note: See Table D1.02.5 for the ICD-10-AM codes included in each principal diagnosis grouping.
Source: Table D1.02.5. AIHW analysis of National Hospital Morbidity Database.
Hospitalisation by sex and age
Between July 2021 and June 2023, 58% of total hospitalisations among First Nations people were for females (428,030 hospitalisations, excluding dialysis). First Nations females were hospitalised at 1.4 times the rate of First Nations males (429 and 306 per 1,000, respectively).
The hospitalisation rate was higher for First Nations females than First Nations males in all jurisdictions. The largest relative difference was in the Northern Territory and the Australian Capital Territory, where the rates for females were 1.5 times the rates for males (Table D1.02.1).
The hospitalisation rate was higher for First Nations females than First Nations males between the age groups 15–24 to 45–54 and was otherwise similar or slightly higher for First Nations males (Table D1.02.2).
First Nations children aged 0–4 had a hospitalisation rate of 303 hospitalisations per 1,000 population in the two-year period from July 2021 to June 2023. The hospitalisation rate was lower among those aged 5–14 (105 per 1,000), then increased with age and was highest for those aged 65 and over (911 per 1,000) (Table D1.02.2, Figure 1.02.2).
Figure 1.02.2: Age-specific hospitalisation rates (excluding dialysis), by Indigenous status, Australia, July 2021 to June 2023
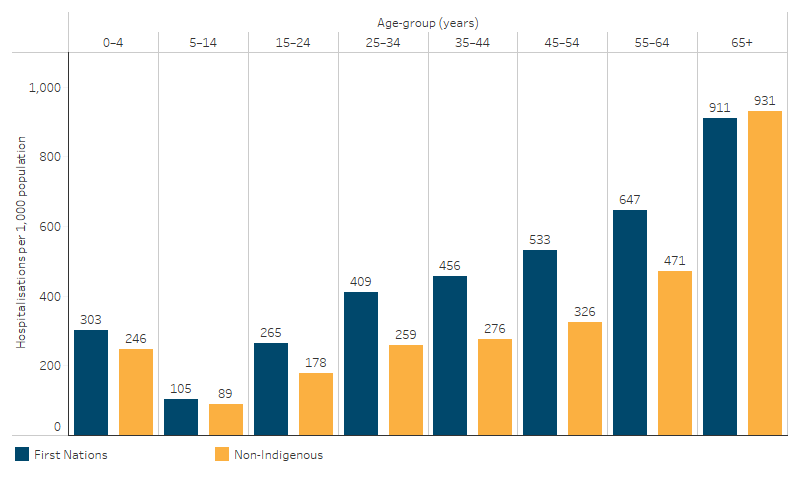
Source: Table D1.02.2. AIHW analysis of National Hospital Morbidity Database.
Looking at the top reasons for hospitalisation (excluding dialysis) by age group:
- Respiratory diseases (22%) were the leading reason for hospitalisation for First Nations people aged 0–4, followed by symptoms, signs and abnormal clinical and laboratory findings not elsewhere classified (11%), and certain infectious and parasitic diseases (8.8%).
- Among First Nations children aged 5–14, injury and poisoning was the leading reason for hospitalisation (18%), followed by digestive system diseases (14%), and respiratory diseases (12%).
- For First Nations people aged 15–24 and 25–44, pregnancy, childbirth and the puerperium was the leading reason for hospitalisation (27% and 18%, respectively), followed by injury and poisoning (16% and 13%, respectively).
- Between the ages of 45–54 and 55–64, the leading reason for hospitalisation was symptoms, signs and abnormal clinical and laboratory findings not elsewhere classified (13% and 12%, respectively), followed by digestive system diseases (11% and 10%, respectively).
- Among First Nations people aged 65 and over, the leading reason for hospitalisations were symptoms, signs and abnormal clinical and laboratory findings not elsewhere classified and cardiovascular diseases (both 10%), followed by respiratory diseases (9.2%) (Table D1.02.8).
Hospitalisation by state and territory
Note that some jurisdictions have slightly different approaches to the collection of the standard Indigenous status question and categories in their hospital collections. As such comparisons by jurisdiction should be interpreted with caution. See Data sources and quality for additional information on this data collection.
Between July 2021 and June 2023, across states and territories, the highest hospitalisation rate for First Nations people was in the Northern Territory (545 per 1,000) followed by Queensland (434 per 1,000). The hospitalisation rate in the Northern Territory was 1.9 times the rate in New South Wales (283 per 1,000), where the rate was the lowest (Table D1.02.1, Figure 1.02.3).
Figure 1.02.3: Hospitalisation rates (excluding dialysis) for First Nations people, by state and territory, July 2021 to June 2023
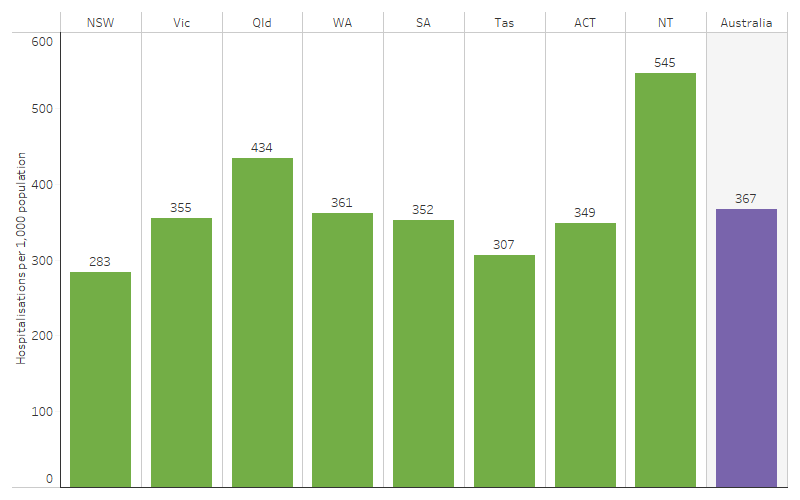
Source: Table D1.02.1. AIHW analysis of National Hospital Morbidity Database.
