Key messages
Why is it important?
Chronic high blood pressure (hypertension) is a leading risk factor for cardiovascular disease (CVD), stroke, kidney disease, and other serious conditions, often developing without symptoms. It is more prevalent among Aboriginal and Torres Strait Islander (First Nations) adults, contributing to earlier and more severe disease. Effective management requires early detection and regular health checks from age 18, with CVD risk assessment by age 30, alongside culturally safe care and strategies to overcome barriers such as cost, access, and lack of culturally appropriate services. Lifestyle changes such as healthy eating, physical activity, reducing salt and alcohol, and quitting smoking remain essential but are shaped by complex social and environmental factors, and many people require lifelong medication and monitoring to reduce long-term risks.
Data findings
-
In 2022–23, 33% (an estimated 198,400) of First Nations adults had high blood pressure (140/90 mmHg or higher) – this includes people who self-reported having high blood pressure (even if their measured blood pressure was normal), as well as those who had their blood pressure measured as part of the survey and it was recorded as high.
-
In 2022–23, First Nations adults were 1.3 times as likely to have high blood pressure as non-Indigenous Australians (after adjusting for differences in the age structure between the two populations), contributing significantly to the burden of CVD.
-
First Nations adults who reported having cardiovascular disease were 3.2 times as likely to have high blood pressure as those who did not have cardiovascular disease (72% or 91,100 adults compared with 23% or 107,800).
-
The rate of hospitalisation due to hypertensive disease for First Nations people was higher in remote than non-remote areas – 141 per 100,000 compared with 42 per 100,000 population respectively, over the period July 2021 to June 2023.
-
From 2016–17 to 2022–23, the age-standardised rate of hospitalisation for hypertensive disease for First Nations males and females fluctuated, as did the gap in the rates for First Nations people and non-Indigenous Australians.
Research and evaluation findings
-
First Nations people experience CVD 10–20 years earlier than non-Indigenous Australians, with delayed presentation and limited access to guideline-based care contributing to poorer outcomes and higher mortality. Hypertension is multifactorial, requiring culturally safe, community-led models and improved specialist access, screening (including endocrine causes), and integrated social supports alongside lifestyle and pharmacotherapy strategies.
-
Cardiometabolic risk factors and high rates of hypertension are often evident by adolescence, especially among males and those with obesity, highlighting the need for targeted screening and prevention programs for children and adolescents.
-
Preventive health attendance among young First Nations people is low, and follow-up after blood pressure checks is inconsistent. Waist circumference should complement BMI measurement in routine screening. Primary aldosteronism – the most frequent endocrine cause of hypertension – remains underdiagnosed due to lack of guidelines and limited diagnostic capacity in remote areas.
-
Pre-pregnancy obesity and metabolic syndrome significantly increase the risk of hypertensive disorders in pregnancy among First Nations women, contributing to adverse maternal and infant outcomes – early identification and culturally safe preconception care are essential.
-
Reviews identify integration with existing services and culturally appropriate delivery as key features of effective programs. Aboriginal Community Controlled Health Services play a vital role by embedding cultural safety, addressing social determinants, and improving patient engagement and outcomes.
Implications
Despite being easily detectable and treatable, hypertension remains underdiagnosed and contributes substantially to CVD, kidney disease, and stroke. Addressing this requires culturally safe, early interventions starting in adolescence, improved access to MBS health assessments, Chronic Disease Management Plans, and PBS-subsidised medicines. Strengthening community-led models of care and embedding continuous quality improvement will help reduce preventable hospitalisations and improve long-term health outcomes.
Why is it important?
Chronic high blood pressure, or hypertension, is one of the most common and serious conditions affecting the heart and blood vessels, often developing silently without noticeable symptoms. It is a major risk factor for heart disease, heart failure, stroke, kidney disease, and blood vessel damage including to the legs and feet (peripheral arterial disease), the eyes (hypertensive retinopathy) and the brain (leading to vascular dementia) (American Heart Association n.d., Blood Pressure Association n.d.). High blood pressure is defined as a systolic blood pressure greater than 140 mmHg and/or diastolic pressure greater than 90 mmHg and/or a patient receiving medication for high blood pressure (National Heart Foundation of Australia 2016). Over time, untreated hypertension can lead to severe damage to vital organs, including the heart, brain, and kidneys, significantly increasing the risk of life-threatening complications. Hypertension becomes more prevalent with age and is influenced by having a family history of the condition as well as modifiable risk factors such as poor diet, high salt intake, heavy alcohol consumption, physical inactivity and smoking (National Heart Foundation of Australia 2025a, 2025b). A number of these risk factors are more prevalent among Aboriginal and Torres Strait Islander (First Nations) people (see measures 2.15 Tobacco use, 2.16 Risky alcohol consumption, 2.18 Physical activity, and 2.19 Dietary behaviour).
First Nations adults have a higher prevalence of hypertension than non-Indigenous Australians, contributing significantly to the burden of cardiovascular disease (CVD). CVD is a major cause of morbidity and mortality among First Nations people, with higher rates and earlier age of onset than non-Indigenous Australians (see measure 1.05 Cardiovascular disease). Ischaemic heart disease (also known as coronary heart disease) was the leading cause of death for First Nations people in 2024 (ABS 2025).
The Australian Guideline for assessing and managing cardiovascular disease risk emphasises the importance of culturally responsive care and tailored approaches for First Nations communities. It recommends early and regular health checks, with blood pressure monitoring starting at age 18 and estimating CVD risk from age 30 (rather than 35 years). These recommendations reflect the earlier onset and higher prevalence of CVD among First Nations people, aiming to improve early detection and preventive care. The guideline also recognises that the gap in health outcomes for First Nations people stems from dispossession, discrimination, disadvantage and disempowerment (DoHAC 2023).
Management of hypertension in the primary health care setting is critically important for preventing cardiovascular events. However, effective management faces challenges with inconsistent measurement and treatment approaches in Australia (Hespe et al. 2025). Management of hypertension should not solely rely on blood pressure thresholds but should be part of a holistic health assessment.
Under the Medicare Benefits Schedule (MBS), First Nations-specific health assessments (such as MBS item 715) conducted by qualified health professionals provide a culturally safe and tailored approach to managing hypertension and broader cardiovascular risks. Addressing barriers to care, such as geographic isolation, unaffordability, lack of transportation, and the absence of culturally safe services, is critical for ensuring effective management of chronic disease. For many, antihypertensive medications are necessary to control blood pressure and reduce long-term risks, often as part of lifelong treatment. First Nations people are eligible to access subsidised medicines through the Closing the Gap PBS Co-payment Program. Regular monitoring by health-care professionals, supported by home measurements, helps track progress and ensure successful management. While early detection and lifestyle changes such as maintaining a healthy weight, being physically active, reducing salt and alcohol intake, and quitting smoking remain essential, it is important to recognise these behaviours are shaped by complex social, cultural, and environmental determinants which may not reflect individual choice alone (National Heart Foundation of Australia 2025a, 2025b).
