Key messages
Why is it important?
The all-cause age-standardised death rate measures overall population health by adjusting death rates to a standard age distribution. These rates are valuable for comparing the overall health status of different populations (with different age profiles) and to monitor changes over time. As life expectancy estimates for Aboriginal and Torres Strait Islander (First Nations) people are only available every 5 years, death rates allow more regular monitoring of progress towards Closing the Gap Target 1 – Close the Gap in life expectancy by 2031.
The disparities in death rates highlight the impact of the significantly greater burden of disease and health needs for First Nations people, and the importance of orienting and resourcing appropriate services towards meeting those needs. This is in addition to addressing the upstream modifiable risk factors and social determinants of health which have been impacted by historical and ongoing impacts from colonisation, including intergenerational trauma, and systemic and interpersonal racism.
Data findings
-
Nationally, in 2019–2023 there were 22,275 deaths of First Nations people, 90% (19,993) of which occurred in the 5 jurisdictions with adequate Indigenous status identification for reporting death rates (New South Wales, Queensland, Western Australia, South Australia and the Northern Territory). In these 5 jurisdictions, there were 464 deaths per 100,000 population.
-
In 2019–2023, the proportion of First Nations males and females who died at or after age 65 was 6 percentage points higher than in 2014–2018 – 39% compared with 33% and 51% compared with 45%, respectively.
-
The age-specific death rate was higher for First Nations people than for non-Indigenous Australians across all age groups. The relative difference in the age-specific death rates initially widened as age increased, peaking at 3.9 times as high for First Nations people aged 35–44, after which the relative difference declined to 1.2 times as high for First Nations people aged 75 and over.
-
From 2016 to 2021, the age-standardised death rate for First Nations people increased by 5.1%, while the non-Indigenous rate declined by 10%. This resulted in a widening in the absolute gap between the two populations by 41% and a slight increase in the relative gap from 1.4 to 1.6 times as high.
-
In 2019–2023, First Nations people aged under 75 experienced higher rates of potential years of life lost due to premature death than non-Indigenous Australians. The biggest gap in potential years of life lost (PYLL) between First Nations people and non-Indigenous Australians was for men aged 50–54, with a difference of 159 PYLL per 1,000 people, and for women aged 60–64, with a difference of 115 PYLL per 1,000 people.
Research and evaluation findings
-
Increases in life expectancy for First Nations men in the Northern Territory were linked to fewer years of life lost to cancer, unintentional injuries and cardiovascular disease. Increased life expectancy for First Nations women came from fewer life years lost to cancer, intentional injuries and kidney disease.
-
Smoking is strongly linked to higher mortality. Mortality was highest among high-frequency smokers, and lowest for those who had never smoked. Quitting smoking at any age had benefits, with those quitting before age 45 having a similar mortality risk to those who had never smoked.
-
Research has shown the importance of cultural determinants of health for First Nations people with strong links between health and wellbeing and family/community, Country and place, cultural identity and self-determination. Further research is needed to better understand the complex causal pathways through which cultural determinants influence health outcomes.
Implications
Death rates among First Nations people decreased between 1998 and 2006, but this trend should be interpreted cautiously due to changes in data quality, improved identification in death records, and population growth – particularly from non-demographic factors. Since 2006, progress slowed and plateaued. Key contributors to mortality include chronic disease, social and emotional wellbeing and injuries.
Timely access to culturally appropriate and well-resourced primary health care is essential for prevention, screening, early detection and management of conditions sensitive to health intervention. Addressing the upstream modifiable risk factors and social determinants of health are crucial but need to be understood in the context of the ongoing impacts of colonisation, including intergenerational trauma, systemic and interpersonal racism, and the disruption of cultural, social, and economic systems. The broader heath system has its role to play by eliminating racism, adapting services to more appropriately meet the needs of First Nations people, and working in partnership with First Nations people.
Why is it important?
The all-cause age-standardised death rate measures overall population health by adjusting death rates to a standard age distribution. It can then be used to compare with other populations that have different age structures (by removing the confounding effect of age). While useful, it has limitations: these rates are modelled having been adjusted for age, they may not reflect immediate health improvements, and do not capture non-fatal illnesses like arthritis and depression. Despite these limitations, these rates remain valuable for comparing the overall health status of different populations and to monitor changes over time.
The all-cause age-standardised death rate is particularly important for Aboriginal and Torres Strait Islander (First Nations) people for several reasons:
- In 2019–2023, the all-cause death rate for First Nations people is 1.7 times the rate for non-Indigenous Australians (age-standardised), highlighting the need for health improvement.
- Tracking this rate over time allows for the monitoring of progress in closing the health gap more frequently than life expectancy estimates. It helps evaluate the effectiveness of health programs and policies aimed at reducing mortality and improving health.
- This measure helps garner policy attention to the areas where health interventions are most needed.
- Providing communities with information about death rates empowers them to take proactive steps in improving their health and wellbeing.
