Key messages
Why is it important?
Chronic respiratory diseases (CRDs) – including asthma and chronic obstructive pulmonary disease (COPD) – and acute respiratory illnesses such as pneumonia, influenza and invasive pneumococcal disease, are a major cause of poor health and death for Aboriginal and Torres Strait Islander (First Nations) people.
These conditions are driven by a combination of biomedical, behavioural, and environmental factors, and are exacerbated by social determinants such as overcrowded housing, poor infrastructure, tobacco exposure, and limited access to culturally safe health care, prevention and treatment. Historical and ongoing impacts of colonisation have contributed to persistent inequities, particularly in remote and underserved communities.
Data findings
- In 2018, respiratory diseases caused an estimated 17,920 years of healthy life lost due to illness and or death – accounting for 7.5% of the total burden of disease for First Nations people. The age-standardised burden due to respiratory diseases for First Nations people was 2.7 times the rate for non-Indigenous Australians.
- Respiratory diseases were the fourth leading cause of death for First Nations people. Nationally, over the 5-year period 2019–2023, there were 2,095 deaths of First Nations people that were due to respiratory disease. Over the same period, in the 5 jurisdictions with adequate Indigenous status identification, there were 1,871 deaths of First Nations people due to respiratory diseases. This corresponds to 9% of all deaths in New South Wales, Queensland, Western Australia, South Australia and the Northern Territory combined, or a rate of 43 deaths per 100,000 population.
- The major contributor to deaths due to respiratory diseases among First Nations people in 2019–2023 was COPD (1,270 deaths or 68% of all deaths due to respiratory diseases), followed by influenza and pneumonia (256 deaths or 14%).
- In 2020–2023 there were 241 deaths of First Nations people due to COVID-19, corresponding to a crude death rate of 6.9 deaths per 100,000 population. The death rate due to COVID-19 among First Nations people was 1.5 times the rate for non-Indigenous Australians, after adjusting for differences in the age-structure of the two populations.
- Rates of death due to specific respiratory diseases were similar for First Nations males and females for COPD, and influenza and pneumonia. The death rates due to asthma and bronchiectasis were higher for females while pulmonary oedema and other interstitial pulmonary diseases were higher for males.
- In 2019–2023 the respiratory disease death rate was 2.2 times as high for First Nations people as for non-Indigenous Australians (2.6 times in remote areas and 1.9 times in non-remote areas). The death rate due to COPD for First Nations people was 3.1 times that of non-Indigenous Australians, and the death rate due to asthma and bronchiectasis were 2.4 and 2.5 times higher respectively.
- From 2016 to 2021, there was no significant change in the age-standardised death rate due to respiratory diseases for First Nations people, nor in the gap in the rates for First Nations people and non-Indigenous Australians in the 5 jurisdictions.
- Between July 2021 and June 2023, there were 59,271 hospitalisations due to respiratory disease among First Nations people (8.1% of total First Nations hospitalisations, excluding dialysis). Of these, 21% were due to pneumonia, with a further 18% due to COPD.
- Over the same period, the hospitalisation rate for respiratory diseases for First Nations people was highest for those aged 65 and over (84 per 1,000), followed by those aged 0–4 (68 per 1,000).
- The age-standardised hospitalisation rate due to respiratory diseases for First Nations people decreased in 2019–20 and 2020–21, but increased in 2021–22 and 2022–23.
- The age-standardised hospitalisation rates due to respiratory diseases decreased faster for non-Indigenous Australians compared with First Nations people (23% decline compared with 10%), resulting in a widening of the gap (increasing from 19 per 1,000 in 2016–17 to 22 per 1,000 in 2022–23).
Research and evaluation findings
- Early-life exposures – such as tobacco smoke, poor housing, air pollution, and limited access to medicines – can impair lung development and contribute to lifelong and intergenerational respiratory disease risk, including COPD and bronchiectasis.
- Vaccination programs have reduced bacterial pneumonia hospitalisations, but environmental factors continue to drive high disease rates.
- Bronchiectasis and COPD are more common and more severe among First Nations adults, often co-occurring and linked to high smoking rates.
- A place-based, co-designed and strengths-based approach to public health strategies is essential in ensuring the social determinants and risk factors exacerbating CRDs are addressed, including improving living conditions, and reducing smoking.
Implications
Much of the respiratory disease burden among First Nations people is preventable through targeted public health strategies that address smoking (including second-hand smoke), immunisation, living conditions and overcrowded housing. Culturally appropriate communication and access to culturally safe primary health care are vital to ensure First Nations people feel comfortable participating in disease prevention and medical therapies for acute and chronic respiratory illnesses.
The National Strategic Action Plan for Lung Conditions focuses on reducing lung disease burden, recognising First Nations people as a priority. It emphasises prevention, early diagnosis, equitable access to care, and research to improve outcomes for conditions like COPD, lung cancer, and respiratory infections. The National Immunisation Strategy for Australia 2025–2030 aims to improve equitable access to immunisation for First Nations people across the life course by partnering with communities and co-designing strategies to improve access, including the use of innovative service delivery.
Why is it important?
Respiratory diseases, such as asthma, chronic obstructive pulmonary disease (COPD, including chronic bronchitis and emphysema), pneumonia, influenza and invasive pneumococcal disease, are a major cause of poor health and death for Aboriginal and Torres Strait Islander (First Nations) people. Drivers for respiratory diseases in First Nations communities include age, genetics, inadequate nutrition and sedentary behaviour, tobacco use, environmental conditions, occupational exposures and hazards, and health conditions.
Respiratory health inequities are shaped by historical and ongoing impacts of colonisation, including intergenerational trauma, racism, and social disadvantage. Social determinants such as household crowding, poor housing infrastructure, early childhood infections, tobacco exposure, and limited access to health care are particularly evident in remote areas and non-urban First Nations communities (Griffiths 2016; Paradies 2016). Respiratory disease patterns also differ by remoteness, with non-remote areas reporting higher rates of asthma, hay fever and chronic sinusitis due to greater exposure to pollen and air pollution and better access to diagnostic services, while remote areas face under-reporting linked to limited health care access and lower health literacy but higher respiratory disease death rates (ABS 2024; Rheault et al. 2019; Russell et al. 2025; Salimi et al. 2018). These social and environmental conditions have led to persistently higher rates of chronic respiratory diseases (CRDs) and hospitalisation compared to non-Indigenous Australians (Bush et al. 2024). Asthma, the most commonly reported CRD, affects around 17% of First Nations people, is more commonly reported in non-remote (18%) areas than remote areas (8%) and is associated with higher rates of poor health, emergency department presentations and hospitalisation (ABS 2024; AIHW 2023b).
Smoking is the leading contributor to CRDs, accounting for 47% of the respiratory disease burden among First Nations people (AIHW 2022). COPD, linked to smoking and lung cancer risk, is more prevalent and severe in First Nations patients, often with co-existing bronchiectasis (AIHW 2019). Pneumonia risk is heightened by poor living conditions, malnutrition, smoking, and alcohol use, with mortality highest in older adults and those with comorbidities (Aliberti et al. 2021) These studies highlight the need to focus resources on reducing smoking rates and improving primary health care (see measure 2.15 Tobacco use). Acute lower respiratory infections remain a major cause of hospitalisation for First Nations children, especially in remote communities and among preterm or low birthweight infants (Binks et al. 2020).
The COVID-19 pandemic highlighted the health inequities for First Nations people. Early protective measures and community-led responses kept initial mortality low (AIHW 2023a), but underlying risk of severe illness persisted due to the prevalence of chronic disease, multimorbidity, smoking, overcrowded housing, and limited access to culturally appropriate care. Historic inequities, trauma, and distrust of services left First Nations communities highly vulnerable, underscoring the need for targeted, culturally responsive interventions (Yashadhana et al. 2020). Through strong collaboration between the Aboriginal Community Controlled Health sector and Australian governments, early responses helped protect communities (NACCHO n.d.); however, cases and deaths still rose as the pandemic progressed, with death rates for First Nations people 1.5 times higher than for non-Indigenous Australians between 2022 and 2025. In 2025, influenza caused more deaths among First Nations people than COVID-19 or respiratory syncytial virus (RSV), with only 22 COVID-19-related deaths recorded to November 2025 (ABS 2025). Tuberculosis (TB) also remains a significant concern, with incidence rates among Australian-born First Nations people exceeding those of Australian-born non-Indigenous Australians. This highlights the need for sustained surveillance and community-led strategies like the REACT Project, which aims to stop TB transmission through empowerment and culturally safe approaches (Devlin et al. 2019; NSW Health 2023).
Addressing the high burden of respiratory disease among First Nations people requires culturally appropriate health care interventions. Prevention efforts must explicitly focus on improving housing conditions and reducing tobacco use – two of the most significant modifiable risk factors. While smoking rates among First Nations people have declined over the past two decades the reduction has not been as substantial as that seen in the general population, and rates remain disproportionately high (see measure 2.15 Tobacco use). Notably, smoking prevalence in remote areas has remained largely unchanged, highlighting persistent inequities. A place-based, co-designed and strengths based approach to public health strategies is essential in ensuring the social determinants and risk factors exacerbating CRDs are addressed, including improving living conditions, and reducing smoking. The increasing use of e-cigarettes (or vaping device) is a growing concern, with rates highest for First Nations people in non-remote areas (ABS 2024).
