Key messages
Why is it important?
Cardiovascular disease (CVD) is a leading cause of death and disease burden among Aboriginal and Torres Strait Islander (First Nations) people, with earlier onset and higher prevalence compared to non-Indigenous Australians. These disparities are shaped by behavioural risk factors – such as smoking, poor nutrition, and physical inactivity – that are themselves influenced by broader social determinants including poverty, racism, and limited access to culturally safe care.
Historical and ongoing impacts of colonisation, systemic exclusion, and intergenerational trauma continue to affect cardiovascular health outcomes. Primary health care plays a pivotal role in early detection and managing CVD related risks preventing advancement of disease. Better access to specialist cardiac care and improvements in acute care settings will improve the equitability of access to important CVD treatments and services for First Nations people.
Data findings
-
In the 5-year period 2019–2023 in the 5 jurisdictions with adequate Indigenous identification, cardiovascular disease (CVD) accounted for 4,283 deaths (21% of total deaths) among First Nations people. The leading specific causes of death from CVD were coronary heart disease, with 2,259 deaths (53%), and cerebrovascular disease, with 723 deaths (17%).
-
Over the same period, after adjusting for differences in age structure, the CVD death rate for First Nations people was 1.6 times the rate for non-Indigenous Australians, with a higher gap in remote areas (2.3 times as high).
-
From 2016 to 2021, there was no significant change in the age-standardised rates for deaths due to CVD among First Nations people.
-
Between July 2021 and June 2023, the hospitalisation rate due to CVD among First Nations people was 18 hospitalisations per 1,000 population, with similar rates for First Nations males (18 per 1,000) and First Nations females (17 per 1,000).
-
Over the same period, after adjusting for differences in the age structure between the two populations, the hospitalisation rate for CVD for First Nations people was 1.6 times the rate for non Indigenous Australians. The relative difference was highest in Remote and very remote areas (2.4 times the hospitalisation rate).
-
Nationally, age-standardised hospitalisation rates for First Nations people due to CVD remained similar between 2016–17 and 2022–23, however the relative difference in rates between First Nations and non-Indigenous Australians (rate ratio) increased from 1.4 in 2016–17 to 1.6 in 2022–23 and the absolute difference in rates (rate difference) increased from 8.3 to 11 per 100,000 population over the same period.
-
Results from the 2022–23 National Aboriginal and Torres Strait Islander Health Survey showed that among First Nations people aged 15 and over, 45% (34,200) of people with diabetes, 58% (7,600) of people with kidney disease, and 27% (40,500) of people with measured high blood pressure reported also having one or more long-term cardiovascular conditions.
-
Undiagnosed high blood pressure is a significant risk factor for CVD. In 2022–23, 80% of First Nations adults whose blood pressure was measured as high reported not knowing they had high blood pressure.
-
In 2021–23, after adjusting for differences in the age structure of the two populations, First Nations people who were hospitalised for coronary heart disease were less likely than non-Indigenous Australians to receive a coronary angiography – a diagnostic procedure (53% compared with 56%), or to receive a revascularisation procedure – surgical procedure to restore blood supply to the heart (29% compared with 32%).
Research and evaluation findings
-
Evidence strongly suggests changes are required across the health system to improve cultural safety and to make the health system more responsive to the needs of First Nations people, as well as making specialist care more accessible and affordable, particularly in regional and remote areas.
-
Improving cardiovascular outcomes for First Nations people requires a culturally safe, holistic approach – addressing prevention, mental health and social and emotional wellbeing, early detection, access to specialist care, coordinated services, and social determinants.
-
CVD risk calculators in general practice software often omit key factors and use outdated data, leading to underestimation of high-risk First Nations patients, with variation across systems. Improved governance and validated, culturally appropriate tools are needed to ensure accurate risk assessment.
-
There is evidence the Aboriginal Community Controlled Health Services (ACCHSs) primary health-care model has shown better outcomes in managing CVD risk compared to mainstream services.
-
Studies show systematic differences in hospital treatment, including lower rates of coronary procedures, stroke unit treatment and timely allied health assessments for First Nations patients. First Nations people are underrepresented in cardiac rehabilitation, despite its effectiveness in reducing mortality and improving outcomes.
-
Potentially preventable medication-related hospitalisations account for over one-third of CVD-related admissions among First Nations people, often due to inappropriate medicine use or underuse of recommended treatments. These gaps contribute to severe outcomes, including deaths within 30 days post-discharge, underscoring the need for culturally safe medication review and continuity of care.
-
The culturally responsive Work It Out program, a 12-week chronic condition self-management program implemented by ACCHSs, demonstrated significant improvements in key clinical outcome measures such as blood pressure, weight and a six-minute walk test. Improvements were most evident in clinical outcome measures that were responsive to exercise and behavioural change.
Implications
Reducing CVD disparities requires a holistic and integrated approach that addresses both medical and social determinants. This includes:
- targeted prevention and healthy lifestyle strategies for smoking, nutrition, physical activity
- culturally safe and comprehensive primary health care for CVD risk assessment, monitoring, and early detection and chronic disease management
- improved access to specialist cardiac care and improved access to appropriate acute care
- addressing systemic barriers such as racism, affordability, and geographic isolation.
National strategies such as the National Aboriginal and Torres Strait Islander Health Plan 2021–2031, the National Strategic Action Plan for Heart Disease and Stroke, and the Australian Guideline for Assessing and Managing CVD Risk provide frameworks to support these efforts. However, implementation challenges remain, particularly in service accessibility, cultural safety and data accuracy.
Why is it important?
Cardiovascular disease (CVD) refers to a group of conditions affecting the heart (cardio) and blood vessels (vascular), including coronary heart disease, stroke, peripheral arterial disease, and congenital heart defects. These conditions are often caused by blockages that restrict blood flow, leading to serious events such as heart attacks and strokes. Important behavioural risk factors include unhealthy diet, physical inactivity, smoking and harmful use of alcohol. However, these behaviours are not simply individual choices – they are shaped by broader social, economic, and environmental determinants. Factors such as poverty, chronic stress, food insecurity, and limited access to culturally safe health care services influence the ability to make and sustain healthy lifestyle changes. Environmental exposures like air pollution also contribute to disease risk and disease progression. These influences can lead to high blood pressure, elevated blood glucose, and high cholesterol, increasing the risk of heart failure and other complications. Addressing both individual behaviours and the underlying social determinants is essential to reducing the prevalence of CVD and improving heart health outcomes (WHO 2021).
The cardiovascular health of Aboriginal and Torres Strait Islander (First Nations) people must be understood within the historical and social context of colonisation, which brought dispossession, displacement, racism, and loss of culture, leading to entrenched disadvantage and intergenerational trauma. These legacies disrupted access to traditional foods and ways of living, contributing to socioeconomic inequality and a higher burden of chronic disease. Government policies and systemic exclusion have further shaped health behaviours and outcomes. Deprivation in early childhood development, education, employment, income, and community infrastructure continues to influence cardiovascular risk factors today (Merone et al. 2019).
Risk factors such as physical inactivity, obesity, diabetes, high blood pressure and tobacco smoking are more prevalent among First Nations people than non-Indigenous Australians (Merone et al. 2019). Tobacco smoking levels are high among First Nations adults, although rates have declined in recent years (AIHW 2024; Cho et al. 2024; Jeong et al. 2021) (see measure 2.15 Tobacco use).
Cardiovascular risk remains strongly linked to early-life disadvantage, where poorer socioeconomic conditions at birth can have harmful effects. While food insecurity in disadvantaged communities is associated with lower body mass index (BMI) in childhood, these same communities also experience high rates of obesity and malnutrition, creating a dual burden of underweight and overweight issues. Limited access to healthy food, limited health awareness, and environmental factors further complicate efforts to manage cardiovascular risk (Thurber and Bell 2019). Low socioeconomic status is linked to a higher risk of developing CVD and with lower chance of receiving appropriate treatment (Beard et al. 2008; Cunningham 2010).
International evidence highlights the importance of addressing individual behaviours, broader social determinants and health system factors – such as improving cultural safety and tackling structural racism, as crucial to improving heart health outcomes among socially disadvantaged and vulnerable populations (Chaturvedi et al. 2024; Powell-Wiley et al. 2022).
CVD is a major cause of illness and death among First Nations people, with higher rates and earlier onset compared with non-Indigenous Australians (see measure 1.23 Leading causes of death). Around three-quarters of First Nations adults under 35 have at least one CVD risk factor. Despite progress in improving access to cardiac-related health services and reducing mortality, significant disparities remain, especially in remote areas. Efforts to increase uptake of health assessments and adherence to secondary prevention medications have shown some success. Addressing these disparities requires a continued focus on culturally sensitive health care, better access to specialist cardiac care, and ongoing community engagement (AIHW 2024; NACCHO 2020).
CVD is more common among First Nations people compared with non-Indigenous Australians, with onset typically occurring 10 and 20 years earlier (AIHW 2015; Bradshaw et al. 2011; Brown 2012; Brown and Kritharides 2017; Katzenellenbogen et al. 2014). According to the 2018–19 National Aboriginal and Torres Strait Islander Health Survey (NATSIHS), First Nations children aged 2–14 were twice as likely to have a heart or cardiovascular disease compared with non-Indigenous children (ABS 2019). This early onset can lead to late presentation, delayed treatment, and poorer outcomes (Merone et al. 2019).