The disparity in death rates is shaped by the ongoing impacts of colonisation, including intergenerational trauma, systemic and interpersonal racism, and the historical disruption of cultural, social, and economic systems. These factors continue to influence health and wellbeing across both remote and non-remote communities (Paradies 2016; Paradies and Cunningham 2012).
The National Agreement on Closing the Gap (the National Agreement), was developed in partnership between Australian governments and the Coalition of Aboriginal and Torres Strait Islander Peak Organisations. It is built around 4 Priority Reforms directly informed by First Nations people. These reforms aim to change how governments work with First Nations people by fostering partnership and shared decision-making, building the Aboriginal community-controlled sector, transforming government organisations, and improving and sharing access to data and information to enable informed decision making by First Nations communities. The National Agreement has identified the importance of making sure First Nations people enjoy long and healthy lives, and that First Nations people enjoy high levels of social and emotional wellbeing. To support these outcomes the National Agreement specifically outlines the following targets to direct policy attention and monitor progress:
- Target 1 – Close the Gap in life expectancy within a generation, by 2031
- Target 14 – Significant and sustained reduction in suicide of Aboriginal and Torres Strait Islander people towards zero
These targets are part of a broader framework aimed at addressing various socioeconomic and health disparities faced by First Nations communities.
For the latest data on the Closing the Gap targets, see the Closing the Gap Information Repository.
As life expectancy estimates for First Nations people are published every 5 years by the Australian Bureau of Statistics (ABS), the National Agreement also identified several supporting indicators, which may be used to direct policy attention and provide proxy information for monitoring progress towards the target in the intervening years (Productivity Commission 2021). One of the supporting indicators for this target is all-cause death rates (the focus of this HPF measure). Other supporting indicators that draw on deaths data are leading causes of death and potentially avoidable death rates (see measures 1.23 Leading causes of death and 1.24 Avoidable and preventable deaths, respectively, for information on these topics).
The National Aboriginal and Torres Strait Islander Health Plan 2021–2031 (the Health Plan), provides a strong overarching policy framework for First Nations health and wellbeing and is the first national health document to address the health targets and priority reforms of the National Agreement.
The vision of the Health Plan is that First Nations people enjoy long, healthy lives centred in culture, with access to services that are prevention-focused, culturally safe and responsive, equitable, and free of racism.
Both the National Agreement and the Health Plan are discussed further in the Implications section of this measure.
Burden of disease
Burden of disease analysis is a way of measuring the impact of both living with poor health (the non-fatal burden of disease) and dying prematurely (fatal burden). It is measured using ‘disability-adjusted life years’ (DALY), where 1 DALY represents 1 year of healthy life lost, either through premature death (‘years of life lost’ or YLL) or from living with an illness or injury (‘years lived with disability’ or YLD).
In 2018, First Nations people lost 239,942 years of healthy life (DALY) at a rate of 289 DALY per 1,000 population. Of the total DALY experienced by First Nations people just under half can be attributed to the fatal burden (47% or 113,445 YLL) and the remainder to the non-fatal burden (53% or 126,496 YLD) (AIHW 2022).
Focusing on the fatal burden of disease for First Nations people shows that, in 2018:
- Males experienced a higher proportion (58% or 66,285 YLL) of the fatal burden than females (42% or 47,160 YLL).
- Age-specific fatal burden rates were higher for males than females for those aged under 85. The largest relative difference was for those aged 20–24 where the rate was 2.4 times as high for males as for females (91 compared with 37 YLL per 1,000, respectively). The largest absolute difference between the sexes was for those aged 70–74, a difference of 165 YLL per 1,000 population (599 compared with 434 YLL per 1,000, respectively).
- After adjusting for differences in age structure between the sexes, fatal burden was 1.4 times as high for males as for females (238 compared with 166 YLL per 1,000, respectively) (AIHW 2022).
First Nations people experienced fatal burden at 2.5 times the rate for non-Indigenous Australians (AIHW 2022).
Data findings
Deaths data in this measure are sourced from the National Mortality Database. The data are used to report the total number of deaths in Australia (nationally), which includes Australian residents of all states and territories. However, when reporting death rates, data have been limited to 5 jurisdictions (New South Wales, Queensland, Western Australia, South Australia and the Northern Territory), in which the quality of Indigenous status identification in the deaths data is considered adequate. National death rates are not published due to concerns around the quality of Indigenous status identification in Victoria, Tasmania and the Australian Capital Territory.
When reporting death rates by remoteness, data from all jurisdictions have been included.
Nationally, over the 5-year period 2019–2023, there were 22,275 deaths of First Nations people, or an average of 4,455 deaths annually. Of these 12,165 (55%) were deaths of First Nations males and 10,110 (45%) were deaths of First Nations females.
Over the same 5-year period, for the 5 jurisdictions considered to have adequate Indigenous status identification, there were 19,993 deaths of First Nations people. This accounts for 90% of all 22,275 national deaths and corresponds to a rate of 464 deaths per 100,000 population (Table D1.22.2).