By partnering with First Nations health experts and organisations, governments can fund culturally safe, accessible and trauma-informed services that contribute towards reducing the impact of CRD. Enhanced access to vaccinations for infectious respiratory disease such as influenza and pneumococcal disease, and access to early treatment, can also lower the risk of severe illness and improve the health of First Nations communities.
Burden of disease
In 2018, respiratory diseases caused an estimated 17,920 years of healthy life lost due to illness and or death (17,920 Disability-Adjusted Life Years or DALY) (excludes acute infections such as influenza) – accounting for 7.5% of the total burden of disease for Indigenous Australians.
Respiratory diseases accounted for 9% of the total non-fatal burden (years lived in ill health or with disability (YLD)) for Indigenous Australians and 5.8% of the fatal burden (premature death (YLL)).
Of the total burden due to respiratory diseases, a larger proportion was experienced by Indigenous females (54%) than Indigenous males (46%). Asthma was the leading cause of respiratory burden among Indigenous Australians under 45 years (80% of total respiratory burden for this age group), while COPD was the leading cause of respiratory burden for those aged 45 and older (65% of total respiratory burden for this age group) (AIHW 2022).
The age-standardised burden due to respiratory diseases for Indigenous Australians was 2.7 times the rate for non-Indigenous Australians (AIHW 2022).
Between 2003 and 2018, the age-standardised rate of total burden due to respiratory diseases for Indigenous Australians decreased slightly (from 38 to 34 DALY per 1,000 people). This was driven by a decrease in the fatal burden, mainly from COPD. The rate of non-fatal burden due to respiratory diseases remained relatively stable (20 and 19 YLD per 1,000, respectively) (AIHW 2022).
Data findings
Deaths from respiratory diseases
Deaths data in this measure are sourced from the National Mortality Database. The data are used to report the total number of deaths in Australia (nationally), which includes Australian residents of all states and territories. However, when reporting death rates, data have been limited to 5 jurisdictions (New South Wales, Queensland, Western Australia, South Australia and the Northern Territory), in which the quality of Indigenous status identification in the deaths data is considered adequate. National death rates are not published due to concerns around the quality of Indigenous status identification in Victoria, Tasmania and the Australian Capital Territory.
When reporting death rates by remoteness, data from all jurisdictions has been included.
Nationally, over the 5-year period 2019–2023, there were 2,095 deaths of First Nations people that were due to respiratory disease.
Over the same period, in the 5 jurisdictions with adequate Indigenous status identification, there were 1,871 deaths of First Nations people due to respiratory diseases, corresponding to a rate of 43 deaths per 100,000 population. First Nations males and females each accounted for around 50% (951 and 920, respectively) of these deaths and rates of death were similar between the sexes (44 compared with 43 per 100,000). Respiratory diseases were the fourth leading cause of death among First Nations people, accounting for 9% of all deaths (Table D1.23.1).
Among First Nations people, the death rate due to respiratory diseases was highest for those in the Northern Territory (67 per 100,000), followed by South Australia (53 per 100,000), New South Wales (47 per 100,000), Western Australia (37 per 100,000) and was lowest in Queensland (34 per 100,000). Respiratory diseases accounted for a higher proportion of total deaths in New South Wales and South Australia (both 11%) than in the other three jurisdictions (Table D1.23.2).
In 2019–2023, among First Nations people in the 5 jurisdictions with adequate Indigenous status identification, the specific leading causes of death due to respiratory disease were:
- chronic obstructive pulmonary disease (COPD), which accounted for 68% (1,270 deaths) of all respiratory disease deaths
- influenza and pneumonia – 14% (or 256 deaths) and
- asthma, which accounted for a further 5% (or 84 deaths) of all respiratory disease deaths.
Looking at the specific leading causes of respiratory disease deaths, rates of death due to COPD and influenza and pneumonia were similar between First Nations males and females. For deaths due to asthma and bronchiectasis the rate was higher for First Nations females than males (relative differences of 1.4 and 1.3, respectively) while the death rate due to pulmonary oedema and other interstitial pulmonary diseases was higher for males (relative difference of 2.1) (Table D1.23.14, Figure 1.04.1).
Figure 1.04.1: Death rates due to specific respiratory diseases among First Nations people, by sex, NSW, Qld, WA, SA and NT, 2019–2023
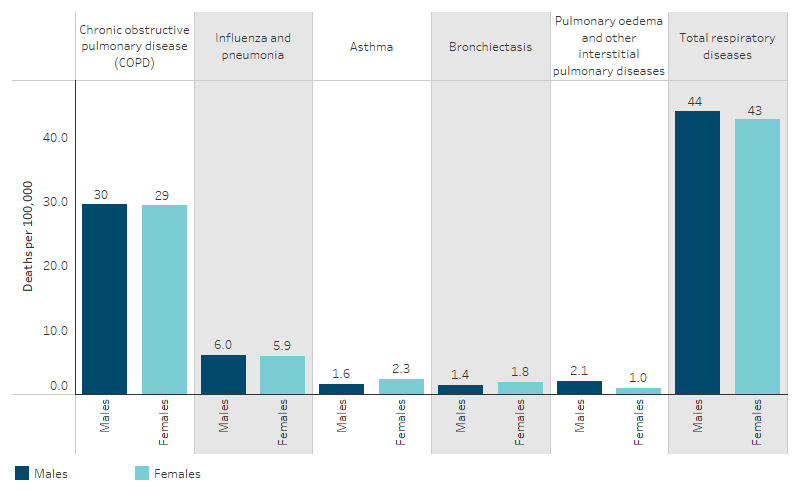
Source: Table D1.23.14. AIHW National Mortality Database.
In the 5-year period 2019–2023 in the 5 jurisdictions with adequate Indigenous status identification, deaths due to respiratory diseases increased with age for First Nations people, with those aged 65 and over accounting for 59% of all deaths. The death rate due to respiratory diseases was lowest for First Nations people aged 0–34 (1.9 deaths per 100,000 population) and increased in each subsequent 10-year age group to a high of 829 per 100,000 for those aged 75 and over (Table D1.23.15, Figure 1.04.2).
Figure 1.04.2: Death rates due to respiratory diseases for First Nations people, by age, NSW, Qld, WA, SA and NT, 2019–2023
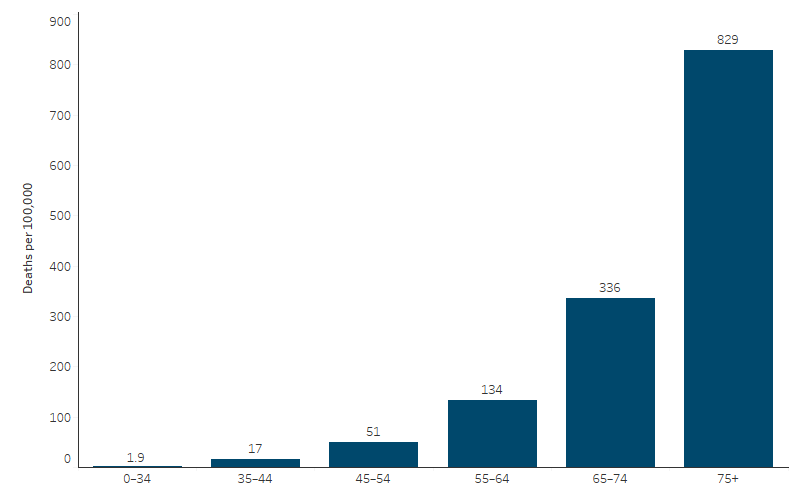
Source: Table D1.23.15. AIHW National Mortality Database.
For First Nations people aged 0–34, asthma was the leading cause of deaths accounting for 31% of all respiratory disease deaths in this age group (17 deaths, a rate of 0.6 deaths per 100,000 population). For those aged over 35, COPD was the leading cause of death accounting for a higher proportion of all respiratory disease deaths in each 10-year age group up to 65–74. COPD accounted for 39% of all respiratory disease deaths for those aged 35–44 and 77% of deaths for those aged 65–74 (Table D1.23.15).
Coronavirus disease 2019 (COVID-19) is a respiratory illness caused by infection with the SARS-CoV-2 virus. COVID-19 was declared to be a pandemic by the World Health Organization on 11 March 2020. Over the 4-year period 2020–2023, in the 5 jurisdictions with adequate Indigenous status identification, there were 241 deaths of First Nations people due to COVID-19, corresponding to a crude death rate of 6.9 deaths per 100,000 population (a 4-year period is used to present COVID-19 deaths data instead of the usual 5-year period for other deaths data due to the timing of the pandemic). The rate of COVID-19 deaths was highest among those aged 75 and over (109 deaths, a rate of 201 deaths per 100,000 population), followed by those aged 70–74 (22 deaths, 41 deaths per 100,000) (Table D1.04.22).
In 2019–2023, the proportion of total deaths among First Nations people that were due to respiratory diseases were similar in non-remote and remote areas (9% for Major cities, Inner regional and Outer regional areas combined, compared with 8% in Remote and Very remote areas combined). However, the rate of deaths due to respiratory disease in remote areas was 1.5 times as high as the rate in non-remote areas (44 compared with 29 per 100,000, respectively) (Table D1.23.30).