Burden of disease
In 2018, high blood pressure was estimated to be responsible for 4.3% (10,382 attributable DALY) of the total disease burden for First Nations people, and this proportion increased with age. Total burden due to high blood pressure was highest among those aged 45–64 for both First Nations males and females (AIHW 2022a, 2022b).
Among First Nations people, 84% of total disease burden attributed to high blood pressure was due to premature death (that is, fatal burden). There were 348 deaths attributable to high blood pressure (9.6% of total deaths) for First Nations people, equivalent to 8,729 years of life lost due to premature death.
Among First Nations people, 62% of the burden due to hypertensive heart disease in 2018 was attributed to high blood pressure. High blood pressure also contributed to 41% of the burden of coronary heart disease, 39% of stroke burden, 32% of atrial fibrillation & flutter burden and 30% of chronic kidney disease burden.
In 2018, high blood pressure was one of the leading risk factors contributing to the gap in attributable disease burden, accounting for 6.5% of the health gap between First Nations people and non-Indigenous Australians (AIHW 2022b).
Data findings
First Nations adults with high blood pressure
In 2022–23, in the National Aboriginal and Torres Strait Islander Health Survey (NATSIHS), people were asked whether they had been told by a health professional that they had high blood pressure (hypertension). They were also invited to have their blood pressure measured during the interview. Where a valid measurement was not obtained (for example, due to equipment issues or incomplete readings) the imputation of values was used to improve completeness and reduce bias in estimates of measured blood pressure (ABS 2024b). A high blood pressure reading does not necessarily mean the person had hypertension but may indicate a person may have undiagnosed or untreated hypertension.
In 2022–23, 33% (an estimated 198,400) of First Nations adults had high blood pressure. This included:
- 50,700 adults who self-reported having current and long-term high blood pressure, but had measured blood pressure in the normal (<120/80 mmHg) or pre-hypertensive range (<140/90 mmHg) at the time of the interview
- 29,400 adults who self-reported having high blood pressure and had measured blood pressure in the high blood pressure range (140/90 mmHg or higher)
- 118,900 adults who did not self-report having high blood pressure but did have measured blood pressure in the high blood pressure range (140/90 mmHg or higher) (Table D1.07.1).
After adjusting for differences in the age structure between the two populations, First Nations adults were 1.3 times as likely to have high blood pressure as non-Indigenous adults – 37% (198,400) compared with 30% (6,259,100), respectively. For measured data only (that is, not including self-reported), First Nations adults were also 1.3 times as likely as non-Indigenous adults to have high blood pressure (Table D1.07.1).
Undiagnosed high blood pressure
In 2022–23, of First Nations adults who had their blood pressure measured:
- 25% had high blood pressure (140/90 mmHg or higher) (an estimated 148,400 of 602,200 adults).
- 36% (218,000) had blood pressure elevated above normal levels, but not considered high (pre-hypertensive; between 120/80 to 140/90 mmHg).
- The remaining 39% (235,500) had a measured blood pressure within normal ranges (Table D1.07.1, Figure 1.07.1).
Figure 1.07.1: Proportion of First Nations people aged 18 and over by measured blood pressure status and whether reported high blood pressure, 2022–23
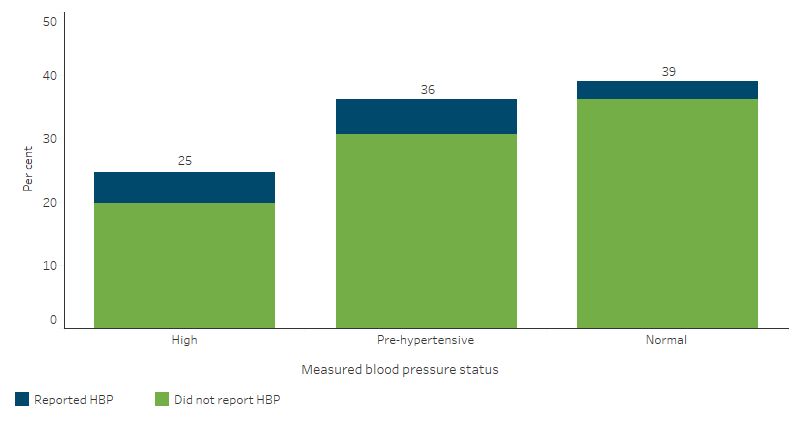
Source: Table D1.07.1. AIHW and ABS analysis of National Aboriginal and Torres Strait Islander Health Survey 2022–23.
Of the 148,400 First Nations adults whose blood pressure was measured as high, 20% (an estimated 29,400 people) reported having hypertension that was current and long-term, and 30% (an estimated 44,100) reported having ever been diagnosed with hypertension (Table D1.07.2, Table D1.07.3). Therefore, 70% (an estimated 104,500) of those with blood pressure measured as high reported having never been diagnosed with hypertension, indicating possible underdiagnosis (Table D1.07.3).
After adjusting for differences in the age structure between the two populations, the proportion of adults with measured high blood pressure that did not report current and long-term hypertension was not statistically significantly different between First Nations and non-Indigenous adults (ratio of 1.0) (Table D1.07.2).
In 2022–23, of the First Nations adults who reported having hypertension and had their blood pressure measured as part of the NATSIHS survey, 22% (an estimated 17,600) returned results within normal ranges, suggesting their hypertension was likely controlled at the time of the survey (Table D1.07.1).
In 2022–23, nearly 9 in 10 First Nations adults (85% or 511,600) reported having had their blood pressure checked in the last 2 years (Table D1.07.2).
Who has high blood pressure?
For all Australians, the likelihood of high blood pressure increases with age. The highest proportions of reported and measured high blood pressure were for those aged 55 and over in both First Nations and non-Indigenous populations. These proportions were higher for First Nations people across all age groups compared with non-Indigenous Australians, excluding the 55+ age group (see Figure 1.07.2). The largest gap between First Nations and non-Indigenous Australians was in the 45–54 age group (16 percentage points) (Table D1.07.7, Figure 1.07.2). For First Nations people, the proportion of reported and measured high blood pressure were similar between non-remote (ranging from 14% to 58%) and remote areas (ranging from 8% to 56%) across age groups (Table D1.07.7).