By state and territory
In 2019–2023, of the 19,993 deaths of First Nations people in the 5 jurisdictions with adequate Indigenous identification, over one-third (35% or 6,953 deaths) occurred in New South Wales, consistent with the population distribution (with 35% of First Nations people living in New South Wales) (Table D1.22.3; Table D1). Across the 5 jurisdictions, the death rate (which accounts for population size) was highest for First Nations people living in the Northern Territory (718 deaths per 100,000) followed by Western Australia (545 deaths per 100,000), South Australia (493 per 100,000) and Queensland (419 per 100,000) (Table D1.22.3).
By age and sex
Of the 19,993 deaths recorded for First Nations people in the 5 jurisdictions combined in 2019–2023, 54% (10,888) were males and 46% (9,105) were females – corresponding to rates of 503 and 424 deaths per 100,000 population, respectively. Death rates for males were higher than females for all 10-year age groups between 15 and 75 and over. The highest relative difference was for those aged 15–24, where the rate for males was 2 times as high as the rate for females. In each subsequent 10-year age group the relative difference continued to narrow to a low of 1.1 for those aged 75 and over (Table D1.22.2, Figure 1.22.1).
Figure 1.22.1: Age-specific death rates among First Nations people, by sex, NSW, Qld, WA, SA and the NT, 2019–2023
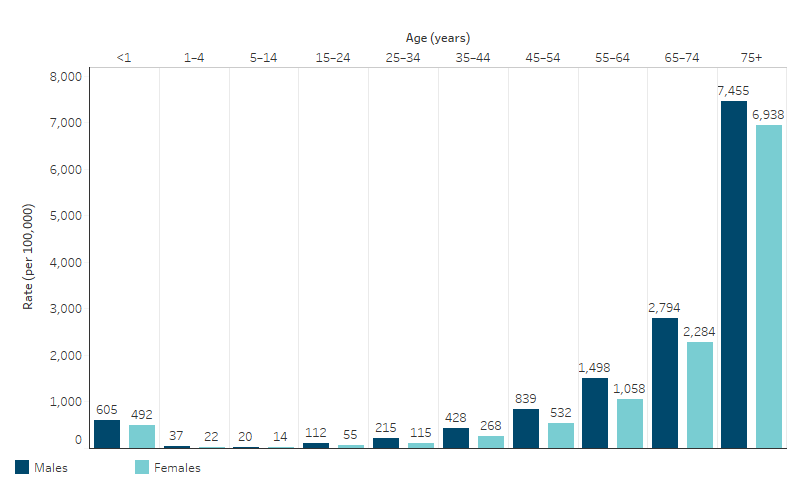
Source: Table D1.22.2. AIHW National Mortality Database.
Over the 5-year period 2019–2023, the proportion of total deaths that occurred under 65 years of age was 11 percentage points higher for First Nations males than for First Nations females – 61% of all male deaths (6,621 deaths) compared with 50% of all female deaths (4,495 deaths). Conversely, deaths of those aged 65 and over accounted for a higher proportion of deaths among females than males (51% compared with 39%) (Table D1.22.1, Figure 1.22.2).
Comparing the 2014–2018 data with that for 2019–2023 shows that, for First Nations people:
- The proportion of males who died at or after age 65 was 6 percentage points higher in 2019–2023 (39% compared with 33%), as was the case for females (51% compared with 45%).
- There were corresponding reductions in the proportion of deaths among those aged under 65, with the largest percentage point reductions for males and females aged 45–49 (2.1 and 1.4 percentage points, respectively) (Table D1.22.1, Figure 1.22.2).
Figure 1.22.2: Distribution of deaths, by sex, age and Indigenous status, NSW, Qld, WA, SA and the NT, 2014–2018 and 2019–2023
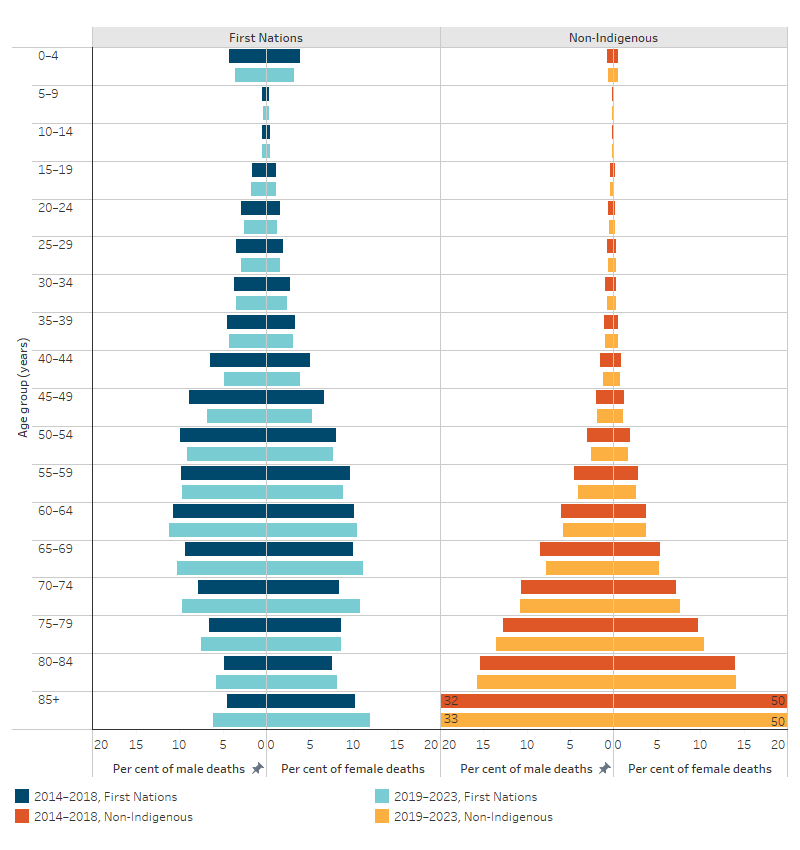
Source: D1.22.1. AIHW National Mortality Database.