After adjusting for differences in the age structure between the two populations, in 2019–2023:
- The respiratory disease death rate was 2.2 times as high for First Nations people as for non-Indigenous Australians.
- In remote areas, the death rate from respiratory diseases for First Nations people was 2.6 times that of non-Indigenous Australians, while in non-remote areas, the rate for First Nations people was 1.9 times that of non-Indigenous Australians.
- The rate of deaths due to COPD for First Nations people was 3.1 times that of non-Indigenous Australians.
- Rates of deaths due to asthma and bronchiectasis were 2.4 and 2.5 times higher for First Nations people respectively than for non-Indigenous Australians (Table D1.23.30, Table D1.23.14).
In the 4 year-period 2020–2023 in the 5 jurisdictions with adequate Indigenous status identification, the rate of deaths due to COVID-19 among First Nations people was 1.5 times the rate for non-Indigenous Australians, after adjusting for differences in the age-structure of the two populations (age-standardised rates of 17 compared with 11 per 100,000, respectively) (Table D1.04.22).
Prevalence from the ABS survey
Reported data on respiratory diseases is available from the 2022–23 National Aboriginal and Torres Strait Islander Health Survey (NATSIHS). Estimates of respiratory disease from the 2022–23 NATSIHS may have been impacted by a change in collection methodology which may affect the number of persons reporting emphysema. For more information see 2022–23 National Aboriginal and Torres Strait Islander Health Survey Methodology.
Based on these data, in 2022–23, an estimated 31% (310,900) of First Nations people had a respiratory disease lasting or likely to last 6 months or more (Table D1.04.2). The most commonly reported conditions were hay fever and allergic rhinitis (19%), asthma (17%), chronic sinusitis (8.5%) and chronic obstructive pulmonary disease (COPD) (2.1%) (Table D1.04.21, Figure 1.04.3).
Figure 1.04.3: Proportion of First Nations people reporting respiratory disease, by type, 2022–23
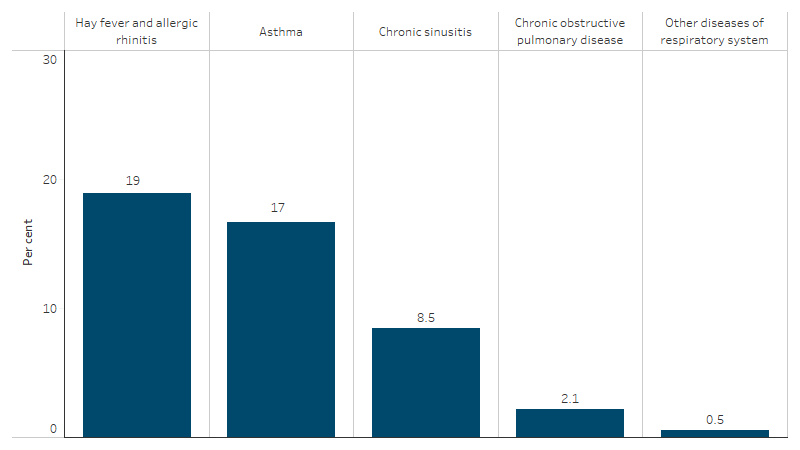
Notes
1. The Chronic Obstructive Pulmonary Disease (COPD) category includes chronic bronchitis, emphysema and chronic airflow limitation. Asthma is reported separately. Other diseases of respiratory system include influenza and pneumonia, asbestosis, acute bronchiolitis, other diseases of the respiratory system, and breathing difficulties or shortness of breath.
2. Estimates for First Nations people may have been impacted by a change in collection methodology which may affect the number of persons reporting emphysema. For more information see 2022–23 National Aboriginal and Torres Strait Islander Health Survey Methodology.
Source: Table D1.04.21. National Aboriginal and Torres Strait Islander Health Survey 2022–23.
In 2022–23, based on self-report, the rate of respiratory disease was lowest for First Nations people aged 0–14 (18%), and ranged between 33% (for those aged 25–34), and 44% (45–54) in the other age groups (Table D1.04.2).
First Nations people living in non-remote areas reported a higher rate of respiratory disease (34%) than those in remote areas (16%). By jurisdiction, First Nations people living in Victoria reported the highest rate (43%), while those in the Northern Territory reported the lowest (16%) (Table D1.04.2).
First Nations people living in remote areas were less likely to report asthma (8%) than those in non-remote areas (18%) (Table D1.04.20).
By jurisdiction, in 2022–23, the highest rates of asthma were reported by First Nations people in Victoria (24%), with the lowest in the Northern Territory (8%). By age, asthma prevalence was higher in older age groups, with rates of 12% and 13% for ages 0–14 and 15–24 respectively, compared with 26% for ages 45–54 and 25% for ages 55 and over (Table D1.04.20).
In 2022–23, of First Nations people who still get asthma or have had symptoms in the last 12 months, 38% had a written asthma action plan, and 36% indicated that their asthma got worse or out of control in the last 12 months. From the latter group, two out of three (64%) reported they did not go to hospital after asthma got worse. Of those with asthma or symptoms in the last 12 months, two out of three (65%) reported using asthma medication within the last 2 weeks (Table D1.04.20).
After adjusting for differences in the age structure between the two populations, the proportion of First Nations people and non-Indigenous Australians reporting respiratory disease was similar (35% and 33% respectively) (Table D1.04.3). However:
- Asthma prevalence for First Nations people was 1.8 times the rate of non-Indigenous Australians (19% and 11%, respectively).
- COPD prevalence was 1.3 times higher (3% and 2%, respectively).
- Chronic sinusitis prevalence was 1.3 times higher (10% and 8%, respectively).
- Hay fever and allergic rhinitis prevalence was lower for First Nations people, at a ratio of 0.9 (21% and 24%, respectively) (Table D1.04.21).
Hospitalisations
Hospitalisation statistics are a measure of the occurrence of conditions requiring acute care. It is important to note that levels of hospital use do not necessarily reflect prevalence or incidence of diseases in the community.
Between July 2021 and June 2023, there were 59,271 hospitalisations (a rate of 30 per 1,000 population) with a principal diagnosis of respiratory disease among First Nations people (8.1% of total First Nations hospitalisations, excluding care involving dialysis) (Table D1.02.5).
The hospitalisation rate for respiratory diseases for First Nations people was highest for those aged 65 and over (84 hospitalisations per 1,000 population), followed by children aged 0–4 (68 per 1,000) (Table D1.04.8, Figure 1.04.4).
Figure 1.04.4: Age-specific hospitalisation rates for diseases of the respiratory system (based on principal diagnosis), by Indigenous status and age, Australia, July 2021 to June 2023
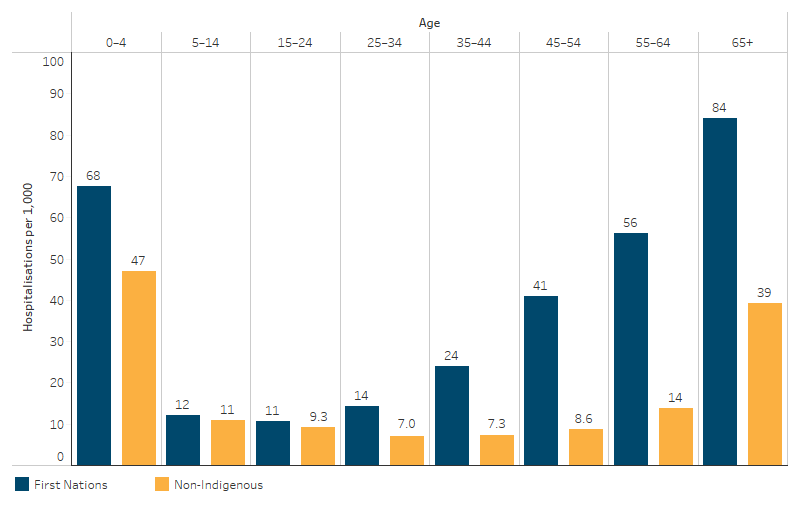
Source: Table D1.04.8. AIHW analysis of National Hospital Morbidity Database.
Across all age groups, the hospitalisation rate for respiratory diseases was higher for First Nations people than for non-Indigenous Australians (Table D1.04.8, Figure 1.04.4). The largest relative difference was among those aged 45–54, where the rate for First Nations people was 4.8 times the rate for non-Indigenous Australians.
After adjusting for differences in the age structure between the two populations, the hospitalisation rate of First Nations people for respiratory diseases was 2.3 times the rate for non-Indigenous Australians (Table D1.04.7).
Between July 2021 and June 2023, pneumonia accounted for 21% of respiratory disease hospitalisations for First Nations people, with COPD accounting for a further 18% (Table D1.04.10).
First Nations people had higher rates of hospitalisation than non-Indigenous Australians for COPD (ratio 5.7), influenza (ratio 3.9), pneumonia (ratio of 2.8), bronchiectasis (ratio 2.7), and asthma (ratio 1.9), while the rate of hospitalisation due to chronic sinusitis was lower (ratio 0.7). The largest gaps, based on difference in hospitalisation rates for respiratory disease between First Nations people and non-Indigenous Australians were for COPD (a difference of 7.6 per 1,000) and pneumonia (a difference of 5.6 per 1,000) (Table D1.04.10).