Mortality from heart disease also occurs at younger ages among First Nations people, with a significantly higher proportion of deaths in younger adults due to CVD compared to non-Indigenous Australians. While cardiovascular risk factor screening should commence from age 18, CVD risk assessments using the Australian cardiovascular disease risk calculator are not advised until age 30, potentially overlooking younger First Nations people at high risk. Structural and social determinants, such as social marginalisation, racism, and trauma contribute to disengagement from health care. Access to culturally safe services remains limited outside Aboriginal Community Controlled Health Services (ACCHSs), further exacerbating health inequities (Reath and O'Mara 2018).
Acute Rheumatic Fever (ARF) and Rheumatic Heart Disease (RHD) are preventable conditions that affect the heart valves. While rare in countries with strong housing standards and access to primary health care, these diseases remain common in First Nations communities in Australia. This is due to factors such as overcrowded and poor-quality housing, socioeconomic disadvantage, and barriers to accessing culturally safe and continuous primary health care. First Nations communities in Australia experience among the highest rates of ARF and RHD globally, comparable only to rates seen in developing countries (End Rheumatic Heart Disease Centre of Research Excellence 2021; Menzies School of Health Research 2024) (see measure 1.06 Acute rheumatic fever and rheumatic heart disease for more information).
CVD rarely occurs in isolation, with many First Nations people experiencing multimorbidity – the presence of two or more chronic conditions. Multimorbidity significantly increases the complexity of care and contributes to higher rates of hospitalisation and premature death (AIHW 2026a). Multimorbidity is around 2.5 times more common among First Nations people than non-Indigenous Australians, and is a key contributor to the higher mortality observed in this population (Randall et al. 2018).
First Nations people often face significant barriers in accessing health services compared to non-Indigenous Australians. These barriers include inaccessibility, unaffordability, lack of cultural safety, long travel distances (especially in rural and remote areas) and previous experiences of racism and discrimination in health care environments. The unaffordability of care is becoming increasingly critical, with many mainstream general practices transitioning to private billing models. In some areas, the out-of-pocket costs – or ‘gap fees’ – can be two to three times higher than charges under previous billing models, further discouraging First Nations people from accessing essential GP services. Combined with transport challenges and limited availability of ACCHSs, this raises serious concerns about how First Nations people will access basic health care. Addressing these systemic barriers is essential to achieving Target 1 of the National Agreement on Closing the Gap: closing the gap in life expectancy within a generation, by 2031.
Burden of disease
In 2018, CVD was the third leading cause of total disease burden (‘disability adjusted life years’ – DALY) among First Nations people, accounting for 10% (24,612 DALY) of the total disease burden, 19% of fatal burden (premature death – 21,266 ‘years of life lost’ or YLL), and 2.6% of non-fatal burden (living with illness or disability – 3,346 YLD). Most of the burden due to CVD was fatal (86%), with 14% being non-fatal.
Coronary heart disease and stroke were the main causes of the total CVD burden (57% and 13%, respectively). This varied by age group. Among First Nations children under 5 years, inflammatory heart disease was the leading cause of CVD burden (40% of CVD burden). For ages 5–14, rheumatic heart disease and non-rheumatic valvular disease were the leading causes of burden (46% and 21%, respectively). For those aged 15–24, rheumatic heart disease was the leading cause of burden (25%), while coronary heart disease accounted for over half the CVD burden in those aged 25 and over.
The age-standardised rate of CVD burden for First Nations people was 2.4 times the rate for non-Indigenous Australians and was the second leading cause of the gap in disease burden between First Nations people and non-Indigenous Australians (14% of the total gap) (AIHW 2022b).
Data findings
Deaths from cardiovascular disease
Deaths data in this measure are sourced from the National Mortality Database. The data are used to report the total number of deaths nationally, which includes Australian residents of all states and territories. However, when reporting death rates, data have been limited to 5 jurisdictions (New South Wales, Queensland, Western Australia, South Australia and the Northern Territory) in which the quality of Indigenous status identification in the deaths data is considered adequate. National death rates are not published due to concerns around the quality of Indigenous status identification in Victoria, Tasmania and the Australian Capital Territory.
Data in this measure are presented by both broad and specific cause of death. Broad causes of death are grouped by International Classification of Diseases (ICD-10) chapters, which classify deaths based on disease type, affected body system, or the circumstances causing death. Specific causes of death, used for more detailed analysis like identifying leading causes, combine chapters, blocks, and individual diseases to better reflect health priorities and reduce ambiguity, following WHO guidelines adapted for the Australian context (see Becker et al. 2006). See Deaths in Australia (AIHW) for more information.
Nationally, in the period 2019–2023 there were 4,728 deaths due to cardiovascular disease (CVD) among First Nations people, of which 56% were among First Nations males and 44% among First Nations females.
In the 5-year period 2019–2023 for the 5 jurisdictions with adequate Indigenous identification, among First Nations people:
- CVD was the second broad leading cause of death accounting for 4,283 deaths (21% of total deaths) (Table D1.23.1). Of these, 56% were deaths of First Nations males.
- The rate of deaths due to CVD among First Nations people was 99 deaths per 100,000 population, with a higher rate for males than females (110 compared with 88 per 100,000, respectively).
- The leading specific causes of death from CVD were coronary heart disease, with 2,259 deaths (53%), and cerebrovascular disease, with 723 deaths (17%) (Table D1.23.8).
Between 2019 and 2023, the death rate due to CVD among First Nations people was lower in non-remote areas (Major cities, Inner regional and Outer regional areas combined) (63 per 100,000) than in remote areas (Remote and Very remote areas combined) (127 per 100,000) (Table D1.23.30).
Hospitalisations due to cardiovascular disease
Between July 2021 and June 2023, there were 35,425 hospitalisations for First Nations people with a principal diagnosis of CVD. It contributed to 2.8% of all hospitalisations of First Nations people (including care involving dialysis) (Table D1.02.5).
The hospitalisation rate due to CVD among First Nations people was 18 hospitalisations per 1,000 population, with similar rates for First Nations males (18 per 1,000) and First Nations females (17 per 1,000).
Hospitalisation rates for CVD increased with age and were highest among First Nations people aged 65 and over (93 per 1,000), with First Nations men aged over 45 experiencing higher rates of hospitalisation than First Nations women (Table D1.05.6, Figure 1.05.1).
Figure 1.05.1: Hospitalisation rates for cardiovascular disease (based on principal diagnosis) for First Nations people, by sex and age, Australia, July 2021 to June 2023
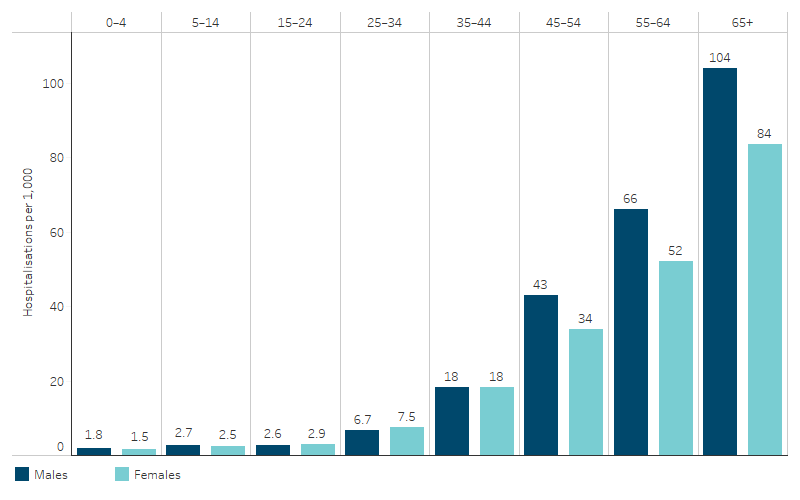
Source: Table D1.05.6. AIHW analysis of National Hospital Morbidity Database.
By remoteness, the hospitalisation rate for CVD for First Nations people was lower in Major cities and Inner and outer regional areas (13 and 17 per 1,000 respectively) than in Remote and very remote areas (30 per 1,000) (Table D1.05.8).
Hospitalisation rates for CVD for First Nations people also varied by jurisdiction – the lowest was 11 per 1,000 in Tasmania, and the highest was 33 per 1,000 in the Northern Territory (Table D1.05.7).
Between July 2021 and June 2023, of the 35,425 hospitalisations for CVD among First Nations people:
- 32% (11,293 hospitalisations, a rate of 5.6 per 1,000) were due to ‘other forms of heart disease’, which includes atrial fibrillation and flutter, and heart failure.
- Heart failure, which occurs when the heart is unable to pump blood to meet the body’s needs (AIHW 2025a), was the principal diagnosis for 13% of CVD hospitalisations (4,624 hospitalisations, a rate of 2.3 per 1,000).
- Atrial fibrillation and flutter, which is a disturbance of the electrical system of the heart (AIHW 2020), was the principal diagnosis for 7.9% of CVD hospitalisations (2,816 hospitalisations, a rate of 1.4 per 1,000).