Comparisons with non-Indigenous Australians
During 2019–2023, in the 5 jurisdictions with adequate Indigenous status identification, First Nations people were more likely to die at a younger age than non-Indigenous Australians, with 56% of deaths occurring before age 65 compared with 16% for non-Indigenous Australians (Table D1.22.2). This difference was larger for males than females:
- 61% of deaths occurred before age 65 for First Nations males compared with 19% for non-Indigenous males (42 percentage point difference).
- 50% of deaths occurred before age 65 for First Nations females compared with 13% for non-Indigenous females (37 percentage point difference) (Table D1.22.1, Figure 1.22.2).
This is because of both the younger age profile of the First Nations population, as well as the higher death rates of First Nations people within each age group. The age-specific death rate was higher for First Nations people across all 10-year age groups than for non-Indigenous Australians. The relative difference in the age-specific death rates initially widened as age increased, peaking at 3.9 times as high for First Nations people aged 35–44 as for non-Indigenous Australians, after which the relative difference declined to 1.2 times as high for First Nations people aged 75 and over (Table D1.22.2).
In 2019–2023, after adjusting for differences in the age structure between the two populations, the death rate for First Nations people was 1.7 times the rate for non-Indigenous Australians (Table D1.22.2).
During 2019–2023, age-standardised death rates were higher for First Nations people than non-Indigenous Australians in all 5 jurisdictions for which rates are available. The relative difference was highest for the Northern Territory (2.8 times as high) (Table D1.22.3).
Potential years of life lost (PYLL)
Over the 2019–2023 period, in the 5 jurisdictions with adequate Indigenous status identification there were 15,273 deaths of First Nations people aged under 75, who collectively had 360,108 PYLL. These deaths account for over three-quarters (76%) of the total First Nations deaths and correspond to a rate of 85 PYLL per 1,000 population, or an average of 24 PYLL per death (Table D1.22.8).
Among First Nations males and females, rates of PYLL were lowest for those aged 5–9 (12 and 7.4 PYLL per 1,000, respectively). The rate increased with age until 50–54 for males (reaching 229 per 1,000) and 60–64 for females (169 per 1,000). The rate of PYLL was higher for First Nations males than females in all 5-year age groups. The absolute difference in rates of PYLL between First Nations males and females ranged from a low of 3.7 per 1,000 for those aged 10–14 to a peak of 82 per 1,000 for those aged 50–54 (Table D1.22.8).
The rate of PYLL was higher for First Nations people than non-Indigenous Australians in all 5-year age groups, with the absolute gap being particularly high for the 0–4 age group, and then increasing to peak in middle age. The absolute difference in rates of PYLL between First Nations and non-Indigenous males peaked for those aged 50–54 at a difference of 159 PYLL per 1,000 and for females aged 60–64 at a difference of 115 PYLL per 1,000 (Table D1.22.8, Figure 1.22.3).
Figure 1.22.3: The gap in potential years of life lost before age 75 (PYLL) per 1,000 population between First Nations people and non-Indigenous Australians, by age and sex, 2019–2023
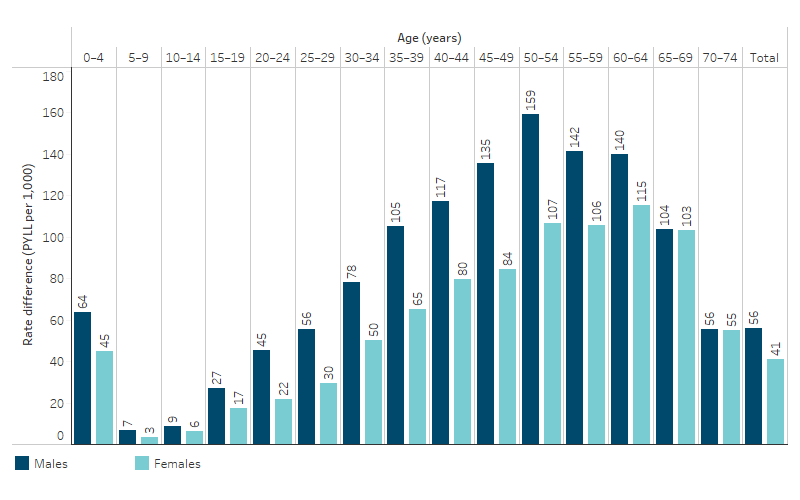
Source: Table D1.22.8. AIHW National Mortality Database.