Figure 1.07.2: High blood pressure, by Indigenous status and age group, 2022–23
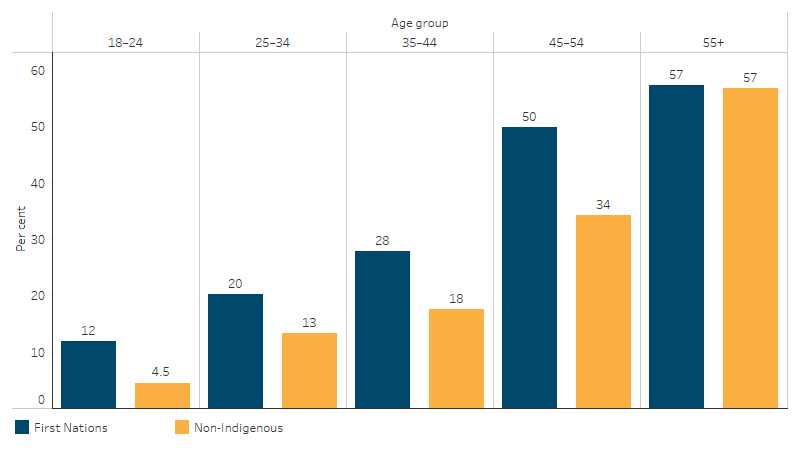
Note: The difference between First Nations and non-Indigenous Australians was not statistically significant for the 55+ age group. The prevalence of high blood pressure includes those reporting having high blood pressure/hypertension (regardless of measured blood pressure) plus those who did not report having high blood pressure/hypertension but who had a measured blood pressure of 140/90 mmHg or above.
Source: Table D1.07.7. AIHW and ABS analysis of National Aboriginal and Torres Strait Islander Health Survey 2022–23.
The 2022–23 NATSIHS showed that 35% (an estimated 103,100) of First Nations males and 31% (95,600) of First Nations females had high blood pressure when measured using both self-report and a collected blood pressure reading (Table D1.07.4). Using only the collected blood pressure reading, 27% of First Nations males and 23% of First Nations females had high measured blood pressure in 2022–23 (Table D1.07.3).
In 2022–23, the proportion of First Nations adults with high blood pressure, based on both reported and measured data, was not statistically different in remote areas (35%, or 34,400 adults) and non-remote areas (33% or 164,500 adults) (Table D1.07.4).
The 2022–23 NATSIHS showed that First Nations adults who completed Year 9 or below were 1.7 times as likely to have high blood pressure (45%) as those who had completed Year 12 (26%) (Table D1.07.5).
There were also several associations between health risk factors and other health conditions and high blood pressure. First Nations adults who:
- reported having cardiovascular disease were 3.2 times as likely to have high blood pressure as those who did not have cardiovascular disease (72% or 91,100 adults compared with 23% or 107,800).
- were obese were 1.8 times as likely as those not obese to have high blood pressure (44% or 116,900 compared with 24% or 81,500).
- considered their health to be fair/poor were 1.6 times as likely as those reporting excellent/very good/good health to have high blood pressure (45% or 72,900 compared with 29% or 125,800).
- reported having diabetes were 1.8 times as likely to have high blood pressure as those who did not have diabetes (54% or 40,600 compared with 30% or 158,100).
- reported having kidney disease were 1.8 times as likely to report having high blood pressure as those who did not have kidney disease (60% or 7,700 compared with 32% or 191,000) (Table D1.07.6).
High blood pressure and management of type 2 diabetes
High blood pressure is common among people with diabetes and regular monitoring is recommended as part of ongoing care. The Royal Australian College of General Practitioners (RACGP) diabetes management guidelines note that the general target blood pressure for people with type 2 diabetes is generally less than or equal to 140/90 mmHg (RACGP and Diabetes Australia 2024).
In June 2025, Commonwealth-funded First Nations-specific primary health care organisations provided national Key Performance Indicators (nKPI) data based on best practice guidelines. In the 6 months to June 2025, of the 49,376 regular clients with type 2 diabetes, 66% (32,806) had their blood pressure assessed. Of those who had their blood pressure assessed, 21,829 (67%) had results in the recommended range (less than or equal to 140/90mmHg) (Table D3.05.16).
Hospitalisation for hypertensive disease
Prolonged high blood pressure can cause damage to the heart and other organs, known as hypertensive disease (AIHW 2026). Between July 2021 and June 2023, there were 1,147 hospitalisations of First Nations people with a principal diagnosis of hypertensive disease, accounting for 0.2% of all hospitalisations for First Nations people, excluding dialysis (Table D1.07.10, Table D1.02.1).
Hospitalisation by sex, age group and by Indigenous status
Between July 2021 and June 2023, the overall hospitalisation rate for hypertensive disease was 71 hospitalisations per 100,000 population for First Nations females and 44 hospitalisations per 100,000 population for First Nations males. Hospitalisation rates for hypertensive disease among First Nations people increased with age. First Nations females had a higher rate of hospitalisations for hypertensive disease than First Nations males for age groups 35 and over (Table D1.07.9, Figure 1.07.3).
Figure 1.07.3: Hospitalisation rates for hypertensive disease (based on principal diagnosis) for First Nations people, by age group and sex, Australia, July 2021 to June 2023
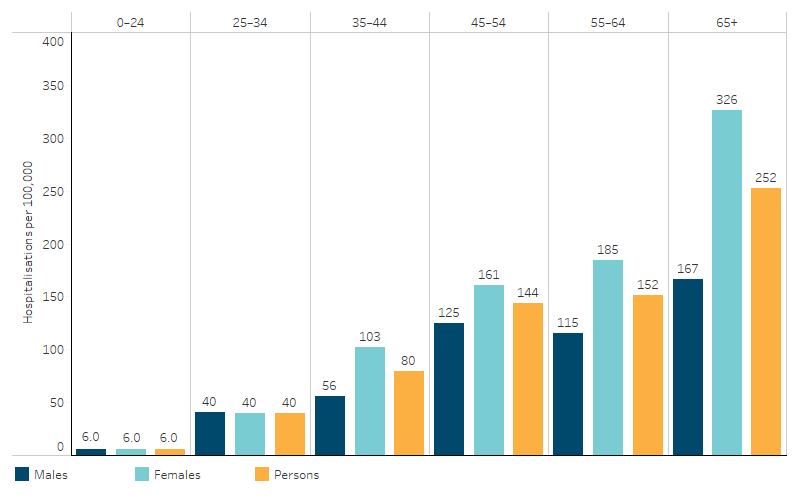
Source: Table D1.07.9. AIHW analysis of National Hospital Morbidity Database.
The rate of hospitalisation for hypertensive disease was higher for First Nations people than non-Indigenous Australians across all age groups. After adjusting for differences in the age structure between the two populations, the rate of hospitalisations due to hypertensive disease for First Nations people was 2.2 times the rate for non Indigenous Australians. The greatest relative difference in hospitalisation rates between the two populations was for those aged 25–34, where the rate for First Nations people was 4.7 times the rate for non-Indigenous Australians (Table D1.07.9).
Hospitalisation by remoteness, jurisdiction and by Indigenous status
Between July 2021 and June 2023, the rate of hospitalisations due to hypertensive disease for First Nations people varied across jurisdictions, from 31 per 100,000 population in New South Wales and Victoria to 146 per 100,000 population in the Northern Territory (Table 1.07.14; excludes Tasmania and the Australian Capital Territory, Figure 1.07.4).
The rate of hospitalisations due to hypertensive disease for First Nations people was higher in remote than non-remote areas across all jurisdictions and nationally: 141 hospitalisations per 100,000 population compared with 42 per 100,000, respectively (Figure 1.07.4).