- 31% (10,982 hospitalisations, a rate of 5.5 per 1,000) were due to coronary (or ischaemic) heart disease. Coronary heart disease is due to blockages in the heart’s own (coronary) arteries, with two main clinical forms being angina and heart attack (AIHW 2025a).
- Heart attack (acute myocardial infarction) was the principal diagnosis for 17% of CVD hospitalisations (5,996 hospitalisations, a rate of 3.0 per 1,000).
- 12% (4,204 hospitalisations, a rate of 2.1 per 1,000) were due to cerebrovascular disease, which is any disorder of the blood vessels supplying the brain or its covering membranes (AIHW 2025a).
- One major form of cerebrovascular disease is stroke, which occurs when a blood vessel supplying blood to the brain either suddenly becomes blocked (ischaemic stroke) or ruptures and begins to bleed (haemorrhagic stroke) (AIHW 2025a). Stroke was the principal diagnosis of 10% of CVD hospitalisations (3,651 hospitalisations, a rate of 1.8 per 1,000) (Table D1.05.9, Figure 1.05.2).
Figure 1.05.2: Hospitalisation rates for cardiovascular disease (based on principal diagnosis) for First Nations people, by disease type, Australia, July 2021 to June 2023
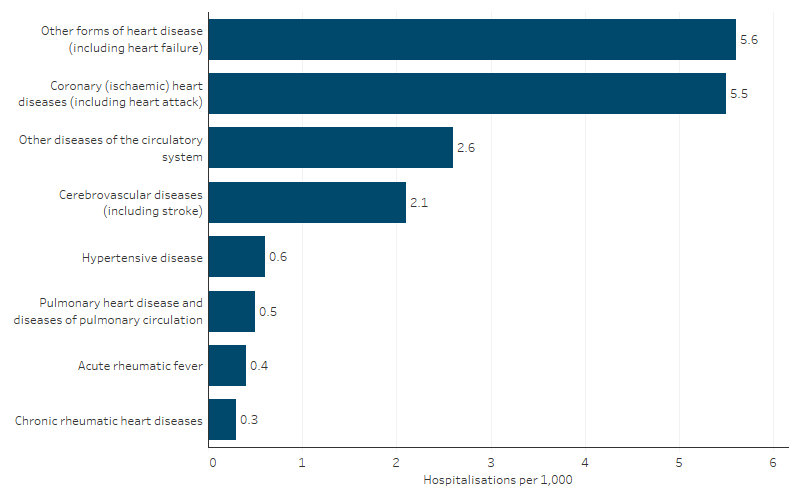
Source: Table D1.05.9. AIHW analysis of National Hospital Morbidity Database.
In 2021–23, after adjusting for differences in the age structure between the two populations, First Nations people who were hospitalised for coronary heart disease were less likely to receive a coronary angiography (a diagnostic procedure) than non-Indigenous Australians (53% compared with 56%, a ratio of 0.9 based on age-standardised rates), and less likely to receive a revascularisation procedure (surgical procedure to restore blood supply to the heart) (29% compared with 32%, a ratio of 0.9) (see also measure 3.06 Access to hospital procedures) (Table D3.06.9).
The age-standardised proportion of First Nations adults hospitalised for a heart attack who received an angiography or revascularisation procedure increased from 35% in 2006–07 to 65% in 2020–21. This is lower than the proportion for non-Indigenous adults in 2020–21 (76%). This was for New South Wales, Victoria, Queensland, Western Australia, South Australia and the Northern Territory combined (AIHW 2024).
Primary health care data
Information on cardiovascular risk assessments for First Nations people attending First Nations specific primary health care organisations is available using data from the national Key Performance Indicators (nKPI). At 30 June 2025, 55% (or around 65,000) of First Nations regular clients aged 35–74 with no known history of CVD had the necessary risk factors recorded within the previous 24 months to assess their absolute CVD risk. This has increased from 47% in December 2022 (AIHW 2026a, 2026b). There is limited information available about primary health care for CVD for First Nations patients visiting mainstream practices (that is, practices other than First Nations specific primary health care organisations). Previously, information was sourced from the Bettering the Evaluation and Care of Health survey, however this has now ceased.
MedicineInsight is another valuable data collection that provides longitudinal surveillance data of GP services and medicine prescriptions. In 2020¬–21, for every 100 GP clinical encounters with First Nations patients, 3 had a record of cardiovascular diseases (including coronary artery disease, peripheral vascular disease, atrial fibrillation, heart failure, stroke and transient ischaemic attack). These encounters resulted in 41,722 issued prescriptions and 222,019 total prescriptions (issued and repeated prescription) of medicines for First Nations patients with CVD. That contributed to 13% and 23% of all issued and total prescriptions for First Nations patients, respectively (NPS MedicineWise 2022).
Findings from ABS survey data
Based on reported data from the 2022–23 National Aboriginal and Torres Strait Islander Health Survey (NATSIHS) (ABS 2024a), 14% (136,100) of First Nations people had cardiovascular conditions (Table D1.05.1). First Nations people were 1.3 times as likely as non-Indigenous Australians to report having cardiovascular conditions, based on age-standardised rates (Table D1.05.2).
Looking at subcategories of CVD, among First Nations people in 2022–23, an estimated:
- 4.0% (39,600) had heart, stroke and vascular disease: this includes people who had ischaemic heart diseases (angina, heart attack and other ischaemic heart diseases), cerebrovascular diseases (stroke and other cerebrovascular diseases), oedema, heart failure, and diseases of the arteries, arterioles and capillaries.
- 8.1% (80,800) had high blood pressure (hypertension) (see also measure 1.07 High blood pressure). High blood pressure is a major risk factor for stroke, coronary heart disease, heart failure, as well as chronic kidney disease.
- 5.1% (51,000) had other diseases of the circulatory system: this includes any cardiovascular diseases not included in the categories above, such as tachycardia, low blood pressure, and cardiac murmurs (ABS 2024b: Tables 5.1 and 5.3).
In 2022–23, reported rates for CVD increased with age, and were higher for First Nations people than non-Indigenous Australians in every age group, though the difference was only statistically significant in the 15–24 and 45–54 age groups (Table D1.05.2, Figure 1.05.3).
Figure 1.05.3: Persons reporting cardiovascular disease, by Indigenous status and age, 2022–23
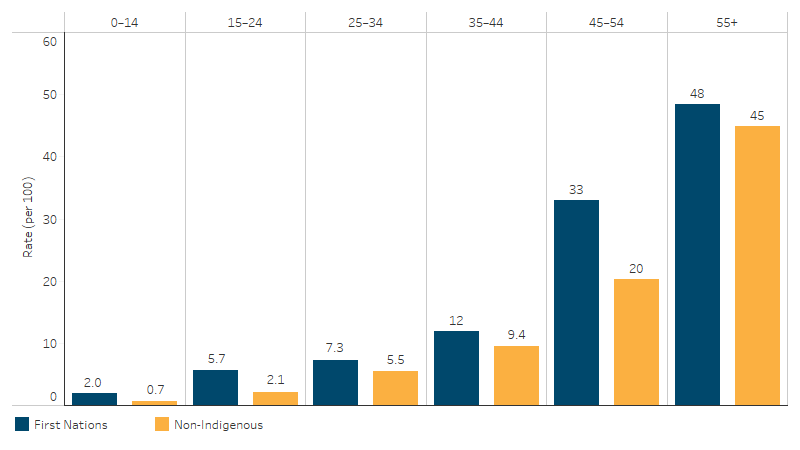
Source: Table D1.05.2. AIHW and ABS analysis of National Aboriginal and Torres Strait Islander Health Survey 2022–23 and National Health Survey 2022.
Cardiovascular disease was reported at similar rates by First Nations males (14%) and First Nations females (14%) (Table D1.05.1).
First Nations people living in remote areas reported higher rates of cardiovascular conditions (16%, 24,400 people), compared with those in non-remote areas (13%, 111,600 people). Across jurisdictions, the proportion of First Nations people reporting heart or cardiovascular conditions ranged between 12% (in Western Australia) and 20% (in South Australia) (Table D1.05.1).
In 2022–23, First Nations people who were aged 15 and over and living in the lowest equivalised household income quintile were 1.6 times as likely to report having heart or cardiovascular conditions as those in the highest equivalised household income quintiles (4th and 5th quintiles) (22% compared with 14%). First Nations people who had completed schooling to Year 9 or below were also more likely to report having CVD (31%) compared with those who completed Year 12 (12%) (Table D1.05.3).
Results from the 2022–23 NATSIHS showed that among First Nations people aged 15 and over, 45% (34,200) of people with diabetes, 58% (7,600) of people with kidney disease, and 27% (40,500) of people with measured high blood pressure reported also having cardiovascular conditions (Table D1.05.4). Undiagnosed high blood pressure is of particular concern as a risk factor for CVD given 80% of First Nations adults whose blood pressure was measured as high in 2022–23 reported not knowing they had high blood pressure (see measure 1.07 High blood pressure) (Table D1.07.2).
Comparisons with non-Indigenous Australians
Deaths from cardiovascular disease
In the 5-year period 2019–2023 for the 5 jurisdictions with adequate Indigenous identification, after adjusting for differences in the age structure between the two populations, the CVD death rate for First Nations people was 1.6 times the rate for non-Indigenous Australians (Table D1.23.1). The gap was higher in remote areas, where the rate of death due to CVD among First Nations people was 2.3 times the rate for non-Indigenous Australians (Table D1.23.30).