First Nations people aged 35–44 were 25 times as likely as non-Indigenous Australians to be hospitalised for chronic obstructive pulmonary disease (3.5 and 0.1 per 1,000 respectively) (Table D1.04.16).
Looking at data by state and territory, the crude hospitalisation rate of First Nations people for respiratory diseases was highest in the Northern Territory (54 hospitalisations per 1,000 population) and lowest in Tasmania (15 per 1,000) (Table D1.04.7, Figure 1.04.5).
Figure 1.04.5: Hospitalisation rates for First Nations people for diseases of the respiratory system (based on principal diagnosis), by jurisdiction, Australia, July 2021 to June 2023
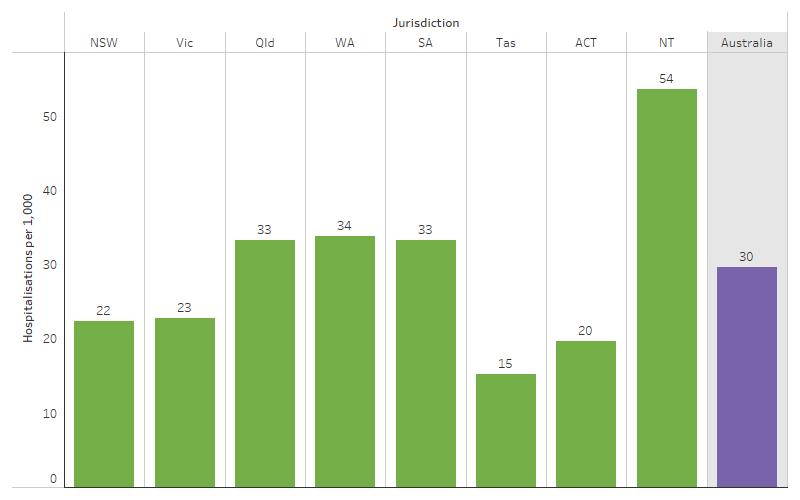
Source: Table D1.04.7. AIHW analysis of National Hospital Morbidity Database.
Between July 2021 and June 2023, across remoteness areas, First Nations people living in Remote and very remote areas were 2.2 times as likely to be hospitalised for respiratory diseases as First Nations people living in Major cities (51 and 24 hospitalisations per 1,000 population, respectively). Those living in Inner and outer regional areas had a similar rate to those in Major cities (27 per 1,000 population). In contrast, the rate was similar across remoteness areas for non-Indigenous Australians (Table D1.04.9, Figure 1.04.6).
Figure 1.04.6: Hospitalisations among First Nations people for diseases of the respiratory system (based on principal diagnosis), by remoteness, Australia, July 2021 to June 2023
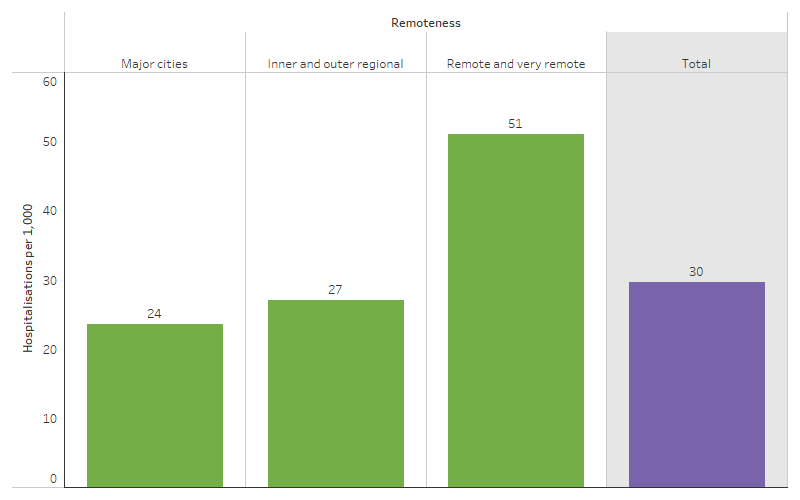
Source: Table D1.04.9. AIHW analysis of National Hospital Morbidity Database.
Considering age-standardised hospitalisation rates for respiratory diseases by jurisdiction and remoteness, the largest relative difference between First Nations people and non-Indigenous Australians was in Remote and very remote areas of Western Australia, followed by non-remote areas of the Northern Territory (where the rates for First Nations people were 4.7 times and 4.5 times the rates for non-Indigenous Australians, respectively) (Table D1.04.17).
Notifiable diseases
Notifiable diseases data are collected by states and territories under their public health legislation. This legislation requires medical practitioners, clinicians, laboratories and hospitals to notify health authorities of certain communicable and other diseases (DoH 2003).
Pneumococcal disease is a bacterial infection caused by Streptococcus pneumoniae infecting the respiratory tract, causing significant illness and death worldwide, especially in the very young, older people and those with predisposing risk factors (DoH 2022). In the 3-year period of 2021–2023 there were 643 notifications of invasive pneumococcal disease for First Nations people, representing 14% of all cases notified (Table D1.04.15).
Tuberculosis (TB) is a nationally notifiable disease in Australia and is reportable by states and territories to the National Notifiable Diseases Surveillance System. Australia has one of the lowest TB incidence rates globally at 6.1 notifications per 100,000 population in 2024–25, with people born overseas contributing to over 90% of these notifications. First Nations people and communities experience a disproportionate impact from TB, with a higher incidence rate in Australian-born First Nations populations than Australian-born non-Indigenous populations, at 3.4 notifications compared to 0.8 notifications per 100,000 population in 2024–25. The public health response to TB is led and coordinated by state and territory governments (DoHAC 2025a).
Change over time in deaths and hospitalisations
To describe trends in deaths and hospital data, linear regression has been used to calculate the per cent change over time. This means that information from all years of the specified time period are used, rather than only the first and last points in the series (see Statistical terms and methods).
Time series analysis of deaths data has been limited to the 2016 to 2021 period due to a break in time series for First Nations death statistics in New South Wales from 2022 (for more information see measure 1.22 All-cause age-standardised death rates and Data Sources and Quality).
Between 2016 and 2021, in the 5 jurisdictions combined (New South Wales, Queensland, Western Australia, South Australia and the Northern Territory), there was no significant change in the age-standardised death rate due to respiratory diseases for First Nations people, nor in the gap between First Nations people and non-Indigenous Australians (Table D1.23.21).
For hospitalisations, after adjusting for changes in the age-structure of the population over time, there is not a clear trend over the period. In 2019–20 and 2020–21 there was a decrease in the hospitalisation rate due to respiratory diseases for First Nations people, followed by an upward trend in 2021–22 and 2022–23 (Table D1.04.11, Figure 1.04.7).
The hospitalisation rate due to respiratory diseases for First Nations children aged 0–4 similarly decreased between 2018–19 and 2021–22 and was followed by upwards trend in 2022–23 (Table D1.04.12).
Based on linear regression, age-standardised hospitalisation rates due to respiratory diseases decreased faster for non-Indigenous Australians compared with First Nations people (23% decline compared with 10%), resulting in a widening of the gap (increasing from 19 per 1,000 in 2016–17 to 22 per 1,000 in 2022–23) (Table D1.04.11, Figure 1.04.7).
Figure 1.04.7: Age-standardised hospitalisation rates for diseases of the respiratory system (based on principal diagnosis), by Indigenous status, NSW, Vic, Qld, WA, SA and NT, 2016–17 to 2022–23
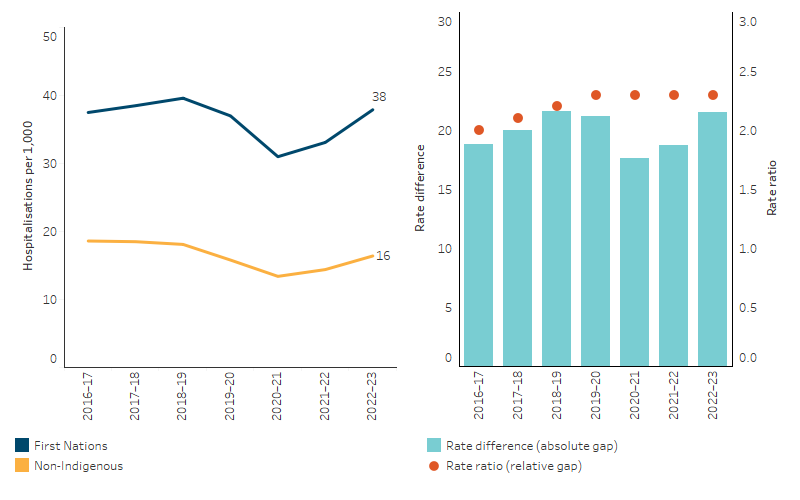
Note: Rate difference is the age-standardised rate (per 1,000) for First Nations people minus the age-standardised rate (per 1,000) for non-Indigenous Australians. Rate ratio is the age-standardised rate for First Nations people divided by the age-standardised rate for non-Indigenous Australians.
Source: Table D1.04.11. AIHW analysis of National Hospital Morbidity Database.