After adjusting for differences in the age structure between the two populations, First Nations people living in remote areas were hospitalised for hypertensive disease at 3.7 times the rate of non-Indigenous Australians; in non-remote areas, the rate for First Nations people was 1.7 times as high. By jurisdiction, the largest difference in hospitalisation rates between the two populations was in the Northern Territory, with the rate for First Nations people 4 times the rate for non-Indigenous Australians (Table D1.07.10).
Figure 1.07.4: Hospitalisation rates for hypertensive disease (based on principal diagnosis) for First Nations people, by jurisdiction and remoteness, Australia, July 2021 to June 2023
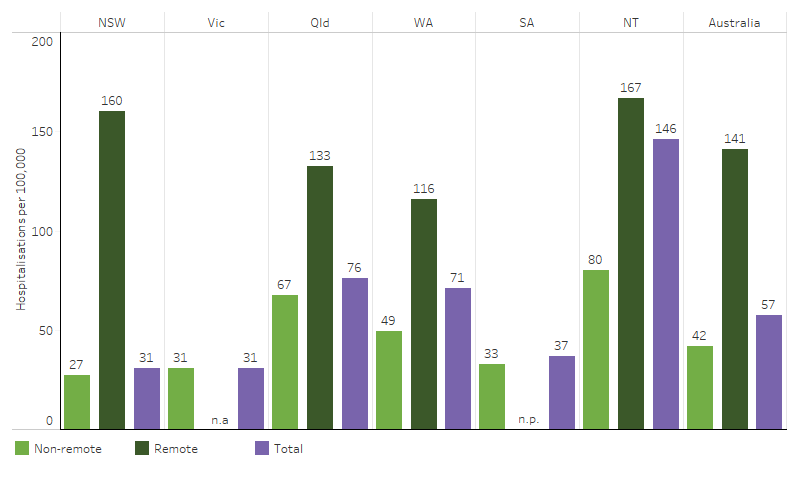
Note: Due to small numbers, Remote areas of Victoria are excluded from the remote category and instead included in the non-remote category. Data for the Australian Capital Territory and Tasmania are not published for confidentiality and/or reliability reasons, but are included in the ‘Australia’ totals.
Source: Table D1.07.14. AIHW analysis of National Hospital Morbidity Database.
Change over time
Looking at burden of disease statistics, between 2003 and 2018, there was a 45% reduction in age-standardised total burden attributable to high blood pressure (from 41 to 23 per 1,000 population). The age-standardised rate of disease burden attributed to high blood pressure declined for both First Nations and non-Indigenous Australians, with First Nations people having 2.8 times the rate of non-Indigenous Australians in 2018 (as compared with 2.6 times in 2003) (AIHW 2022b).
Looking at hospitalisations data, from 2016–17 to 2022–23, the (crude) rate of hospitalisations due to hypertensive disease among First Nations people fluctuated over the period, ranging from a low of 46 per 100,000 in 2016–17 to a high of 62 per 100,000 population in 2020–21 (Table D1.07.13).
The (crude) hospitalisation rate due to hypertensive disease among First Nations males fluctuated between a low of 34 per 100,000 in 2016–17 and a high of 50 per 100,000 in 2022–23, while the rate for First Nations females fluctuated between a low of 57 per 100,000 in 2016–17 and a high of 77 per 100,000 in 2020–21 (Table D1.07.13).
Changes in the rate over time can be affected by ageing of the population. From 2016–17 to 2022–23, based on age-standardised rates (which adjusts for changes in age-structure over time), the rate of hospitalisations due to hypertensive disease for First Nations males and females also fluctuated, as did the gap between First Nations people and non-Indigenous Australians (Table D1.07.13, Figure 1.07.5).
Figure 1.07.5: Age-standardised hospitalisation rates for a principal diagnosis of hypertensive disease, by Indigenous status, Australia, 2016–17 to 2022–23
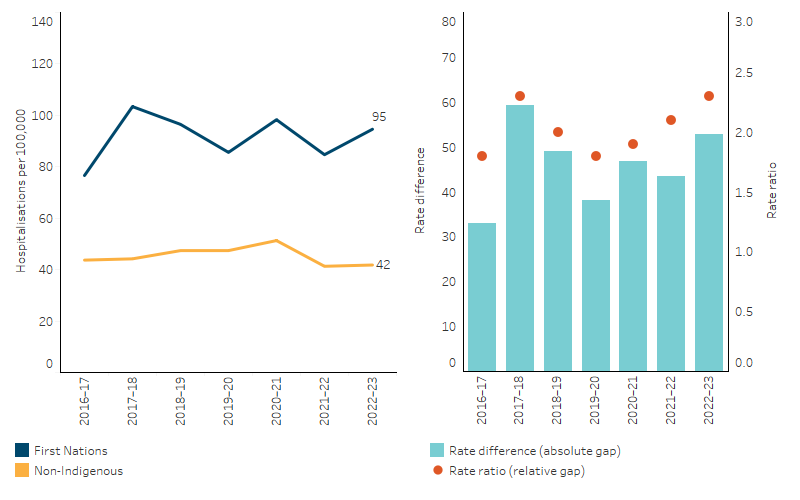
Note: Rate difference is the age-standardised rate (per 100,000) for First Nations people minus the age-standardised rate (per 100,000) for non-Indigenous Australians. Rate ratio is the age-standardised rate for First Nations people divided by the age-standardised rate for non-Indigenous Australians.
Source: Table D1.07.13. AIHW analysis of National Hospital Morbidity Database.
Research and evaluation findings
Overview
Chronic high blood pressure, or hypertension, is more common among First Nations people than non-Indigenous Australians. It contributes to significantly higher rates of heart attacks, strokes and other cardiovascular diseases as well as premature deaths. While genetic predisposition plays a role for some people, research has shown that hypertension is often preventable or controllable through risk-factor modification such as regular physical activity, healthy eating, maintaining a healthy weight, avoidance and cessation of smoking, management of stress and sleep levels, and taking prescribed medicines. Evidence also emphasises the importance of culturally tailored risk‑factor management approaches for First Nations communities (Charchar et al. 2024; Semlitsch et al. 2013).
However, these steps are not equally accessible to everyone. Many First Nations people face barriers such as the cost of healthy food, limited access to culturally safe health care, transport challenges and local environments that do not support preventive health actions. These barriers are further shaped by broader social determinants, including housing, income, and food security, which influence people’s ability to stay healthy (NACCHO and RACGP 2024; National Heart Foundation of Australia 2026).
There is also evidence that genetic risk for hypertension may differ between population groups across the world (Keaton et al. 2021), but this area remains under‑studied in First Nations communities.
Maternal health
A cohort study of First Nations women in North Queensland identified pre pregnancy obesity and metabolic syndrome features, including elevated waist circumference and two or more of high triglycerides, high blood pressure, high blood sugar, or low high-density lipoprotein (HDL) cholesterol, as strong predictors of hypertension in pregnancy, with associated risks to infant health (Campbell et al. 2013).