Changes over time
Over the period from 2016 to 2021, in the 5 jurisdictions combined, the age-standardised death rate among First Nations people increased by 5.1%. This was predominantly driven by a 7% increase in the rate for First Nations males as the rate did not change significantly for First Nations females over this period.
In contrast, over the same period, the age-standardised death rate for non-Indigenous Australians declined by 10% with a similar decrease between males and females (10% and 9%, respectively). As a result, the absolute difference in the age-standardised death rate between First Nations people and non-Indigenous Australians widened by 41%. The relative difference ranged between 1.4 times as high in 2016 and 1.6 times as high in 2021 for First Nations people (Table D1.22.5; Figure 1.22.4).
Figure 1.22.4: Age-standardised death rates, by Indigenous status, NSW, Qld, WA, SA and NT, 2016–2023
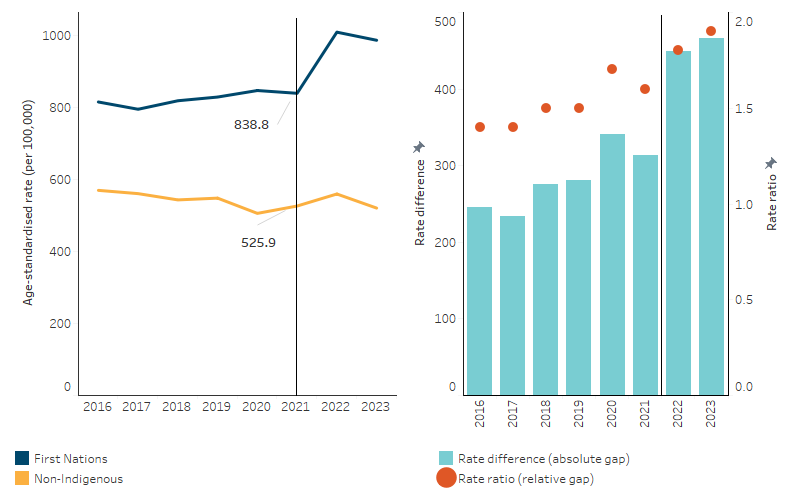
Note: The vertical line indicates break in series in 2022 due to changes in Indigenous identification method in New South Wales. Caution should be used when interpreting changes in death rates over time (see Box 1.22.1 for more information).
Source: Table D1.22.5. AIHW National Mortality Database
By state and territory
For First Nations people over the period from 2016 to 2023, the age-standardised death rate did not change significantly in Queensland, Western Australia and the Northern Territory. For First Nations people in South Australia, the age-standardised death rate increased by an average of 37 deaths per 100,000 population annually over this period. Among non-Indigenous Australians over the same period, the age-standardised death rate decreased by between 6 and 8 deaths per 100,000 annually in Western Australia, South Australia and the Northern Territory. As a result, the absolute gap between First Nations people and non-Indigenous Australians widened in South Australia and Western Australia.
Comparable time trends for New South Wales are available over the shorter period from 2016 to 2021. In this period, the age-standardised death rate increased by an average of 22 deaths per 100,000 annually for First Nations people in New South Wales while rates for non-Indigenous Australians did not change significantly (Table D1.22.6).
By remoteness
For First Nations people, over the period 2016 to 2021, the age-standardised death rate increased in non-remote areas (that is, Major cities, Inner regional, and Outer regional areas combined) and remained unchanged in remote areas (Remote and Very remote areas combined).
Between 2016 and 2021, in non-remote areas:
- The age-standardised death rate increased by 12% for First Nations people but decreased by 10% for non-Indigenous Australians. As a result, the absolute difference between First Nations people and non-Indigenous Australians more than doubled (increased by 147%) over this period.
- The relative difference in the age-standardised death rate was higher for First Nations people than non-Indigenous Australians in all years, and ranged from a low of 1.2 times as high in 2016 to 1.5 times as high in 2020 (Table D1.22.11, Figure 1.22.5).
Over the period 2016 to 2021, in remote areas:
- The age-specific death rates improved for those aged 65–74, with a decline of 15%. This was the only age group with a statistically significant change in either remote or non-remote areas.
- Based on age-standardised rates, the death rate for First Nations people did not change significantly while the rate for non-Indigenous Australians declined by 11%.