Cardiovascular diseases were the leading broad cause of the gap in death rates between First Nations people and non-Indigenous Australians in 2019–2023 (21% of the total gap in age-standardised death rates) (Table D1.23.1). Coronary heart disease was the largest contributor to the gap in CVD deaths (67% of gap) (Table D1.23.8).
Hospitalisation due to cardiovascular disease
After adjusting for differences in the age structure between the two populations, the hospitalisation rate for CVD for First Nations people was 1.6 times the rate for non Indigenous Australians (Table D1.05.7).
The relative difference between the two population groups was highest in Remote and very remote areas, where the age-standardised rate for First Nations people was 2.4 times the rate for non-Indigenous Australians, compared with 1.4 and 1.5 for Major cities and Inner and outer regional areas respectively (Table D1.05.8).
Changes over time in deaths
Time series analysis has been limited to the period 2016 to 2021 for New South Wales and for the 5 jurisdictions combined. This is due to the changes in the derivation of Indigenous status in deaths data, and to changes in population data. Data for Queensland, Western Australia, South Australia and the Northern Territory are available for the period 2016 to 2023 (for more information see measure 1.22 All-cause age-standardised death rates and Data sources and quality).
From 2016 to 2021, there was no significant change in the age-standardised rates for deaths due to CVD among First Nations people in New South Wales nor the 5 jurisdictions combined. In contrast, for non-Indigenous Australians the age-standardised rates for CVD deaths decreased by 20% in both New South Wales and the 5 jurisdictions combined. Despite this, there was no statistically significant change in the gap between First Nations people and non-Indigenous Australians from 2016 to 2021 (Table D1.23.18, Figure 1.05.4).
For First Nations people, across the whole period from 2016 to 2023, the age-standardised rate of deaths due to CVD did not significantly change in Queensland, Western Australia, South Australia or the Northern Territory. Among non-Indigenous Australians the age-standardised death rate decreased in all 4 jurisdictions, with declines ranging between 20% (Western Australia) and 32% (Northern Territory) (Table D1.23.28).
Figure 1.05.4: Age-standardised death rates due to cardiovascular disease, by Indigenous status, NSW, Qld, WA, SA and NT, 2016 to 2023
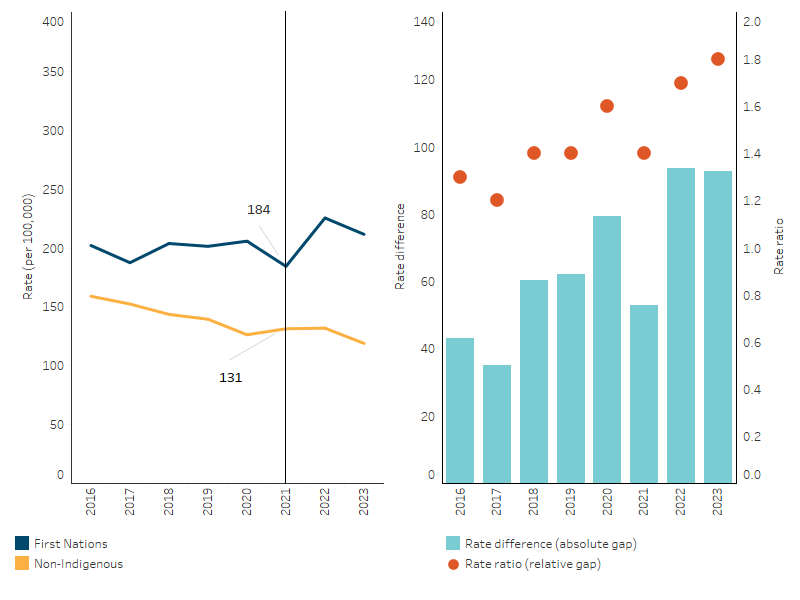
Notes
1. Rate difference is the age-standardised rate (per 100,000) for First Nations people minus the age-standardised rate (per 100,000) for non-Indigenous Australians. Rate ratio is the age-standardised rate for First Nations people divided by the age-standardised rate for non-Indigenous Australians.
2. Caution should be used when interpreting changes in death rates over time due to a break in the series in 2021 (see measure 1.22 All-cause age-standardised death rates and Data sources and quality).
Source: Table D1.23.18. AIHW National Mortality Database.
Changes over time in hospitalisations
Nationally, age-standardised hospitalisation rates for First Nations people due to CVD remained similar between 2016–17 and 2022–23. Hospitalisations of First Nations males for CVD increased by 5% over this period, while hospitalisations for First Nations females decreased by 4%. For non-Indigenous Australians during this same period, the rate decreased by 14%.
From 2016–17 to 2022–23, the relative difference in rates between First Nations and non-Indigenous Australians (rate ratio) increased from 1.4 in 2016–17 to 1.6 in 2022–23. The absolute difference in rates (rate difference) increased from 8.3 to 11 per 1,000 population over this same period (Table D1.05.11, Figure 1.05.5).
Figure 1.05.5: Age-standardised hospitalisation rates for a principal diagnosis of cardiovascular disease, by Indigenous status, Australia, 2016–17 to 2022–23
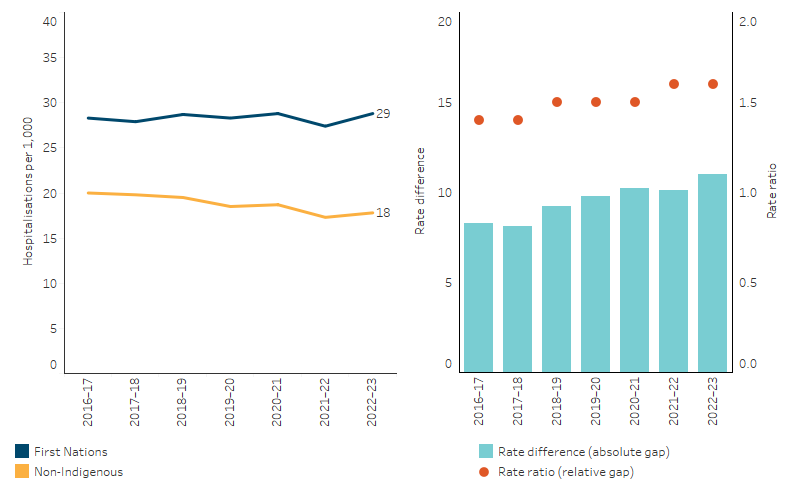
Note: Rate difference is the age-standardised rate (per 1,000) for First Nations people minus the age-standardised rate (per 1,000) for non-Indigenous Australians. Rate ratio is the age-standardised rate for First Nations people divided by the age-standardised rate for non-Indigenous Australians.
Source: Table D1.05.11. AIHW analysis of National Hospital Morbidity Database.
For hospitalisations with a principal diagnosis of coronary heart disease:
- Age-standardised rate for First Nations people decreased by 15% over the period 2016–17 and 2022–23, with First Nations females experiencing a larger decrease than First Nations males (20% and 11% respectively).
- Over this same period, the rate of hospitalisation for coronary heart disease for non-Indigenous Australians decreased by 19% (Table D1.05.13).
For hospitalisations with a principal diagnosis of cerebrovascular disease:
- Age-standardised rate for First Nations people increased by 19% over the period 2016–17 and 2022–23, with both First Nations males and First Nations females showing similar increases (19% and 20% respectively).
- Over this same period, the rate of hospitalisation for cerebrovascular disease for non-Indigenous Australians decreased by 11% (Table D1.05.14).
Research and evaluation findings
Social determinants and remoteness
International studies highlight the significant role of social determinants in shaping cardiovascular disease (CVD) outcomes. Factors such as socioeconomic status, education, neighbourhood and physical environment, employment, and social support networks profoundly impact cardiovascular health. Addressing structural racism and its impact on these social determinants is essential for reducing CVD disparities (Chaturvedi et al. 2024; Javed et al. 2022; Powell-Wiley et al. 2022).
Analysis of CVD events and outcomes for First Nations people across selected Melbourne hospitals (2011–2019) found that the median age at first CVD event was around 60 years, occurring 11 years earlier than for non-Indigenous patients. Coronary heart disease was the most frequent CVD event, with social determinants of health playing a significant role, as more than half of First Nations patients lived in the two lowest socioeconomic quintiles (Price et al. 2024).
Coronary (ischaemic) heart disease outcomes are consistently worse outside major cities in the general Australian population. However, among First Nations populations, differences by remoteness are less pronounced, with some coronary heart disease outcomes not associated with remoteness (Alston et al. 2017). Another study found a lack of clarity among policy makers at the local, state and federal levels of government in Australia regarding responsibility for implementing evidence-based policy to address CVD in rural areas, potentially contributing to limited policy action and persistent health disparities in rural areas (Alston et al. 2020).