An international systematic review and meta-analysis of literature on Indigenous peoples found that pre-pregnancy obesity was linked to about 1.9 times higher odds of preeclampsia and hypertensive disorders of pregnancy (odds ratio [OR] of 1.88), while being overweight carried about 1.3 times higher odds (OR of 1.32). Pre-existing diabetes was associated with about 3.6 times higher odds (OR of 3.63), and microalbuminuria, a marker of kidney stress, was linked to about 2.8 times higher odds (OR of 2.76). These findings highlight the importance of early identification and management of cardiometabolic risk factors in First Nations women, particularly through culturally safe preconception care and antenatal screening to improve maternal and infant health outcomes (Stephens et al. 2025).
Hypertension among young people
Being born with a low birthweight may have consequences later in life. The fetal origins hypothesis associated with David J. Barker posits that chronic, degenerative conditions of adult health, such as type 2 diabetes and heart disease, may be triggered by circumstances in utero (Almond and Currie 2011). Low birthweight has been identified as a risk factor for elevated blood pressure later in life, particularly when combined with higher adult body weight (Singh and Hoy 2003; Zhang et al. 2021).
Analysis of baseline data from the Next Generation: Youth Wellbeing Study of First Nations young people aged 10–24 years, found that 19% of participants had hypertension and 12% had pre-hypertension, with similar prevalence across regional, remote, and urban communities. Rates were highest among those aged 20–24 years, where more than one-third (37%) had hypertension. Risk was much higher for men, who were about 4 times as likely to have pre-hypertension (Relative Risk Ratio [RRR] of 4.22) and nearly twice as likely to have hypertension (RRR of 1.93) compared to women. People with obesity were more than 3 times as likely to have hypertension (RRR of 3.20), highlighting the importance of early interventions to prevent heart disease (Sahle et al. 2025).
One study in New South Wales found that blood pressure is frequently elevated in urban First Nations children, aged 2–17 years. The study found that the strongest predictors of blood pressure were parent’s blood pressure and the child’s BMI. The study recommended family-based interventions to reduce blood pressure in this high-risk group (Larkins et al. 2017).
First Nations people experience cardiovascular disease at much earlier ages (10–20 years earlier), typically in their late 20s or early 30s, compared with non-Indigenous Australians. A young patient with severe disease may ignore symptoms until very late, resulting in late presentation, delayed treatment and a poor outcome (Agostino et al. 2020; AIHW 2024a).
Disparities in screening and care
Hypertension screening and follow-up care remain inconsistent, particularly in remote First Nations communities. A review of preventive health attendance at primary health care centres found that 46% of First Nations people aged 15–34 attended for acute health needs while only 12% attended for preventive assessment. Blood pressure was recorded in 85% of young First Nations patients, but only 28% of those with elevated blood pressure had documented management plans. The high frequency of risk factors for cardiac conditions and diabetes evident by the age of 15 years, indicate that primary preventive health care should target First Nations people earlier in life with programs aimed at adolescents, children, babies and mothers to circumvent development of these risk factors (Crinall et al. 2017).
Another study examined primary aldosteronism in young First Nations people. Primary aldosteronism is the most frequent endocrine cause of hypertension indicated by an elevated plasma aldosterone-to-renin ratio (ARR), with higher ARR at 17 years of age associated with higher blood pressure at 27 years of age. Patients with primary aldosteronism have a higher risk of stroke, atrial fibrillation, acute myocardial infarction and heart failure. The study found that about one-third of a Top End Cohort and remote First Nations Birth Cohort participants and one-quarter of urban First Nations Birth Cohort participants with ARRs exceeding 70 pmol/mU had at least grade 1 hypertension. However, screening for primary aldosteronism is infrequently performed in primary health care. Barriers to the diagnosis of primary aldosteronism in First Nations people in the Northern Territory include lack of specific guidelines, the inadequacy of local diagnostic services, and the risk of renin cryoactivation during sample transport from remote areas. The study highlighted the need for culturally sensitive and accessible screening services for First Nations people, as the burden of cardiovascular disease among First Nations people is high and information on the prevalence of primary aldosteronism is limited (Ng et al. 2023).
Disparities in early diagnosis and cardiac care likely contribute to the higher death rate from cardiac conditions among First Nations people. This elevated burden is linked to interconnected risk factors, including hypertension, obesity, diabetes, chronic kidney disease and psychosocial stress. For First Nations people, health and wellbeing are deeply rooted in culture, identity, family and community, where physical, emotional and spiritual health are seen as inseparable and sustained through strong relationships and cultural connectedness. This cultural foundation is a protective factor, yet the need to travel long distances for diagnosis or treatment can disrupt these connections and responsibilities, creating barriers to accessing timely care. Additional barriers include geographic isolation, cost, lack of transportation, and the absence of culturally safe specialist care, which can lead to delays in diagnosis and treatment and poorer health outcomes. Hypertension often coexists with other chronic diseases, requiring a holistic, culturally safe approach involving First Nations health workers and multidisciplinary teams. Addressing broader determinants such as socioeconomic disadvantage and healthy living remain critical for hypertension management and cardiovascular health (McBride et al. 2021).
First Nations people are less likely than non-Indigenous Australians to receive guideline-based therapy for acute coronary syndrome (ACS), which includes heart attacks. Among First Nations adults, between 2018 and 2021, 72% of hospitalised ST-segment Elevation Myocardial Infarction (STEMI) events (a severe type of heart attack caused by a complete blockage of a coronary artery) were treated by Percutaneous Coronary Intervention (PCI). After adjusting for age, this was around 0.9 times the rate for non-Indigenous adults. PCI is a procedure that uses a balloon and stent to quickly open blocked heart arteries. Over the same period, 61% of ACS events among First Nations people aged 18 and over included diagnostic angiography or definitive revascularisation (procedures to restore blood flow to the heart), after adjusting for age this was around 0.9 times the rate for non-Indigenous adults (AIHW 2024a).
Access to culturally safe specialist care remains a critical barrier in managing cardiovascular disease among First Nations people. Despite improvements in primary care, many individuals face challenges navigating mainstream health systems that do not reflect their cultural values or lived experiences, leading to delayed diagnosis, reduced treatment adherence, and poorer outcomes. A 2025 scoping review of chronic disease interventions found that cultural safety was most often assessed through First Nations community perspectives, with community acceptance commonly used as a proxy measure. The review recommended using the Australian Health Practitioner Regulation Agency (AHPRA) definition of cultural safety and emphasised co-design with First Nations communities to ensure interventions address practitioner behaviours, knowledge of colonisation impacts, and partnerships with culturally safe services (Woodall et al. 2025). The Better Cardiac Care report also reinforces the importance of improving specialist access and continuity of care to reduce disparities in cardiac outcomes (AIHW 2024a).
Lifestyle management of hypertension should be the first line of prevention or delay the onset of high blood pressure and to reduce CVD risk. Specific recommendations are to start healthy lifestyle early in life (from childhood), including maintaining a healthy body weight, increased levels of different types of physical activity, healthy eating and drinking, avoidance and cessation of smoking and alcohol use, management of stress and sleep levels (Charchar et al. 2024).