- The absolute difference in death rates between the two populations did not change significantly over the period and the relative difference ranged from 2.2 times as high for First Nations people in 2017 to 2.4 times as high in 2020 and 2021 (Table D1.22.11, Figure 1.22.5).
Figure 1.22.5: Age-standardised death rates, by Indigenous status and remoteness, Australia, 2016 to 2023
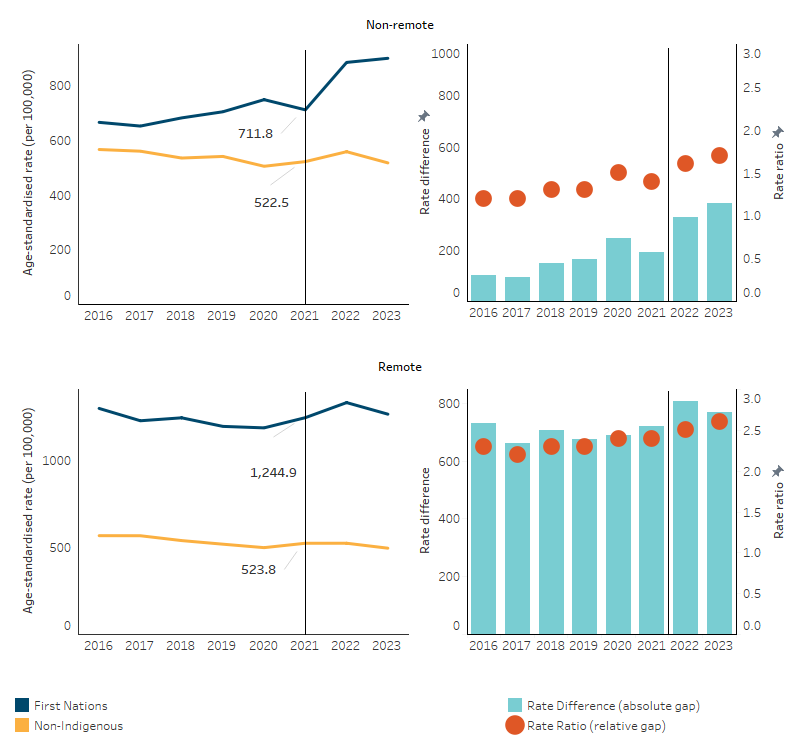
Note: The vertical line indicates break in series in 2022 due to changes in Indigenous identification method in New South Wales. Caution should be used when interpreting changes in death rates over time (see Box 1.22.1 for more information).
Source: Table D1.22.11. AIHW National Mortality Database.
International comparisons
Death rates are also available for other countries where Indigenous people share a similar history of European colonisation, such as New Zealand and the United States. In New Zealand in 2022, the age-standardised death rate for the Māori population was 1.5 times the rate for other New Zealanders (884 and 588 per 100,000, respectively) (Table D1.22.7). In the United States in 2023, the age-standardised death rate for American Indians and Alaskan Natives was 1.1 times the rate for non-Hispanic whites (831 and 778 per 100,000, respectively) (Ahmad et al. 2024).
In 2023, for the 5 Australian jurisdictions with adequate Indigenous status identification, the age-standardised death rate for First Nations people was 1.9 times the rate for non-Indigenous Australians.
Caution must be used when comparing Australian data with data from other countries due to variations in data quality, methods applied to addressing data quality issues and definitions for identifying Indigenous peoples.
Research and evaluation findings
A review of research relating to cultural determinants of health for First Nations people identified strong links between health and wellbeing and cultural determinants such as family/community, Country and place, cultural identity and self-determination, noting the need for further research to better understand the complex causal pathways through which cultural determinants influence health outcomes (Verbunt et al. 2021).
Cultural determinants are anchored in First Nations ways of knowing, being and doing that encompass a holistic understanding of health and wellbeing. Culture is central to this understanding and shapes the relationship between self and Country, kin, community and spirituality – all of which are key factors of health and wellbeing. This notion extends to a First Nations focus on life-giving values from which individuals, families and communities can draw strength, resilience and empowerment (Verbunt et al. 2021; Williamson et al. 2021). This includes culturally appropriate care at all life stages, including palliative and end-of-life care, where connection to Country and community is often disrupted by hospitalisation or standard mortuary practices. Respecting cultural values in treatment decision-making, particularly at the end of life, is essential to delivering culturally safe and responsive care (Neller et al. 2024). The cultural determinants approach has demonstrated significant health gains in Indigenous populations internationally, including in New Zealand, Canada and the United States (Verbunt et al. 2021).
A study of the mortality gap for First Nations people in the Northern Territory found a large proportion of the increases in life expectancy between 1966–71 and 2011–16 were due to improvements in mortality for children under 5 years of age (Wilson et al. 2019). This is in contrast to the Australian population as a whole, where life expectancy gains came predominantly from mortality declines in older age groups, and where child mortality was already very low.