Hospitalisation by remoteness
Between July 2021 and June 2023, the hospitalisation rate for First Nations people in remote areas (Remote and Very remote areas combined) was 1.5 times the rate in non-remote areas (Major cities, Inner regional and Outer regional areas combined) (507 per 1,000 compared with 337 per 1,000) (Table D1.02.13, Figure 1.02.4). This is likely due to a combination of higher disease burden, poorer determinants of health (including housing and other socioeconomic factors) and reduced access to primary care.
This pattern was the same in most states and territories (ranging from 1.0 to 1.7 times as high in remote areas as non-remote areas) (Table D1.02.13).
Figure 1.02.4: Hospitalisation rates (excluding dialysis) for First Nations people, by remoteness, Australia, July 2021 to June 2023
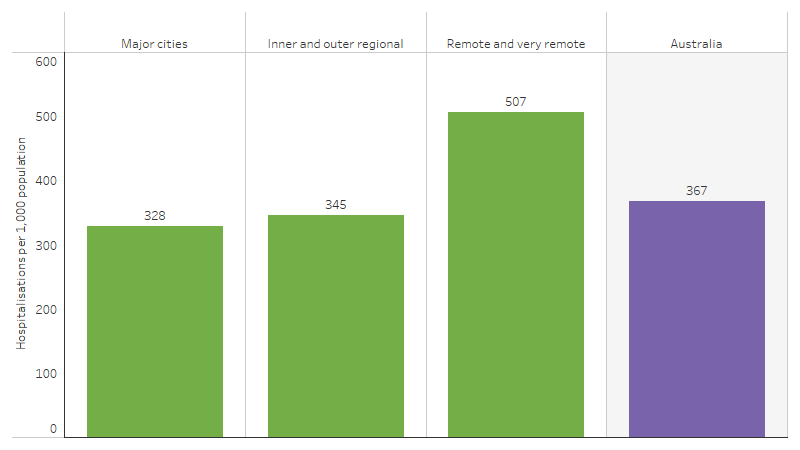
Source: Table D1.02.3. AIHW analysis of National Hospital Morbidity Database.
Same-day and overnight hospitalisation
Between July 2021 and June 2023, there were 835,173 same-day hospital separations (including dialysis) for First Nations people, corresponding to a rate of 417 per 1,000 population. Care involving dialysis was the most common reason for same-day separations, accounting for about two-thirds of these separations (65%, or 539,234) (based on principal diagnosis). The rate of same-day separations among First Nations people excluding dialysis was 148 per 1,000.
Based on principal diagnosis, symptoms, signs and abnormal clinical and laboratory findings not elsewhere classified was the next leading reason for same-day hospital separations for First Nations people (a rate of 20 per 1,000; 4.7% of same-day separations), followed by digestive system diseases (16 per 1,000; 3.9%) and injury, poisoning and other external causes (16 per 1,000; 3.8%) (Table D1.02.11).
Between July 2021 and June 2023, there were 441,354 overnight hospital separations (including dialysis) for First Nations people, a rate of 220 per 1,000. Dialysis accounted for a smaller proportion of overnight separations for First Nations people (0.3%, 1,188 hospitalisations) than same-day separations (65%).
The top reason for overnight hospital separations for First Nations people was injury and poisoning (26 per 1,000 population; 12% of overnight separations), followed by respiratory diseases (24 per 1,000; 11%).
Pregnancy, childbirth and the puerperium was also a top reason for overnight hospital separations for First Nations women (44 per 1,000 female population; 10% of total overnight separations for First Nations people) (Table D1.02.12).
Comparisons with non-Indigenous Australians
Variations in hospitalisation rates between First Nations people and non-Indigenous Australians provide important insights into health needs, patterns of care use and service access, but should be interpreted with caution to ensure context and underlying factors are considered. Higher hospitalisation rates in one population group compared to another may reflect a greater burden of disease and poor access to primary and secondary healthcare, however they may also reflect better availability and access to hospital care.
Between July 2021 and June 2023, after adjusting for differences in the age structure between the two populations, First Nations people were hospitalised at:
- 2.2 times the rate of non-Indigenous Australians when care involving dialysis was included
- 1.3 times the rate of non-Indigenous Australians when dialysis was excluded
- 9.0 times the rate of non-Indigenous Australians for care involving dialysis (Table D1.02.5).
The difference in rates between the two populations, excluding dialysis, were similar for males and females (a ratio of 1.3 and 1.4 respectively) (Table D1.02.2).
Excluding dialysis, for the age group 65 and over, hospitalisation rates were similar between the two populations (a ratio of 1.0). For other age groups, rates for First Nations people ranged from 1.2 times the rate for non-Indigenous Australians (for those aged under 15) to 1.7 times as high (for those aged 35–44) (Table D1.02.2, Figure 1.02.2).