CVD risk factor reduction
A systematic review of programs to improve cardiovascular health for First Nations people in Australia found studies of varying degrees of methodological quality. Interventions spanned across the disease continuum including healthy lifestyle promotion as well as disease management and treatment. There were varying degrees of effectiveness among the studies. Programs in the study had largely been designed within a mainstream health model with limited consideration to First Nations perspectives, but there was some evidence of effectiveness when interventions were integrated within primary health care and delivered in culturally appropriate ways including with active involvement from Aboriginal Health Workers, and by providing transport. There is a need for more rigorous evaluation of CVD programs for First Nations people (Mbuzi et al. 2018).
A review of 21 nutrition programs targeting CVD outcomes for First Nations people found that most programs reported improvements in measurable CVD risk factors, including reductions in body mass index (BMI), waist circumference, weight, blood pressure, and improved lipid profiles. Diet quality improvements were observed in some programs, primarily through increased consumption of fruits and vegetables, while others found significant improvements in fitness parameters and engagement in physical activity. Programs generally performed well in community engagement and capacity strengthening, though many lacked the inclusion of First Nations research paradigms, governance, and strengths-based approaches. The review highlights the need for future nutrition programs to be multifaceted, integrating both nutrition and physical activity to effectively improve CVD health outcomes (Porykali et al. 2021).
The Work It Out program, a 12-week chronic condition self-management program, was evaluated for its impact on clinical outcomes among urban First Nations adults with, or at risk of, CVD (Mills et al. 2017). Delivered in a culturally safe environment through Aboriginal Community Controlled Health Services (ACCHSs) in Southeast Queensland (2012–2014), the program combined yarning-based education with tailored group exercise. Participants attended flexible sessions to accommodate family and community responsibilities. The evaluation found improvements in walking distance, weight reduction for those with extreme obesity, and decreased systolic blood pressure. Additionally, participants with social and emotional wellbeing conditions reported notable benefits, warranting further investigation (Mills et al. 2017).
Primary health care
Culturally safe interventions are essential for improving cardiovascular health outcomes. Programs delivered by ACCHSs have demonstrated positive impacts on cardiovascular health by providing culturally informed, holistic health services that address both immediate health care needs and broader social determinants of health (Pearson et al. 2020).
There is evidence the ACCHS primary health care model has contributed to improved cardiovascular health outcomes for First Nations people (Campbell et al. 2018). Analysis of cardiovascular morbidity and mortality from 1995 to 2004 in a Northern Territory community where the sole provider of health care is an ACCHS found that, compared with all First Nations people in the Northern Territory, the community had lower mortality from all causes and from CVD and lower rates of hospitalisation with CVD as a primary cause. There was also a lower prevalence of diabetes, hypertension, obesity and smoking in the community. Rowley et al. (2008) concluded that a likely contributor was the nature of the primary health care services provided by the ACCHS, including regular outreach to outstation communities (Rowley et al. 2008).
Further evidence supporting the effectiveness of ACCHSs was found in the Treatment of cardiovascular Risk in Primary care using Electronic Decision SuppOrt (TORPEDO) study, a randomised controlled trial of the use of an electronic decision-support system measuring absolute cardiovascular risk, which showed that ACCHSs outperformed general practices in managing CVD risk (Peiris et al. 2015).
CVD risk assessment
The 2023 Australian guideline for assessing and managing cardiovascular disease risk provides updated evidence-based recommendations for the clinical assessment and management of CVD risk for primary prevention. It emphasises the importance of integrating multiple risk factors, including social and environmental determinants, to accurately predict CVD risk. The guideline introduces the new Aus CVD Risk Calculator and offers practical advice on assessing and managing CVD risk, with specific recommendations for First Nations people. This approach aims to improve shared decision-making, target pharmacotherapy effectively, and enhance clinical outcomes (Commonwealth of Australia as represented by the Department of Health and Aged Care 2023).
Agostino et al. (2020) recommended updated CVD risk assessment guidelines tailored for First Nations people, including lowering the screening age to 18 years to improve early detection and management. Given the persistent socioeconomic disadvantage and poor emotional wellbeing contributing to CVD disparities, the consensus statement emphasised the need to expand risk assessment beyond traditional biological markers (Agostino et al. 2020). However, an audit of CVD risk calculators embedded in Australian general practice clinical software products (CSPs) and a data extraction tool found significant implementation gaps in applying these guidelines. The study found that 80% of high-risk First Nations patients were identified through clinically determined high-risk conditions, yet some CSPs failed to include these variables, leading to substantial underestimation of high-risk patients. Analysis of 2020 national Key Performance Indicators (nKPI) data on CVD risk among First Nations people assessed in the previous two years revealed a three-fold variation in those identified as high risk across different systems (9.6% in one CSP versus 34.3% in another), with the largest discrepancies in younger age groups, where clinically determined high risk is particularly critical. Further, outdated clinical data, sometimes over 10 years old, was used in risk calculations, compromising accuracy. The study highlights the need for better governance of CVD risk algorithms, including a centralised, cloud-based tool to ensure validated, up-to-date risk assessments that address Indigenous data sovereignty, data management, and security considerations (Agostino et al. 2024).
Acute care and hospitalisation
The Lighthouse Hospital Project, previously funded through the Indigenous Australians’ Health Programme was a joint initiative between the Heart Foundation and the Australian Healthcare and Hospitals Association aimed at addressing institutional racism and improving CVD care for First Nations people. The project supported hospitals with governance frameworks, clinical quality improvements, and training to deliver culturally safe and clinically competent care. In 2017, phase three of the project expanded to 18 hospitals across Australia. Evaluations from this phase highlighted that more than three-quarters of First Nations people with acute coronary syndrome (ACS) rated their hospital experience as ‘very good’ or ‘good’ (Heart Foundation 2022), suggesting improvements in patient experience.
Spinks et al. (2025) found that potentially preventable medication-related hospitalisations (PPMRHs) in Queensland (2013–2017) contributed significantly to the CVD burden and mortality among First Nations people. More than one-third of CVD-related hospitalisations were potentially preventable, often linked to the use of medicines known to worsen heart conditions or the underuse of recommended cardiovascular treatments, such as lipid-lowering therapy. Critically, 136 deaths occurred within 30 days of hospital discharge following a PPMRH, reinforcing the severe health consequences of medication-related gaps in care (Spinks et al. 2025).
The Better Cardiac Care for Aboriginal and Torres Strait Islander People project tracks progress in reducing cardiac-related deaths and ill health among First Nations people. The eighth national report highlights improvements in access to cardiac-related health services for First Nations people.
Key improvements include:
- MBS-subsidised health assessments increased six-fold from 4% in 2006–07 to 24% in 2021–22. In 2018–19, nearly 9 in 10 First Nations people at high CVD risk had a blood pressure check, while smoking cessation discussions and secondary prevention medication use improved, though access remains lower in remote areas.
- Outcomes for acute coronary syndrome (ACS) improved from 2006–07 to 2020–21. First Nations patients receiving percutaneous coronary intervention (PCI) following a severe heart attack doubled (from 28% to 70%). However, in 2020–21, First Nations people were about 14% less likely to receive PCI than non-Indigenous Australians.
- In 2018–19, 97% of First Nations patients discharged from hospital with a cardiac condition were reviewed by a primary health care professional within 12 months and 87% of First Nations people discharged from hospital with acute coronary syndrome (ACS) in 2018–19 were on CVD medicines within 30 days.
- Chronic Disease Management follow-up service for First Nations people also rose from 42% in 2010–11 to 64% in 2018–19 (AIHW 2024).
Despite these improvements, access to cardiac-related diagnostic services has remained unchanged since 2006–07, and hospitalisation rates for cardiac conditions remain nearly double those of non-Indigenous Australians. In 2021–22, only 25% of First Nations patients with suspected or confirmed cardiac disease were reviewed by a cardiologist (AIHW 2024). The AIHW report does not detail the reasons for this low rate, but recent evaluations suggest contributing factors include cost, accessibility, and lack of culturally safe care. First Nations people are 2.8 times more likely to be hospitalised for heart failure, yet many live with undiagnosed conditions due to limited access to diagnostic tools and specialist follow-up (NACCHO 2025). Broader analyses also highlight geographic isolation, underfunding, and systemic issues in mainstream service delivery as key obstacles. The Core Services and Outcomes Framework emphasises the importance of culturally safe, community-led models, while the First Nations Health Funding Transition Program aims to shift service delivery to First Nations-led organisations to improve access and outcomes (DHDA 2025).
Linked data following 71,500 people for a year after a heart failure admission show that First Nations people made up 4% of the cohort (around 2,900 people), but a substantially higher proportion among those under 50 years of age (13% of males and 17% of females). They were more likely to have comorbidities such as type 2 diabetes, chronic kidney disease, chronic liver disease and Chronic Obstructive Pulmonary Disease (COPD). Readmissions within one year were higher among First Nations patients (64%), consistent with the compounding effects of multiple chronic conditions and lower continuity of care. Only 43% of First Nations patients had high continuity of care, compared with 59% of other Australians, with regional patterns showing lower post-discharge GP contact and continuity of care in Remote and Very remote areas. Additionally, 72% of First Nations patients attended an emergency department within a year, compared with 65% of other Australians, and were more likely to have at least one visit that did not result in a hospital admission. These findings highlight distinct disparities in post-hospital care patterns and comorbidity profiles among First Nations people with heart failure within the study cohort (AIHW 2025b).