Pharmacotherapy
Evidence highlights the role of pharmacotherapy in achieving effective blood pressure control. Effective treatment typically requires two or more medications. Single-pill combination therapies improve adherence and blood pressure control but remain underused due to treatment hesitancy. Modelling from the United States has shown that treatment of hypertension would prevent the greatest number of deaths compared with other preventive services (colonoscopy, mammography and flu vaccinations), given its high prevalence and the proven effectiveness of affordable pharmacological treatment (Schutte et al. 2024).
Community-led models and innovations
Hypertension programs for First Nations people work best when care is integrated with culturally safe, community-led models. Effective approaches combine screening and follow-up within primary care and outreach, support continuity of care, and link patients to social supports and determinants such as housing, food security, and transport. These features improve participation and long-term management of chronic disease (AIHW 2024b; Yadav et al. 2024).
Aboriginal Community Controlled Health Services (ACCHSs) play a critical role in addressing hypertension and chronic disease outcomes through a model of comprehensive, holistic and community-led primary health care. These services integrate clinical care with community development, health promotion and empowerment that addresses both medical needs and the broader determinants of health. Guided by principles of self-determination and cultural safety, ACCHSs deliver care that is accessible, culturally grounded and responsive to community priorities. Continuous Quality Improvement (CQI) processes are embedded across governance, clinical practice and partnerships to ensure service excellence and accountability. Workforce capacity is strengthened by developing First Nations leaders and supporting staff training, wellbeing and retention that sustains high-quality, culturally safe care across the sector (NACCHO 2021).
Evidence on the effectiveness of First Nations-specific hypertension programs remains limited, particularly regarding their long-term health impacts. However, a 2018 review identified effective cardiovascular programs as those integrated into existing services, culturally appropriate, with a central role for First Nations health workers, and provision of support for communities such as transportation (Mbuzi et al. 2018). Digital health platforms show potential for enhancing prevention, treatment, and monitoring of hypertension by providing accessible tools to manage cardiovascular health, particularly in remote communities (CSIRO 2021).
A study of community-based self-guided blood pressure kiosks in pharmacies in 430 locations in Australia recorded nearly one million checks over 3 years, with 22% of users meeting criteria for possible hypertension (systolic ≥140 mmHg or diastolic ≥90 mmHg, or taking blood pressure medication). More than 60% of participants had not had a blood pressure check in the previous 12 months, indicating the kiosks reached individuals with limited recent blood pressure screening. Adults with high blood pressure were more likely to return for repeat checks, while older adults (≥70 years), smokers, and those in Very remote areas were less likely to return. Among users with possible hypertension, nearly half had additional cardiovascular risk factors such as obesity or diabetes. These findings suggest that community kiosks have potential to identify individuals with elevated blood pressure and support self-monitoring, though disparities in uptake remain. Although the study did not investigate uptake by First Nations people the study suggests there is potential for emerging digital innovations to complement screening and preventive health services in primary health care settings, particularly in non-remote areas and in reaching people not regularly screened (O’Hagan et al. 2024).
Implications
Hypertension significantly increases the risk of heart disease, stroke and kidney diseases, and is one of the top causes of death and disease throughout the world. It can be easily detected through measuring blood pressure, at home or in a health centre, and can often be treated effectively with medications that are low cost. The World Health Organization (WHO) reported the global burden of hypertension has doubled to 1.28 billion people over the past 30 years, with most cases (82%) now occurring in low- and middle-income countries. Hypertension remains underdiagnosed and undertreated worldwide, with 720 million people not receiving the necessary care. Factors such as population growth, ageing and limited access to affordable treatments exacerbate this issue, particularly in regions with inequitable health systems. Despite the availability of low-cost medications and straightforward diagnostic measures, fewer than 1 in 4 women and 1 in 5 men with hypertension globally have their blood pressure effectively controlled. Addressing this ‘public health failure‘ requires international collaboration, equitable access to treatment, and comprehensive health strategies to improve detection, treatment, and management of hypertension (WHO 2021).
In an Australian context, similar challenges are evident among First Nations people, who experience higher rates of hypertension and cardiovascular disease, often occurring 10–20 years earlier than in non-Indigenous populations. Studies highlight the structural barriers, geographic isolation and inequitable access to culturally appropriate care which contribute to gaps in prevention, detection and management of hypertension.
The ABS survey data highlight that undiagnosed hypertension is a significant and urgent health challenge, particularly for First Nations people. Combined self‑reported and measured data show that around a third of First Nations adults have high blood pressure, at a rate around 1.3 times as high as for non-Indigenous adults. Hospitalisation rates for hypertension remain twice as high among First Nations people, underscoring the need for culturally tailored, proactive screening, starting in adolescence, and for targeted interventions to better identify patients with high blood pressure, have it well managed, and prevent avoidable hospitalisations (Australian Indigenous HealthInfoNet 2025).
Improving blood pressure outcomes for First Nations people requires culturally safe, well-coordinated primary health care that leverages mechanisms such as Medicare Benefits Schedule (MBS) health assessments and Chronic Disease Management Plans. These tools support early identification of cardiometabolic risk and facilitate access to allied health services (AIHW 2025a, 2025b). Embedding continuous quality improvement (CQI) approaches into routine care has been shown to enhance blood pressure control and reduce cardiovascular risk (Yadav et al. 2024). The Australian Government supports this through MBS-funded GP health assessments and follow-up care, incentive payments for chronic disease management, and subsidised medicines via the Pharmaceutical Benefits Scheme (PBS). However, further analysis of PBS data is needed to determine whether dispensing rates for blood pressure medications differ between First Nations and non-Indigenous Australians, and to identify potential disparities in access and adherence (ABS 2024a). Addressing these gaps is essential to achieving equitable chronic disease management and improving long-term health outcomes for First Nations communities.
Evaluations highlight the need for culturally safe, community-led hypertension interventions for First Nations people, with emerging models such as digital health platforms (Dingli et al. 2024) and culturally informed care frameworks (Woodall et al. 2025) showing promise for improving engagement, outcomes, and sustainability. The National Aboriginal and Torres Strait Islander Health Plan 2021–2031 (the Health Plan) recognises early access to responsive primary care is also key to addressing the higher hospitalisation rates of First Nations people, where presentation often occurs at a later stage of disease and can lead to higher rates of death. The Health Plan provides a holistic framework to achieve health equity for First Nations people. By emphasising self-determination, cultural safety, and the elimination of racism, the plan integrates social and cultural determinants of health across all life stages. This includes addressing factors such as education, housing, and employment that contribute to the prevention of chronic disease. The plan also aligns with the National Agreement on Closing the Gap (the National Agreement) promoting culturally responsive care and inclusive governance to improve access to preventive and chronic disease management strategies.