After adjusting for differences in age structure between the two populations, the relative gap in hospitalisation rates between First Nations and non-Indigenous Australians (excluding dialysis):
- ranged across jurisdictions from a ratio of 1.1 in Tasmania to a ratio of 1.8 in the Northern Territory (Table D1.02.1)
- ranged by remoteness areas from a ratio of 1.3 in non-remote areas (Major cities, Inner regional and Outer regional areas combined), to a ratio of 1.9 in remote areas (Remote and Very remote areas combined) (Table D1.02.13).
The age-standardised rate of same-day hospital separations among First Nations people (including dialysis) was 2.5 times the rate for non-Indigenous Australians. However, excluding dialysis, the rate for First Nations people was lower: 0.9 times the rate for non-Indigenous Australians. By principal diagnosis, the age-standardised rate of same-day separations was lower for First Nations people for cancer and other neoplasms (rate ratio of 0.6), digestive diseases (rate ratio of 0.7), musculoskeletal system and connective tissue diseases, and nervous system diseases (rate ratio of 0.8 for both) (Table D1.02.11).
The leading principal diagnosis for same-day hospital separations was dialysis for both First Nations people and non-Indigenous Australians, though it accounted for a higher proportion of separations for First Nations people (accounting for 65% of same-day separations, compared with 20% for non-Indigenous Australians). Dialysis also had the largest relative difference in same-day separations rates between the two populations, with the age-standardised rate for First Nations people 9.1 times that of non-Indigenous Australians. This was followed by pregnancy and childbirth and injury and poisoning (rate ratio of 1.6 for both) (Table D1.02.11).
Overnight hospital separations (including dialysis) for First Nations people were 1.9 times the rate for non-Indigenous Australians, after adjusting for age. The largest relative difference in overnight separations between the two populations was for skin and subcutaneous tissue diseases (rate ratio of 3.3), followed by endocrine, nutritional and metabolic diseases (a ratio of 3.1) and mental and behavioural disorders (rate ratio of 2.7) (Table D1.02.12).
Changes in hospitalisations over time
To describe trends in hospital data, linear regression has been used to calculate the per cent change over time. This means that information from all years of the specified time period are used, rather than only the first and last points in the series (see Statistical terms and methods).
From 2016–17 to 2022–23, the number of hospitalisations for First Nations people increased by around 155,000 – from 501,317 to 656,760. After adjusting for differences in the age structure across the period, the hospitalisation rate increased from 783 to 874 per 1,000 population. Based on linear regression, this corresponds to a 10% increase over the period, or an average increase of 14 hospitalisations per 1,000 population each year (Table D1.02.7).
After adjusting for differences in the age structure across the period, the hospitalisation rate (excluding dialysis) for First Nations people increased from 398 to 468 per 1,000 population – an increase of 16% over the period, or an average increase of 11 hospitalisations per 1,000 population each year (Table D1.02.4).
Excluding dialysis, the causes with the highest average increase in age-standardised hospitalisation rates for First Nations people per year were:
- pregnancy, childbirth and the puerperium – from 55 to 65 per 1,000 (female) population, or an average increase of 1.7 hospitalisations per 1,000 (female) population each year
- symptoms, signs and abnormal clinical and laboratory findings, not elsewhere classified – from 41 to 49 per 1,000 population, or an average increase of 1.6 hospitalisations per 1,000 population each year
- digestive diseases – from 35 to 43 per 1,000 population, or an average increase of 1.3 hospitalisations per 1,000 population each year (Table D1.02.7).
From 2016–17 to 2022–23, after adjusting for differences in the age structure between the two populations, the hospitalisation rate (excluding dialysis) increased by 16% for First Nations people and decreased by 5% for non-Indigenous Australians. This resulted in a widening of the rate difference (absolute gap) (from 43 per 1,000 in 2016–17 to 125 per 1,000 in 2022–23) and the ratio of the hospitalisation rate for First Nations people to the rate for non-Indigenous Australians (from a ratio of 1.1 in 2016–17 to 1.4 in 2022–23) (Table D1.02.4, Figure 1.02.5).
Figure 1.02.5: Trends in age-standardised hospitalisation rates (excluding dialysis), by Indigenous status, Australia, 2016–17 to 2022–2023
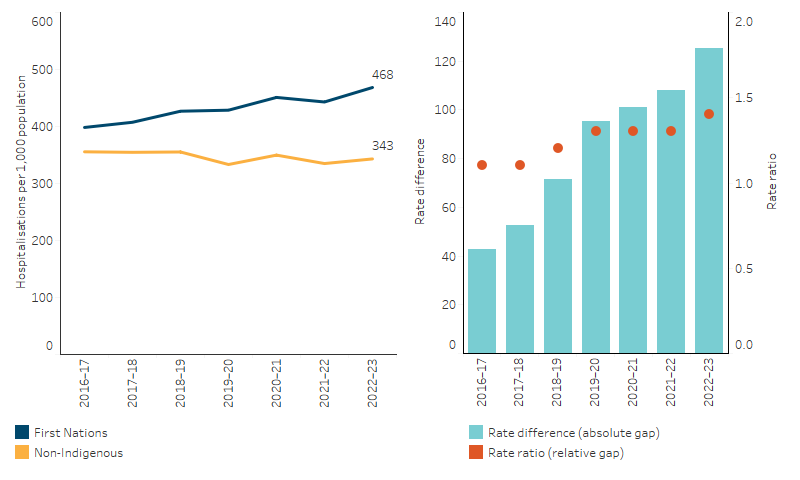
Note: Rate difference is the age-standardised rate (per 1,000) for First Nations people minus the age-standardised rate (per 1,000) for non-Indigenous Australians. Rate ratio is the age-standardised rate for First Nations people divided by the age-standardised rate for non-Indigenous Australians.