Cardiac rehabilitation
Cardiac rehabilitation is an effective, evidence-based intervention that reduces recurrent events, readmissions and death. However, First Nations people remain under represented in cardiac rehabilitation, limiting the realisation of those benefits. For cardiac rehabilitation to deliver its full impact on cardiovascular health for First Nations communities, this requires culturally appropriate, patient centred models with clear health pathways and dedicated resources, alongside greater involvement of First Nations people and improved cultural awareness among non Indigenous staff (Field et al. 2018; Hamilton et al. 2016).
From October 2011 to July 2013, an evaluation was conducted for a cardiovascular and pulmonary rehabilitation program designed and provided by an ACCHS in Tasmania to First Nations people with diagnosed chronic heart or respiratory disease or at high risk of developing such conditions (Davey et al. 2014). The evaluation found that the program increased participation in rehabilitation and led to positive changes in health behaviours, exercise capacity and health related quality of life.
Barriers to improving First Nations access to cardiac rehabilitation include limited First Nations health workforce participation, poor cultural alignment of services, fragmented care pathways, and geographic isolation. National guidelines recommend culturally appropriate, flexible, and multidisciplinary models of care, with active involvement of Aboriginal Health Workers and communities. Improved data collection – including Indigenous status collection – is also recommended to monitor access and outcomes (Hayman et al. 2006; National Heart Foundation of Australia and Australian Cardiac Rehabilitation Association 2004).
The Aboriginal Healthy Hearts Feasibility Study evaluated a family-centred, outreach model of cardiac rehabilitation for First Nations people and their families in the Illawarra Shoalhaven region. The program included an intensive eight-week rehabilitation phase followed by follow-up appointments, focusing on exercise, nutrition, health education, and support for reducing tobacco and alcohol use. Delivered by Aboriginal Health Workers and a multidisciplinary team in community settings, the model aimed to improve program uptake and completion among First Nations patients discharged from hospital. The study also explored its potential to support secondary prevention of chronic diseases including diabetes, cancer, and kidney disease (Illawarra Shoalhaven Local Health District 2023).
Stroke
Stroke, a significant component of CVD, also occurs at disproportionately high rates among First Nations people compared with non-Indigenous Australians. This disparity is greater than that observed between Indigenous and non-Indigenous populations in other developed countries including the United States, Sweden/Norway and Singapore (Balabanski et al. 2024). Hospital outcomes for First Nations stroke patients are also poorer, with lower rates of stroke unit treatment, appropriate care, and timely allied health assessments (Kilkenny et al. 2013). Studies in the Northern Territory showed survival for stroke has improved among both non-Indigenous and First Nations people over time, from 1999–2011 by You et al. (2015); and from 1992–2013 by Zhao et al. (2015). However, the incidence rate did not change for First Nations or non-Indigenous Australians in the Northern Territory from 1999–2011 (You et al. 2015; Zhao et al. 2015).
Similarly, a study in a New South Wales rural referral hospital found that First Nations stroke patients were less likely than non-Indigenous patients to receive essential investigations, such as carotid imaging, or appropriate post-discharge follow-up. These findings highlight systemic failures in stroke care and reinforce the need for culturally safe health care environments, improved communication between non-Indigenous health professionals and First Nations patients, and innovative approaches such as community-based rehabilitation and telehealth (Blacker and Armstrong 2019; Tiedeman et al. 2019).
Implications
Cardiovascular disease (CVD) remains one of the leading causes of death among First Nations people. Some improvements in outcomes have been driven by reductions in smoking, improved management of high blood pressure and heart disease, and advancements in treatments for heart attack and stroke. However, the continued high prevalence of obesity, diabetes and chronic kidney disease threatens to slow or reverse these improvements. Smoking remains a critical issue and efforts to reduce smoking prevalence in remote areas have struggled to gain sufficient traction. This highlights the need for more effective, culturally responsive strategies to address tobacco use. Closing the gap in cardiovascular outcomes requires a holistic and integrated approach that combines medical and public health interventions. This includes targeted prevention strategies focused on smoking, nutrition, physical activity, and mental health and social and emotional wellbeing; improved early detection and access to specialist cardiac care; culturally safe and comprehensive primary health care; and better coordination across health services. Addressing the social determinants of health is also essential to tackling the root causes of CVD (DoH 2021).
Australia's Long Term National Health Plan includes a commitment to eradicate rheumatic heart disease by 2030 and identifies smoking, diabetes, and obesity as key contributors to CVD among First Nations people. The RACGP’s National Guide to Preventive Health Assessment for Aboriginal and Torres Strait Islander People provides clinical recommendations to support early detection and management of these risk factors through regular health checks and culturally safe care. These efforts are further supported by national investments in strengthening culturally safe primary health care and promoting community-led research to improve prevention, management, and outcomes for cardiovascular health and related chronic conditions.
The National Aboriginal and Torres Strait Islander Health Plan 2021–2031 (the Health Plan) provides an overarching policy framework to drive structural reform across the health system. Developed in partnership with First Nations health leaders and experts, it promotes prevention and early intervention, integration of primary, secondary, and tertiary health systems, and accountability to First Nations communities. The Health Plan aligns with the Priority Reforms of the National Agreement on Closing the Gap (National Agreement), focusing on:
- Locally Determined, Place-Based Approaches: Embedding multidisciplinary care and partnerships to ensure that health services are tailored to the specific needs of local communities.
- Strengthening ACCHS: Providing culturally safe, holistic, and affordable services through ACCHS to ensure early intervention across the life course.
- Eliminating Racism: Ensuring healthcare is culturally safe and responsive, addressing systemic racism within the health system.
- Enhanced Data Collection and Quality: Improving data collection to better monitor and evaluate the effectiveness of health interventions, enabling First Nations communities to access and use location-specific data for informed decision-making.
The Health Plan highlights the need for early access to primary care to prevent late-stage presentations of CVD, and prioritises action on CVD, diabetes, renal health, and rheumatic heart disease. Early intervention is crucial for managing and slowing the progression of these conditions. Addressing RHD and reducing the incidence of acute rheumatic fever (ARF) also requires improvements in housing and environmental health, including access to appropriate housing and functioning health hardware. Australia’s Long Term National Health Plan commits to ending RHD, which involves coordinated action across health service delivery and social infrastructure.
To support workforce capacity, the National Aboriginal and Torres Strait Islander Health Workforce Strategic Framework and Implementation Plan 2021–2031 sets a target of 3.43% First Nations representation in the health workforce by 2031, with actions to attract, recruit, and retain First Nations health workers across all roles and locations.
Early detection and ongoing risk management are central to reducing the CVD burden. The National Strategic Action Plan for Heart Disease and Stroke (the Action Plan) provides a roadmap to improve CVD prevention, diagnosis, treatment, and care. Recognising the disproportionate burden on First Nations people, the plan prioritises strengthening screening and risk factor management for prevention and early detection; improving access to timely and equitable care for diagnosis and treatment; enhancing culturally appropriate support mechanisms for support and care; and driving innovation in prevention and treatment through research (DHDA 2021).
In line with these priorities, the Australian Guideline for Assessing and Managing Cardiovascular Disease Risk integrates specific recommendations for First Nations people, such as screening for risk factors from age 18 and conducting CVD risk assessments from age 30 (DoHAC 2023). However, there are significant challenges in implementing these guidelines effectively.
The study by Agostino et al. (2024) highlighted that cardiovascular risk calculators embedded in general practice software often omit key risk factors, leading to underestimation of high-risk First Nations patients and outdated clinical data compromised risk calculations. To address these gaps, the following measures are essential: ensuring robust oversight and accountability in the implementation of guidelines through improved governance; developing and integrating risk calculators that accurately reflect the unique risk profiles of First Nations people with validated risk assessment tools; and enhancing the quality and timeliness of clinical data to support accurate risk assessments through strengthened data management. These steps are crucial for improving cardiovascular care and outcomes for First Nations communities.
A longstanding commitment by Australian governments has sought to embed cultural respect in the health system to improve First Nations health outcomes. The Cultural Respect Framework 2016–2026 provides a nationally consistent approach to integrating cultural respect into governance, management, policy, and service delivery for First Nations health. It acknowledges systemic barriers, including institutional racism, and promotes culturally safe, responsive, and equitable health services (Australian Health Ministers' Advisory Council 2016). Progress is monitored through the Aboriginal and Torres Strait Islander Health Performance Framework which includes measures such as 3.08 Cultural competency. Additionally, the Cultural safety in health care for Indigenous Australians: monitoring framework assesses progress in achieving cultural safety in the health system. This framework is structured around three modules: culturally respectful health care services, patient experience of health care, and access to health care service (AIHW 2022a). However, significant data gaps remain, particularly regarding cultural safety in mainstream health services. These gaps pose challenges to ensuring effective care for First Nations people, highlighting the need for improved data collection and analysis to better monitor and address these issues.
The 2025–26 Federal Budget includes $9.2 million over 3 years to improve monitoring and detection of ARF and RHD, including education and training. It also allocates $3.5 million to extend the Deadly Choices initiative, which promotes uptake of MBS Item 715 Health Checks.