Research and evaluation findings
A recent overview of respiratory diseases in First Nations children found a lack of research among children living in urban and regional areas, as most research has been conducted in remote areas (Australian Indigenous HealthInfoNet 2020). The overview identified a 2013–2015 study of First Nations children who visited the Caboolture Community Medical clinic in northern Brisbane, which found that 33% had symptoms of an acute respiratory infection, and 22% went to the clinic specifically because of an acute respiratory infection (Hall et al. 2017). A subsequent study of mostly First Nations children who visited the Caboolture Community Medical clinic over a similar period in 2013–2015 found that, in an average month, about one-quarter of the children were attending the clinic with an acute respiratory infection with a cough. The study results indicated that one in five children will develop a chronic cough following acute respiratory infections with a cough. The overview also identified several community-based studies in remote areas. A 2010–2013 study of First Nations children from 25 remote communities in the Northern Territory found that 59% of children had a runny nose and 39% had a cough (Leach et al. 2016). Another study of First Nations children born between 2001 and 2006 in five remote communities in the Northern Territory found that by the time they turned one year old, 96% of babies had gone to their health service with at least one infection, many infections were recurrent, and infections of the upper respiratory tract were the most common (Kearns et al. 2013).
Hospitalisation rates for respiratory diseases among First Nations people are significantly higher in early childhood and older adulthood compared to non-Indigenous Australians. Children aged 0–4 are frequently admitted for pneumonia and bronchiolitis, largely due to overcrowded housing, poor indoor air quality, and early-life exposure to tobacco smoke – factors that impair lung development and increase lifelong risk of chronic disease (Binks et al. 2020; Laird et al. 2022). Among adults aged 35 years and older, chronic obstructive pulmonary disease (COPD) and bronchiectasis account for most hospitalisations, reflecting cumulative impacts of high smoking prevalence and recurrent infections (Howarth et al. 2024; Heraganahally et al. 2019). These patterns are further shaped by social determinants such as poverty, inadequate housing, and limited access to culturally safe care, particularly in remote areas (Meharg et al. 2025; Russell et al. 2025). Studies indicate that when COPD and bronchiectasis occur together, patients experience significantly worse lung function, more frequent exacerbations, and higher mortality rates (Polverino et al. 2018).
Bronchiectasis is also more common among First Nations patients (Kruavit et al. 2017). A Northern Territory study on bronchiectasis found that 87% of adult First Nations patients diagnosed with this chronic lung condition had at least one respiratory-related hospital admission between 2011 and 2020, averaging one admission per year. Co-morbid COPD was common, affecting 88% of hospitalised bronchiectasis patients, with nearly one-third requiring admission to the intensive care unit at some point. The study underscores the heavy burden of respiratory infections and chronic lung disease among First Nations people (Howarth et al. 2024).
The higher prevalence of asthma for First Nations people in non-remote areas may reflect environmental and social determinants of urban living, such as heightened exposure to vehicle exhaust, industrial pollution, and pollen allergens. For example, long-term environmental exposures in Sydney have shown weak positive associations with hospitalisation for asthma (Salimi et al. 2018), while Melbourne’s inner west has been linked to elevated childhood asthma risk due to the proximity of schools and childcare centres to high-traffic routes (Walter et al. 2024). Climate variability further shapes pollen dynamics, with Melbourne experiencing earlier and longer grass pollen seasons, increasing allergic rhinitis and asthma risks (Dhankhar et al. 2025). These findings align with international evidence that urban environments are associated with more severe and prolonged allergic symptoms compared to rural areas (Gledson et al. 2023).
However, the impact of asthma for First Nations people compared to non-Indigenous Australians is nonetheless evident in regional and remote settings, as illustrated by a recent study of emergency department presentations of asthma in 12 public hospitals in the Central Queensland Hospital and Health Service catchment area. The study found the incidence of asthma presentations for First Nations people was more than twice as high as for non-Indigenous people (Shifti et al. 2025).
A study in the Northern Territory found pulmonary cysts in 5% of First Nations people referred for lung function testing. Most affected individuals were male (65%), middle-aged (mean age: 49.9 years), and had a history of smoking, with moderate lung function impairment. Over half had multiple cysts (more than 5), often with bilateral involvement, and many also had concurrent emphysema or bronchiectasis. The cause of cystic lung disease in First Nations people remains unknown, highlighting the need for further research to determine if it is a distinct condition, a genetic predisposition, or an outcome of environmental and lifestyle factors. Improving diagnostic and management pathways is crucial to reduce respiratory illness and death in First Nations people (Mishra et al. 2024).
A population study of First Nations children in four remote Western Australian communities found high rates of chronic respiratory disease, with 17.9% of children having a chronic respiratory condition or abnormal lung function. Protracted bacterial bronchitis (PBB), chronic suppurative lung disease (CSLD), and bronchiectasis were common, affecting 12.2% of children. PBB was the most common diagnosis (7.7%), with CSLD (3.3%) and bronchiectasis (1.3%) also prevalent. Chronic wet cough, often a precursor to more severe conditions, became more common with age, and many cases of PBB were misdiagnosed as asthma, potentially delaying treatment and increasing the risk of disease progression. The findings highlight the urgent need for improved early detection and culturally appropriate management strategies to prevent long-term respiratory complications in First Nations children (Laird et al. 2022).
McCallum and colleagues conducted a review of studies from 1996 to 2017 in northern Australia, focusing on the prevalence of respiratory syncytial virus (RSV) in children, due to the high rate of respiratory disease in the region. The review included data from 11 prospective studies involving 1,127 children, predominantly First Nations (90%), with a median age of 1.8 years. RSV was the second most common virus after human rhinoviruses (HRV), with a prevalence of 15%. It was most prevalent in children under 2 years hospitalised with bronchiolitis (47%), especially those under 6 months. The study proposed that effective maternal and infant RSV vaccines could significantly reduce RSV bronchiolitis-related hospitalisations, particularly for First Nations infants from remote areas (McCallum et al. 2019). Since February 2025 the maternal RSV vaccine is free under the National Immunisation Program (NIP) (Butler 2025).
Universal pneumococcal conjugate vaccine (PCV) programs began for First Nations children in 2001 and all Australian children in 2005 (Meder et al. 2020). First Nations children are recommended to receive the 20-valent PCV at 2, 4, 6 and 12 months of age. First Nations children in the Northern Territory, Queensland, Western Australia and South Australia who have completed their age appropriate PCV schedule with only 13vPCV or 15vPCV are recommended to receive a single dose of 20vPCV at 4 years of age or 12 months after their last PCV dose, whichever is later (DoHAC 2026).An assessment of PCV’s impact on acute lower respiratory infection (ALRI) hospitalisations of First Nations infants in the Northern Territory from 2006 to 2015 found a 30% reduction in bacterial pneumonia hospitalisations during the 2011–2015 period with the 13-valent PCV. Despite this, one in five First Nations infants continued to be hospitalised with an ALRI within their first year of life, indicating the need for both environmental and biomedical approaches (Binks et al. 2020).
A study in the Northern Territory found that First Nations patients referred to respiratory specialist outreach teams in remote and rural communities have a significantly higher rate of smoking and COPD compared with non-Indigenous patients referred to this service. Bronchiectasis is also more common among First Nations patients (Kruavit et al. 2017). The study suggested there is a need to focus resources on reducing the rate of smoking in these areas, and further improve the quality of health care with a focus on primary health care. In addition to education provided by the respiratory outreach team, Aboriginal health workers could provide information on tobacco and quit support to the community. Another recent study conducted in the Top End of the Northern Territory found that First Nations patients with COPD had a higher prevalence of smoking, moderate to severe airflow obstruction on spirometry and were frequently co-diagnosed with bronchiectasis with increased severity of ventilatory impairment, compared with First Nations patients who did not have a diagnosis of COPD (Heraganahally et al. 2019).
The social determinants of respiratory health significantly impact outcomes from birth and throughout life. Adverse exposures before conception, during pregnancy, and in early childhood have lasting effects on lung function, contributing to diseases like asthma, COPD, bronchiectasis, and early mortality. These issues disproportionately affect populations of lower socioeconomic status, including First Nations people in Australia. Factors such as passive tobacco exposure, air pollution, poor housing conditions, and limited access to affordable medications contribute to lung health disparities. Climate change further exacerbates respiratory health issues for disadvantaged children. Early-life lung function impairment is influenced by intergenerational factors, including parental lung function and genetic predisposition. Reviews highlight the role of life-course determinants and early disadvantage (Bush et al. 2024; Howarth et al. 2023), while genetic studies confirm a strong heritable component (Shrine et al. 2023) and evidence from cohort studies shows that parental lung function not only predicts infant respiratory health but also demonstrates an influence beyond environmental factors, suggesting a genetic and physiological component in respiratory outcomes (van Putte-Katier et al. 2011).
Studies on respiratory disease services have shown positive outcomes. In Western Australia, an integrated COPD multidisciplinary community service reduced long-term respiratory hospitalisations (Chung et al. 2016). A large pilot study in Queensland highlighted the importance of working with communities and First Nations staff to develop and deliver a culturally appropriate and accessible specialist respiratory service (Medlin et al. 2014). The Indigenous Respiratory Outreach Care (IROC) program aims to provide culturally appropriate specialist respiratory outreach services and resources to First Nations people in rural and remote Queensland, improve access to specialist respiratory services, and increase lung health awareness. A study of children attending IROC clinics found significant lung function improvement for First Nations children with asthma and bronchiectasis (Collaro et al. 2020).