Source: Table D1.02.4. AIHW analysis of National Hospital Morbidity Database.
Research and evaluation findings
Primary health care can play a pivotal role in closing the gap in First Nations health and reducing health inequalities and hospitalisation rates. Aboriginal Community Controlled Health Organisations (ACCHOs) and other First Nations-specific primary health care initiatives deliver culturally safe primary health care across Australia. However, many First Nations people access health care through mainstream services, either by necessity or by choice (DoH 2017). While ACCHOs are a preferred source of culturally safe care, their availability is limited in many areas due to uneven geographic distribution, funding constraints, and workforce shortages. In urban and regional locations, mainstream general practices are often more accessible than First Nations-specific services, leaving many First Nations people with no choice but to access mainstream care. Systemic barriers – such as Medicare rules that prevent mobile clinics from claiming rebates – further restrict the ability of ACCHOs to deliver flexible, community-based services.
These limitations contribute to reduced access to preferred care and reinforce reliance on mainstream providers, even when they may not meet needs for cultural safety or comprehensive healthcare (AIHW 2025b). Access to health care is shaped not only by the availability and affordability of services but also by organisational, social, and cultural factors that influence whether people can perceive, seek, reach, pay for, and engage with care. International evidence shows that even when services are clinically sound and subsidised, failing to acknowledge the cultural values of Indigenous communities can create resistance and limit engagement (George et al. 2020). For First Nations people in Australia, cultural security is essential, as its absence can cause emotional and physical discomfort that reduces service use and contributes to poorer health outcomes (see 3.14 Access to services compared with need).
Research highlights the critical role of primary health care in preventing hospitalisations. In the Northern Territory, optimal primary health care access has reduced preventable hospitalisations, particularly for chronic conditions such as diabetes and chronic kidney disease (Zhao et al. 2013). Evidence suggests that access to primary health care tailored to the needs of, and owned or managed by, First Nations people can significantly improve access and outcomes (Davy et al. 2016). Primary care in remote First Nations communities has also been associated with cost-savings for public hospitals and health benefits for individual patients (Zhao et al. 2014).
Comprehensive, culturally safe primary health care in remote communities plays a vital role not only in preventing hospitalisations but also in providing life-long follow-up care for individuals with chronic conditions or post-surgical care needs – such as cardiac care. However, the ability of ACCHOs to deliver this ongoing care is heavily dependent on adequate and sustained resourcing. The National Aboriginal Community Controlled Health Organisation (NACCHO) Core Services and Outcomes Framework highlights that underinvestment in infrastructure, workforce shortages, and fragmented funding models can undermine the capacity of ACCHOs to provide holistic, continuous care tailored to community needs. Without sufficient support, remote ACCHOs struggle to maintain the long-term care pathways essential for managing complex conditions and improving health outcomes over time (NACCHO 2021).
A 2024 linked data study found that First Nations people continue to experience higher rates of cardiovascular disease (CVD) hospitalisations, often presenting with acute events more than a decade earlier than non-Indigenous patients. Among First Nations patients admitted for CVD at major Melbourne hospitals between 2011 and 2019, the median age of admission was 60.1 years compared to 71.3 years for non-Indigenous Australians. The study also found that over half of First Nations CVD patients lived in the most socioeconomically disadvantaged areas, highlighting the significant impact of social determinants on high hospitalisation rates (Price et al. 2024).
Preventable medication-related hospitalisations are another significant issue in First Nations cardiovascular health. A retrospective cohort study found that among 31,472 CVD-related hospitalisations for First Nations people in Queensland between 2013 and 2017, over one-third were potentially preventable due to underuse or misuse of medications. More than 74% of myocardial infarction hospitalisations were in patients who were not receiving guideline-recommended treatment. The study shows that inadequate medication management arises from both clinical gaps, such as not prescribing or not using recommended therapies and the use of medicines that can worsen certain conditions, as well as systemic barriers including inequitable access to culturally safe medication reviews, poor monitoring, cost and literacy issues, and limited access to primary care in regional areas. These factors collectively contributed to the high proportion of preventable hospitalisations, including the 62% of ischaemic event hospitalisations in patients with diabetes. Recent research highlights that medication safety can be improved for First Nations people through culturally tailored and holistic approaches. Moreover, emerging primary care strategies must prioritise inclusion of those people with the greatest health needs to reduce preventable hospitalisations and deaths (Spinks et al. 2025).
Across Australia, there is a growing need for out-of-hospital palliative and chronic disease care. The high prevalence of chronic diseases and limited access to primary services among First Nations people have resulted in high hospitalisation rates. In the Northern Territory, the establishment of a flexible, community-based, and culturally safe palliative and chronic disease respite facility in Alice Springs led to a reduction in local hospital admissions (Carey et al. 2017).
Dialysis is the leading cause of hospitalisation for First Nations people, occurring at 9 times the rate of non-Indigenous Australians. Evidence from the Northern Territory shows that missing two or more dialysis treatments per month was associated with a two-fold increase in hospital admissions and more than three-fold increase in emergency department presentations. Patients on dialysis in remote areas had significantly lower hospitalisation rates compared to those who relocated to urban centres for treatment (Gorham et al. 2022). In South Australia, a pilot model at Kanggawodli – a culturally safe, urban hostel-based dialysis service – demonstrated improved attendance, reduced missed treatment, and enhanced patients’ wellbeing. The model allowed flexible scheduling, wrap-around allied health support, and family-centred care, aligning with First Nations ways of being and improving health literacy and engagement (Shearing et al. 2023).