Targeted investment in research and innovation further supports CVD prevention and management. The Medical Research Future Fund’s (MRFF) Targeted Translation Research Accelerator (TTRA) Research Plan has allocated $77.5 million to advance the prevention, diagnosis, and treatment of diabetes and CVD. This initiative focuses on improving healthcare accessibility and quality for disproportionately affected populations, including First Nations communities. Key areas of investment include developing advanced risk prediction tools to better predict and manage CVD risk, particularly for high-risk populations; integrating technology-driven solutions such as remote patient monitoring systems to support patient-centred care across diverse settings; and ensuring that healthcare services are accessible and of high quality for all populations, with a focus on those disproportionately affected by CVD and diabetes.
Resources to support health professionals in delivering culturally safe CVD care include the Cardiovascular Disease Risk Communication Toolkit for Aboriginal and Torres Strait Islander Peoples. Developed by the Australian National University, the toolkit provides evidence-based strategies to enhance patient engagement, improve health literacy, and support prevention efforts. The toolkit includes a visual CVD risk guide to help patients understand their cardiovascular risk, motivational interviewing techniques to encourage positive health behaviour changes, and Medicare Benefits Schedule (MBS) item guides to facilitate comprehensive, patient-centred care by guiding the use of relevant MBS items.
Additionally, the National Strategic Action Plan for Childhood Heart Disease (2019) provides a nationally coordinated approach to improving lifelong management and specialised care for individuals with childhood heart disease. It acknowledges the unique challenges faced by First Nations communities recognising the disproportionate burden on First Nations people. Key actions include ensuring health services are culturally safe and responsive; expanded specialist outreach in rural and remote areas; building strong relationships with First Nations communities to support better heart health outcomes; workforce initiatives to strengthen First Nations-led care models; and holistic approaches addressing the interconnectedness of physical, social, emotional, cultural, and spiritual wellbeing. The plan also integrates First Nations perspectives in healthcare design (DoH 2019).
References
-
ABS (Australian Bureau of Statistics) (2019) National Aboriginal and Torres Strait Islander Health Survey 2018–19, ABS website, accessed 11 November 2025.
-
ABS (2024a) National Aboriginal and Torres Strait Islander Health Survey 2022–23, ABS website.
-
ABS (2024b) Table 5: Detailed long-term health conditions [data set], National Aboriginal and Torres Strait Islander Health Survey 2022–23, ABS website.
-
Agostino J, Skewes K, Wong D, Timothy A, Wyber R and Greaves K (2024) 'Inaccuracy of cardiovascular disease calculators in Australian primary healthcare software', Australian Journal of General Practice, 53(10):782–784, doi:10.31128/AJGP-09-23-6975.
-
Agostino JW, Wong D, Paige E, Wade V, Connell C, Davey ME, Peiris DP, Fitzsimmons D, Burgess CP and Mahoney R (2020) 'Cardiovascular disease risk assessment for Aboriginal and Torres Strait Islander adults aged under 35 years: a consensus statement', Medical Journal of Australia, 212(9):422–427, doi:10.5694/mja2.50529.
-
AIHW (Australian Institute of Health and Welfare) (2015) Cardiovascular disease, diabetes and chronic kidney disease—Australian facts: Aboriginal and Torres Strait Islander people 2015, Cardiovascular, Diabetes and Chronic Kidney Disease Series, AIHW, Australian Government.
-
AIHW (2020) Atrial fibrillation in Australia, AIHW, Australian Government, accessed 29 January 2026.
-
AIHW (2022a) Cultural safety in health care for Indigenous Australians: monitoring framework, AIHW, Australian Government.
-
AIHW (2022b) Impact and causes of illness and death in Aboriginal and Torres Strait Islander people 2018, Australian Burden of Disease Study, AIHW, Australian Government, doi:10.25816/xd60-4366.
-
AIHW (2024) Better Cardiac Care measures for Aboriginal and Torres Strait Islander people: eighth national report 2023, AIHW, Australian Government.
-
AIHW (2025a) Heart, stroke and vascular disease: Australian facts, AIHW, Australian Government, accessed 30 January 2025.
-
AIHW (2025b) Hospital to community: how Australians with heart failure receive health care, AIHW, Australian Government.
-
AIHW (2026a) Aboriginal and Torres Strait Islander specific primary health care: results from the OSR and nKPI collections, AIHW, Australian Government, accessed 30 January 2026.
-
AIHW (2026b) nKPI preventative health indicators [data set], AIHW website, accessed 30 January 2026.
-
Alston L, Allender S, Peterson K, Jacobs J and Nichols M (2017) 'Rural inequalities in the Australian burden of ischaemic heart disease: a systematic review', Heart, Lung and Circulation, 26(2):122–133, doi:10.1016/j.hlc.2016.06.1213.
-
Alston L, Bourke L, Nichols M and Allender S (2020) 'Responsibility for evidence-based policy in cardiovascular disease in rural communities: implications for persistent rural health inequalities', Australian Health Review, 44(4):527–534, doi:10.1071/AH19189.
-
Australian Health Ministers' Advisory Council (2016) Cultural Respect Framework 2016–2026 for Aboriginal and Torres Strait Islander health, AHMAC website.
-
Balabanski AH, Dos Santos A, Woods JA, Mutimer CA, Thrift AG, Kleinig TJ, Suchy-Dicey AM, Siri SRA, Boden-Albala B, Krishnamurthi RV, Feigin VL, Buchwald D, Ranta A, Mienna CS, Zavaleta-Cortijo C, Churilov L, Burchill L, Zion D, Longstreth WT, Jr., Tirschwell DL, Anand SS, Parsons MW, Brown A, Warne DK, Harwood M, Barber PA and Katzenellenbogen JM (2024) 'Incidence of stroke in Indigenous populations of countries with a very high Human Development Index: a systematic review', Neurology, 102(5):e209138, doi:10.1212/wnl.0000000000209138.
-
Beard JR, Earnest A, Morgan G, Chan H, Summerhayes R, Dunn TM, Tomaska NA and Ryan L (2008) 'Socioeconomic disadvantage and acute coronary events: a spatiotemporal analysis', Epidemiology, 19(3):485–492, doi:10.1097/EDE.0b013e3181656d7f.
-
Becker R, Silvi J, Ma Fat D, L’Hours A and Laurenti R (2006) 'A method for deriving leading causes of death', Bulletin of the World Health Organization 84(4):297–304, doi:10.2471/blt.05.028670.
-
Blacker D and Armstrong E (2019) 'Indigenous stroke care: differences, challenges and a need for change', Internal Medicine Journal, 49(8):945–947, doi:10.1111/imj.14399.
-
Bradshaw PJ, Alfonso HS, Finn J, Owen J and Thompson PL (2011) 'A comparison of coronary heart disease event rates among urban Australian Aboriginal people and a matched non-Aboriginal population', Journal of Epidemiology and Community Health, 65(4):315–319, doi:10.1136/jech.2009.098343.
-
Brown A (2012) 'Addressing cardiovascular inequalities among indigenous Australians', Global Cardiology Science & Practice, 2012(1):2, doi:10.5339/gcsp.2012.2.
-
Brown A and Kritharides L (2017) 'Overcoming cardiovascular disease in Indigenous Australians', Medical Journal of Australia, 206(1):10–12, doi:10.5694/mja16.00693.
-
Campbell MA, Hunt J, Scrimgeour DJ, Davey M and Jones V (2018) 'Contribution of Aboriginal Community-Controlled Health Services to improving Aboriginal health: an evidence review', Australian Health Review, 42(2):218–226, doi:10.1071/ah16149.
-
Chaturvedi A, Zhu A, Gadela NV, Prabhakaran D and Jafar TH (2024) 'Social determinants of health and disparities in hypertension and cardiovascular diseases', Hypertension, 81(3):383–395, doi:10.1161/HYPERTENSIONAHA.123.21354.
-
Cho JH, Shin SY, Kim H, Kim M, Byeon K, Jung M, Kang K-W, Lee W-S, Kim S-W and Lip GYH (2024) 'Smoking cessation and incident cardiovascular disease', JAMA Network Open, 7(11):e2442639–e2442639, doi:10.1001/jamanetworkopen.2024.42639.
-
Commonwealth of Australia as represented by the Department of Health and Aged Care (2023) Australian Guideline for assessing and managing cardiovascular disease risk, Australian Chronic Disease Prevention Alliance.
-
Cunningham J (2010) 'Socio-economic gradients in self-reported diabetes for Indigenous and non-Indigenous Australians aged 18–64', Australian and New Zealand Journal of Public Health, 34 Suppl 1:S18–S24, doi:10.1111/j.1753-6405.2010.00547.x.
-
Davey M, Moore W and Walters J (2014) 'Tasmanian Aborigines step up to health: evaluation of a cardiopulmonary rehabilitation and secondary prevention program', BMC Health Services Research, 14(1):349, doi:10.1186/1472-6963-14-349.
-
DHDA (Department of Health, Disability and Ageing) (2021) National Strategic Action Plan for Heart Disease and Stroke, DHDA, Australian Government.
-
DHDA (2025) First Nations Health Funding Transition Program (FNHFTP), DHDA website.
-
DoH (Department of Health) (2019) National Strategic Action Plan for Childhood Heart Disease – beyond the heart: transforming care, DoH, Australian Government, accessed 4 March 2025.