Poor housing conditions are associated with frequent respiratory health issues in young First Nations children. Increasing housing stock that meets local geographic, climatic, and cultural needs, along with solutions led and governed by First Nations communities are needed. Economic opportunities, eliminating food insecurity, and providing potable water will help communities maintain existing houses and improve overall health (Kovesi et al. 2022).
First Nations people experience higher death rates from acute respiratory diseases due to socioeconomic disadvantage, higher rates of chronic diseases, and barriers to accessing culturally safe health care. From 2022 to 2024, COVID-19 was the leading cause of acute respiratory infection related deaths, with 500 First Nations people having COVID-19 certified as a cause of death in that period (this includes people who died with COVID as a contributing factor), with an additional 22 deaths to November 2025. The COVID-19 death rate was 1.5 times higher for First Nations people than non-Indigenous Australians, with First Nations women experiencing a rate 2.3 times as high as non-Indigenous women. Additionally, deaths from influenza and RSV also disproportionately affected First Nations people, with the number of influenza-related deaths increasing in 2024 and 2025 compared with previous years (ABS 2025).
A review of the COVID-19 pandemic response highlighted First Nations communities in Australia as a global exemplar of self-determination achieving positive health outcomes. However, as the world transitioned to the endemic phase, the review identified the need to examine pandemic stressors' impacts on mental health and wellbeing. In April 2020, an initial roundtable of First Nations mental health leaders and allies provided key recommendations in response to the crisis. As the pandemic evolved, a second roundtable in December 2021 re-evaluated emerging challenges and actions needed to address them. The findings reinforce the global consensus on the importance of First Nations self-determination and emphasise four priority actions:
- Strengthening and funding Aboriginal Community Controlled Health Organisations to enhance empowerment and self-determination.
- Adopting strengths-based and culturally informed strategies addressing social and cultural determinants of social and emotional wellbeing.
- Implementing system changes for more effective responses to future pandemics.
- Delivering on the four Priority Reforms in the National Agreement on Closing the Gap, including formal partnerships, community-controlled sector growth, government transformation, and shared access to data.
The review underscores the ongoing need for governments to uphold these commitments to support First Nations communities’ holistic wellbeing and recovery post-pandemic (Dudgeon et al. 2023).
Implications
First Nations people continue to experience higher rates of respiratory diseases compared with non-Indigenous Australians. Chronic respiratory diseases (CRDs), particularly asthma and chronic obstructive pulmonary disease (COPD), remain significant contributors to the overall disease burden among First Nations communities (AIHW 2024). Chronic lower respiratory diseases are among the leading causes of death for First Nations people, alongside Ischaemic heart disease, diabetes, lung cancer, and intentional self-harm (see measure 1.23 Leading causes of death).
While effective management of CRDs is crucial, much of this burden is preventable. Public health approaches, including those in partnership with Aboriginal Community Controlled Health Organisations, are essential to prevent their occurrence. Initiatives addressing smoking (including second-hand smoke), immunisation, living conditions, overcrowded housing, chronic disease, and access to health care can significantly improve respiratory health (Hunt 2021a, 2021b; Johnston et al. 2010; Torzillo and Chang 2014). Culturally appropriate communication and health services are vital to ensure First Nations people feel comfortable participating in disease prevention and medical therapies.
The National Strategic Framework for Chronic Conditions offers comprehensive policy guidance for preventing, managing, and treating chronic conditions in Australia. It emphasises coordinated care, equity, and addressing social determinants of health to improve outcomes, particularly First Nations people. The framework prioritises person-centred care, prevention, and targeted interventions to reduce the burden of chronic diseases. Key strategies include integrating health-care services for holistic care, reducing health disparities by addressing social determinants like housing and education, tailoring health-care to meet individual needs, implementing proactive measures such as smoking cessation and immunisation, and developing strategies to address chronic diseases in vulnerable populations. By focusing on these areas, the framework aims to improve health outcomes and reduce the burden of chronic diseases, especially for First Nations communities.
The National Aboriginal and Torres Strait Islander Health Plan 2021–2031 (the Health Plan) emphasises self-determination, cultural safety, and community control in health policy, aligning with the National Agreement on Closing the Gap. The Indigenous Australians’ Health Programme (IAHP) supports Aboriginal Community Controlled Health Services (ACCHSs) and mainstream providers to improve primary health care access, chronic disease management, and workforce development. These policies and programs enhance prevention, early intervention, and culturally responsive care, ensuring equitable health outcomes for First Nations people.
The National Strategic Action Plan for Lung Conditions (Action Plan) provides direction for efforts to address lung disease and proposed six priority areas for action to reduce chronic lung disease, recognising First Nations people as a priority. It emphasised prevention, early diagnosis, equitable access to care, and research to improve outcomes for conditions like COPD, lung cancer, and respiratory infections. Recommended actions included addressing tobacco exposure, poor housing, and barriers to culturally safe health promotion and care. At that time in 2019, the Australian Government announced commitments of up to $4 million to support the Action Plan focused on training, education resources for professionals and patients, and awareness raising about occupational hazards and the benefits of immunisation for respiratory infections. This was in addition to investments in access to respiratory medicines through the Pharmaceutical Benefits Scheme (PBS) (Hunt 2019).
Australia, as a signatory to the World Health Organization Framework Convention on Tobacco Control (FCTC), is committed to reducing tobacco use and its associated health, social, and economic harms. The FCTC emphasises Indigenous participation in tobacco control and the effectiveness of measures like advertising bans, health warnings, public education, and access to cessation treatments. The Australian Government has been implementing policies to lower smoking rates, prevent tobacco-related harm, and support community-led initiatives (DoHAC 2025b). As a result, smoking among First Nations people has decreased. To ensure smoking continues to decrease in First Nations communities the Australian Government has committed to further measures in the National Tobacco Strategy 2023–2030.
The National Asthma Strategy 2018 aims to reduce the asthma burden, improve control, and optimise diagnosis and management. It aligns with broader national health policies, identifying First Nations people as a priority, due to their higher asthma rates and related mortality. The strategy focuses on self-management, access to culturally safe health care, community awareness, prevention efforts, research, workforce development, and improved data collection.
Improving respiratory disease outcomes for First Nations people requires integrated action across housing, behavioural risk factors, chronic disease management, and immunisation initiatives. Successful interventions to improve respiratory health outcomes for First Nations communities include the Indigenous Respiratory Outreach Care (IROC) program in Queensland, which provides culturally appropriate specialist respiratory services and has significantly improved lung function in children with asthma and bronchiectasis. The Tackling Indigenous Smoking (TIS) program focuses on reducing smoking rates through community-led initiatives, education, and support for smoking cessation. In Western Australia, an integrated COPD multidisciplinary community service has reduced long-term respiratory hospitalisations by offering comprehensive care and support. Effective chronic disease management is guided by the National Strategic Framework for Chronic Conditions, the Health Plan and the IAHP.
The National Immunisation Program (NIP) provides free vaccines, including pneumococcal and influenza vaccines to high-risk First Nations populations, helping reduce vaccine-preventable respiratory illnesses (AIHW 2025). In addition, monthly reporting on First Nations COVID-19 vaccination coverage is published by the Australian Government, providing national and state-level data to monitor uptake and identify gaps in access (DoHAC 2024). The National Immunisation Strategy for Australia 2025–2030 reinforces the need for culturally safe, innovative, community-led vaccine delivery, supporting ACCHSs to expand access to immunisation for First Nations people, particularly in remote and underserved areas (DoHDA 2025).
Australian born First Nations people experience greater incidence of Tuberculosis (TB) than Australian born non-Indigenous populations. The public health response to TB is led and coordinated by state and territory governments. The Australian Government is continuing to work with jurisdictions through the National Tuberculosis Advisory Committee to improve long-term outcomes for communities impacted by TB outbreaks, improve access to TB medicines for priority populations and strengthen TB epidemiological surveillance.
Addressing the need for housing will help reduce risks for respiratory disease. The Housing Sector Strengthening Plan (Housing-SSP) aims to improve housing conditions by supporting Aboriginal and Torres Strait Islander community-controlled housing organisations to address overcrowding and poor living conditions that contribute to respiratory infections and chronic lung disease. Together, these initiatives highlight the importance of culturally appropriate care, community involvement, and comprehensive strategies to address social determinants of health for improving respiratory outcomes for First Nations people (see measures 2.01 Housing; 2.02 Access to functional housing with utilities; 2.03 Environmental tobacco smoke; 2.15 Tobacco use; 3.02 Immunisation; 3.05 Chronic disease management).
References
-
ABS (Australian Bureau of Statistics) (2024) National Aboriginal and Torres Strait Islander Health Survey 2022–23, ABS website.
-
ABS (2025) Deaths due to acute respiratory infections in Australia, ABS, Australian Government, accessed 21 January 2025.
-
AIHW (Australian Institute of Health and Welfare) (2019) Chronic obstructive pulmonary disease (COPD), AIHW website.
-
AIHW (2022) Impact and causes of illness and death in Aboriginal and Torres Strait Islander people 2018, Australian Burden of Disease Study, AIHW, Australian Government, doi:10.25816/xd60-4366.