A Northern Territory study on bronchiectasis, a chronic lung condition, found that 87% of adult First Nations patients diagnosed with bronchiectasis had at least one respiratory-related hospital admission between 2011 and 2020, averaging one admission per year. Co-morbid chronic obstructive pulmonary disease (COPD) was common, affecting 88% of hospitalised bronchiectasis patients, and nearly one-third required the Intensive Care Unit at some point. The study highlights the heavy burden of respiratory infections and chronic lung disease requiring hospitalisation for First Nations people (Howarth et al. 2024).
In 2021–22, hospitalisation rates for Acute Rheumatic Fever (ARF) and Rheumatic Heart Disease (RHD) were 6.2 times higher for First Nations people than for non-Indigenous Australians, and 8.5 times higher in Remote and very remote areas compared to Major Cities. Death rates were 5.9 times higher overall for First Nations people, and up to 26 times higher among adults aged 25–64 years (AIHW 2024d). In an average year, approximately 125 RHD-related cardiothoracic surgeries are performed across Queensland, Western Australia, South Australia, and the Northern Territory. These procedures are conducted exclusively in tertiary referral hospitals. However, First Nations patients experience higher rates of early discharge and post-operative complications, particularly those from remote regions (Casey 2023). Long-term survival following valve replacement surgery for RHD among First Nations patients in the Northern Territory has not improved since 1964. The 10-year survival rate remains at 62%, with outcomes significantly affected by comorbidities such as chronic kidney disease, coronary artery disease, and pulmonary hypertension (Doran et al. 2023).
A nationwide study examined hospitalisation patterns and costs associated with ARF and RHD among Australians aged under 65 years, with a particular focus on First Nations people. Using linked hospital and RHD register data from five states (2012–2017), the study found disproportionately high rates of ARF and RHD-related hospitalisations among First Nations people. First Nations people comprised 86.3% of child (<16 years) hospitalisations and 44.8% of adult (aged 16–64) hospitalisations for ARF/RHD or associated complications. Hospitalisation rates increased annually, contributing to a total health care cost of $130.6 million over five years. First Nations patients were more likely to be from remote areas, require emergency hospitalisation, and undergo air ambulance transfers (Stacey et al. 2024).
A 2024 data-linkage study of 21,189 children born in the Northern Territory found that First Nations children had an injury hospitalisation rate 28.6% higher than non-Indigenous children, with falls, burns, and accidental poisonings being the most common causes. Children living in remote and socioeconomically disadvantaged areas had the highest risk of injury hospitalisation (Su et al. 2024).
Although hospitalisation rates are higher for First Nations people than for non-Indigenous Australians, they do not access health services to the level expected given their experience of poorer health outcomes (Alford 2015). This underutilisation is partly due to an inadequate supply of First Nations-specific primary health care services and barriers to accessing mainstream health services, including cost, location, and cultural safety concerns (AIHW 2023). Many First Nations people prefer First Nations-specific services, such as ACCHOs, which provide culturally safe, community-driven care addressing both immediate health needs and broader structural determinants of health (Pearson et al. 2020). Despite this preference, mainstream government expenditure still dominates health funding for First Nations people. Government expenditure is not commensurate with the substantially greater and more complex health needs of First Nations people, and the proportion of health funding allocated to First Nations people has failed to keep pace with population growth and disease burden (Alford 2015). First Nations people experience a disease burden 2.3 times that of other Australians, which equates to 2.03 times the cost of service delivery (NACCHO 2025). Reflecting this mismatch between need and funding, it’s estimated that the gap in health expenditure is approximately $4.4 billion per year (Equity Economics and NACCHO 2022). See measure 3.21 Expenditure on Aboriginal and Torres Strait Islander health compared to need.
Elevated rates of multimorbidity among the First Nations population is closely linked to social determinants of health. Factors such as socioeconomic disadvantage, limited access to culturally appropriate healthcare, and the enduring impacts of colonisation – including intergenerational trauma and systemic racism – continue to influence health outcomes (Carman et al. 2022). Several studies have linked multimorbidity (having two or more chronic conditions) to an increased use of health services, particularly in hospitalisation (Gruneir et al. 2016). It is therefore consistent that hospitalisation rates are higher among First Nations people compared with non-Indigenous Australians, given that prevalence of multimorbidity is higher for First Nations people than non-Indigenous Australians (Hussain et al. 2018). A recent study found that approximately 21% of First Nations people experience multimorbidity, which significantly impacts their health-related quality of life (Keramat et al. 2024).
Another study using New South Wales hospital and death data found that multimorbidity is approximately 2.5 times more frequent among First Nations people compared to non-Indigenous Australians, after adjusting for age, sex, and socioeconomic status. This difference accounted for a large proportion of the difference in death rates between the two groups of patients. The prevalence of multimorbidity was higher among First Nations people in all age groups. In younger age groups this was because of the higher prevalence of mental health conditions (for example, alcohol or drug use disorders, depression, psychoses), while in the older age group (over 60 years) it was because of physical health conditions (Broe and Radford 2018).
Lower access to hospitals and health services can lead to poorer health outcomes. Findings of a project that examined spatial variation in First Nations women’s access to hospitals with public birthing services and three other types of maternal health services across Australia found that the lowest levels of access to maternal health services are in remote areas. Poorer access to maternal health services is associated with higher rates of pre-term birth and low birthweight (AIHW 2017). Additionally, culturally safe maternity services, such as those provided by ACCHOs, are crucial for improving health outcomes for First Nations mothers and babies (AIHW 2024c).