A retrospective observational study analysed deaths among the Tiwi people on Bathurst and Melville Islands off the coast of the Northern Territory between 1960 and 2010. The study illustrated the epidemiological transition of these communities with improvements in preventable infant deaths leading to changes in the demographic and mortality profile of the population over time. High numbers of infant deaths in the 1960s from diarrhoea, respiratory disease and failure to thrive shifted to deaths in older age groups from chronic lung disease, cardiovascular disease and renal failure. The study also illustrated the Barker Hypothesis, showing that many children with low birthweight who were once at greater risk of early death are surviving to adulthood but with enhanced susceptibility to chronic disease. Improvements in birthweights and in the prevention and management of chronic disease will lead to continued improvements in mortality. The study also showed a concerning pattern of deaths among 15–45 year olds from non-natural causes such as accidents, suicide, and homicide from the mid-1980s and peaking in the early 2000s, suggesting that improvements in socioeconomic determinants as well as health services are needed for these age groups (Hoy et al. 2017).
Another study comparing the life expectancy trends of First Nations people and non-Indigenous Australians in the Northern Territory found that increases in life expectancy for First Nations men were linked to fewer years of life lost to cancer, unintentional injuries and cardiovascular disease. Increased life expectancy for First Nations women came from fewer life years lost to cancer, intentional injuries and kidney disease (Zhao et al. 2022).
A study of the effect of smoking on the mortality of First Nations people in Australia found that smoking was strongly linked to higher mortality (Thurber et al. 2021). Mortality was highest among high-frequency smokers, and lowest for those who had never smoked. Quitting smoking at any age had benefits, with those quitting before age 45 having a similar mortality risk to those who had never smoked.
Implications
While the death rate among First Nations people decreased between 1998 to 2006, this trend should be interpreted with caution. Changes in data quality, improved identification in death records, and population growth – particularly from non-demographic factors such as changes in self-identification – have influenced these estimates. Since 2006, progress has slowed, and in more recent years has plateaued (up to 2021). More time is needed to assess the impact of more recent changes to data collection since 2022.
Much more effort is required to further improve the health status of First Nations people. In particular, continued and enhanced efforts are needed to address the contributing factors to mortality including maternal and child health, social and emotional wellbeing, and chronic disease. Timely and appropriate access to primary health care is critical to improve prevention, screening, detection and management of chronic disease in order to reduce mortality from causes that are sensitive to population health interventions and medical care. Efforts to address the impact of modifiable behavioural risk factors such as smoking, and socioeconomic disadvantage such as education, employment and housing, are critical but need to be understood in the context of the ongoing impacts of colonisation (see measures across Tier 2 of this Health Performance Framework). Improved regional and local data would assist in identifying areas of greatest need and assist in efforts to strengthen the capacity of primary health care services to meet that need.
Analysis of death rates by remoteness illustrates the stark disadvantage experienced by First Nations people in remote areas. On average, First Nations people living in remote areas have higher rates of disease burden and lower life expectancy compared with those in non-remote areas. Key contributors to this include differences in educational and employment opportunities, in access to health services, in housing circumstances, and in other factors that support healthy behaviours such as the availability and cost of fresh fruit and vegetables (AIHW 2024). However, the recent rise in First Nations mortality in non-remote areas needs further unpacking. Findings from this and other measures reinforce the need for continued and enhanced policy effort nationwide to address the health needs of First Nations people and provide impetus for continued efforts under the National Agreement and the Health Plan.
There are a range of health initiatives aimed at improving the health and wellbeing of First Nations people in Australia, funded by Australian governments and non-government organisations. One key program is the Indigenous Australians' Health Programme (IAHP), which primarily funds Aboriginal Community Controlled Health Services to provide high-quality, culturally appropriate health care for First Nations people. The IAHP supports primary health care services, improves access to culturally appropriate health care, and funds targeted health activities such as managing chronic conditions and improving ear and eye health. The First Nations Health Funding Transition Program (FNHFTP) focuses on transitioning health service delivery to First Nations-led organisations. It aims to improve health outcomes by ensuring that health care is provided by organisations that understand and respect the cultural context of First Nations people. Overall, these programs have made significant strides in improving health outcomes for First Nations people, but ongoing efforts are needed to close the health gap and address remaining barriers to access and equity.
The National Agreement was developed in partnership between all Australian governments and the Coalition of Aboriginal and Torres Strait Islander Peak Organisations. Each party to the National Agreement has developed their own Implementation Plan and reports annually on their actions to achieve the outcomes of the National Agreement. The FNHFTP is a strong example of work aligned with the National Agreement on Closing the Gap. However, successive reviews have found that governments are not fully meeting their commitments under the Agreement. Both the Productivity Commission and the Jumbunna Institute have highlighted that more needs to be done to uphold the shared commitments, particularly in enacting the Priority Reforms and shifting from business-as-usual approaches to genuine partnership and structural change (Lavearch et al. 2025; Productivity Commission 2024).