-
AIHW (2023a) 'Changes in Aboriginal and Torres Strait Islander people’s use of health services in the early part of the COVID-19 pandemic', in Australia’s health 2022: data insights, AIHW, Australian Government, doi:10.25816/ggvz-vr80.
-
AIHW (2023b) First Nations people with asthma, AIHW, Australian Government.
-
AIHW (2024) Aboriginal and Torres Strait Islander people: health and wellbeing of First Nations people, AIHW, Australian Government, accessed March 2025.
-
AIHW (2025) Fact sheet: vaccine preventable disease among First Nations people, AIHW, Australian Government.
-
Aliberti S, Cruz CSD, Amati F, Sotgiu G and Restrepo MI (2021) 'Community-acquired pneumonia', The Lancet, 398(10303):906–919, doi:10.1016/S0140-6736(21)00630-9.
-
Australian Indigenous HealthInfoNet (2020) Summary of respiratory diseases among Aboriginal and Torres Strait Islander children.
-
Binks MJ, Beissbarth J, Oguoma VM, Pizzutto SJ, Leach AJ, Smith-Vaughan HC, McHugh L, Andrews RM, Webby R and Morris PS (2020) 'Acute lower respiratory infections in Indigenous infants in Australia's Northern Territory across three eras of pneumococcal conjugate vaccine use (2006–15): a population-based cohort study', The Lancet Child & Adolescent Health, 4(6):425–434, doi:10.1016/S2352-4642(20)30090-0.
-
Bush A, Byrnes CA, Chan KC, Chang AB, Ferreira JC, Holden KA, Lovinsky-Desir S, Redding G, Singh V, Sinha IP and Zar HJ (2024) 'Social determinants of respiratory health from birth: still of concern in the 21st century?', European Respiratory Review, 33(172):230222, doi:10.1183/16000617.0222-2023.
-
Butler M (19 January 2025) Protection against RSV for mums and bubs with free vaccine available from 3 February [media release], Office of the Hon Mark Butler MP, Minister for Health and Ageing, Minister for Disability and the National Disability Insurance Scheme, Department of Health, Disability and Ageing, accessed 30 January 2026.
-
Chung LP, Lake F, Hyde E, McCamley C, Phuangmalai N, Lim M, Waterer G, Summers Q and Moodley Y (2016) 'Integrated multidisciplinary community service for chronic obstructive pulmonary disease reduces hospitalisations', Internal Medicine Journal, 46(4):427–434, doi:10.1111/imj.12984.
-
Collaro AJ, Chang AB, Marchant JM, Masters IB, Rodwell LT, Takken AJ and McElrea MS (2020) 'Culturally appropriate outreach specialist respiratory medical care improves the lung function of children in regional and remote Queensland', Lung, 198(2):361–369, doi:10.1007/s00408-020-00332-7.
-
Devlin S, MacLaren D, Massey PD, Widders R and Judd JA (2019) 'The missing voices of Indigenous Australians in the social, cultural and historical experiences of tuberculosis: a systematic and integrative review', BMJ Global Health, 4(6):e001794, doi:10.1136/bmjgh-2019-001794.
-
Dhankhar A, Darssan D, Dey S, Lampugnani ER, Haberle S, Katelaris C, Burton P, Nattala U and Osborne NJ (2025) 'Influence of ENSO, droughts, and temperature rise on pollen and pollen seasons in Australia', Science of The Total Environment, 975:179326, doi:10.1016/j.scitotenv.2025.179326.
-
DoH (Department of Health) (2003) Notifiable diseases surveillance, 1917 to 1991, DoH website.
-
DoH (2022) Invasive pneumococcal disease (IPD) in Australia [annual reports], DoH website, accessed 17 November 2025.
-
DoHAC (Department of Health and Aged Care) (2024) First Nations COVID-19 vaccination coverage reports, DoHAC website, accessed 20 November 2025.
-
DoHAC (2025a) The National Aboriginal and Torres Strait Islander Health Protection AHPC subcommittee, Australian Centre for Disease Control website.
-
DoHAC (2025b) WHO Framework Convention on Tobacco Control, DoHAC website.
-
DoHAC (2026) Aboriginal and Torres Strait Islander children are recommended to receive pneumococcal conjugate vaccine, DoHAC, Australian Immunisation Handbook website, accessed 30 January 2025.
-
DoHDA (Department of Health, Disability and Ageing) (2025) National Immunisation Strategy for Australia 2025–2030, Australian Centre for Disease Control website.
-
Dudgeon P, Collova JR, Derry K and Sutherland S (2023) 'Lessons learned during a rapidly evolving COVID-19 pandemic: Aboriginal and Torres Strait Islander-led mental health and wellbeing responses are key', International Journal of Environmental Research and Public Health, 20(3):2173, doi:10.3390/ijerph20032173.
-
Gledson A, Lowe D, Reani M, Topping D, Hall I, Cruickshank S, Harwood A, Woodcock J and Jay C (2023) 'A comparison of experience sampled hay fever symptom severity across rural and urban areas of the UK', Scientific Reports, 13:3060, doi:10.1038/s41598-023-30027-x.
-
Griffiths K (2016) 'How colonisation determines social justice and Indigenous health—a review of the literature', Journal of Population Research, 33:9–30, doi:10.1007/S12546-016-9164-1.
-
Hall KK, Chang AB, Anderson J, Dunbar M, Arnold D and O'Grady KAF (2017) 'Characteristics and respiratory risk profile of children aged less than 5 years presenting to an urban, Aboriginal‐friendly, comprehensive primary health practice in Australia', Journal of Paediatrics and Child Health, 53(7):636–643, doi:10.1111/jpc.13536.
-
Heraganahally SS, Wasgewatta SL, McNamara K, Eisemberg CC, Budd RC, Mehra S and Sajkov D (2019) 'Chronic obstructive pulmonary disease in Aboriginal patients of the Northern Territory of Australia: a landscape perspective', International Journal of Chronic Obstructive Pulmonary Disease, 14:2205–2217, doi:10.2147/COPD.S213947.
-
Howarth T, Gibbs C, Heraganahally SS and Abeyaratne A (2024) 'Hospital admission rates and related outcomes among adult Aboriginal Australians with bronchiectasis - a ten-year retrospective cohort study', BMC Pulmonary Medicine, 24(1):118, doi:10.1186/s12890-024-02909-x.
-
Howarth TP, Jersmann HP, Majoni SW, Mo L, Saad HB, Ford LP and Heraganahally SS (2023) 'The ‘ABC’ of respiratory disorders among adult Indigenous people: asthma, bronchiectasis and COPD among Aboriginal Australians–a systematic review', BMJ Open Respiratory Research, 10:e001738, doi:10.1136/bmjresp-2023-001738.
-
Hunt G (21 February 2019) National action on lung conditions to help millions of Australians [media release], Office of the Hon Greg Hunt, Former Minister for Health and Aged Care, Department of Health and Aged Care, Australian Government.
-
Hunt G (3 February 2021) COVID-19 vaccine rollout for regional, rural and remote Australians [media release], Office of the Hon Greg Hunt, Former Minister for Health and Aged Care, Department of Health and Aged Care, Australian Government.
-
Hunt G (31 May 2021) World No Tobacco Day 2021 – helping more Australians quit smoking [media release], Office of the Hon Greg Hunt, Former Minister for Health and Aged Care, Department of Health and Aged Care, Australian Government.
-
Johnston V, Walker N, Thomas DP, Glover M, Chang AB, Bullen C, Morris P, Brown N, Vander Hoorn S, Borland R, Segan C, Trenholme A, Mason T, Fenton D and Ellis K (2010) 'The study protocol for a randomized controlled trial of a family-centred tobacco control program about environmental tobacco smoke (ETS) to reduce respiratory illness in Indigenous infants', BMC Public Health, 10:114, doi:10.1186/1471-2458-10-114.
-
Kearns T, Clucas D, Connors C, Currie BJ, Carapetis JR and Andrews RM (2013) 'Clinic attendances during the first 12 months of life for Aboriginal children in five remote communities of northern Australia', PloS One, 8(3):e58231, doi:10.1371/journal.pone.0058231.
-
Kovesi T, Mallach G, Schreiber Y, McKay M, Lawlor G, Barrowman N, Tsampalieros A, Kulka R, Root A, Kelly L, Kirlew M and Miller JD (2022) 'Housing conditions and respiratory morbidity in Indigenous children in remote communities in Northwestern Ontario, Canada', Canadian Medical Association Journal, 194(3):E80–E88, doi:10.1503/cmaj.202465.
-
Kruavit A, Fox M, Pearson R and Heraganahally S (2017) 'Chronic respiratory disease in the regional and remote population of the Northern Territory Top End: a perspective from the specialist respiratory outreach service', Australian Journal of Rural Health, 25(5):275–284, doi:10.1111/ajr.12349.
-
Laird P, Ball N, Brahim S, Brown H, Chang AB, Cooper M, Cox D, Cox D, Crute S, Foong RE, Isaacs J, Jacky J, Lau G, McKinnon E, Scanlon A, Smith EF, Thomason S, Walker R and Schultz A (2022) 'Prevalence of chronic respiratory diseases in Aboriginal children: a whole population study', Pediatric Pulmonology, 57(12):3136–3144, doi:10.1002/ppul.26148.