Implications
Despite higher hospitalisation rates, health services are underutilised by First Nations people due to inadequate supply and inequitable access to primary care. The health system needs to effectively address the high burden of disease and complex health needs of First Nations people, underscoring the necessity for broader access improvements. This points to a broader issue of access to care, explored further in measure 3.14 Access to services compared with need.
Given the high proportion of hospitalisations for First Nations people requiring dialysis, more attention should be given to alternatives that can provide dialysis outside of the hospital system, such as mobile dialysis units. Initiatives like the South Australian Mobile Dialysis Truck and Purple House’s mobile units have shown success in providing treatment closer to home, improving social and emotional wellbeing (Conway et al. 2018; Purple House). The Australian Government is improving access to kidney care for First Nations people by expanding dialysis services in remote communities through the Better Renal Services for First Nations Peoples initiative. The program funds new dialysis units in high-need areas of Queensland, Western Australia and the Northern Territory, reducing travel burdens and allowing patients to receive treatment while remaining on Country (DoHAC 2024a; DoHAC 2024b; Morse 2024) (see measure 1.10 Kidney disease).
The 2020–25 Addendum to the National Health Reform Agreement (NHRA), an agreement between the Australian Government and all state and territory governments, commits to improving health outcomes for Australians, by providing better coordinated and joined up care in the community, and ensuring the future sustainability of Australia’s health system. Through this agreement, the Australian Government contributes funds to the states and territories for public hospital services. The NRHA’s Long-term Health Reforms Roadmap commits the Australian and state and territory governments to working in partnership with First Nations communities to co-design approaches tailored to their needs. The Roadmap acknowledges Aboriginal Community Controlled Health Organisations (ACCHOs) as key partners in implementing the reforms.
Expanding access to culturally appropriate primary health care is essential. ACCHOs are a leading model of comprehensive primary health care, integrating cultural safety, multidisciplinary care, chronic disease management, and an understanding of the social determinants of health into their service delivery. Priority Reform Two of the National Agreement on Closing the Gap (National Agreement) emphasises building the community-controlled sector to deliver services that support Closing the Gap. The implication being that strengthening the community-controlled health sector can lead to earlier intervention and treatment, thereby reducing the high (preventable) hospitalisation rates among First Nations people. ACCHOs are funded under the Australian Government’s Indigenous Australians’ Health Programme (IAHP) and have demonstrated stronger engagement with First Nations patients compared to mainstream services, supporting early intervention and continuity of care (AIHW 2024b).
The Australian Government also funds Primary Health Networks (PHNs) to support the coordination and integration of local health care services, including collaboration with Local Hospital Networks. PHNs are required to increase cultural awareness and competency through quality improvement activities and partnerships with general practices. However, national monitoring indicates that cultural safety in mainstream health services – including PHNs – is not consistently measured, and significant data gaps remain regarding the experiences of First Nations healthcare users in these settings (AIHW 2023).
Incentive-based programs also support culturally responsive care. The Practice Incentives Program – Indigenous Health Incentive provides payments to general practices, Aboriginal Medical Services, and ACCHOs to improve chronic disease management for First Nations people. The program aims to prevent, identify, and manage chronic conditions contributing to the health gap.
The Integrated Team Care (ITC) program supports First Nations people with complex chronic conditions by improving access to coordinated and culturally appropriate health care. Also funded under the IAHP, the initiative addresses the high burden of chronic disease – such as heart disease and diabetes – by providing individualised care coordination, linking patients to appropriate services, and reducing barriers to timely treatment. The program funds First Nations health project officers, outreach workers, and care coordinators, who work together to ensure patients receive the right care when needed, improve communication between health services, and enhance culturally safe service delivery. By fostering collaboration between mainstream and First Nations health providers, the ITC program strengthens chronic disease management, reduces preventable hospitalisations, and helps First Nations people navigate complex care pathways more effectively (DHDA 2025a).
The Services Australia Indigenous Access Line (1800 556 955) provides culturally trained support to First Nations people needing assistance with Medicare services and payments. This service is also available to First Nations health workers, helping to facilitate access to essential healthcare support and reducing barriers that may contribute to preventable hospitalisations (DHDA 2025b).
Addressing social determinants of health, such as overcrowded housing and environmental factors, is crucial for reducing the high rates of infectious diseases among First Nations people. The Australian and NT Government investment of $4 billion over 10 years for remote housing in the Northern Territory, aims to improve living conditions in remote communities, thereby reducing health risks (AIHW 2024a). Additionally, the National Strategy for Food Security in Remote First Nations Communities, launched in 2025, focuses on increasing access to affordable and nutritious food in remote First Nations communities. This strategy includes reducing the cost of essential products in remote stores, building a nutrition workforce by upskilling local First Nations staff, and creating governance and support packages for remote stores. These initiatives align with the priority reforms of the National Agreement, aiming to address the broader social determinants of health and improve overall health outcomes for First Nations people.
The National Aboriginal and Torres Strait Islander Health Plan 2021–2031 (the Health Plan) provides a strong overarching policy framework for First Nations health and wellbeing, and is the first national health document to address the health targets and priority reforms of the National Agreement. The Health Plan consists of 12 priorities that guide the development of all First Nations health policies, programs and initiatives. Priority 9 of the Health Plan focuses on improving access to person-centred and family-centred care that is culturally safe and trauma-aware, across the health system, including acute care. Early access to responsive primary care, and addressing barriers to accessing care, are identified by the Health Plan as key to addressing high hospitalisation rates of First Nations people, where presentation often occurs at a later stage of disease.