The Health Plan, released in December 2021, is the overarching policy framework to drive progress against the Closing the Gap health targets and priority reforms. The Australian Government is responsible for implementing the Health Plan at a national level. States, territories and other implementation partners, while also responsible for its implementation, can take flexible approaches to implementing Health Plan priorities. Their approaches will depend on local needs and priorities, led by First Nations people and communities.
Implementation of the Health Plan aims to drive structural reform towards models of care that are prevention and early intervention focused, with greater integration of care systems and pathways across primary, secondary and tertiary care. It also emphasises the need for mainstream services to address racism and provide culturally safe and responsive care, and be accountable to First Nations people and communities.
References
- ABS (Australian Bureau of Statistics) (2023a) Causes of death, Australia methodology (2022), ABS website, accessed 27 January 2026.
- ABS (2023b) Understanding change in counts of Aboriginal and Torres Strait Islander Australians: Census (2021), ABS website, accessed 27 January 2026.
- ABS (2024) Causes of death, Australia methodology (2023), ABS website, accessed 27 January 2026.
- ABS (2025) Excess mortality by selected causes of death, 2020–23, ABS website, accessed 27 January 2026.
- Ahmad F, Cisewski J and Anderson R (2024) 'Mortality in the United States — provisional data, 2023', Morbidity and Mortality Weekly Report, 73(31):677–681, doi:10.15585/mmwr.mm7331a1.
- AIHW (Australian Institute of Health and Welfare) (2022) Impact and causes of illness and death in Aboriginal and Torres Strait Islander people 2018, Australian Burden of Disease Study, AIHW, Australian Government, doi:10.25816/xd60-4366.
- AIHW (2024) Aboriginal and Torres Strait Islander people: health and wellbeing of First Nations people, AIHW, Australian Government, accessed March 2025.
- Hoy WE, Mott SA and McLeod BJ (2017) 'Transformation of mortality in a remote Australian Aboriginal community: a retrospective observational study', BMJ Open, 7(8):e016094, doi:10.1136/bmjopen-2017-016094.
- Lavearch L, Coombes L, Gray K, Anthony C, Nolan-Smith S, Ah Matt M, Beaufils J, Compton A, Garay M, Hammond A, Highfold A, Hood P, Hemmings S, McDaniel L, Olsen K, Sentence G, Sherwood J, Taylor A and Toy M (2025) Closing the Gap: independent Aboriginal and Torres Strait Islander led review, Jumbunna Institute for Indigenous Education and Research, University of Technology Sydney.
- Neller P, Feeney R, Willmott L, Then S-N, Munro E, Cain K, Yates P and White BP (2024) 'Australian Indigenous people and treatment decision-making at end-of-life', Alternative Law Journal, 49(2):104–113, doi:10.1177/1037969x241255172.
- Paradies Y (2016) 'Colonisation, racism and Indigenous health', Journal of Population Research, 33:83–96, doi:10.1007/s12546-016-9159-y.
- Paradies YC and Cunningham J (2012) 'The DRUID study: racism and self-assessed health status in an Indigenous population', BMC Public Health, 12:131, doi:10.1186/1471-2458-12-131.
- Productivity Commission (2021) Closing the Gap annual data compilation report July 2021, Annual Data Compilation Report Series, Productivity Commission, Australian Government, accessed 28 September 2025.
- Productivity Commission (2024) Review of the National Agreement on Closing the Gap - study report, Productivity Commission, Australian Government, accessed 7 October 2025.
- Thurber KA, Banks E, Joshy G, Soga K, Marmor A, Benton G, White SL, Eades S, Maddox R, Calma T and Lovett R (2021) 'Tobacco smoking and mortality among Aboriginal and Torres Strait Islander adults in Australia', International Journal of Epidemiology, 50(3):942–954, doi:10.1093/ije/dyaa274.
- Verbunt E, Luke J, Paradies Y, Bamblett M, Salamone C, Jones A and Kelaher M (2021) 'Cultural determinants of health for Aboriginal and Torres Strait Islander people – a narrative overview of reviews', International Journal for Equity in Health, 20:181, doi:10.1186/s12939-021-01514-2.
- Williamson L, Dent P and Bowman N (2021) Culture is key: towards cultural determinants-driven health policy – final report, Lowitja Institute, doi:10.48455/k9vd-zp46.
- Wilson T, Zhao Y and Condon J (2019) 'Limited progress in closing the mortality gap for Aboriginal and Torres Strait Islander Australians of the Northern Territory', Australian and New Zealand Journal of Public Health 43(4):340–345, doi:10.1111/1753-6405.12921.
- Zhao Y, Li S, Wilson T and Burgess P (2022) 'Improved life expectancy for Indigenous and non‐Indigenous people in the Northern Territory, 1999–2018: overall and by underlying cause of death', Medical Journal of Australia, 217:30–35, doi:10.5694/mja2.51553.