-
DoH (2021) National Aboriginal and Torres Strait Islander Health Plan 2021–2031, DoH, Australian Government, accessed 2 May 2025.
-
DoHAC (Department of Health and Aged Care) (2023) Australian guideline and calculator for assessing and managing cardiovascular disease risk, DoHAC website, accessed 4 March 2025.
-
End Rheumatic Heart Disease Centre of Research Excellence (2021) Rheumatic Heart Disease Endgame Strategy: what does it mean to community?, The Kids Research Institute Australia website, accessed 3 October 2025.
-
Field PE, Franklin RC, Barker RN, Ring I and Leggat PA (2018) 'Cardiac rehabilitation services for people in rural and remote areas: an integrative literature review', Rural Remote Health, 18(4):4738, doi:10.22605/rrh4738.
-
Hamilton S, Mills B, McRae S and Thompson S (2016) 'Cardiac rehabilitation for Aboriginal and Torres Strait Islander people in Western Australia', BMC Cardiovascular Disorders, 16(1):150, doi:10.1186/s12872-016-0330-3.
-
Hayman NE, Wenitong M, Zangger JA and Hall EM (2006) 'Strengthening cardiac rehabilitation and secondary prevention for Aboriginal and Torres Strait Islander peoples', Medical Journal of Australia, 184(10):485–486, doi:10.5694/j.1326-5377.2006.tb00338.x.
-
Heart Foundation (2022) About the Lighthouse Hospital Project, Heart Foundation website.
-
Illawarra Shoalhaven Local Health District (2023) Aboriginal Healthy Hearts, NSW Health website, accessed 3 October 2025.
-
Javed Z, Haisum Maqsood M, Yahya T, Amin Z, Acquah I, Valero-Elizondo J, Andrieni J, Dubey P, Jackson RK, Daffin MA, Cainzos-Achirica M, Hyder AA and Nasir K (2022) 'Race, racism, and cardiovascular health: applying a social determinants of health framework to racial/ethnic disparities in cardiovascular disease', Circulation: Cardiovascular Quality and Outcomes, 15(1):e007917, doi:10.1161/CIRCOUTCOMES.121.007917.
-
Jeong S-M, Jeon KH, Shin DW, Han K, Kim D, Park SH, Cho MH, Lee CM, Nam K-W and Lee SP (2021) 'Smoking cessation, but not reduction, reduces cardiovascular disease incidence', European Heart Journal, 42(40):4141–4153, doi:10.1093/eurheartj/ehab578.
-
Katzenellenbogen JM, Knuiman MW, Sanfilippo FM, Hobbs MST and Thompson SC (2014) 'Prevalence of stroke and coexistent conditions: disparities between Indigenous and non-Indigenous Western Australians', International Journal of Stroke, 9(SA100):61–68, doi:10.1111/ijs.12278.
-
Kilkenny MF, Harris DM, Ritchie EA, Price C and Cadilhac DA (2013) 'Hospital management and outcomes of stroke in Indigenous Australians: evidence from the 2009 Acute Care National Stroke Audit', International Journal of Stroke, 8(3):164–171, doi:10.1111/j.1747-4949.2011.00717.x.
-
Mbuzi V, Fulbrook P and Jessup M (2018) 'Effectiveness of programs to promote cardiovascular health of Indigenous Australians: a systematic review', International Journal for Equity in Health, 17:153, doi:10.1186/s12939-018-0867-0.
-
Menzies School of Health Research (2024) Rheumatic heart disease, Menzies School of Health Research website, accessed 3 October 2025.
-
Merone L, Burns J, Poynton M and McDermott R (2019) 'Review of cardiovascular health among Aboriginal and Torres Strait Islander people', Australian Indigenous Health Bulletin, 19(4).
-
Mills K, Gatton ML, Mahoney R and Nelson A (2017) '‘Work it out’: evaluation of a chronic condition self-management program for urban Aboriginal and Torres Strait Islander people, with or at risk of cardiovascular disease', BMC Health Services Research, 17:680, doi:10.1186/s12913-017-2631-3.
-
NACCHO (National Aboriginal Community Controlled Health Organisation) (2020) New advice to help stop early heart attacks for Indigenous Australians, NACCHO website.
-
NACCHO (2025) Optimising heart failure care for Aboriginal and Torres Strait Islander people with reduced ejection fraction, NACCHO website.
-
National Heart Foundation of Australia and Australian Cardiac Rehabilitation Association (2004) Recommended Framework for Cardiac Rehabilitation ‘04, National Heart Foundation of Australia.
-
NPS MedicineWise (2022) General practice insights report July 2020–June 2021.
-
Pearson O, Schwartzkopff K, Dawson A, Hagger C, Karagi A, Davy C, Brown A, Braunack-Mayer A and on behalf of the Leadership Group guiding the Centre for Research Excellence in Aboriginal Chronic Disease Knowledge and Translation Exchange (2020) 'Aboriginal community controlled health organisations address health equity through action on the social determinants of health of Aboriginal and Torres Strait Islander peoples in Australia', BMC Public Health, 20:1859, doi:10.1186/s12889-020-09943-4.
-
Peiris D, Usherwood T, Panaretto K, Harris M, Hunt J, Redfern J, Zwar N, Colagiuri S, Hayman N, Lo S, Petel B, Lyford M, MacMahon S, Neal B, Sullivan D, Cass A, Jackson R and Patel A (2015) 'Effect of a computer-guided, quality improvement program for cardiovascular disease risk management in primary health care: the treatment of cardiovascular risk using electronic decision support cluster-randomized trial', Circulation: Cardiovascular Quality and Outcomes, 8(1):87–95, doi:10.1161/CIRCOUTCOMES.114.001235.
-
Porykali B, Davies A, Brooks C, Melville H, Allman-Farinelli M and Coombes J (2021) 'Effects of nutritional interventions on cardiovascular disease health outcomes in Aboriginal and Torres Strait Islander Australians: a scoping review', Nutrients, 13(11):4084, doi:10.3390/nu13114084.
-
Powell-Wiley TM, Baumer Y, Baah FO, Baez AS, Farmer N, Mahlobo CT, Pita MA, Potharaju KA, Tamura K and Wallen GR (2022) 'Social determinants of cardiovascular disease', Circulation Research, 130(5):782–799, doi:10.1161/CIRCRESAHA.121.319811.
-
Price E, Kotevski A, Lamb K, Koye D, Taylor G, Ebsworth G and Burchill L (2024) 'Presentations to selected Melbourne hospitals with cardiovascular disease by Indigenous and non-Indigenous people, 2011–19: a linked administrative data analysis', Medical Journal of Australia, 220(4):208–210, doi:10.5694/mja2.52215.
-
Randall DA, Lujic S, Havard A, Eades SJ and Jorm L (2018) 'Multimorbidity among Aboriginal people in New South Wales contributes significantly to their higher mortality', Medical Journal of Australia, 209(1):19–23, doi:10.5694/mja17.00878.
-
Reath JS and O'Mara P (2018) 'Closing the gap in cardiovascular risk for Aboriginal and Torres Strait Islander Australians', Medical Journal of Australia, 209(1):17–18, doi:10.5694/mja18.00345.
-
Rowley K, O'Dea K, Anderson I, McDermott R, Saraswati K, Tilmouth R, Roberts I, Fitz J, Wang Z, Jenkins A, Best J, Wang Z and Brown A (2008) 'Lower than expected morbidity and mortality for an Australian Aboriginal population: 10-year follow-up in a decentralised community', Medical Journal of Australia, 188(5):283–287, doi:10.5694/j.1326-5377.2008.tb01621.x.
-
Spinks J, Mihala G, Jennings W, Ware RS, Kalisch Ellett LM, Roughead EE and Williamson D (2025) 'Potentially preventable medication-related hospitalisations with cardiovascular disease of Aboriginal and Torres Strait Islander people, Queensland, 2013–2017: a retrospective cohort study', Medical Journal of Australia, 222(4):198–204, doi:10.5694/mja2.52600.
-
Thurber KA and Bell KJ (2019) 'Socio-economic disadvantage and cardiovascular risk factors in young Aboriginal and Torres Strait Islander Australians', Medical Journal of Australia, 211(6):259–260, doi:10.5694/mja2.50327.
-
Tiedeman C, Suthers B, Julien B, Hackett A and Oakley P (2019) 'Management of stroke in the Australian Indigenous population: from hospitals to communities', Internal Medicine Journal, 49(8):962–968, doi:10.1111/imj.14303.
-
WHO (World Health Organisation) (2021) Cardiovascular diseases (CVDs), WHO website, accessed 25 February 2025.
-
You J, Condon JR, Zhao Y and Guthridge SL (2015) 'Stroke incidence and case-fatality among Indigenous and non-Indigenous populations in the Northern Territory of Australia, 1999–2011', International Journal of Stroke, 10(5):716–722, doi:10.1111/ijs.12429.
-
Zhao Y, Condon J, You J, Guthridge S and He V (2015) 'Assessing improvements in survival for stroke patients in the Northern Territory 1992–2013: a marginal structural analysis', Australian Health Review, 39(4):437–443, doi:10.1071/ah14146.