Person-centred care involves placing the experience of First Nations patients at the centre of determining responsive care, allowing patients to set their own health priorities and care pathways. This includes embedding trauma-aware and healing-informed approaches to care.
Strategies to improve hospital service delivery to First Nations people by improving access and removing barriers to hospital services will improve the patient journey through the health system and improve outcomes. In order to provide access to flexible, culturally safe and responsive acute care, hospital services need to work with communities to understand their needs and to address the systemic factors that result in patients taking own leave from hospital or discharging against medical advice.
References
-
AIHW (Australian Institute of Health and Welfare) (2017), Spatial variation in Aboriginal and Torres Strait Islander women's access to 4 types of maternal health services, AIHW, Australian Government.
-
AIHW (2023), Cultural safety in health care for Indigenous Australians: monitoring framework, AIHW, Australian Government.
-
AIHW (2024a), Determinants of health for First Nations people, AIHW, Australian Government.
-
AIHW (2024b), Social determinants of health, AIHW, Australian Government, accessed May 2025.
-
AIHW (2024c), Maternity models of care in Australia, AIHW, Australian Government, accessed 21 March 2025.
- AIHW (2024d), Heart, stroke and vascular disease: Australian facts, AIHW, Australian Government.
- AIHW (2025a), Hospitals at a glance, AIHW, Australian Government.
-
AIHW (2025b), Aboriginal and Torres Strait Islander people’s preferences for, use of, and access to primary health care 2025, AIHW, Australian Government.
-
Alford K (2015) 'Indigenous health expenditure deficits obscured in Closing the Gap reports', Medical Journal of Australia, 203(10):403, doi:10.5694/mja15.00349.
-
ANZDATA Registry (2021) 'Haemodialysis', ANZDATA Annual Reports, Australia and New Zealand Dialysis and Transplant Registry, Adelaide.
-
Australians for Native Title and Reconciliation (2021), Racism in healthcare background: background paper 2021, ANTAR.
-
Beckwith K and Glover J (2018), Potentially preventable hospitalisations in Australia: variations by sociodemographic characteristics and geographical areas, with a focus on Aboriginal and Torres Strait Islander people, 2012/13 to 2014/15, Public Health Information Development Unit, Torrens University Australia, doi:10.25905/5c5ccc93cc109.
-
Broe G and Radford K (2018) 'Multimorbidity in Aboriginal and non-Aboriginal people', Medical Journal of Australia, 209(1):16–17, doi:10.5694/mja18.00348.
-
Carey TA, Arundell M, Schouten K, Humphreys JS, Miegel F, Murphy S and Wakerman J (2017) 'Reducing hospital admissions in remote Australia through the establishment of a palliative and chronic disease respite facility', BMC Palliative Care, 16(1):54, doi:10.1186/s12904-017-0247-3.
-
Carman W, Ishida M, Trounson JS, Mercer SW, Anindya K, Sum G, Armstrong G, Oldenburg B, McPake B and Lee JT (2022) 'Epidemiology of physical-mental multimorbidity and its impact among Aboriginal and Torres Strait Islander in Australia: a cross-sectional analysis of a nationally representative sample', BMJ Open, 12(10):e05999, doi:10.1136/bmjopen-2021-054999.
-
Casey D (2023) 'Aboriginal and Torres Strait Islander leadership in ARF and RHD: priorities, partnerships and progress', World Congress on Rheumatic Heart Disease, [conference presentation], NACCHO, Abu Dhabi.
-
Conway J, Lawn S, Crail S and McDonald S (2018) 'Indigenous patient experiences of returning to country: a qualitative evaluation on the Country Health SA Dialysis Bus', BMC Health Services Research, 18(1):1010, doi:10.1186/s12913-018-3849-4.
-
Davy C, Harfield S, McArthur A, Munn Z and Brown A (2016) 'Access to primary health care services for Indigenous peoples: a framework synthesis', International Journal for Equity in Health, 15:163, doi:10.1186/s12939-016-0450-5.
-
DHDA (Department of Health, Disability and Ageing) (2025a) Integrated Team Care program, accessed 2025.
-
DHDA (2025b) Services Australia Indigenous Access Line, accessed March 2025.
-
DoH (Department of Health) (2017), My life my lead – opportunities for strengthening approaches to the social determinants and cultural determinants of Indigenous health: report on the national consultations, DoH, Australian Government.
-
DoHAC (Department of Health and Aged Care) (2024a), More dialysis units for remote communities, [media release], DoHAC, Australian Government.
-
DoHAC (2024b), Three new renal units to open in remote Queensland and Western Australia, [media release], DoHAC, Australian Government.
-
Doran J, Canty D, Dempsey K, Cass A, Kangaharan N, Remenyi B, Brunsdon G, McDonald M, Heal C, Wang Z, Royse C, Royse A, Mein J, Gray N, Bennetts J, Baker RA, Stewart M, Sutcliffe S, Reeves B, Doran U, Rankine P, Fejo R, Heenan E, Jalota R, Ilton M, Roberts-Thomson R, King J, Wyber R, Doran J, Webster A and Hanson J (2023) 'Surgery for rheumatic heart disease in the Northern Territory, Australia, 1997–2016: what have we gained?', BMJ Global Health, 8(3):e011763, doi:10.1136/bmjgh-2023-011763.
-
Equity Economics and NACCHO (National Aboriginal Community Controlled Health Organisation) (2022), Measuring the gap in health expenditure: Aboriginal and Torres Strait Islander Australians, Equity Economics, NACCHO.