The National Preventive Health Strategy 2021–2030 aims to reduce modifiable risk factors for hypertension, such as poor diet, obesity, physical inactivity, and smoking. It prioritises collaboration across sectors to create environments that support healthy living and enhance health literacy, while targeting improved health equity for First Nations people. By setting measurable targets and integrating prevention into the health system, this strategy strengthens early detection and monitoring efforts.
Programs under the Indigenous Australians’ Health Programme (IAHP) address barriers to health care access, ensuring culturally appropriate and timely services for First Nations people. These programs support the prevention, detection, and management of hypertension by improving access to high-quality primary care:
- The Primary Health Care Activity initiative enhances preventive health services, such as health promotion and education, while supporting clinical services for early detection and monitoring of hypertension.
- The Integrated Team Care program improves care coordination for individuals with complex chronic conditions, facilitating early intervention and ensuring continuous management.
- The Medical Outreach Indigenous Chronic Diseases Program ensures access to essential health services in rural and remote areas, addressing geographical barriers to preventive and chronic disease care. The program supports specialists and allied health providers to provide targeted chronic disease management for First Nations people, including conditions such as hypertension and diabetes, ensuring equitable care.
The Practice Incentives Program – Indigenous Health Incentive (PIP IHI) supports better chronic disease management by incentivising healthcare providers to enhance care quality, enabling ongoing monitoring and reducing hypertension-related complications.
Access to affordable and timely medicines is critical for both preventing and managing hypertension. Programs that address these needs include:
- The Remote Area Aboriginal Health Services Program, which simplifies access to essential medicines in remote areas by removing logistical barriers such as allowing Aboriginal health services in remote areas to provide free PBS medicines to their patients without the need for a PBS prescription form.
- The Closing the Gap (CTG) PBS Co-payment Program, expanded in the 2024–25 Budget, reduces or eliminates out-of-pocket costs for PBS medicines for First Nations people, ensuring financial barriers do not prevent individuals from accessing necessary treatment.
- The Eighth Community Pharmacy Agreement (8CPA) ensures the availability of affordable, safe, and timely medicines through community pharmacies, with additional measures that benefit First Nations communities.
These programs collectively support the prevention of hypertension-related complications and enhance the management of chronic conditions through improved access to essential medicines. For further information see measure 3.15 Access to prescription medicines.
Programs targeting chronic disease management aim to mitigate the long-term impacts of hypertension by ensuring comprehensive and culturally appropriate care. By focusing on effective management, these programs address the outcomes of hypertension, including its role in other chronic diseases such as cardiovascular and kidney disease, improving overall health and wellbeing for First Nations people.
References
- ABS (Australian Bureau of Statistics) (2024a) Medications, ABS, Australian Government, accessed 26 March 2026.
- ABS (2024b) National Aboriginal and Torres Strait Islander Health Survey 2022–23, ABS website, accessed 30 March 2026.
-
ABS (2025) Causes of death, Australia (2024), ABS website, accessed 31 March 2026.
-
Agostino JW, Wong D, Paige E, Wade V, Connell C, Davey ME, Peiris DP, Fitzsimmons D, Burgess CP, Mahoney R, Lonsdale E, Fernando P, Malamoo L, Eades S, Brown A, Jennings G, Lovett RW and Banks E (2020) 'Cardiovascular disease risk assessment for Aboriginal and Torres Strait Islander adults aged under 35 years: a consensus statement', The Medical Journal of Australia, 212(9):422–427, doi:10.5694/mja2.50529.
-
AIHW (Australian Institute of Statistics) (2022a) Australian Burden of Disease Study 2018: interactive data on risk factor burden among Aboriginal and Torres Strait Islander people, AIHW, Australian Government, accessed 30 March 2026.
-
AIHW (2022b) Impact and causes of illness and death in Aboriginal and Torres Strait Islander people 2018, AIHW, Australian Government, accessed 30 March 2026, doi:10.25816/xd60-4366.
-
AIHW (2024a) Better Cardiac Care measures for Aboriginal and Torres Strait Islander people: eighth national report 2023, AIHW, Australian Government, accessed 31 March 2026.
-
AIHW (2024b) Determinants of health for First Nations people, AIHW, Australian Government, accessed 31 March 2026.
-
AIHW (2025a) Health checks and follow-ups for Aboriginal and Torres Strait Islander people, AIHW, Australian Government, accessed 26 March 2026.
-
AIHW (2025b) Pharmaceutical Benefits Scheme prescriptions: monthly data, AIHW, Australian Government, accessed 26 March 2026.
-
AIHW (2026) Heart, stroke & vascular diseases, AIHW website, accessed 26 March 2026.
-
Almond D and Currie J (2011) 'Killing me softly: the fetal origins hypothesis', Journal of Economic Perspectives, 25(3):153–172, doi:10.1257/jep.25.3.153.
-
American Heart Association (n.d.) Health threats from high blood pressure, American Heart Association website, accessed 26 March 2026.
-
Australian Indigenous HealthInfoNet (2025) Latest information and statistics on Cardiovascular health, Australian Indigenous HealthInfoNet website, accessed 31 March 2026.
-
Blood Pressure Association (n.d.) Why is high blood pressure a problem?, Blood Pressure UK website, accessed 31 March 2026.
-
Campbell SK, Lynch J, Esterman A and McDermott R (2013) 'Pre-pregnancy predictors of hypertension in pregnancy among Aboriginal and Torres Strait Islander women in north Queensland, Australia; a prospective cohort study', BMC Public Health, 13:138, doi:10.1186/1471-2458-13-138.
-
Charchar FJ, Prestes PR, Mills C, Ching SM, Neupane D, Marques FZ, Sharman JE, Vogt L, Burrell LM, Korostovtseva L, Zec M, Patil M, Schultz MG, Wallen MP, Renna NF, Islam SMS, Hiremath S, Gyeltshen T, Chia Y-C, Gupta A, Schutte AE, Klein B, Borghi C, Browning CJ, Czesnikiewicz-Guzik M, Lee H-Y, Itoh H, Miura K, Brunström M, Campbell NRC, Akinnibossun OA, Veerabhadrappa P, Wainford RD, Kruger R, Thomas SA, Komori T, Ralapanawa U, Cornelissen VA, Kapil V, Li Y, Zhang Y, Jafar TH, Khan N, Williams B, Stergiou G and Tomaszewski M (2024) 'Lifestyle management of hypertension: International Society of Hypertension position paper endorsed by the World Hypertension League and European Society of Hypertension', Journal of Hypertension, 42(1):23–49, doi:10.1097/hjh.0000000000003563.
-
Crinall B, Boyle J, Gibson‐Helm M, Esler D, Larkins S and Bailie R (2017) 'Cardiovascular disease risk in young Indigenous Australians: a snapshot of current preventive health care', Australian and New Zealand Journal of Public Health, 41(5):460–466, doi:10.1111/1753-6405.12547.
-
CSIRO (Commonwealth Scientific and Industrial Research Organisation) (2021) Mobile health to mitigate Indigenous CVD, accessed 31 March 2026.