-
Leach A, Wigger C, Beissbarth J, Woltring D, Andrews R, Chatfield M, Smith-Vaughan H and Morris P (2016) 'General health, otitis media, nasopharyngeal carriage and middle ear microbiology in Northern Territory Aboriginal children vaccinated during consecutive periods of 10-valent or 13-valent pneumococcal conjugate vaccines', International Journal of Pediatric Otorhinolaryngology, 86:224–232, doi:10.1016/j.ijporl.2016.05.011.
-
McCallum G, Grimwood K, Oguoma V, Leach A, Smith-Vaughan H, Versteegh L and Chang A (2019) 'The point prevalence of respiratory syncytial virus in hospital and community-based studies in children from Northern Australia: studies in a ‘high-risk’ population', Rural and Remote Health, 19(4):5267, doi:10.22605/RRH5267.
-
Meder KN, Jayasinghe S, Beard F, Dey A, Kirk M, Cook H, Strachan J, Sintchenko V, Smith H and Giele C (2020) 'Long-term impact of pneumococcal conjugate vaccines on invasive disease and pneumonia hospitalizations in Indigenous and non-Indigenous Australians', Clinical Infectious Diseases, 70(12):2607–2615, doi:10.1093/cid/ciz731.
-
Medlin LG, Chang AB, Fong K, Jackson R, Bishop P, Dent A, Hill DC, Vincent S and O'Grady KA (2014) 'Indigenous Respiratory Outreach Care: the first 18 months of a specialist respiratory outreach service to rural and remote Indigenous communities in Queensland, Australia', Australian Health Review, 38(4):447–453, doi:10.1071/ah13136.
-
Meharg DP, Pavlovic SP, Jenkins CR, Maguire GP, Jan S, Shaw T, Dennis SM, McKeough Z, Rambaldini B, Gwynne KG, McCowen D, Newman J, Longbottom H, Eades SJ, Chao J and Alison JA (2025) 'Scanning the respiratory service landscape in NSW-based Aboriginal Community Controlled Health Services', BMC Health Services Research, 25:1135, doi:10.1186/s12913-025-13361-w.
-
Mishra K, Fazal R, Howarth T, Mutai J, Doss AX and Heraganahally SS (2024) 'Cystic lung disease in adult Indigenous Australians in the Northern Territory of Australia', Journal of Medical Imaging and Radiation Oncology, 68(1):67–73, doi:10.1111/1754-9485.13593.
-
NACCHO (National Aboriginal Community Controlled Health Organisation) (n.d.) COVID-19, NACCHO website.
-
NSW Health (2023) NSW tuberculosis surveillance report 2023: Australian-born cases, NSW Health, Australian Government, accessed 30 October 2025.
-
Paradies Y (2016) 'Colonisation, racism and Indigenous health', Journal of Population Research, 33:83–96, doi:10.1007/s12546-016-9159-y.
-
Polverino E, Dimakou K, Hurst J, Martinez-Garcia M, Miravitlles M, Paggiaro P, Shteinberg M, Aliberti S and Chalmers JD (2018) 'The overlap between bronchiectasis and chronic airway diseases: state of the art and future directions', European Respiratory Journal, 52(3):1800328, doi:10.1183/13993003.00328-2018.
-
Rheault H, Coyer F, Jones L and Bonner A (2019) 'Health literacy in Indigenous people with chronic disease living in remote Australia', BMC Health Services Research, 19:523, doi:10.1186/s12913-019-4335-3.
-
Russell DJ, Humphreys J, Veginadu P, Mathew S, Williams R, Cooney S, Menezes L, Boffa J, Baghbanian V, Robinson A, Zhao Y, Ramjan M, DeMasi K, Murray W, Taylor S, Stephens D, Lawrence K and Wakerman J (2025) 'Remote health: what are the problems and what can we do about them? Insights from Australia', BMC Health Services Research, 25:641, doi:10.1186/s12913-025-12828-0.
-
Salimi F, Morgan G, Rolfe M, Samoli E, Cowie CT, Hanigan I, Knibbs L, Cope M, Johnston FH, Guo Y, Marks GB, Heyworth J and Jalaludin B (2018) 'Long-term exposure to low concentrations of air pollutants and hospitalisation for respiratory diseases: a prospective cohort study in Australia', Environment International, 121:415–420, doi:10.1016/j.envint.2018.08.050.
-
Shifti DM, Al Imam MH, Maresco-Pennisi D, Whitcombe R, Sly PD, Munns CF, Peters RL, Khandaker G and Koplin JJ (2025) 'Emergency department presentations related to asthma and allergic diseases in Central Queensland, Australia: a comparative analysis between First Nations Australians and Australians of other descents', BMJ Open, 15(3):e091482, doi:10.1136/bmjopen-2024-091482.
-
Shrine N, Izquierdo AG, Chen J, Packer R, Hall RJ, Guyatt AL, Batini C, Thompson RJ, Pavuluri C, Malik V, Hobbs BD, Moll M, Kim W, Tal-Singer R, Bakke P, Fawcett KA, John C, Coley K, Piga NN, Pozarickij A, Lin K, Millwood IY, Chen Z, Li L, China Kadoorie Biobank Collaborative Group, Wijnant SRA, Lahousse L, Brusselle G, Uitterlinden AG, Manichaikul A, Oelsner EC, Rich SS, Barr RG, Kerr SM, Vitart V, Brown MR, Wielscher M, Imboden M, Jeong A, Bartz TM, Gharib SA, Flexeder C, Karrasch S, Gieger C, Peters A, Stubbe B, Hu X, Ortega VE, Meyers DA, Bleecker ER, Gabriel SB, Gupta N, Smith AV, Luan Ja, Zhao J-H, Hansen AF, Langhammer A, Willer C, Bhatta L, Porteous D, Smith BH, Campbell A, Sofer T, Lee J, Daviglus ML, Yu B, Lim E, Xu H, O’Connor GT, Thareja G, Albagha OME, The Qatar Genome Program Research Consortium, Ismail SI, Al-Muftah W, Badji R, Mbarek H, Darwish D, Fadl T, Yasin H, Ennaifar M, Abdellatif R, Alkuwari F, Alvi M, Al-Sarraj Y, Saad C, Althani A, Fethnou E, Qafoud F, Alkhayat E, Afifi N, Tomei S, Liu W, Lorenz S, Syed N, Almabrazi H, Vempalli FR, Temanni R, Saqri TA, Khatib M, Hamza M, Zaid TA, El Khouly A, Pathare T, Poolat S, Al-Ali R, Al-Khodor S, Alshafai M, Badii R, Chouchane L, Estivill X, Fakhro K, Mokrab Y, Puthen JV, Tatari Z, Suhre K, Granell R, Faquih TO, Hiemstra PS, Slats AM, Mullin BH, Hui J, James A, Beilby J, Patasova K, Hysi P, Koskela JT, Wyss AB, Jin J, Sikdar S, Lee M, May-Wilson S, Pirastu N, Kentistou KA, Joshi PK, Timmers PRHJ, Williams AT, Free RC, Wang X, Morrison JL, Gilliland FD, Chen Z, Wang CA, Foong RE, Harris SE, Taylor A, Redmond P, Cook JP, Mahajan A, Lind L, Palviainen T, Lehtimäki T, Raitakari OT, Kaprio J, Rantanen T, Pietiläinen KH, Cox SR, Pennell CE, Hall GL, Gauderman WJ, Brightling C, Wilson JF, Vasankari T, Laitinen T, Salomaa V, Mook-Kanamori DO, Timpson NJ, Zeggini E, Dupuis J, Hayward C, Brumpton B, Langenberg C, Weiss S, Homuth G, Schmidt CO, Probst-Hensch N, Jarvelin M-R, Morrison AC, Polasek O, Rudan I, Lee J-H, Sayers I, Rawlins EL, Dudbridge F, Silverman EK, Strachan DP, Walters RG, Morris AP, London SJ, Cho MH, Wain LV, Hall IP and Tobin MD (2023) 'Multi-ancestry genome-wide association analyses improve resolution of genes and pathways influencing lung function and chronic obstructive pulmonary disease risk', Nature Genetics, 55(3):410–422, doi:10.1038/s41588-023-01314-0.
-
Torzillo PJ and Chang AB (2014) 'Acute respiratory infections among Indigenous children', Medical Journal of Australia, 200(10):559–560, doi:10.5694/mja14.00649.
-
van Putte-Katier N, Koopmans M, Uiterwaal CS, de Jong BM, Kimpen JL, Verheij TJ, Numans ME and van der Ent CK (2011) 'Relationship between parental lung function and their children's lung function early in life', European Respiratory Journal, 38(3):664–671, doi:10.1183/09031936.00034210.
-
Walter C, Sly PD, Head BW, Keogh D and Lansbury N (2024) 'Traffic-related air pollution and childhood asthma—are the risks appropriately migated in Australia?', Atmosphere, 15(7):842, doi:10.3390/atmos15070842.
-
Yashadhana A, Pollard-Wharton N, Zwi AB and Biles B (2020) 'Indigenous Australians at increased risk of COVID-19 due to existing health and socioeconomic inequities', The Lancet Regional Health West Pacific, 1:100007, doi:10.1016/j.lanwpc.2020.100007.