-
George MS, Davey R, Mohanty I and Upton P (2020) '“Everything is provided free, but they are still hesitant to access healthcare services”: why does the Indigenous community in Attapadi, Kerala continue to experience poor access to healthcare?', International Journal for Equity in Health, 19(1):105, doi:10.1186/s12939-020-01216-1.
-
Gorham G, Howard K, Cunningham J, Lawton PD, Ahmed AMS, Barzi F and Cass A (2022) 'Dialysis attendance patterns and health care utilisation of Aboriginal patients attending dialysis services in urban, rural and remote locations', BMC Health Services Research, 22:251, doi:10.1186/s12913-022-07628-9.
-
Gruneir A, Bronskill SE, Maxwel. CJ, Bai YQ, Kone AJ, Thavorn K, Petrosyan Y, Calzavara A and Wodchis WP (2016) 'The association between multimorbidity and hospitalization is modified by individual demographics and physician continuity of care: a retrospective cohort', BMC Health Services Research, 16(154), doi:10.1186/s12913-016-1415-5.
-
Howarth T, Gibbs C, Heraganahally SS and Abeyaratne A (2024) 'Hospital admission rates and related outcomes among adult Aboriginal Australians with bronchiectasis - a ten-year retrospective cohort study', BMC Pulmonary Medicine, 24(1):118, doi:10.1186/s12890-024-02909-x.
-
Hussain M, Katzenellenbogen J, Sanfilippo F, Murray K and Thompson S (2018) 'Complexity in disease management: a linked data analysis of multimorbidity in Aboriginal and non-Aboriginal patients hospitalised with atherothrombotic disease in Western Australia', PLoS ONE, 3(8):e0201496, doi:10.1371/journal.pone.0201496.
-
Keramat S, Perales F, Alam K, Rumana R, Haque R, Monasi N, Hashmi R, Siddika F, Hassan Z, Ali M, Gebremariam N and Kondalsamy-Chennakesavan S (2024) 'Multimorbidity and health-related quality of life amongst Indigenous Australians: a longitudinal analysis', Quality of Life Research, 33:195–206, doi:10.1007/s11136-023-03500-3.
-
Morse C (2024) ''Essential, lifesaving treatment': more dialysis units on the way to remote First Nations communities', National Indigenous Times.
-
NACCHO (2021), Core Services and Outcomes Framework: the Model of Aboriginal and Torres Strait Islander Community-Controlled Comprehensive Primary Health Care, National Aboriginal Community Controlled Health Organisation.
-
NACCHO (2025), NACCHO key facts, NACCHO.
-
Pearson O, Schwartzkopff K, Dawson A, Hagger C, Karagi A, Davy C, Brown A, Braunack-Mayer A and on behalf of the Leadership Group guiding the Centre for Research Excellence in Aboriginal Chronic Disease Knowledge and Translation Exchange (2020) 'Aboriginal community controlled health organisations address health equity through action on the social determinants of health of Aboriginal and Torres Strait Islander peoples in Australia', BMC Public Health, 20:1859, doi:10.1186/s12889-020-09943-4.
-
Price E, Kotevski A, Lamb K, Koye D, Taylor G, Ebsworth G and Burchill L (2024) 'Presentations to selected Melbourne hospitals with cardiovascular disease by Indigenous and non-Indigenous people, 2011–19: a linked administrative data analysis', Medical Journal of Australia, 220(4):208–210, doi:10.5694/mja2.52215.
-
Purple House (n.d.) The Purple Truck.
-
Shearing T, Sivak L, Mejia G, Clinch N, O’Donnell K, Sinclair N, Kartinyeri J, Owen K, Clinch D and Morey K (2023) 'A pilot place-based renal dialysis model of care responding to Aboriginal and Torres Strait Islander priorities in South Australia', Australian and New Zealand Journal of Public Health, 47(6):100107, doi:10.1016/j.anzjph.2023.100107.
-
Spinks J, Mihala G, Jennings W, Ware RS, Kalisch Ellett LM, Roughead EE and Williamson D (2025) 'Potentially preventable medication-related hospitalisations with cardiovascular disease of Aboriginal and Torres Strait Islander people, Queensland, 2013–2017: a retrospective cohort study', Medical Journal of Australia, 222(4):198–204, doi:10.5694/mja2.52600.
-
Stacey I, Katzenellenbogen J, Hung J, Seth R, Francia C, MacDonald B, Marangou J, Murray K and Cannon J (2024) 'Pattern of hospital admissions and costs associated with acute rheumatic fever and rheumatic heart disease in Australia, 2012–2017', Australian Health Review, 49(1):AH24148, doi:10.1071/AH24148.
-
Su J, He V, Lithgow A and Guthridge S (2024) 'Risk factors for unintentional injury hospitalisation among Aboriginal and non-Aboriginal children in Australia’s Northern Territory: a data linkage study', PLoS One, 19(11):e0311586, doi:10.1371/journal.pone.0311586.
-
Zhao Y, Thomas S, Guthridge S and Wakerman J (2014) 'Better health outcomes at lower costs: the benefits of primary care utilisation for chronic disease management in remote Indigenous communities in Australia's Northern Territory', BMC Health Services Research, 14:463, doi:10.1186/1472-6963-14-463.
-
Zhao Y, Wright J, Guthridge SL and Lawton P (2013) 'The relationship between number of primary health care visits and hospitalisations: evidence from linked clinic and hospital data for remote Indigenous Australians', BMC Health Services Research, 13(1):466, doi:10.1186/1472-6963-13-466.