-
Dingli K, Mahoney R, Hobson G and Goodman A (2024) Hypertension scoping study: exploring mobile health technology for the management of hypertension in the Aboriginal and Torres Strait Islander community controlled health sector, CSIRO, QAIHC, accessed 26 March 2026, doi:10.25919/14v6-j245.
-
DoHAC (Department of Health and Aged Care) (2023) Australian guideline and calculator for assessing and managing cardiovascular disease risk, DoHAC website, accessed 31 March 2025.
-
Hespe C, Stocks N and Nelson M (2025) 'Hypertension – a major modifiable and undertreated risk factor', Australian Prescriber, 48(6):194–196, doi:10.18773/austprescr.2025.049.
-
Keaton JM, Hellwege JN, Giri A, Torstenson ES, Kovesdy CP, Sun YV, Wilson PWF, O'Donnell CJ, Edwards TL, Hung AM and Velez Edwards DR (2021) 'Associations of biogeographic ancestry with hypertension traits', Journal of Hypertension, 39(4):633–642, doi:10.1097/hjh.0000000000002701.
-
Larkins N, Teixeira-Pinto A, Banks E, Gunasekera H, Cass A, Kearnes J and Craig JC (2017) 'Blood pressure among Australian Aboriginal children', Journal of Hypertension, 35(9):1801–1807, doi:10.1097/hjh.0000000000001401.
-
Mbuzi V, Fulbrook P and Jessup M (2018) 'Effectiveness of programs to promote cardiovascular health of Indigenous Australians: a systematic review', International Journal for Equity in Health, 17:153, doi:10.1186/s12939-018-0867-0.
-
McBride KF, Franks C, Wade V, King V, Rigney J, Burton N, Dowling A, Howard NJ, Paquet C, Hillier S, Nicholls SJ and Brown A (2021) 'Good heart: telling stories of cardiovascular protective and risk factors for Aboriginal women', Heart, Lung and Circulation, 30(1):69–77, doi:10.1016/j.hlc.2020.09.931.
-
NACCHO (National Aboriginal Community Controlled Health Organisation) (2021) Core Services and Outcomes Framework: the Model of Aboriginal and Torres Strait Islander Community-Controlled Comprehensive Primary Health Care, NACCHO, accessed 31 March 2026.
-
NACCHO and RACGP (Royal Australian College of General Practitioners) (2024) National guide to preventive healthcare for Aboriginal and Torres Strait Islander people: recommendations, RACGP, accessed 26 March 2026.
-
National Heart Foundation of Australia (2016) Guideline for the diagnosis and management of hypertension in adults – 2016, NHFA, accessed 26 March 2026.
-
National Heart Foundation of Australia (2025a) Blood pressure and your heart, Heart Foundation website, accessed 31 March 2026.
-
National Heart Foundation of Australia (2025b) For professionals: CVD risk assessment for Aboriginal and Torres Strait Islander peoples, Heart Foundation website, accessed 31 March 2026.
-
National Heart Foundation of Australia (2026) First Nations heart health, Heart Foundation website, accessed 31 March 2026.
-
Ng E, Gwini SM, Stowasser M, Young MJ, Fuller PJ, Singh GR and Yang J (2023) 'Aldosterone and renin concentrations and blood pressure in young Indigenous and non-Indigenous adults in the Northern Territory: a cross-sectional study', The Medical Journal of Australia, 219(6):263–269, doi:10.5694/mja2.52062.
-
O’Hagan ET, Marschner SL, Mishra S, Min H, Schutte AE, Schlaich MP, Hannebery P, Duncan N, Shaw T and Chow CK (2024) 'Self-guided blood pressure screening in the community: opportunities, and challenges', Hypertension, 81(12):2559–2568, doi:10.1161/HYPERTENSIONAHA.124.23283.
-
RACGP and Diabetes Australia (2024) Management of type 2 diabetes: a handbook for general practice, RACGP, accessed 26 March 2026.
-
Sahle BW, Banks E, Williams R, Joshy G, Jennings G, Craig JC, Larkins NG, Eades F, Ivers RQ and Eades S (2025) 'Blood pressure in young Aboriginal and Torres Strait Islander people: analysis of baseline data from a prospective cohort study', The Medical Journal of Australia, 222(2):91–101, doi:10.5694/mja2.52558.
-
Schutte AE, Bennett B, Chow CK, Cloud GC, Doyle K, Girdis Z, Golledge J, Goodman A, Hespe CM, Hsu MP, James S, Jennings G, Khan T, Lee A, Murphy L, Nelson MR, Nicholls SJ, Raffoul N, Robson B, Rodgers A, Sanders A, Shang C, Sharman JE, Stocks NP, Usherwood T, Webster R, Yang J and Schlaich M (2024) 'National Hypertension Taskforce of Australia: a roadmap to achieve 70% blood pressure control in Australia by 2030', The Medical Journal of Australia, 221(3):126–134, doi:10.5694/mja2.52373.
-
Semlitsch T, Jeitler K, Hemkens LG, Horvath K, Nagele E, Schuermann C, Pignitter N, Herrmann KH, Waffenschmidt S and Siebenhofer A (2013) 'Increasing physical activity for the treatment of hypertension: a systematic review and meta-analysis', Sports Medicine, 43(10):1009–1023, doi:10.1007/s40279-013-0065-6.
-
Singh GR and Hoy WE (2003) 'The association between birthweight and current blood pressure: a cross-sectional study in an Australian Aboriginal community', The Medical Journal of Australia, 179(10):532–535, doi:10.5694/j.1326-5377.2003.tb05679.x.
-
Stephens J, Grande ED, Roberts T, Kerr M, Northcott C, Johnson T, Sleep J and Ryder C (2025) 'Factors associated with preeclampsia and the hypertensive disorders of pregnancy amongst Indigenous women of Canada, Australia, New Zealand, and the United States: a systematic review and meta-analysis', Current Hypertension Reports, 27:10, doi:10.1007/s11906-025-01327-6.
-
WHO (World Health Organisation) (25 August 2021) More than 700 million people with untreated hypertension [media release], WHO, accessed 26 March 2026.
-
Woodall H, Larkins S, Pinidiyapathirage J, Ward R and Evans R (2025) 'Determining the cultural safety of chronic disease interventions for Aboriginal and Torres Strait Islander Australians: a scoping review', Frontiers in Public Health, 13:1462410, doi:10.3389/fpubh.2025.1462410.
-
Yadav UN, Davis JM, Bennett-Brook K, Coombes J, Wyber R and Pearson O (2024) 'A rapid review to inform the policy and practice for the implementation of chronic disease prevention and management programs for Aboriginal and Torres Strait Islander people in primary care', Health Research Policy and Systems, 22:34, doi:10.1186/s12961-024-01121-x.
-
Zhang Y, Liang J, Liu Q, Fan X, Xu C, Gu A, Zhao W and Hang D (2021) 'Birth weight and adult obesity index in relation to the risk of hypertension: a prospective cohort study in the UK Biobank', Frontiers in Cardiovascular Medicine, 8:637437, doi:10.3389/fcvm.2021.637437.

